
I have spent most of my career working to improve eye care and reduce the burden of blindness in developing areas and disadvantaged populations. For the opportunities this experience has afforded me, I must thank Fred Hollows, AC, the New Zealand ophthalmologist well known for his work restoring vision to countless individuals in Australia. The Fred Hollows Foundation continues his work to this day.
One could say I was led astray by Dr. Hollows when I was a young ophthalmologist, and, in many ways, I have been astray ever since. My career has been committed to finding ways to improve eye care for underserved groups. In the process, I have learned many lessons that apply to practice in the developed world as well.
A MEMORABLE CAREER PATH
Having just finished my ophthalmology training, I spent part of a year working with Professor Hollows as Assistant Director of the National Trachoma and Eye Health Program of Australia, in which more than 60,000 Aboriginal people were examined and some 27,000 were treated for trachoma.
Since then, my interests have remained focused on problems in underserved areas and what can be done from a public health or epidemiologic approach to try to find solutions to those problems. In these efforts, I have worked with the International Agency for the Prevention of Blindness, which represents many of the vision-oriented nongovernmental organizations (NGOs) around the world, and with the World Health Organization (WHO), developing a Collaborative Center for the Prevention of Blindness and serving on a number of WHO advisory groups. Most recently, since 2014, I have served as President of the International Council of Ophthalmology (ICO, Figure 1).


Figure 1. The author as president of the ICO.
What is often striking when working in underserved areas is the extent of the unmet needs for eye care. The scale of need, and the types of interventions that can be undertaken, can be vastly different from the sorts of problems and solutions one might see in one’s own clinic or hospital service.
For example, one of the most salient things I remember from fairly early in my career was working for the WHO in Pakistan in 1980, during the Russian invasion of Afghanistan. I spent 4 days in four different refugee camps for Afghan refugees (Figure 2). I examined 1,000 or more children in the four camps and noted high levels of vitamin A deficiency and trachoma. When I returned to Islamabad, I sat down with representatives from the WHO and the United Nations High Commission for Refugees and discussed what could be done. These discussions led to ordering treatment for vitamin A deficiency and trachoma for 1.5 million people. It would take a long time to influence care for that many people working in my clinic!
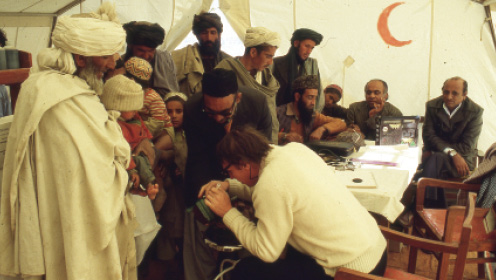
Figure 2. The author examining Afghan refugees in refugee camps in western Pakistan in 1980.
More broadly, in the area of trachoma, we worked to coordinate research projects in different parts of the world helping to build evidence for what is now known as the SAFE strategy for trachoma control: Surgery for trichiasis, the use of Antibiotics, and the importance of Facial cleanliness, and Environmental improvement (Figure 3).1 This is now implemented by the WHO.

Figure 3. The launch of new health promotion and educational material on trachoma for use in Australian Aboriginal communities.
Similarly, the work we did in developing the drug ivermectin, which is now being used to treat 150 million people per year, has had a tremendous impact (Figure 4). It has eliminated river blindness, or onchocerciasis, from most of the countries in Latin America and several countries in Sub-Saharan Africa.

Figure 4. The author treating the first patient in Liberia in the first clinical trial assessing ivermectin and diethylcarbamazine, 1984. Ivermectin has been a game-changer in the treatment of onchocerciasis; the discoverers received the 2015 Nobel prize.
Another important public health initiative stemmed from identifying cigarette smoking as a risk factor for age-related macular degeneration (AMD). We began a public health campaign alerting people to the fact that blindness is one of the many complications of cigarette smoking, and this has been effective in curbing smoking rates, now used in many parts of the world.
CROSSOVER IN PRACTICE
Although these efforts have taken me to many places around the world, they have enormous relevance to ophthalmic practice at home as well. There is a great deal of crossover between this work in underserved populations and office- or hospital-based practice in the developed world, and my work has afforded me certain lessons.

