When the Universal Declaration of Human Rights was proclaimed by the United Nations General Assembly in 1948, it set the stage for an era of universal protection of fundamental human rights. Among the rights listed in the declaration is Article 25, which reads in part, “Everyone has the right to a standard of living adequate for the health and well-being of himself and of his family, including food, clothing, housing, and medical care and necessary social services.”1
The language of Article 25, like that of other articles in the declaration, leaves much open to interpretation. In the modern day, should laser vision correction (LVC) be included as a fundamental human right? The Refractive Surgery Alliance (RSA) argues that it should.
In a press release issued by the RSA in December 2015, Richard A. Norden, MD, FACS, said, “Refractive errors limit safety, lifestyle, and occupational fitness. People who wear glasses are at a competitive disadvantage. [LVC] technology is so good and the economics are so compelling that every suitable candidate should have their vision corrected.”
Also included in the press release were two intriguing statistics: 62.6% of refractive surgeons who responded to a 22-question global survey on refractive surgery and were candidates for refractive surgery have had their vision corrected, and more than 91% of respondents recommended refractive surgery for their immediate family members. These and other statistics were reported in a study published late last year.2
FOUR TIMES MORE LIKELY
The online survey was emailed to 250 randomly selected practicing refractive surgeons in order to establish the prevalence of undergoing LVC among this population. The secondary objective was to characterize attitudes and satisfaction rates among the respondents who had undergone LVC.
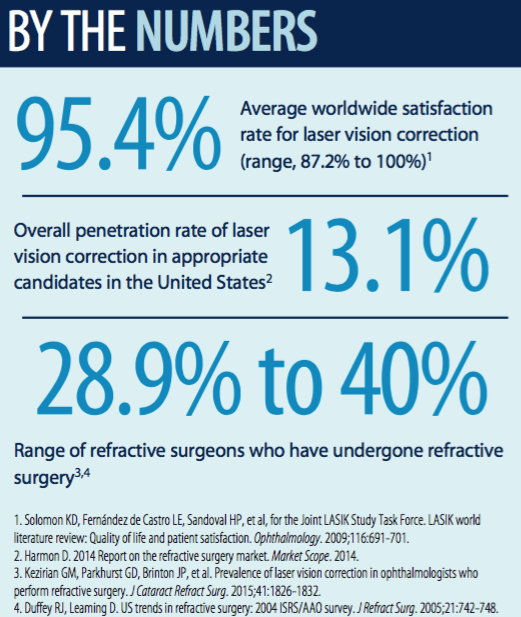
All but two surgeons participated in the survey, and 232 met the study criteria. Of the 107 respondents who answered that they were candidates for LVC, 67 reported that they had undergone LVC in their own eyes. Of these, 65.7% had undergone LASIK and 34.3% had undergone PRK. The reasons for not undergoing LVC in the other 40 respondents are listed in Table 1.
The authors concluded that refractive surgeons are more than four times more likely to have had refractive surgery than the general population. Among the surgeons who had undergone LVC, 65 of 67 answered that they were “better off for having had corneal laser refractive surgery.” Additionally, 55 said they were completely satisfied with their results, 10 that they were mostly satisfied, one was neutral, and one was completely dissatisfied.
When asked if they would recommend LVC to adult members of their immediate family who are candidates and can afford to have it, 211 of the 214 who responded said that they do whenever possible (n = 185) or only in selected cases (n = 26).
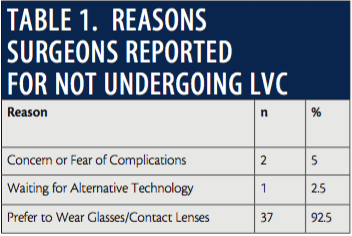
“The results in this study generally agree with those in previously published surveys of the members of the [International Society of Refractive Surgery] as reported by Duffey and Leaming. Their 2014 survey, although challenged by a response rate of 15%, reported that 40% of all refractive surgeons had refractive surgery,” the authors wrote.2 “This compares with 28.9% found in the current study.”
ANSWERING THE QUESTION
But even with these convincing statistics, should LVC really be considered a human right? According to Arthur B. Cummings, MB ChB, FCS(SA), MMed(Ophth), FRCS(Edin), it would be more accurate to say that the need to obtain optimal vision correction is a human right, as “refractive surgery [is] a first-world luxury—a choice for those who wish to see better without the use of contact lenses or glasses.”
Joaquin Fernández, MD agreed. “I believe that the better focus in ocular health should be to end preventable blindness from conditions such as diabetic retinopathy, glaucoma, and keratoconus.”
