The FineVision HP (PhysIOL) is a new trifocal aspheric, diffractive IOL, similar to the company’s FineVision trifocal but made with a hydrophobic rather than hydrophilic material. The hydrophilic FineVision IOL has been successful in certain markets, but, in other territories, notably in the United States, surgeons prefer hydrophobic materials. The company developed this version to allow surgeons to have a choice of materials.
In the first series of patients to receive the lens, the FineVision HP was implanted in one eye and its hydrophilic sister lens in the other. From the patients’ perspectives, as well as from objective measurements, there were no significant differences between the two. By 1-month postoperative, 100% of eyes achieved J1 UNVA, and, at 3 months, 100% of patients achieved 20/20 CDVA. These data were presented at the 2016 European Society of Cataract and Refractive Surgeons (ESCRS) meeting in Copenhagen.1
AT A GLANCE
• The FineVision HP is similar to the FineVision trifocal but made with a hydrophobic rather than hydrophilic material.
• The lens’ haptics have waves on the surface that reduce their stickiness and help them separate in the eye after injection without manipulation.
DESIGN INNOVATIONS
The one-piece hydrophobic FineVision HP is a true microincision implant; just like the hydrophilic FineVision, the lens is implantable through a 1.8-mm incision in powers up to about 28.00 D. The glistening-free material is less yellow than other blue light–filtering lenses, such as the AcrySof Restor IOL (Alcon).
The haptic configuration of the hydrophobic lens is different from that of the hydrophilic FineVision IOL. The haptics feature what the company calls Wavetech technology, with waves on the surface of the haptics that reduce their stickiness and help them separate in the eye after injection without manipulation (see image in The Lens). It is highly likely that posterior capsular opacification is reduced with this lens, but that has not been demonstrated yet because follow-up is too short.
FAVORITE LENS
The trifocals from PhysIOL, both hydrophilic and hydrophobic, are my favorite lenses at present, and more than 80% of my patients receive them. Typically, these are patients who want to be spectacle independent, and, because trifocal lenses provide good distance, intermediate, and near vision, most typical patients can be satisfied with this solution (Figure 1). These are patients who live ordinary lives: office workers and those who require good vision for a variety of activities in daily life, including driving, computer use, and reading. The FineVision HP, like its sister lens, can be used in cataract surgery and in refractive lens exchange for hyperopic patients over 40 years of age.

Figure 1. Optical simulation of near, intermediate, and distance vision using Fourier optics and the Helmholtz equation.
There are some relative contraindications. As with all multifocal technologies, I am careful to avoid people with type A personalities or unstable personality traits. And, for someone who drives extensively at night, a trifocal lens may not be the best option. However, for typical drivers who spend most of their time driving in the daytime and only sometimes at night, I do not hesitate to implant these lenses.
I have implanted more than 6,000 trifocal lenses in total, and my experience is that, in general, patients adapt quite quickly to trifocal vision. This is even true in my early experience with the FineVision HP.

One key to my success with this lens is that I schedule surgery in both eyes close together—the next day or even the same day—and spend time educating patients preoperatively about what to expect. Patients are told that they will need time to adapt, which might take from a few weeks up to a few months, and they are also informed about the possibility of halos and glare at night from the headlights of oncoming cars and other light sources. Patients must also understand the possible need for laser fine-tuning to achieve emmetropia, which I typically do with PRK at about 2 to 3 months after implantation.
Additionally, my staff and I commit to spending more chair time with these patients postoperatively, so that they can tell us about their halos and glare and other issues. We spend the time with them and offer them guidance to get through the adaptation. With that effort and time, we are able to make the great majority of patients happy in the end.
implanted IN A FELLOW SURGEON
Just the other day, I got an email from a local orthopedic surgeon in whom I had implanted the FineVision HP. Like us eye surgeons, he works a lot with a microscope. He was hesitant to choose a trifocal technology because of the possibility of halos and glare interfering with his use of the microscope. After much discussion, however, he decided to proceed with the FineVision HP.
The Lens: FineVision HP
PHYSIOL
• Proven trifocal IOL technology in a glistening-free hydrophobic material
• Double C-loop haptics with Wavetech technology to facilitate implantation
• Overall length 11.4 mm; optic diameter 6 mm
• Physiologic chromatic aberration optical performance
• Three focal points to achieve good near (3.50 D), intermediate (1.75 D), and distance vision
• Available in powers from 10.00 to 30.00 D; in summer 2017, it will be available from 6.00 to 35.00 D
For more information: http://www.physiol.eu/en/multifocal-iol/finevision/
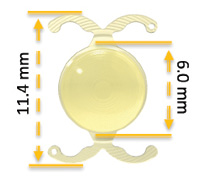
Courtesy of PhysIOL
He told me in his email that he has no problems with the microscope, and he sees almost no halos and glare at night.
POINTERS AND PEARLS
It is well-known that, with trifocal IOLs specifically and multifocal IOLs in general, we need to achieve emmetropia to deliver the spectacle independence that patients desire. Surprisingly often, I hear surgeons say that astigmatism is a contraindication for a trifocal implant. This is not true, and it has never been so at our clinics. The caveat is this: We must target that astigmatism and compensate for it as part of our surgical plan.
I use fewer toric IOLs than many surgeons. I perform the cataract incision on the steep radius, and I enlarge the incision up to 2.5 mm to treat up to 2.50 D cylinder. For higher amounts of cylinder, from 2.50 to 3.00 D, I use laser arcuate keratotomy with the Victus femtosecond laser (Technolas Perfect Vision, a Bausch + Lomb company). I use a toric implant only for astigmatism higher than 3.00 D.
There is a toric version of the FineVision hydrophilic IOL (FineVision Toric), and its hydrophobic toric sister lens (FineVision HP Toric) is expected to be available by the end of 2017.
Another pointer I recommend with trifocal IOLs is to use a capsular tension ring (CTR) in every eye. These are premium lenses and premium patients, and, if a trifocal implant becomes tilted or decentered by capsular fibrosis or phimosis, it can be difficult to make the patient happy. With a CTR in place, the lens is stabilized and long-term centration is ensured.
CONCLUSION
From my point of view, the FineVision HP is the most advanced implant for microincision surgery. It delivers spectacle freedom to almost all patients at near, intermediate, and far.
I have been using this lens recently with the CapsuLaser (CapsuLaser), the microscope-mounted thermal laser that makes fast, cost-efficient circular capsulotomies. So, for 2017, my favorite surgical combination is going to be the CapsuLaser capsulotomy with implantation of the FineVision HP IOL.
1. Stodulka P. First clinical outcomes with new hydrophobic trifocal IOL FineVision Evo. Paper presented at: European Society of Cataract and Refractive Surgeons Annual Meeting; September 10-14, 2016; Copenhagen, Denmark.



