Case Presentation
A 76-year-old woman presented with reduced visual acuity and increased glare over the past year. On slit-lamp examination, she had 1+ cornea guttata with 1 to 2+ nuclear sclerotic and 1 to 2+ posterior subcapsular cataracts in each eye. Her manifest refraction was +8.00 -3.50 X 126° = 20/40 OD and +4.25 -3.00 X 5° = 20/40 OS.
Biometry measurements in her right eye on the IOLMaster (Carl Zeiss Meditec) were as follows: axial length, 21.78 mm; keratometry (K) readings, 41.41 X 44.47 D @ 80°; anterior chamber depth, 2.83 mm; white-to-white distance, 12.3 mm. Simulated Ks on Atlas (Carl Zeiss Meditec) topography were 40.83 X 44.13 @ 80°.
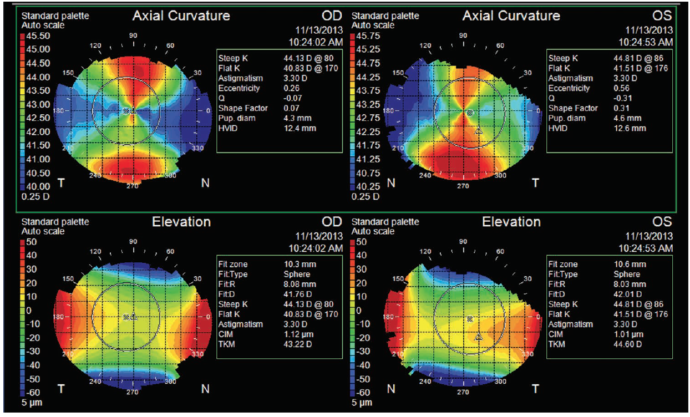
Figure 1. On corneal topography, significant astigmatism was apparent.
When I discussed the need for cataract surgery with the patient, she expressed a desire for spectacle independence. Because of her significant astigmatism (Figure 1), I recommended the use of a toric IOL, to which the patient agreed. Figure 2 shows an enhanced pupil image from the Atlas, with the astigmatic axis from 80° to 260° labeled. Surgery was scheduled for the patient’s right eye first, with the left eye to follow 2 weeks later.
For her right eye, I aimed for plano with a 29.00 D IOL with 4.00 D cylinder power (Tecnis Toric ZCT400; Abbott), to be implanted at an axis of 80º. For toric IOL implantations, my surgical technique is similar to that with a standard nontoric IOL, with special attention paid to creating a self-sealing wound and a well-sized and well-centered capsulorrhexis. Additionally, I mark the eye with reference to the pupil image (Figure 2). I also like to spin the toric IOL several times in the bag in order to polish the capsule, to remove any residual OVD, and to seat the lens firmly on the posterior capsule. Then I seal the wound well with careful hydration.
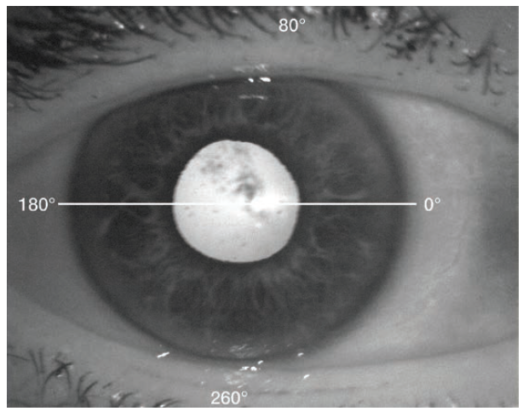
Figure 2. Enhanced pupil image: The astigmatic axis is labeled from 80º to 260º.
On postoperative day 1, the patent’s UDVA was 20/80 OD, and her manifest refraction was +1.00 -1.75 X 139° = 20/40. At the slit lamp, 1+ corneal edema was evident, and some capsular striae could be seen at about 170°. On dilation, the IOL axis was positioned at 117°.
By postoperative day 11, the patient’s UDVA decreased to 20/200, and her refraction was +1.75 -3.25 X 145° = 20/25. The cornea was clear, and the IOL was positioned at 119°, almost 40° from the intended axis (Figure 3).
My questions to the contestants include the following:
- Was the IOL positioned wrong, or did it rotate?
- What would you do to address the error?

