ISBCS Has Many Efficiencies
Abdullah S. AlQahtani, MD, DES, DISSO, FEBO
Jeddah, Saudi Arabia

As the need for cataract surgery increases worldwide and the waiting lists lengthen in many countries, the appeal of immediate sequential bilateral cataract surgery (ISBCS) grows. In the Kingdom of Saudi Arabia, where I practice, ISBCS is not routine at many hospitals, but it is becoming more popular when operating on patients who live in remote areas of the country. This is because of its cost-effectiveness and convenience.
During the COVID-19 pandemic, ISBCS offers additional advantages. When the lockdown was lifted in my country, the waiting list for cataract surgery was long. Moreover, safety precautions such as a requirement that patients undergo COVID-19 testing before surgery decrease efficiency. ISBCS can help to offset these delays.
Patient education must include a thorough explanation of the risk of endophthalmitis with cataract surgery and bilateral endopthtalmitis with ISBCS. A complete patient history should include allergies to medications. Whenever ISBCS is performed, it is essential to increase surgical safety through strict adherence to sterilization protocols. The use of modern technology with an excellent safety profile is also advisable.
If a complication occurs during cataract surgery on the first eye, surgery on the second eye should be postponed. In addition to allowing time for the complication to be addressed, the delay can also permit appropriate preparation for the second surgical procedure.
I expect that ISBCS will be performed more frequently in the future as its safety is better established because of the efficiencies it offers.
COVID-19 May Change Our Perspectives on This Controversial Practice
H. Burkhard Dick, MD, PhD, FEBOS-CR
Bochum, Germany

A pattern is emerging that is well-known from the annals of medical history: In times of pandemic, human contact should be restricted to the absolute minimum in order to prevent transmission of the virus—in this case, SARS-CoV-2. In ophthalmology, refractive procedures have therefore been canceled in many countries, at least during stringent lockdowns. In cataract surgery, the current pandemic seems to favor ISBCS over delayed sequential bilateral cataract surgery (DSBCS), which has generally been the norm.
ISBCS is currently an exception, an outlier in the daily practice of cataract surgeons. Of the UK’s Royal College of Ophthalmology members, only 13.9% of those who participated in a 2020 survey on ISBCS stated that they perform the procedure.1 At the 73 centers where ISBCS is performed by Royal College of Ophthalmology survey respondents, ISBCS accounts for only 0.4% of operations.2
I suspect that the hesitancy of so many surgeons to perform ISBCS may be less medically than legally driven. The procedure boasts many advantages, but legal hurdles such as establishing the justification for selecting ISBCS over the routine practice of DSBCS do exist.
SURGICAL RISKS AND BENEFITS
Among the reported benefits of ISBCS are a reduced number of hospital visits, faster rehabilitation, and, for younger patients, a speedier return to work. ISBCS also reduces the number of trips to the hospital or surgery center for patients and their caregivers. The reduced travel burden is a greater benefit in countries with more rural populations, such as parts of the United States and Canada, and, for example, in developing countries, where many patients travel great distances or do not have access to transportation to seek care. In Central Europe, travel distances are usually short, and the number of ophthalmologists and/or ophthalmic surgeons in geographic proximity is high.