Dr. Fernández also said that efforts must be made to promote early diagnosis of diseases and to ensure that all patients receive the best available treatments.
Drs. Cummings and Fernández provide further thoughts in the accompanying commentary, along with a different opinion expressed by Ludger Hanneken, MD. “I would argue that, once optical solutions are consistently financed through public health care, then refractive surgery should be as well. At the very least, it should be cofinanced.”
So, now, CRST Europe asks: What side are you on?
1. United Nations website. The Universal Declaration of Human Rights. www.un.org/en/universal-declaration-human-rights/. Accessed March 9, 2016.
2. Kezirian GM, Parkhurst GD, Brinton JP, et al. Prevalence of laser vision correction in ophthalmologists who perform refractive surgery. J Cataract Refract Surg. 2015;41:1826-1832.
Leave Refractive Surgery as a Self-Pay Procedure
Laser vision correction is a first-world luxury.
As the furthest thing removed from a politician, I may be ill-equipped to provide a succinct reply to the question in this article’s headline, but I will endeavor to do my best.
In my mind, the term human rights evokes serious issues: the right to a fair trial, protection against enslavement, prohibition of genocide, free speech, and the right to an education. This list, taken directly from Wikipedia, is in line with my view on what human rights means.
Refractive surgery is a wonderful, safe, and effective procedure that is arguably more successful than any other procedure in ophthalmology and possibly all of medicine. Because visual impairment is a serious disability, the need to obtain optimal vision correction would be a human right in my mind. It is terribly sad and inefficient that people prosper less than they should due to refractive errors causing poor eyesight. I also think that the need for spectacles to correct poor vision borders on a human right. How does blindness caused by a cataract differ from blindness caused by being a -14.00 D myope? Both stop the afflicted person from living a full and productive life, and both are imminently treatable.
Most of humankind is happy to donate hard-earned cash to charities that support cataract surgery and would likely happily do so, too, for charities that provide the less fortunate with spectacles. One example of the latter is Lions Clubs International (http://www.lionsclubs.org/EN/how-we-serve/health/sight/eyeglass-recycling.php).
But refractive errors can also be treated with contact lenses and refractive surgery. Does this mean that being provided with contact lenses is a human right? I would argue no, especially if spectacles are available.
In the same vein, I do not regard refractive surgery as a human right but as a luxury. Refractive surgery does the same thing as glasses; that is, it corrects vision. The advantages to refractive surgery nowadays, however, are better outcomes and more freedom for patients in terms of the activities that they can participate in. These and other points make refractive surgery a first-world luxury—a choice for those who wish to see better without the use of contact lenses or glasses.
Do not get me wrong: I have had LASIK, as have both of my sons and my wife. If ever there was a believer in LASIK, you are reading his opinion right now. However, I do believe that this is a choice, not a right.
I am a big admirer and supporter of the RSA, and I like immensely what it stands for. I just think that use of the phrase human right is taking it a step too far at this point in the world’s history. There are more pressing issues that can be classified as human rights, such as those I listed at the outset of my contribution.
From a purely selfish point of view, I can attest that, as soon as health care funds become involved in paying for refractive surgery, surgeons will lose another procedure to the downward spiral of depressed fees, less control, and management by administrators. We have enough of that already, and, therefore, from my point of view, please leave refractive surgery in the self-pay category.
Arthur B. Cummings, MB ChB, FCS(SA), MMed(Ophth), FRCS(Edin)
• Consultant Ophthalmologist, Wellington Eye Clinic and Beacon Hospital, Dublin, Ireland
• Associate Chief Medical Editor, CRST Europe
• abc@wellingtoneyeclinic.com
• Financial disclosure: Consultant (Alcon/WaveLight), Chief Medical Officer (ClearSight Innovations)
An Almost Utopian Approach
The ultimate aim of a health-based approach to human rights is to offer solutions that amend inequalities.
When you search for the term human right on the World Health Organization (WHO) website, you will learn that the organization’s constitution “was the first international instrument to enshrine the enjoyment of the highest attainable standard of health as a fundamental right of every human being (‘the right to health’).”1 The WHO is committed to incorporating human rights into health care programs and politics at both national and regional levels.
But what demands or social requirements that favor the health of all people are considered human rights? As I see it, they include the availability of health services, safe working conditions, adequate housing, and nutritious food.
The WHO defines health as “a state of complete physical, mental, and social well-being, and not merely the absence of disease or infirmity.”2 This definition has not been amended since it was entered into force on April 7, 1948.
