
Although it is sometimes still debated who performed the first LASIK procedure—Pallikaris1 or Buratto2,3—one thing is undeniable: In its short history, LASIK has changed the lives of literally millions of people. Since its earliest forms, LASIK has been a safe and effective method of correcting refractive errors. Yet today, despite the procedure’s rich clinical and historical presence, the reputation of LASIK has eroded and, along with it, the reputations of the surgeons who remain its unwavering supporters. Why is this?
AT A GLANCE
• LASIK is the safest, most successful, and most widely studied elective procedure in the world, with the highest patient satisfaction rate of any elective procedure.
• Despite the procedure’s rich clinical and historical presence, the reputation of LASIK has eroded, in part because of the easy accessibility of patient complaints online, but also because several myths related to the procedure are in circulation today.
• It is the responsibility of the ophthalmic community to educate patients, to improve their satisfaction, and, most important, to embrace those who are dissatisfied with their vision following LASIK.
Part of the reason that LASIK’s reputation has suffered is that complaints from unhappy patients are easily available on the Internet and on social media. We cannot, however, place all of the blame there. In addition, many of our peers continue to think in terms of postoperative outcomes data from the earliest days of LASIK (see LASIK: Then and Now), and several myths related to the procedure remain in circulation today.
The aims of this article are to debunk these myths and to provide readers with a better understanding of just how good LASIK truly is.
DEBUNKING SIX MYTHS
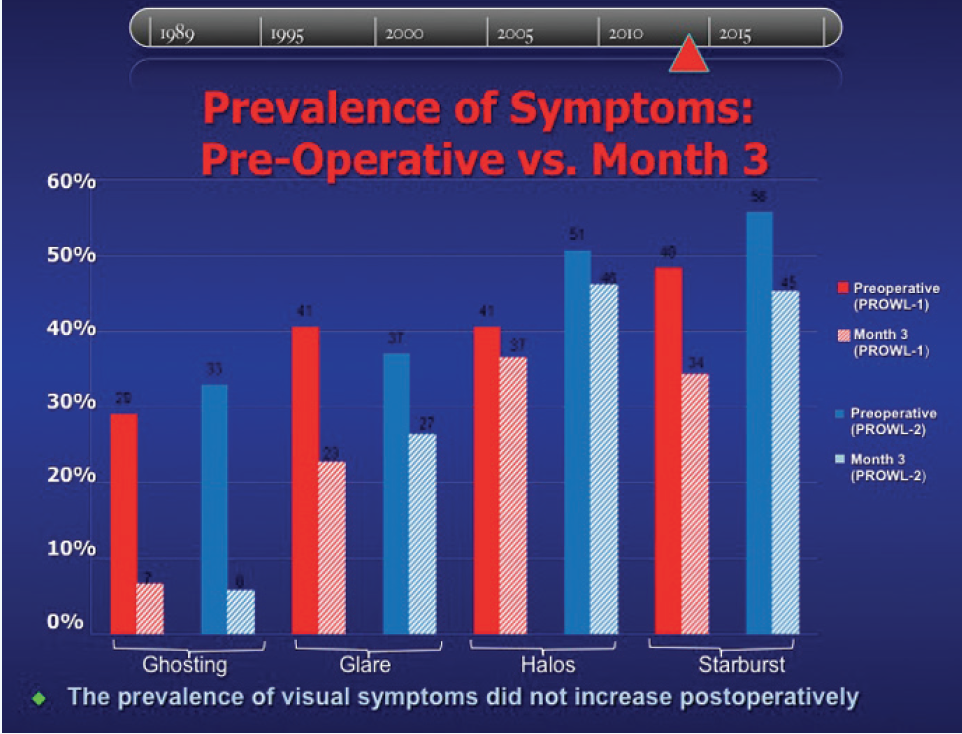
Figure 1. Prevalence of symptoms in the PROWL-1 and PROWL-2 studies: preoperatively to 3 months postoperatively.