There is no doubt in my mind that, in the hands of an experienced surgeon, ISBCS will produce excellent results and have the low complication rates associated with modern cataract surgery. In one analysis, which included 13,711 DSBCS eyes and 3,561 ISBCS eyes, BCVA was 20/20 or better in 48% of the first and 49% of the second eyes in the DSBCS group and 53% of right eyes and 51% of left eyes in the ISBCS group. (The prevalence of ocular comorbidities was slightly higher in the DSBCS population.) Emmetropia (±0.50 D) was achieved in similar proportions of eyes, 61% of first and second DSBCS eyes and 63% and 62% of first and second ISBCS eyes. Statistically, postoperative endophthalmitis occurred in 1 per 10,000 ISBCS eyes and 0.5 per 10,000 DSBCS eyes.3
Postoperative endophthalmitis, probably caused by Pseudomonas aeruginosa, is certainly the biggest concern with ISBCS, and bilateral endophthalmitis is the greatest disaster imaginable. Fortunately, this complication is extremely rare, thanks in part to the introduction of intracameral antibiotic prophylaxis, the efficacy of which was demonstrated in a landmark ESCRS study.4 If practiced according to the highest standards (eg, a complete exchange of each and every material and instrument used, an IOL for the second eye from a different lot, antiseptic preparations by everyone present in the OR), the risk of bilateral endophthalmitis may be extremely small; as Arshinoff recently and rightfully pointed out, it is likely overshadowed by the risk of dying in a traffic accident on the way to the hospital for the second intervention.5

1. Lee E, Balasingam B, Mills EC, Zarei-Ghanavati M, Liu C. A survey exploring ophthalmologists’ attitudes and beliefs in performing immediately sequential bilateral cataract surgery. BMC Ophthalmol. 2020;20(1):210.
2. Buchan JC, Donachie PHJ, Cassels-Brown A, et al. The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: report 7, immediate sequential bilateral cataract surgery in the UK: current practice and patient selection. Eye (Lond). 2020;34(10):1866-1874.
LEGAL CONCERNS AND ALTERNATIVE APPROACHES
Despite all of the factors in favor of ISBCS, I am reluctant to embrace the practice. The reason is not so much the hassle of treating a single patient like two different patients hygiene-wise or all the necessary precautions that demand a skilled OR team (which I fortunately have). Rather it is if—granted a big if—something terrible such as postoperative endophthalmitis, bilateral cystoid macular edema, bilateral corneal decompensation (eg, in cornea guttata), or significant residual refractive error happens, my legal position could be precarious.
COVID-19 may ultimately change the perspectives of lawyers and judges on ISBCS. For now, however, justification for the selection of ISBCS over the routine practice of DSBCS must be established. At least in Germany, the way lawyers conduct fact-finding poses a problem: They rely on expert witnesses who are usually retired or semiretired ophthalmologists and whose expertise in state-of-the-art cataract surgery may be minimal or nonexistent.
When scheduling cataract surgery on the second eye a couple of weeks after surgery on the first may be problematic for a medical, social, or other reason, an approach I call minimally delayed bilateral cataract surgery may be a good alternative. In this scenario, the patient stays overnight in the hospital or at a nearby hotel and undergoes surgery on the second eye the next morning. It is worth noting that, just a generation ago, cataract surgery patients stayed in the hospital for nearly a week after cataract surgery, so one night should not give insurers too big a headache. Of course, a preoperative examination, including visual acuity after cataract surgery of the first eye, is mandatory to exclude relevant problems that may lead to a delay of surgery on the second eye.
CONCLUSION
I may consider performing ISBCS if the aforementioned legal hurdles are eliminated and the approach has proven to be beneficial in the current minimal-contact health care environment where fewer hospital visits may reduce the risk of infection. (It is important to note that ample evidence supports that the transmission of SARS-CoV-2 is more likely to occur in a patient’s private environment than during an appointment with an eye care provider.) Of course, the incidence of complications such as postoperative endophthalmitis after ISBCS must remain as low as in the current literature.3-5 If these requirements are met, a thorough explanation of ISBCS’s risks and benefits must be given to patients to ensure informed consent.6
1. Lee E, Balasingam B, Mills EC, Zarei-Ghanavati M, Liu C. A survey exploring ophthalmologists’ attitudes and beliefs in performing immediately sequential bilateral cataract surgery. BMC Ophthalmol. 2020;20(1):210.
2. Buchan JC, Donachie PHJ, Cassels-Brown A, et al. The Royal College of Ophthalmologists’ National Ophthalmology Database study of cataract surgery: report 7, immediate sequential bilateral cataract surgery in the UK: current practice and patient selection. Eye (Lond). 2020;34(10):1866-1874.
3. Herrinton LJ, Liu L, Alexeeff S, Carolan J, Shorstein NH. Immediate sequential vs delayed sequential bilateral cataract surgery: retrospective comparison of postoperative visual outcomes. Ophthalmology. 2017;124(8):1126-1135.
