Case Presentation

A patient with a history of corneal scarring from previous corneal infections expressed interest in laser vision correction (LVC). He was the 22-year-old son of a prominent family in my community, and I would describe the whole family as having intense personalities. I would also describe this patient as a contact-lens abuser who was unable to comply with a lens care regimen.
He had irregular corneas due to corneal ulcers in both eyes 4 years before the current encounter.
On examination, the patient’s right eye had peripheral corneal scarring that did not affect vision. In his left eye, the scarring caused irregular astigmatism. CDVA in this eye was 20/30-3. He has bad allergies that were making him no longer able to deal with his contact lenses, but he did not like spectacle correction, either. He said, and I quote, “Glasses are really cramping my style, dude.” The refraction in his left eye was -2.00 -1.50 X 22º.
It should be said that, despite the poor CDVA in the patient’s left eye, when he could tolerate a contact lens he could be refracted to 20/30, and his fellow eye could be corrected to 20/20. So, on his best days, he had reasonably good vision with those lenses. Most of the time, however, he could not wear them.
Our team spent a long time trying to optimize the patient’s ocular surface, including performing cutaneous allergy testing to try to get his severe allergies under control. When his ocular surface was as healthy as we could make it, I had a long discussion with the patient about the potential for LVC in his left eye, including frank discussion of the risks and expectations.
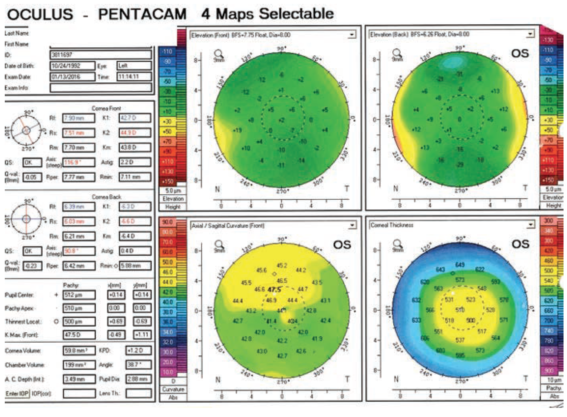
Figure 1. Preoperative topography in the patient’s left eye, with the thickness map (lower right) indicating a fairly thin cornea.
At the end of that conversation, the patient said that he understood the risks of the procedure and that he was willing to accept them. I felt pretty confident about attempting treatment, despite his highly irregular cornea.
Figure 1 shows the preoperative Pentacam (Oculus) maps of his left eye. The thickness map (lower right) shows that he had a fairly thin cornea, 510 µm centrally, with tissue loss inferotemporally and some thickening superiorly due to the scarring. There is considerable variation in curvature, with changes of several diopters in keratometry (K) within the space of a millimeter. There had been multiple ulcers, and the scarring was relatively anterior, within the anterior third of the cornea.
Contestants, please comment on the following aspects of this case:
- What additional diagnostic information would you want before proceeding with treatment in this patient?
- What mode of treatment would you offer this patient?

Contestant No. 1
This is the kind of patient that I see relatively commonly in my refractive practice, and that is a patient population that may have a history of contact lens abuse. These patients may have had some sort of mild corneal ulcers in the past, leading to unusual corneal topographies. If this were my patient, Steven, I would want to look at anterior segment OCT and epithelial thickness, and I would want to see how deep the scarring is before I decided on a treatment plan. The scarring can be assessed clinically as well, but it helps to have the OCT confirm that it is truly anterior.
One option in a patient like this is PRK, but only if I am able to obtain a wavefront reading. PRK may help with his superficial scarring as well as the refractive error. If I was unable to obtain a wavefront reading in an irregular cornea like this, PTK can be helpful to smooth the cornea and address the superficial scarring. Then a wavefront can be attempted several months later with plans for PRK.

Contestant No. 2
Regarding additional diagnostic information, the Holladay equivalent K reading (EKR65) on the Pentacam is helpful to evaluate the large spread of Ks as seen in this patient. The EKR65 metric will tip you off that an eye like this will be a difficult treatment. I would also want to see what the objective scatter index (OSI) is on the HD Analyzer (Visiometrics). I can predict from what you have shown, Steven, that the OSI would be high in this eye, increasing the risk of postoperative glare and halos. However, there are still some options to be discussed.
With this patient’s refraction, there is room to do a two-step procedure. I would do a 50-µm PTK to smooth out the cornea, and, at the same time, add 1.00 D of myopia to make sure I did not create a central island. I have had a disastrous outcome trying to do a straight-through 60-µm PTK, causing a 4.00 D dome in the center of the cornea that I had to fix later. Do not go straight through with a deep PTK because of the risk for a big central island defect.
I have tried to treat irregular eyes like the case you described, Steven, with a first-generation wavefront-guided system, and it did not work. However, over the past year, I have been successful with the iDesign Advanced WaveScan System (Abbott). Based on my experience with this system, I recommend adding a little plus offset; I typically use 0.60 D, although the amount should be chosen conservatively. Even with that, an overcorrection of about 0.50 D is still possible. I do not like shifting patients into hyperopia because it is difficult to correct with a retreatment. If I leave the eye with a little bit of myopia, I can always come back and treat again.