Myth No. 1: Physicians would never have LASIK on their own eyes. As recently reported by Kezirian et al,4 refractive surgeons are more than four times more likely to have had refractive surgery than the general population. Using data from an online survey emailed to 250 randomly selected practicing refractive surgeons, Kezirian’s group identified 107 respondents who were candidates for laser vision correction. Of these, 67 reported that they had undergone laser vision correction (LASIK, 65.7%; PRK, 34.3%) on their own eyes. Furthermore, 91% of all respondents said that they recommend refractive surgery to their immediate family members.
In a separate survey of physicians who underwent laser vision correction at one institution, patient satisfaction among 132 respondents was 95.3%.5 In this physician population, 84.8% of participants who answered a 12-question survey on their unique experiences with refractive surgery noted an improved quality of vision postoperatively compared with their preoperative vision with glasses.
Myth No. 3: LASIK significantly increases the risk of glare and halos. According to results of the Patient-Reported Outcomes With LASIK studies (PROWL-1 and PROWL-2),7,8 the presence of glare and halos was dramatically reduced with patients’ spectacle-free vision 3 months after LASIK as compared with their presence preoperatively with glasses. Additionally, no patient in either cohort experienced significant ghosting after surgery as compared with beforehand (Figure 1).
Another study by Tanzer9 showed that 88% of pilots who land on aircraft carriers at night found their night vision to be better after LASIK with no glasses than they did with their glasses before surgery.

Myth No. 4: Dry eye is extremely common after LASIK. The PROWL-1 and PROWL-2 studies7,8 also looked at post-LASIK dry eye symptoms using the Ocular Surface Disease Index. Three months postoperatively in both study cohorts, 23% of patients reported mild dry eye; only 3% of patients in PROWL-1 and 2% in PROWL-2 reported moderate dry eye, and 1% and 3%, respectively, reported severe dry eye. The studies also indicated that up to 30% of patients developed new dry eye symptoms, but this was at 3 months postoperatively. At the 6-month follow-up visit, there was a significant reduction in dry eye symptoms in both patient cohorts. Overall, patient satisfaction was extremely high, with 96% of patients in PROWL-1 and 98.7% in PROWL-2 expressing satisfaction with their vision at month 3.

Figure 2. Opportunities for growth of LASIK: In attempt to determine what drives people to undergo, consider, or forego LASIK, Abbott Medical Optics asked more than 1,200 US patients and potential patients between the ages of 25 and 40 years to share their thoughts on the procedure. The hope of this study was to gain insights needed to improve the patient journey and convert more prospective patients into patients.
Another thing to consider is that better dry eye point-of-service diagnostic testing is available today, providing the means by which to accurately identify patients at risk of postoperative dry eye and to better treat the condition, both pre- and postoperatively. There is no denying that dry eye is an important issue in LASIK, and, as my colleagues and I reported, there is a significant loss of short-term corneal sensation following the procedure.10 By 6 months postoperative, however, corneal sensation improves to preoperative levels, and dry eye signs and symptoms return to normal.
Myth No. 5: The safety of LASIK has not improved. Debunking this myth requires us to revisit the results of the first LASIK trial, conducted by Kremer et al,11 and to compare them with present-day LASIK results. In Kremer’s study, 2,482 eyes that had undergone myopic LASIK for treatment of -1.00 to -15.00 D of myopia and up to 5.00 D of astigmatism were observed for 1 year. Eyes were broken into two cohorts depending on the amount of myopia (cohort 1, < -7.00 D; cohort 2, ≥ -7.00 D). Six months postoperatively, 40.5% of eyes in cohort 1 and 39.9% in cohort 2 had obtained UCVAs of 20/20 or better, and 90.3% and 92.2% of eyes in those respective cohorts had obtained UCVAs of 20/40 or better. At 12 months, 31.7% and 32.7% of eyes in cohorts 1 and 2, respectively, had obtained UCVAs of 20/20 or better, and 86.7% and 87.4%, respectively, had achieved UCVAs of 20/40 or better.
