
Tremendous changes in cataract surgery have occurred over the years, from the initial days of large-incision intracapsular cataract extraction to the most recent advances in small-incision laser-assisted cataract surgery (LACS). Much of the progress we have witnessed has focused on safely removing a cataract through increasingly smaller incisions. Despite the many advantages of advanced cataract surgery techniques, including phacoemulsification and LACS, surgical pitfalls still exist. It is for this reason that I recently became interested in the miLoop (IanTech; Figure 1), a new device designed to transect the cataract with minimal energy and maximal safety.

PITFALLS IN CURRENT TECHNIQUES
Phacoemulsification with ultrasound, one of the most significant revolutions in cataract surgery to date, has allowed relatively safe lens removal through a sub–2-mm incision. One disadvantage of using ultrasound, however, is that the collateral energy transferred to ocular structures can result in swelling and inflammation. Furthermore, phaco ultrasound requires technical expertise to perform and potentially years of learning to master. It also entails a fixed capital expense for the machine plus additional disposable costs incurred on a per-use basis, possibly limiting availability of the technology in the developing world.
Femtosecond lasers were recently developed to help increase the precision and accuracy of cataract surgery, making the procedure easier among those with broader skill sets. The use of a laser for key steps of surgery has helped to reduce the ultrasound energy required to remove the lens and has resulted in quicker healing. Unfortunately, the technology also drastically increases the cost of the procedure, potentially decreases the efficiency of surgery, and comes with a learning curve that requires time and experience to achieve results that are equal or superior to those achieved with standard cataract surgery. LACS has also made some of the surgical steps more challenging, such as cortical cleanup with irrigation and aspiration (I/A).
ENTER THE miloop
The miLoop sidesteps some of the pitfalls associated with various cataract surgery techniques. After using the device in 40 cases, I believe in its potential to make cataract surgery safer and more efficient by dramatically reducing or potentially eliminating the need for ultrasound energy.
This single-use disposable instrument features a flexible, retractable, nitinol loop that is designed to be deployed within the capsular bag to encircle the cataract. Once that step is complete, the loop is retracted, and the lens is effectively bisected. The loop can be redeployed multiple times at the beginning of the case to break the cataract into smaller, more manageable pieces.
The shape of the loop mirrors the natural anatomy of the capsular bag to prevent capsular damage. Furthermore, the gauge of the nitinol is stiff enough to allow manipulations within the bag to ensnare the cataract but flexible enough to avoid damaging the bag and zonular structures.
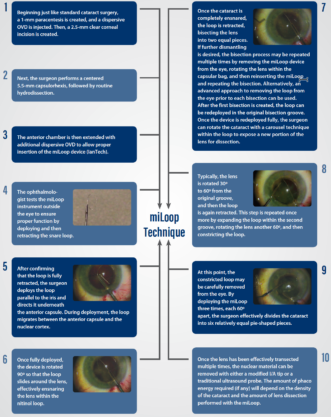
The step-by-step technique that I have been using with the miLoop may be viewed on Eyetube.net (bit.ly/wiley0517E) and is outlined in the graphic on page 32.
ADVANTAGES
I have noticed several unique advantages to the miLoop compared with other techniques for softening and dividing the lens.
No. 1: The miLoop transects the cataract completely, without leaving an untreated area. For safety reasons and owing to technical limitations, the femtosecond laser cannot soften the lens fully to the lens equator, and a buffer zone of at least 500 µm is required between the treated area and the capsular bag.
WATCH IT NOW
William F. Wiley, MD, uses the miLoop device to transcect a cataract.
No. 2: The miLoop can be deployed through a relatively small pupil, ensuring the device’s potential use on nearly every cataract. On the other hand, the treatment area with femtosecond lasers is limited by the size of the pupil because treatment cannot extend beyond the pupillary margin.
No. 3: Constriction of the miLoop slightly lifts and loosens nuclear material, allowing safe and easy removal of nuclear segments. While deployed and rotated, the device loosens the cortical material, making the I/A step of cortical removal easier. Conversely, I/A can be more challenging in a laser-treated eye because the cortex is often closely adherent to the capsular edge.
No. 4: The miLoop works independently of nuclear density. Because the device can cut through both soft and dense nuclei, the effect of apparent variability and the need for technique adjustments with different cataract grades are reduced. Furthermore, compared with traditional lens-dissection techniques, the miLoop appears to be gentler on the ocular structures and to require less of the manipulation and stretching of the capsular bag that are often needed with manual chopping techniques.
RESULTS
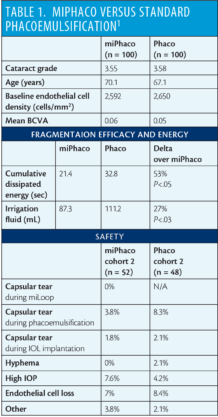
Earlier in 2017, a randomized controlled study was conducted comparing miLoop and phacoemulsification (miPhaco) versus standard phacoemulsification (standard phaco) in moderate to advanced cataracts.1 In all cases, the Centurion Vision System (Alcon) with torsional ultrasound was used for phacoemulsification. Baseline demographic data, visual outcomes, and safety were similar in the miPhaco group (n = 100) and standard phaco group (n = 100), and the average cataract grade was 3.55 and 3.58, respectively. In the cases in which the miLoop was used to fragment the lens, it was done prior to phacoemulsification.
Results are shown in Table 1. In the standard phaco group, mean cumulative dissipated energy and fluidics values were 53% and 27% higher than in the miPhaco group, respectively. Further, endothelial cell loss was 20% higher in the standard phaco group (8.4% vs 7%). The researchers also found that the miLoop greatly improved peripheral cortical removal.
SYNERGIES AND OPPORTUNITIES
Although the miLoop may have the ability to displace some current technologies, there is also an opportunity for the device to work synergistically with available therapeutic options. For instance, it can be used after LACS to assist with nuclear dissection and to help release adherent cortex during I/A. The miLoop can also work well with phaco ultrasound, allowing more efficient and lower energy usage.
With that said, I expect the miLoop to open the door to a whole new set of technologies and approaches to cataract removal. By effectively dissecting the nucleus into small, manageable pieces, there is the potential for a tool other than traditional phacoemulsification and I/A to remove the cataract fragments. This may spur the development of even safer and more effective approaches to cataract extraction.
I can also foresee the use of the miLoop in premium cataract surgery, a procedure that promises to deliver the best outcomes and the quickest healing times. By reducing or eliminating phaco energy during the procedure, the device may allow premium patients to achieve their visual potential more quickly with lower complication rates. Beyond premium cases, surgeons may prefer to use the technique in all cases if it provides a better experience for them and their patients.
As a cost-effective and obtainable technology, the miLoop may provide first-world outcomes in third-world settings. Its disposable and portable nature recommends the device’s use where ophthalmologists may not have access to expensive phaco machines.
CONCLUSION
This new strategy may transform the landscape of cataract surgery. Based on my personal experience, the miLoop has the potential to rock the foundation of recent advances and either drastically improve the effectiveness of current technologies or potentially replace seemingly irreplaceable tools.
1. Tyson FC, MacDonald S, Ahmed I, Calvo EA. Adjunct micro-interventional endocapsular lens fragmentation can significantly reduce phaco energy and fluidics: Results of the Leep 103 RCT. Paper presented at: ASCRS/ASOA Congress & Symposium; May 5-9, 2017; Los Angeles.