4. Endophthalmitis Study Group, European Society of Cataract & Refractive Surgeons. Prophylaxis of postoperative endophthalmitis following cataract surgery: results of the ESCRS multicenter study and identification of risk factors. J Cataract Refract Surg. 2007;33(6):978-988.
5. Arshinoff SA, Claoué C, Mehta C, Johanssen B, Hernandez-Da Mota S. Bilateral Pseudomonas endophthalmitis after immediately sequential bilateral cataract surgery: primum non nocere. Arq Bras Oftalmol. 2020;83(4):346-349.
6. Quinn M, Gray D, Bardan AS, Zarei-Ghanavati M, Sparrow J, Liu C. A stakeholder meeting exploring the ethical perspectives of immediately sequential bilateral cataract surgery. J Med Ethics. Published online September 21, 2020. doi:10.1136/medethics-2020-106412
With Specific Training in ISBCS, the Procedure Is Beneficial
Andrzej Grzybowski, MD, PhD
Poznan, Poland

ISBCS was first described nearly 70 years ago, but its adoption has been hampered by a fear of postoperative complications and limited benefits to patients. Improvements in the safety and predictability of cataract surgery have led to a recent increase in the interest in and use of ISBCS.
BENEFITS AND DRAWBACKS
Infectious endophthalmitis is the most serious complication of intraocular surgery, but evidence suggests that concerns about the risk of bilateral endophthalmitis after ISBCS are overblown.1-3
Another concern raised is that ISBCS prevents surgeons from gathering important information from the first operated eye and using it to guide the optical correction of the second eye. Carefully following the inclusion criteria for ISBCS (described later under the heading My Protocol), however, helps to avoid residual ametropia.
Advantages of ISBCS over DSBCS include a faster return to binocularity and stereopsis. Rapid visual rehabilitation is especially beneficial in patients who receive multifocal IOLs because it supports the process of neural adaptation.
During the current pandemic, additional advantages of ISBCS are that it decreases the time spent in the OR and minimizes the number of follow-up visits required.4-8
MY PROTOCOL
I follow a strict protocol with all ISBCS cases.
Preoperative protocol. I consider ISBCS for patients with bilateral cataracts whose surgery will be performed under general anesthesia only if there are no clear contraindications. For patients with bilateral cataracts whose surgery will be performed under topical anesthesia, my first step is to conduct a risk stratification analysis in order to identify contraindications to ISBCS. In addition to risk factors for intra- and postoperative complications, I also evaluate patients for conditions that can make biometry inaccurate. These include a history of corneal or scleral surgery, an axial length greater than 26 mm or shorter than 21 mm, and a difference of more than 1 mm in the axial lengths of the patient’s eyes.
If patients have no contraindications to ISBCS, I thoroughly discuss with them the pros and cons of this approach based on the particulars of their case, including planned IOL design and their ability to attend follow-up visits.
Intraoperative protocol. I follow the recommendations of the International Society of Bilateral Cataract Surgeons. The most important principle in ISBCS is to treat cataract surgery on each eye as an individual, autonomous procedure. Nothing in physical contact with the first operated eye should be used for surgery on the second eye.7,8
The ocular surface receives irrigation with 5% povidone-iodine for 3 minutes before surgery begins. Intracameral administration of an antibiotic occurs at the conclusion of surgery to decrease the risk of postoperative endophthalmitis. If an intraoperative complication occurs during surgery on the first eye, surgery on the second eye is typically deferred.
It is essential that the nursing staff be trained specifically on ISBCS. Operative checklists should be used if possible. The risk of right eye/left eye errors can be minimized by listing all surgical parameters for both eyes on a board that is visible to everyone in the OR.
1. Callaway NF, Ji MH, Mahajan VB, Moshfeghi DM. Bilateral endophthalmitis after immediately sequential bilateral cataract surgery. Ophthalmol Retina. 2019;3(7):618-619.
2. Li O, Kapetanakis V, Claoué C. Simultaneous bilateral endophthalmitis after immediate sequential bilateral cataract surgery: what’s the risk of functional blindness? Am J Ophthalmol. 2014;157(4):749-751.e1.