With regard to predictability, at 6 months, 71% and 74% of eyes in cohorts 1 and 2 were within ±0.50 D of intended correction, and 87.8% and 92.6%, respectively, were within ±1.00 D. At 12 months, these figures decreased to 67% within ±0.50 D and 85.6% within ±1.00 D in cohort 1 and 62.6% within ±0.50 D and 85.5% within ±1.00 D in cohort 2.
Additionally, 6.8% of eyes with -7.00 D of myopia or more had lost at least 2 lines of BCVA by 6 months postoperatively, and only 45% of the eyes with less than -7.00 D of myopia and 14% with more than -7.00 D of myopia had achieved a UCVA of 20/20.
LASIK has come a long way since that time (Figure 2). In more recent studies, a greater percentage of patients have achieved 20/20 or better UCVA, are happy with their postoperative outcomes, and have not experienced new or worsening dry eye symptoms after LASIK. In fact, it appears that there is a 10-year trend of continual improvement in visual acuity after LASIK and in the safety of the procedure.12
The most definitive studies ever done on LASIK were the PROWL studies,7,8 which were conducted by the US FDA. In PROWL-1 and PROWL-2, 99% and 96% of patients, respectively, achieved 20/20 or better UCVA by 3 months postoperatively, and not a single patient required an enhancement procedure. Furthermore, no patient had a postoperative BCVA worse than 20/40, and no patient with a preoperative BCVA of 20/20 had a postoperative BCVA worse than 20/25. Only one patient across both cohorts lost 2 or more lines of BCVA.
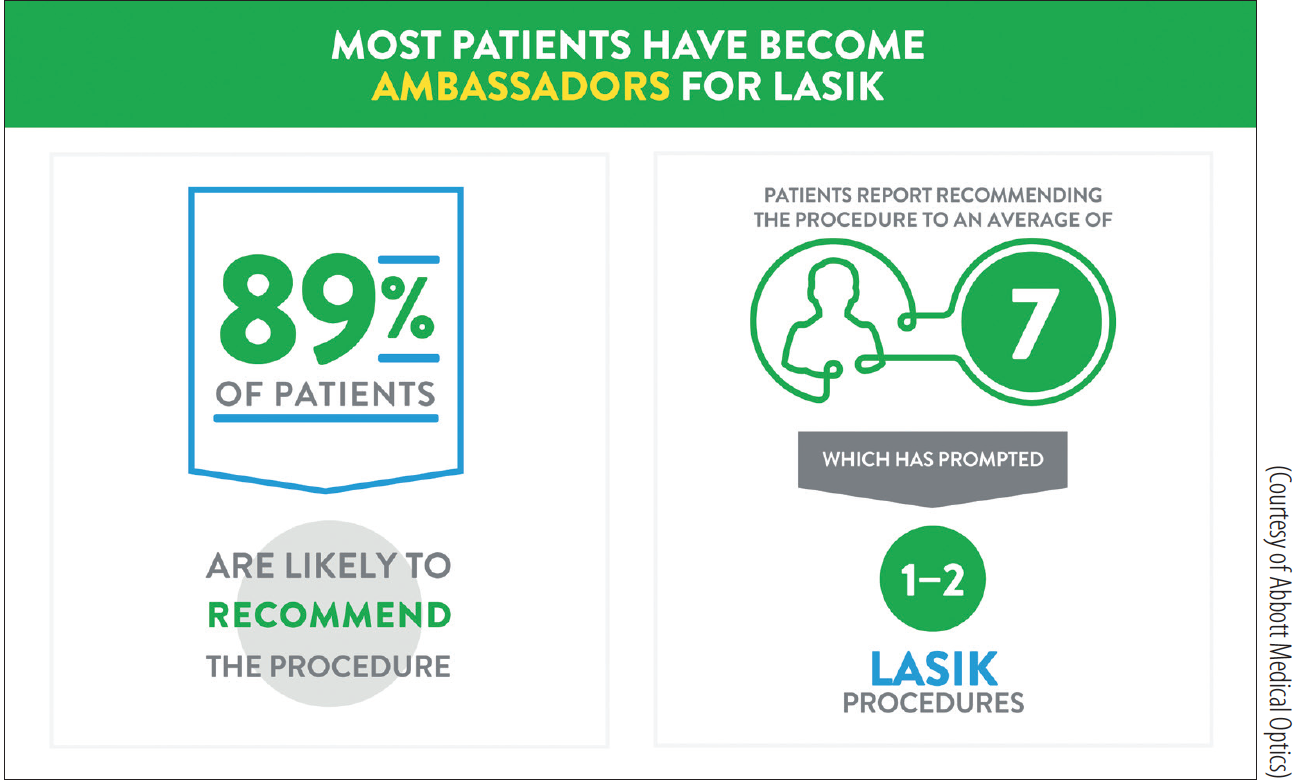
Figure 3. Satisfied patients are likely to become ambassadors for LASIK.