Using this definition in regard to ocular health, the highest attainable degree of health might include correction of refractive errors with laser vision correction. On the other hand, the ultimate aim of a health-based approach in human rights is to offer strategies and solutions that amend inequalities and promote nondiscrimination. Does considering refractive surgery a human right amend inequality? I believe the answer is no.
This is why, to me, it seems a maximalist and almost utopian approach to include refractive surgery among the universal human rights. Just as the WHO definition of health prioritizes complete physical, mental, and social well-being in addition to the absence of disease and illness, I believe that the better focus in ocular health should be to end preventable blindness from conditions such as age-related macular degeneration, glaucoma, and diabetic retinopathy.
In order to uphold human rights in our national health services, we, as practicing physicians, must put forth our best efforts to educate the citizenship and the political authorities; to provide resources to achieve the earliest possible diagnosis and access to the best evidence-based treatments for all patients, regardless of their economic status; and to fight against preventable blindness. However, from my humble point of view, this objective does not include refractive surgery.
1. World Health Organization website. Human rights. http://www.who.int/topics/human_rights/en/. Accessed March 10, 2016.
2. World Health Organization website. WHO definition of health. http://www.who.int/about/definition/en/print.html. Accessed March 10, 2016.
Joaquin Fernández, MD
• Medical Director, Qvision, Almería, Spain
• joaquinfernandezoft@qvision.es
• Financial disclosure: None
Public Health Care Cannot Maintain the Speed of Technological Development
There will always be controversial reimbursement discussions.
Good health is probably the most important criterion for quality of life. Today, established health care systems throughout the developed world exist to provide individuals with access to medical treatment, thereby promoting good health.
But medical treatment does not occur for free. In some countries, taxes are used to finance health care; in others, insurance premiums. Frequently these sources of funding exist in parallel, giving patients a choice between public and private medicine. In most countries with public health care systems, those systems are underfinanced and fight constantly with growing costs. Therefore, every service must be economically justified.
This brings up several questions: Is the correction of refractive errors economically justifiable? Should refractive error be defined as a disease? If yes, must public health systems finance all possible treatment options (glasses, contact lenses, and refractive surgery)? The answers to these questions are not easy, in part because, in relation to refractive errors, there may be no clear definition of what is health and what is a disease.
The way I see it is this: As vision is commonly considered the most important of our five senses, it is only reasonable that individuals should have the right of access to correction of refractive errors, whether they live in a country with a public or private health care system.
In most health care systems, visits to an ophthalmologist in the public sector are covered. Coverage for refractive correction, however, can differ significantly from one system to another. Some health care systems cover the cost of glasses (sometimes with age limitations), and others cover the cost of contact lenses in specific cases only. Yet, in many other systems, glasses and contacts must be self-financed. Furthermore, I do not know of any public system that currently covers refractive surgery. (Brazil did for a short time but has since discontinued this service.) Because nonsurgical solutions for refractive errors, in most cases, must be privately financed, labeling refractive surgery as a human right cannot be justified.
With that said, if refractive surgery is cost efficient, which it is in many cases, why should the public health care system not pay for it? I would argue that, once optical solutions are consistently financed through public health care, then refractive surgery should be as well. At the very least, it should be cofinanced.
Perhaps the more important question today is this: What is the biggest obstacle to growth in the refractive surgery market? LASIK volume could be far higher, but the reasons it is not, in my opinion, are insufficient patient education, bad press, and, most important, patient fear. Therefore, in order for the LASIK market to grow, we must better educate the public about the available methods of refractive correction.
I believe that public health care coverage of refractive surgery would improve awareness of these procedures. But we must also find other ways to promote these interventions. Apart from delivering successful surgery, our job as refractive surgeons is to constantly improve patient education. We must teach patients that, in addition to LASIK, there are other treatments under the umbrella of refractive surgery, including other cornea-based surgeries, phakic lens implantations, lens-based surgery, and combinations of these methods.
Coming back to the original topic of refractive surgery as a human right, I believe that it is the duty of public health care systems to reduce the burden of health risks. Refractive errors, presbyopia, and even cataract are not health risks. With that said, in my opinion, an approach that combines private coverage with an investment plan for this kind of surgery would serve patient needs much better. It would make refractive surgery with all its variations affordable for everyone and would allow us to propose and deliver the best treatment for the individual patient without concern for public reimbursement coverage.
In short, public health care is not able to maintain the speed of technological development in eye care, and controversial reimbursement discussions will always be with us.
Ludger Hanneken, MD
• VallmedicVision, Andorra, Spain
• hanneken@vallmedicvision.com
• Financial disclosure: None