3. Chen Y, Zhang Y, Li X, Yan H. Incidence of acute-onset endophthalmitis after separate bilateral cataract surgeries less than 5 days apart. BMC Ophthalmol. 2019;19(1):32.
4. Arshinoff SA, Bastianelli PA. Incidence of postoperative endophthalmitis after immediate sequential bilateral cataract surgery. J Cataract Refract Surg. 2011;37(12):2105-2114.
5. Grzybowski A, Krzyżanowska-Berkowska P. Immediate sequential bilateral cataract surgery: who might benefit from the procedure? J Cataract Refract Surg. 2013;39(7):1119-1120.
6. Grzybowski A, Kanclerz P. Recent developments in cataract surgery. In: Grzybowski A, ed. Current Concepts in Ophthalmology. Springer; 2019:55-97.
7. Grzybowski A, Wasińska-Borowiec W, Claoué C. Pros and cons of immediately sequential bilateral cataract surgery (ISBCS). Saudi J Ophthalmol. 2016;30(4):244-249.
8. Singh G, Grzybowski A. Evolution of and developments in simultaneous bilateral cataract surgery. Update 2020. Accepted manuscript. Ann Transl Med. Accessed November 18, 2020. http://atm.amegroups.com/article/viewFile/50285/pdf
Proportion of Cataract Surgery Procedures Carried Out as ISBCS Is Growing
Björn Johansson, MD, PhD, FEBO
Linköping, Sweden

Faster rehabilitation and a fewer number of hospital visits result when both eyes are operated on the same day, as with ISBCS. This approach to cataract surgery is beneficial for patients and for society in a broad sense; however, the risk for a bilateral complication threatening vision continues to be a matter of dispute. Reimbursement regulations are also a major obstacle to adoption of ISBCS.
Some national clinical guidelines mention ISBCS but limit its suggested use for patients who require general anesthesia. Thus, in many health care systems as well as in some Swedish counties, administrators and clinicians have said “no!” to the routine use of ISBCS. But the COVID-19 pandemic has fueled the interest in ISBCS, as the benefits of the procedure appear even more obvious and desirable in our current circumstances.
The increased use of ISBCS has been discussed at a number of streamed webinars and virtual meetings, and the Royal College of Ophthalmologists and the United Kingdom and Ireland Society of Cataract and Refractive Surgeons issued a joint statement to “help units develop local guidelines to safely offer ISBCS to patients if they have the wish and logistical capacity to do so.”1
To what extent ophthalmic surgeons have been adopting ISBCS globally remains to be investigated. In Sweden, compared to 2019, the proportion of cataract surgery procedures carried out as ISBCS has indeed grown significantly (Figure), mainly in the private sector, where the majority of public-financed cataract surgery has been carried out in recent years. The average proportion of ISBCS cases in Sweden was 15% of all surgeries (N = 131,015) in 2019 and 19.5% for the period of January to November 2020 (N = 104,480).
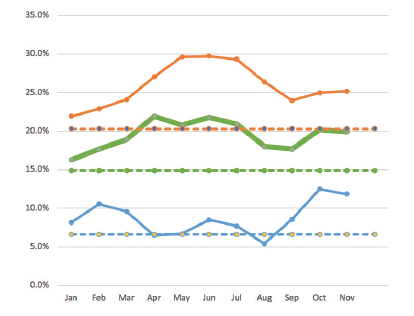
Figure. ISBCS in Sweden: 2019 vs 2020. (Key: dashed lines, 2019 averages; orange, private sector; blue, public sector; green, all clinics)
In my opinion, it may be a good sign that there is no enormous increase in ISBCS rates, as the risk for a bilateral complication threatening vision is not zero. Surgeons and teams should only consider ISBCS after thoroughly reviewing their processes, results, safety records, and complication rates. Adherence to guidelines issued by the International Society for Bilateral Cataract Surgeons is highly recommended (see ISBCS: General Principles for Excellence).