Contestant No. 3
I agree with Contestant No. 1’s comment. It seems like there no longer are any normal refractive patients coming into the office. Either we have done all the normal corneas or these patients do not want to have surgery. So many patients now require us to figure out how to treat them. Do we even want to treat them? Do we want the potential problems?
In this patient, given what you have told us, Steven, it seems there is a good chance you can do something for him that would be much better than what he was expecting after your extensive counseling. The bar is not set very high, in other words. Given that, I agree with you that I would feel fairly confident going forward to try to find a solution for him.
Regarding the surgical approach, I have not seen this eye at the slit lamp, but I would be concerned about trying to make a femtosecond laser flap. If there is scar tissue, flap creation could be a problem. That would probably take LASIK off the table for me, and I would be looking only at surface treatment for him.
For a refractive target, I would want to go a bit hyperopic. A young person like this has a long way to go before that slight hyperopia becomes an issue—another 20 years really. A little bit of hyperopic shift would probably give the patient the best visual result for the time being.

Contestant No. 4
I would want to look at epithelial thickness maps for this patient because, on the maps you showed us (Figure 1), Steven, the corneal curvature change does not match the corneal pachymetry. The bottom left map, which shows the curvature of the anterior corneal surface, does not match the bottom right corneal pachymetry map. This tells me that the eye could have a stromal irregularity, Bowman membrane scarring, or, perhaps, a macropannus creating scarring in the cornea. In addition to Pentacam imaging, I would want to see a Placido-disc topography, because the Scheimpflug image could be distorted by a slight opacity in Bowman membrane. Alternatively, the irregularity could be epithelial.
In my opinion, this is a no-brainer for topography-guided treatment. I would do PRK in lieu of the fact that the patient probably has a irregular epithelium trying to mask this stromal irregularity.