In a world literature review of LASIK, in which 2,915 abstracts and 97 peer-reviewed articles were reviewed and which included 68,000 eyes, the authors concluded that an average of 95.4% of patients were satisfied with their outcome after LASIK (Figure 3).13 This meant that LASIK was the most highly appreciated of any elective procedure, including abdominoplasty, liposuction, brow lift, facial skin tightening, rhinoplasty, breast augmentation or reduction, and botulinum toxin injection.13 In this literature review, the rate of dry eye symptoms did not change significantly between pre- and postoperative assessments (32%–35%).
Myth No. 6: Complications are commonplace. In 1999, Stulting et al14 reported that LASIK-related complications occurred in about 5% of patients. However, this complication rate was directly associated with the experience of the surgeon and the surgical team. Furthermore, Melki and Azar15 reported in 2001 that the majority of complications in LASIK surgery were flap-related. Since the advent of the femtosecond laser as a flap cutter, the incidence of such complications has certainly decreased.
Also important to remember is that LASIK indications have changed drastically over the years. In early days, we performed LASIK on patients with up to -25.00 D of myopia; nowadays, we know that complications associated with LASIK are more likely to occur in patients with more than -7.00 D of myopia.16
IN RESPONSE TO COMPLICATIONS
In response to the complications associated with LASIK, several websites were established to focus attention on these complications. The key ideas behind these websites were (1) to coordinate among eye care professionals to facilitate understanding of the needs of patients with complications of refractive surgery and to advocate for treatment alternatives, (2) to increase public awareness of the potential risks of refractive surgery and advocate for informed decision-making, and (3) to disseminate information about new and emerging treatments for individuals with complications of refractive surgery.