PERSONAL EXPERIENCE
I started with ISBCS more than 20 years ago, and I was somewhat cautious in my approach. I told myself, “I will only do this until I get my first bilateral complication.” I began performing ISBCS in patients with bilateral moderate nuclear sclerosis or posterior subcapsular cataracts reducing vision to between 20/200 and 20/40. The moderate cataract in these patients, I reasoned, was likely to provide good surgical conditions with clear red reflex, and it should be possible to emulsify the lens without excessive levels of ultrasound.
With time, I discovered that the balancing of benefits and risks slowly changed. I started to schedule cases with more potentially complicating factors (eg, dense cataract in at least one eye, limited pupil dilation, macular degeneration). I usually still do unilateral cataract surgery for patients with endothelial dystrophy and for those with significant diabetic retinopathy. Needless to say, uveitis and uncontrolled or advanced glaucoma are absolute contraindications to ISBCS, as is expected low compliance with postoperative care instructions.
I am confident that ISBCS can offer significant benefit to most of our cataract patients and that these benefits have been highlighted by the ongoing pandemic. However, we must be careful and keep our heads clear if health care management and governmental organizations begin to suggest or request an increased use of the concept for financial or other reasons. As clinicians, we must keep the safety of our patients’ vision a priority.
CONCLUSION
The “no” to ISBCS that, for many years, has been common answer to the question in this article’s headline among health care financing bodies, administrators, and professionals has started, and will continue, to change to a definitive yes.
1. Royal College of Ophthalmologists. April 20, 2020. Accessed January 4, 2020. https://www.rcophth.ac.uk/wp-content/uploads/2020/07/Immediate-Sequetial-Bilateral-Cataract-Surgery-Guidance-2.pdf
Reflections on 2 Years of Experience
Mads Kofod, MD, PhD, FEBO, and Lars M. Holm, MD, PhD, FEBO
Rigshospitalet, Denmark


The Department of Ophthalmology at the University Hospital of Copenhagen in Denmark introduced ISBCS as the standard of care in the fall of 2018. ISBCS offers several advantages. For patients, these include a faster visual recovery, fewer visits to the hospital, and a lower risk of anisometropia. From a socioeconomic perspective, patients who require assistance with the administration of eye drops need this help for 1 to 2 weeks less after ISBCS than after DSBCS. For health facilities, the benefit is increased productivity with the same staff and number of ORs.
ADOPTION
In 2013, the National Clinical Guideline on Cataract Surgery published by the Ministry of Health contained a moderate recommendation for ISBCS, after which our department began offering the procedure to patients receiving surgery under general anesthesia. Successful results in this population spurred the introduction of ISBCS for patients receiving surgery under local anesthesia.
Our department performs more than 12,000 cataract surgeries per year. ISBCS accounted for 20.4% of our cases in 2019, and it accounted for 23.4% of our cases at the time of this writing. Because our department prioritizes the training of young cataract surgeons, a proportion of the patients we serve are not available for ISBCS who would otherwise be eligible had an experienced high-volume cataract surgeon performed the surgery.
SAFETY
To minimize the risk of bilateral complications, ISBCS is not offered to patients who are at increased risk of elevated IOP, macular edema, or corneal decompensation after cataract surgery; whose target refraction is uncertain; or who have a history of uveitis. All eligible candidates are offered ISBCS. If they agree, the right eye undergoes the procedure first unless otherwise planned.
Based on an expectation that products acquired from well-respected manufacturers will be safe and thus carry a low risk of contamination, our department deviates from the General Principles for Excellence in ISBCS published by the International Society of Bilateral Cataract Surgeons1 (outlined in the accompanying below) in the following ways:
- We permit the use of gloves, gowns, custom packs, and OVDs from the same lots; and
- Instrument trays may be sterilized on the same date.
On the other hand, we follow the society’s guidelines in the following ways:
- Medications and irrigation fluids are prepared separately by the staff for each surgery;
- Containers are marked for first and second surgeries but may be drawn from the same batch; and
- Intracameral cefuroxime is used for each procedure.