Figure 3. IOL position at day 11 postoperative was almost 40º from the intended axis.

Contestant No. 1
For me, I think the most common reason for a postoperative rotational error with a toric IOL is that I made my marks at 0° and 180° a little bit off. When that happens, the eye ends up slightly torted during surgery—although it looks like I have it absolutely right. Later, when I am watching my video of the surgery, I confirm that the lens was placed well but my markings were actually 5° to 10° off target. Your result here, Daniel, was 40° degrees off; maybe you were a little bit off with your marking plus a little bit more off because of the torsion of the eye.
In terms of a lens rotating on its own, the two biggest potential causes, in my experience, are leaving residual OVD behind the IOL and having a patient who rubs his or her eye.
Before I did anything to address the error, I would recommend waiting until the patient’s 2-week visit to see how satisfied she is. The common wisdom is that, with every 1° the toric IOL is off the target axis, 3.3% of the desired astigmatic effect is lost. When the IOL is just 15° off, you lose about 50% of your intended cylinder power. But if the patient is joyously happy to be seeing better, with less astigmatism, then I probably would not do anything. If the patient is not happy, I would rotate the lens.

Contestant No. 2
I find it important to take into account the astigmatism on the posterior corneal surface, Daniel, and I have experienced some refractive surprises when I have not done this. Diagnostic devices that can help to avoid problems include the OPD Scan III corneal analyzer (Nidek) and the KR-1W Wavefront Analyzer (Topcon). These technologies allow you to measure corneal and internal astigmatism and to determine exactly where the error is, in the eye or on the corneal surface. Postoperatively, these devices provide useful information regarding where to rotate the IOL to fix the residual astigmatism.
Further, to ensure proper placement in toric IOL cases, I always use intraoperative aberrometry. I find it extremely useful in identifying a potential surprise, and then I can rotate the lens during surgery and put it in the right position, rather than having to go back later.
In every premium IOL case—toric and multifocal—I use a capsular tension ring (CTR). This way, if I have a problem, even years later, I can easily open the capsule and take the lens out. Additionally, with use of a CTR, I have seen less IOL tilt, as well as less rotation of toric IOLs. The IOL is much more stable than without a CTR; although the lens can still rotate, it is unusual.
Some newer toric IOLs are being designed with features to prevent rotation. The Ankoris toric IOL (PhysIOL) has four haptics, and the texture of the haptics is a bit rough, which makes the IOL extremely stable. In a large series of eyes with 1-year follow-up, the IOL did not rotate more than 5° (personal data).
Regardless of the technologies and the IOLs that a surgeon uses, if rotation or misalignment does occur, it is not difficult to go back into surgery and dial the lens into the right position. But, of course, it comes with the burden of explaining to the patient that you did not do a perfect job the first time and that you need to go back to the operating room. With the second surgery also comes the added risk of infection and endophthalmitis.

Contestant No. 3
I see a lot of patients for consultations to fix toric IOL problems like this. I find that the No. 1 problem in these cases is that the initial measurement of the axis was wrong. Most often, this occurs because the patient had dry eye that was left untreated. I look at the earlier topography, treat the patient’s dry eye, and then, on subsequent topography, the axis of astigmatism adjusts to where it should have been originally. The take-home message here is that you will miss the target if the astigmatism was corrected based on an abnormal topography.
Daniel, I would advise against your practice of rotating the IOL beyond the target axis. Before you started the rotation, you had accomplished 95% of your goal. By rotating your IOL another 180°, you put yourself in a dangerous position. If you rotate 90° off your intended toric axis and for whatever reason the capsule ruptures at that point, you are in trouble. I would encourage you not to rotate past your target; just go where you need to and stop.
Another habit that is good to get into is, at the end of surgery, after you are finished touching the eye, take your hands away and look at the axis one more time. Often, surgeons will check the axis and then hydrate the wound one more time; that is when they get a little slip of the axis, and they do not notice it. It is helpful to get into the routine of pulling your hands away and looking again, just to make sure the IOL is where you thought it was.