Contestant No. 5
A. John Kanellopoulos, MD, taught me never to do surgery on an eye, whether it is cataract surgery or laser refractive surgery, without looking at an epithelial map. I agree that it gives us valuable information.
My preferred refractive surgery approach is to implant a phakic IOL, specifically the Evo Visian ICL (STAAR Surgical). However, obviously with a cornea like this patient’s, the irregularity cannot be treated with an ICL. In this case, I would also opt for topography-guided PRK.
One other comment that I would like to make, Steven: The index of height decentration, which is on the topometric data on the Pentacam, correlates directly with the contrast sensitivity and OSI on the HD Analyzer. This can be a cheap way to indicate how vision improves (or does not improve) postoperatively.
THE RESOLUTION
I elected to treat this patient’s left eye with wavefront-guided surface ablation on the iDesign laser. I applied mitomycin-C for 30 seconds. Before I discuss the results, a couple of points are worth making.
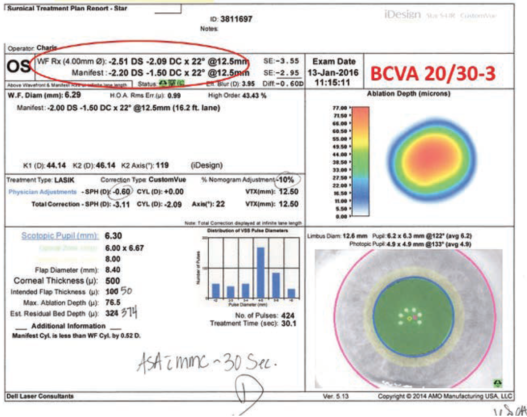
Figure 2. Treatment planning screen: The best possible postoperative refraction agreed with the wavefront refraction (red circle).
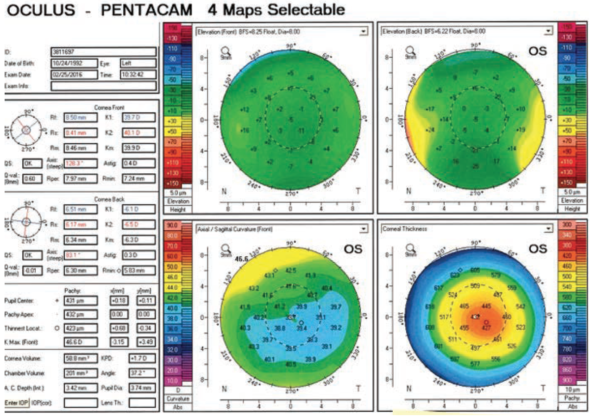
Figure 3. Postoperatively, the patient achieved a more regular corneal surface.
Contestant No. 2 mentioned using an offset with the iDesign, and we do the same. After a learning period, we now use an offset of about 0.50 D more than the manifest refraction, and that generally gives us a plano result. For this patient, we did what I would call an age-related myopic adjustment. For patients this age (he was 22 years old), I like to leave them hyperopic by about 0.40 D. I thought it would be good for him to have some low-grade accommodative stimulus and to keep his pupil a little smaller at night.
Pupil size is actually important in younger patients. As the pupil shrinks in size by 50%, there is a 16-fold reduction in higher-order aberrations (HOAs), which can be beneficial in cases such as this one. Pupil size can be manipulated pharmacologically as well. In patients who are severely debilitated by an irregular cornea, a relatively modest change in pupil size can make a dramatic impact in reducing their HOAs.
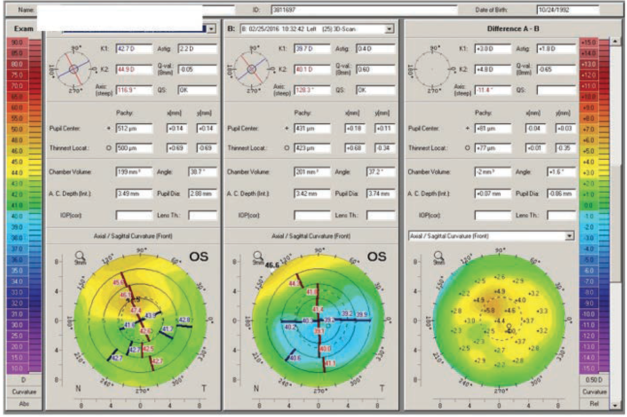
Figure 4. Pre- (left) and postoperative (center) topography and the topographical difference map (right).
Figure 5. The patient’s testimonial, posted to the Dell Laser Consultants Facebook page.
Figure 2 shows the treatment planning screen for the iDesign wavefront-guided treatment. The important thing to note in this case is that the best refraction we could get for this patient agreed reasonably with the wavefront refraction (red circle). This is a crucial point. If there is a disagreement, especially an astigmatic disagreement, between refraction and wavefront, I would not recommend treating that patient with a wavefront-guided treatment, even with an advanced program. There was excellent correlation in this eye between the manifest refraction and the wavefront reading.
Figure 3 shows the postoperative result, a much more regular corneal surface than I expected. Frankly, with the CustomVue software that we had been using previously, we would not have been able to achieve results like this. The higher resolution, the greater density of the Hartmann-Shack array, the greater fidelity, and the wider dynamic range of the iDesign means that we can actually treat these eyes. Figure 4 shows the difference map (right hand image). I was stunned by the result in this case—how incredibly uniform the topography ended up postoperatively.
I performed surface ablation in the patient’s right eye as well. There was some scarring in the periphery in this eye, but it was in better shape than the left. I could have done LASIK, but I decided to use the same approach in both eyes to keep the postoperative regimen simple.
This young man is now 20/15 UDVA in each eye, a phenomenal and unexpected result. The patient was so pleased that he wrote a review on our practice’s Facebook page telling the world how happy he was with the result (Figure 5). This turned out to be a great case for the patient and for our practice. This well-connected individual in our community got a happy ending, and we got a powerful testimonial on social media.
AND THE WINNER IS...
All contestants provided excellent responses, and so we really have a five-way tie for the winning response. But, if I am forced to pick a single winner, I would give the edge to Contestant No. 3 for recognizing the useful role of leaving a bit of hyperopia in an irregular cornea in a young person.
GET TO KNOW THE CONTESTANTS

Contestant No. 1
Sumitra S. Khandelwal, MD
• Assistant Professor of Ophthalmology, Baylor College of Medicine, Houston
• Resident and corneal fellow trainee, Michael E. DeBakey Veterans Affairs Medical Center and Ben Taub General Hospital, Houston
• skhandel@bcm.edu
• Financial disclosure: None acknowledged

Contestant No. 2
James C. Loden, MD
• President, Loden Vision Centers, Nashville, Tennessee
• lodenmd@lodenvision.com
• Financial disclosure: None acknowledged

WINNER
Contestant No. 3
Mark Kontos, MD
• Senior Partner, Empire Eye Physicians, Spokane, Washington, and Coeur d’Alene and Hayden, Idaho
• mkontos58@gmail.com
• Financial disclosure: None acknowledged

Contestant No. 4
A. John Kanellopoulos, MD
• Medical Director, The Laservision.gr Research & Clinical Eye Institute, Athens, Greece
• Clinical Professor of Ophthalmology, NYU Medical School, New York
• Associate Chief Medical Editor, CRST Europe
• ajkmd@mac.com
• Financial disclosure: None acknowledged

Contestant No. 5
Erik L. Mertens, MD, FEBOphth
• Medical Director, Medipolis, Antwerp, Belgium
• Chief Medical Editor, CRST Europe
• e.mertens@medipolis.be
• Financial disclosure: Consultant (STAAR Surgical)