ISBCS: General Principles for Excellence*
Established by the International Society of Bilateral Cataract Surgeons in 2009
1. Cataract or refractive lens surgery should be indicated in both eyes.
2. Any concomitant relevant ocular or periocular disease should be managed.
3. The complexity of the proposed immediate sequential bilateral cataract surgery (ISBCS) procedure should be easily within the competence of the surgeon.
4. The patient should provide suitable informed consent for ISBCS and be free to choose ISBCS or DSBCS.
5. The risk for right–left-eye errors should be minimized by listing all surgical parameters (eg, selected IOL, astigmatism) for both eyes on a board visible to all in the OR at the beginning of each ISBCS case. The World Health Organization operative checklists should also be used if possible.
6. IOL power errors are minimized by having OR personnel familiar with the calculation methods used. The original patient charts should be available in the OR, and everybody passing the IOL to the surgical table should confirm the IOL choice. ISBCS nursing staff should be specifically trained and experienced.
7. Complete aseptic separation of the surgeries on the first and second eyes is mandatory to minimize the risk of postoperative bilateral simultaneous endophthalmitis.
- Nothing in physical contact with the first eye surgery should be used for the second.
- The separate instrument trays for the two eyes should go through complete and separate sterilization cycles with indicators.
- There should be no crossover of instruments, drugs, or devices between the two trays for the two eyes at any time before or during the surgery of either eye.
- Different OVDs and different manufacturers or lots of surgical supplies should be used whenever reasonable (where the device or drug type has ever been found to be causative of endophthalmitis or toxic anterior segment syndrome) and possible (if different lots or manufacturers are available) for the right and left eyes.
- Nothing should be changed with respect to suppliers or devices used in surgery without a thorough review by the entire surgical team to ensure the safety of the proposed changes.
- Before the operation of the second eye, the surgeon and nurse shall use acceptable sterile routines of at least regloving after independent preparation of the second eye’s operative field.
- Intracameral antibiotics have been shown to reduce the risk of postoperative endophthalmitis dramatically. Their use is strongly recommended for ISBCS.
8. Any complication with surgery on the first eye must be resolved before proceeding. Patient safety and benefit are paramount in deciding to proceed to the second eye.
9. ISBCS patients should not be patched. Postoperative topical drops are most effective immediately postoperatively and should be begun immediately postoperatively in high doses, which can be tapered after the first few days. Other ophthalmic medications (eg, for glaucoma) should be continued uninterrupted.
10. ISBCS surgeons should routinely review their cases and the international literature to be sure that they are experiencing no more than acceptable levels of surgical and postoperative complications.
* Adapted from www.isbcs.org/wp-content/uploads/2011/03/2010-07-20-FINAL-ISBCS-SBCS-suggestions-from-ESCRS-B
To avoid errors in IOL power, both the surgeon and the nurse match and check the patient’s chart and IOL calculations. After uneventful surgery on the first eye, the surgeon and assisting nurse change gowns and gloves before continuing with surgery on the second eye.
CONCLUSION
Thus far in our experience, bilateral complications have not occurred in ISBCS eyes. Our clinical quality control in 2019 found no obvious differences in outcomes or safety between eyes that underwent ISBCS and those that received DSBCS. Productivity in the department has increased, whereas stress on the surgeons has not. Although patient satisfaction with ISBCS has not been assessed, the demand for the procedure has grown as patients learn about the offering.
1. ISBCS general principles for excellence in ISBCS 2009. September 2009. Accessed November 24, 2020. http://www.isbcs.org/wp-content/uploads/2011/03/2010-07-20-FINAL-ISBCS-SBCS-suggestions-from-ESCRS-Barcelona.pdf
ISBCS Can Help to Shorten Long Waiting Lists
Christopher Liu, OBE, FRCOphth, FRCS(Ed), FRCP, CertLRS
Brighton and Hove, United Kingdom

As the global pandemic continues, the apprehension some ophthalmologists feel about performing ISBCS is slowly dissipating. The main reason, of course, is that this approach reduces the number of visits, both pre- and postoperative, that are required of patients. But before deciding to implement ISBCS into your practice, it would be wise to weigh the benefits and drawbacks of the procedure (see Advantages and Disadvantages of ISBCS) and to understand which patients typically do best with ISBCS.