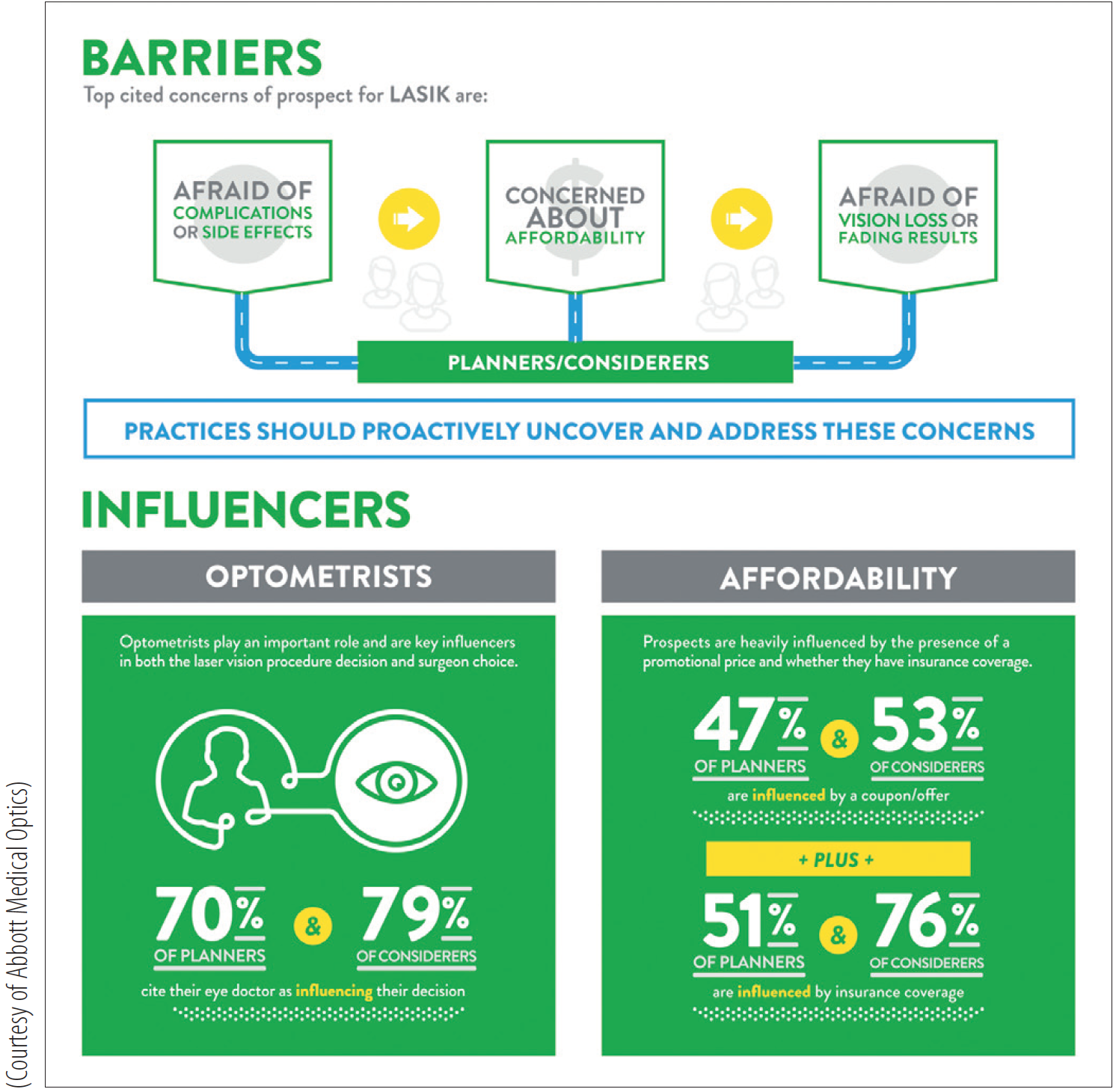
Figure 4. Barriers to and influencers of LASIK.
Unfortunately, as most of us know, these websites were subsequently hijacked by trial lawyers and others, who used them as scare tactics to dissuade people from undergoing LASIK and to encourage them to seek litigation. It is an unfortunate circumstance, as it would benefit refractive surgeons to be able to work together with these organizations, and with consumers, to improve LASIK outcomes.
a different impression
In 2008, after the US FDA received 140 complaints from LASIK patients, a public hearing was held. Anti-LASIK activists expressed their intent to ban the procedure in the United States, with testimonies including personal stories of depression, suicide or suicidal ideation, and other psychological problems. Supporters of LASIK—myself included—also testified at this public hearing, where we spoke to the safety of the procedure.
I came away from this experience with an entirely different impression of unhappy patients. The take-home message for me was that most of these patients had one similar complaint: They felt abandoned by their surgeons. Right then and there, I pledged that I would never again let a patient feel abandoned. If I could not provide a patient with the care that he or she needed, I would find someone who could.