I now think beyond the four walls of my office. For one thing, working in eye camps or refugee situations opens one’s eyes to broader issues in providing access to health care. Patients may face difficulties in accessing care or caring for themselves, whether it is a matter of arranging transportation to get to the clinic or finding someone to look after them at home or help them put drops in their eyes.

I take precautions to ensure that patients do not fall through the cracks. Particularly in terms of health service delivery, you learn in underserved areas that it is vital to have people working efficiently and effectively to make sure that patients do not fall through the cracks. At home, then, you can start to apply some of those same principles. How do I organize my office more effectively? How do I make my outreach service work better?
WORK AT HOME AND ABROAD
I stepped down as Chairman of the Department of Ophthalmology at the University of Melbourne and as Director of the Centre for Eye Research Australia about 8 years ago. I have stopped doing clinical work, and I focus full time on trying to ensure that proper eye care services are provided to the Australian Aboriginal people. In many cases, the same principles can then also be used to improve the provision of eye care to the rest of the Australian population.
The effort to close the gap in vision care for the Australian Aboriginal people is a significant challenge, but we are making progress. When we started this work in 2008, Aboriginal people had six times the rate of blindness of other Australians. In 2016, we halved the gap, and the gap continues to close today. Similarly, trachoma in Aboriginal children has been reduced from 21% in 2008 to 4.6% in 2015. We are making good progress, but there is still a way to go.
My other job at present is as President of the ICO. This takes a good amount of time, with many international trips per year, but it is worthwhile as the organization is doing some very important work, in my opinion. The ICO has some 150 member societies around the world, representing the 205,000 ophthalmologists worldwide. Its focus is on improving skills and abilities for ophthalmologists to be able to provide high-quality eye care and leadership.
During my term as President, I hope to work to expand the relevance and use of the ICO’s education and leadership programs and to improve the efficacy of the work that the ICO does.
My other goal is to help complete the implementation of the WHO’s Universal Eye Health, A Global Action Plan 2014-2019.2 The aim of the plan is to reduce avoidable visual impairment as a global public health problem and to improve access to rehabilitation services for the visually impaired in all countries around the world. The results are to be reported back to the WHO in 2019.
NEVER A BETTER TIME
We all come into medicine or ophthalmology to try to help people and to leave the world a better place. We can do that by treating patients one at a time, or we can do it by performing research to understand how to treat people better or to prevent or cure diseases better. And when we apply that research and see it put into action, that can have significant effects. It is satisfying to be able to see the difference one can make in people’s lives by helping them keep their vision or restoring vision when it is lost.
The sort of work I have devoted my career to does not suit everyone—that is fine. But I think what we all need to do is to think globally and act locally. What can I do in my own community, in my own practice, my hospital, or wherever, to make sure that we are reaching the underserved and needy people? Are we examining everyone with diabetes on a regular basis? Are we making sure everyone who needs cataract surgery is getting it? Is everyone getting the eye examinations and glasses they require?
We know untreated blindness is a global issue, and there is a lot of blindness in the world, but each of us can say, “What can I do in my clinic, my community, or my corner of the world to make a difference to those people who would not otherwise get service?” If we all do this, we can all leave the world a better place.
Today we hear a lot of people say, “Medicine is getting so tough; ophthalmology is so hard. The reimbursements are too low, and the restrictions are too heavy.” But, actually, I believe there has never been a better time to be an ophthalmologist. There has never been a time when we can do so much to help people keep their good vision or to restore vision to those who might have lost it. What we can do today is quite extraordinary. And what we need to do is try to make sure that everyone benefits from these great advances in prevention and treatment.
1. Prevention of Blindness and Visual Impairment: Trachoma. World Health Organization. http://www.who.int/blindness/causes/trachoma/en/. Accessed April 3, 2017.
2. Universal Eye Health: A Global Action Plan 2014-2019. World Health Organization. 2013. http://www.who.int/blindness/AP2014_19_English.pdf?ua=1. Accessed April 3, 2017.