Contestant No. 4
One question is this: How soon does one go back in to reposition a malpositioned toric IOL? Given that this patient has a little bit of corneal edema, you really have to account for how much the wound is contributing to the new axis of astigmatism, Daniel. I typically wait several days. I tell the patient, “We are going to go back in and adjust, but we have to let things settle down first.”
I have a minor procedure room in my office, which, if this were my patient, is where I would have performed the IOL rotation procedure once the eye settled down. I would not use an OVD but rather go into the eye through the paracentesis with a 27-gauge cannula filled with balanced saline solution, and use the cannula to nudge the IOL into the proper position. I have found this works pretty well to re-rotate toric IOLs. If the procedure is done within the first couple of weeks after the primary surgery, the paracentesis will open pretty easily. I usually identify the misalignment at the follow-up on day 1 and then do the adjustment on day 7 postoperative because that is my next day in the operating room.

Contestant No. 5
In this case, with about a 40º miss, I think the lens probably rotated after the patient left the OR for whatever reason, Daniel. In other cases, a lot of little errors can add up to a relatively big one. The original orientation marks might be off a bit, and the steep meridian marks might be off slightly too.
There is another phenomenon that I believe sometimes occurs, in which the surgeon dials the lens clockwise to the desired axis, but, unknowingly, slightly torques the bag and the zonules. Later, the lens and the bag rotate back to their natural neutral positions, which is counterclockwise from where the surgeon left it. This could easily cause a rotation of 10º.
Another potential factor is that, sometimes, after surgeons get the IOL dialed in just where they think it should be, they shift their attention from the lens’ orientation to the wound. My comment here echoes what Contestant No. 3 said: that we should all back out of the eye and look at the axis one last time before hydrating the wound.
The Resolution
Here are a few responses to the contestants’ remarks before I describe the outcome of this case.
First, I agree with Contestant No. 1 about waiting to see if the patient is satisfied with his or her result. We do not treat the numbers, we treat the patient. I also liked his comment about making sure the patient does not rub her eye. I think eye rubbing plays a major role in IOL rotation. If there is postoperative hypotony, the force of rubbing can be transmitted to the sloped haptic of the IOL, thus inducing a counter-clockwise rotation. By focusing on creating and sealing the wound well, hypotony can be prevented.
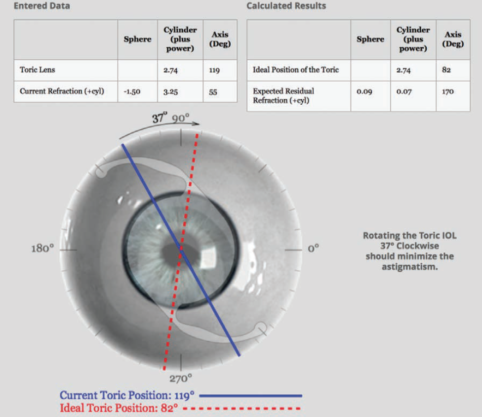
Figure 4. The Toric Results Analyzer suggested rotating the IOL to 82º.
Contestant No. 2 makes some great points regarding posterior corneal curvature, and the technology to measure it continues to improve. To help with rotational stability, the use of CTRs can be a great way to stabilize the IOL and has anecdotally been shown to prevent rotation.
Regarding Contestant No. 3’s comment about dry eye distorting topography, I routinely perform repeated IOLMaster readings and compare them with topography to make sure all the numbers match up. Repeating biometry measurements helps to establish consistency. As Contestant No. 5 also points out, it is important to be meticulous all the way to the end of the case, even when hydrating the wound. While I do not routinely do so, some surgeons even advocate checking the eye after removing the eyelid speculum.
Timing of repositioning is important, both from an operative ease and safety standpoint and from a patient experience standpoint, as well-explained by Contestant No. 4. Thankfully, rotating an IOL within the first few weeks of surgery is typically easy.
ADVICE FROM THE PEANUT GALLERY
I do not place a capsular tension ring (CTR) in primary surgery unless I see something unusual about the case. Regarding placing a CTR at the time of a secondary surgery, for me, it depends on how far out I am from the original surgery. One-piece IOLs are easy to remove, and I have taken them out more than a year after surgery fairly easily. I am much more likely to use a CTR if it has been more than a year since the original surgery. In those cases, there is more strain on the zonules as the lens is removed. I like to gauge this during the surgery and judge how the zonules are reacting. If it has been more than 1 year, I do like to use a CTR.
—Rosa Braga-Mele, MD, Med, FRCSC Director, Cataract Unit, Mount Sinai Hospital Associate Professor, University of Toronto, Canada Director of Research,
Kensington Eye Institute, Toronto, Canada; rbragamele@rogers.com
So, what do I do now? At 1 week postoperative, with a 40° misalignment, it was pretty obvious that I had to go back in and rotate the lens. The patient had decreased visual acuity, and she was unhappy with it. Overall, I find that significant axis alignment errors occur at a rate of around 1%, but patients are sometimes still happy with their results. Of the roughly 300 Tecnis Toric IOLs that I have implanted, this is the only case that I have had to reposition. If the patient is happy postoperatively, I do not intervene.
The patient was scheduled for her second eye surgery 2 weeks after the first, so I told her that we would simply use that time to realign her IOL. My ambulatory surgery center is adjacent to my office, so it is easy for patients to return to the operating room.
In preparing for the repositioning surgery, I consulted the Toric Results Analyzer (astigmatismfix.com; Figure 4) developed by John P. Berdahl, MD, and David R. Hardten, MD. One reason I use that tool is to confirm that the poor refractive result is primarily due to the rotational position of the IOL. The site asks users to enter the IOL power, the postoperative refraction, the current IOL axis, and other information. The program responds with the ideal IOL position and the expected residual astigmatism. In this case, it tells me that if I rotate the IOL back to 82°, the eye will be left with less than 0.10 D astigmatism. Since that is close to my original calculation of 80°, posterior astigmatism does not appear to have been an issue here, and it was clearly a case of malpositioning.
For the reintervention surgery, I marked the target axis of 82° as 37° clockwise from the current IOL axis, rather than remeasuring and registering 0° and 180°. It was less than 2 weeks after the initial surgery, so I used blunt dissection to open the wound. I opened the paracentesis port with a cannula and used OVD under the capsular rim to dissect the capsule open. I was able to free the lens easily and rotate it.
On day 1 after the repositioning, the patient’s UDVA was 20/30. Capsular striae could be seen at 135°. I did not dilate the eye because the patient was doing well. Four days later, I operated on her left eye. At postoperative week 6, UDVA was 20/20 in her right eye and 20/25 in her left, and the patient was doing well and happy.
AND THE WINNER IS...
All contestants made great comments on the mechanism, prevention, and treatment of toric IOL malpositioning. However, based on his comments on the importance of good biometry and good surgical technique, the winner is Contestant No. 3.
GET TO KNOW THE CONTESTANTS