So, to all of the leaders of ophthalmology, let us never allow this to happen to patients again. Moving forward, our responsibilities must be to educate patients; to continue to improve patient satisfaction, with 100% of patients seeing the same or better than they did preoperatively; and, most important, to embrace patients who are dissatisfied with their vision following LASIK and never allow them to feel abandoned (Figure 4).
1. Pallikaris I, Papatzanaki M, Stathi EZ, et al. Laser in situ keratomileusis. Lasers Surg Med. 1990;10:463-468.
2. Buratto L, Ferrari M, Genisi C. Keratomileusis for myopia with the excimer laser (Buratto technique): short-term results. Refract Corneal Surg. 1993:9(2 Suppl);130-133.
3. Buratto L, Ferrari M, Genisi C. Myopic keratomileusis with the excimer laser: 1-year follow-up. Refract Corneal Surg. 1993;9:12-19.
4. Kezirian GM, Parkhurst DG, Brinton JP, et al. Prevalence of laser vision correction in ophthalmologists who perform refractive surgery. J Cataract Refract Surg. 2015;41:1826-1832.
5. Pasquali TA, Smadja D, Savetsky MJ, et al. Long-term follow-up after laser vision correction in physicians: Quality of life and patient satisfaction. J Cataract Refract Surg. 2014;40(3):395-402.
6. McGee HT, Mathers WD. Laser in situ keratomileusis versus long-term contact lens wear: Decision analysis. J Cataract Refract Surg. 2009;35(11):1860-1867.
7. FDA website. Patient-reported outcomes with LASIK (PROWL-1) results. http://www.fda.gov/downloads/MedicalDevices/ProductsandMedicalProcedures/SurgeryandLifeSupport/LASIK/UCM421192.pdf. Accessed June 7, 2016.
8. FDA website. Patient-reported outcomes with LASIK (PROWL-2) results. http://www.fda.gov/downloads/MedicalDevices/ProductsandMedicalProcedures/SurgeryandLifeSupport/LASIK/UCM421193.pdf. Accessed June 7, 2016.
9. Tanzer DJ, Brunstetter T, Zeber R, et al. Laser in situ keratomileusis in United States Naval aviators. J Cataract Refract Surg. 2013;39(7):1047-1058.
10. Donnenfeld ED, Solomon K, Perry HD, et al. The effect of hinge position on corneal sensation and dry eye after LASIK. Ophthalmology. 2003;110(5):1023-1029; discussion 1029-1030.
11. Kremer FB, Pronesti G, Solat J, et al. Prospective LASIK trial for myopia and myopic astigmatism: 1-year results. Ann Ophthalmol. 2001;33(4):315-322.
12. Yuen KH, Chan WK, Kho J, et al. A 10-year prospective audit of LASIK outcomes for myopia in 37,932 eyes at a single institution in Asia. Ophthalmology. 2010;117(6):1236-1244.
13. Solomon KD, Fernández de Castro LE, Sandoval HP, et al. LASIK world literature review. Ophthalmology. 2009;116(4):691-701.
14. Stulting RD, Carr JD, Thompson KP, et al. Complications of laser in situ keratomileusis for the correction of myopia. Ophthalmology. 1999;106(1):13-20.
15. Melki SA, Azar DT. LASIK complications: Etiology, management, and prevention. Surv Ophthalmol. 2001;46(2):95-116.
16. Sugar A, Rapuano CJ, Culbertson WW, et al. Laser in situ keratomileusis for myopia and astigmatism: Safety and efficacy. Ophthalmology. 2002;109(1):175-187.
Eric D. Donnenfeld, MD
• Professor of Ophthalmology, New York University
• Trustee, Dartmouth Medical School, Hanover, New Hampshire
• Member, CRST Europe Global Advisory Board
• ericdonnenfeld@gmail.com
• Financial disclosure: Consultant (Alcon, Abbott Medical Optics, Bausch + Lomb, Carl Zeiss Meditec)