Contestant No. 1
Geoffrey Tabin, MD
• Professor of Surgery and Medicine, Moran Eye Center, University of Utah
• Codirector, Himalayan Cataract Project, Waterbury, Vermont
• Geoffrey.Tabin@hsc.utah.edu
• Financial disclosure: None acknowledged

Contestant No. 2
Erik L. Mertens, MD, FEBOphth
• Medical Director, Medipolis, Antwerp, Belgium
• Chief Medical Editor, CRST Europe
• e.mertens@medipolis.be
• Financial disclosure: Consultant (STAAR Surgical)

WINNER
Contestant No. 3
Kevin L. Waltz, OD, MD
• Adjunct Clinical Professor, Indiana University School of Optometry, Indiana
• TLC Laser Eye Centers, Indianapolis, Indiana
• klwaltz@aol.com
• Financial disclosure: None acknowledged

Contestant No. 4
John A. Vukich, MD
• Surgical Director, Davis Duehr Dean Center for Refractive Surgery, Madison, Wisconsin
• javukich@gmail.com
• Financial disclosure: Consultant (Abbott)

Contestant No. 5
Steven J. Dell, MD
• Director of Refractive and Corneal Surgery, Dell Laser Consultants, Austin, Texas
• Member, CRST Europe Global Advisory Board
• +1 512 327 7000
• Financial disclosure: None acknowledged