Advantages and Disadvantages of ISBCS
Advantages:
- One referral
- One consultation
- One preoperative assessment
- One visit for surgery
- No binocular imbalance in between surgeries
- One visit to the optometrist
- One pair of new glasses
- Health economics
- Reduced travel and reduced time off from work and hobbies
- Reduced carbon footprint
Disadvantages:
- Risk taken with both eyes at the same time
- Potentially increased discomfort during surgery and postoperative recovery
- Requirement of postoperative drops in both eyes
- Potential financial loss to the surgeon and institution
BACKGROUND
COVID-19 is causing untold human suffering and challenging current health care systems. It has forced practices to take a long look at their processes and procedures and, in many ways, change how patient care is administered.
Traditional teaching follows the premise that same-day cataract surgery can cause bilateral blindness through catastrophic complications, including endophthalmitis and cystoid macular edema. Updated guidance from the National Institute for Health and Care Excellence, however, recommends considering ISBCS for routine cases. Further, during the pandemic, some areas of the world have seen up to 45% patient acceptance of ISBCS.
Dr. Liu’s Protocol
- First eye is usually that with the denser cataract
- Topical and intracameral anesthesia
- Long clear temporal corneal incision with low threshold to suture if necessary
- Jelonet gauze, eye pad, and Cartella shield
- Second eye
- Allowing for second eye syndrome and added physical strength and lowered risk of infection, scleral tunnel under anesthesia
- Jelonet gauze, eye pad, and Cartella shield
- Remove eye pad and gauze over first eye and replace with clear shield so patient can see
- Shield wear day and night for first week
- No face mask wear for first week for fear of misdirected breath from oropharynx
GUIDANCE AND PROTOCOLS
Under National Institute for Health and Care Excellence guidance, patients should be considered for ISBCS in the following situations:
- The presence of bilateral visually significant cataracts;
- Eyes at low risk of complications;
- Patients with a low risk of complications;
- Patients for whom the procedure is not expected to be prolonged; and
- Those who need general anesthesia.
ISBCS is not recommended for patients in a variety of situations:
- Those with lenticular abnormalties, including pseudoexfoliation, lens subluxation, phacodonesis, intraocular inflammation, or previous ocular trauma;
- Those at increased risk of glaucoma or retinal detachment; and
- Those with eyes that are at risk of biometry error.
Surgeons should only consider performing ISBCS if they have a foundational understanding of ISBCS, if there is strong cohesion between the surgeon and OR team, and if the hospital has a good track record with ISBCS. Surgeons who are new to performing ISBCS should use this approach only for routine, low-risk cases. My protocol for ISBCS is outlined in the sidebar at the top of this page.
When ISBCS is offered, a description of the procedure must be included in the informed consent. Patients must also understand that the decision to proceed with surgery on the second eye occurs only upon satisfactory completion of surgery in the first eye. If the surgery on the first eye is prolonged or a complication occurs, then surgery on the second eye would be aborted. Finally, ISBCS is only safe when the two eyes are treated as completely separate operations. Between the procedures, the surgeon and team must rescrub and change gowns and gloves, and a separate instrument cart from a different sterilization cycle must be used. Anything entering the second eye must come from different manufacturers or bear different batch numbers from what was used for the first eye.
Some critics of ISBCS argue that use of the same-day technique in tandem with routine cataract surgery creates two queues of patients—those awaiting surgery on their first eye and those waiting for ISBCS. It is true that there will be an initial increase in the number of patients on the waiting list. After a few months, however, patients will not need to return for cataract surgery on their second eye, and the waiting list will be reduced thanks to the increased efficiency of ISBCS.
During the COVID-19 pandemic, efficient patient flow and a simplified patient journey have been crucial. Reducing the duplication of steps or eliminating unnecessary steps, as can be achieved with ISBCS, can help to enhance not only safety but also the patient experience.
Suggested Reading:
1. Shah V, Naderi K, Maubon L, et al. Acceptability of immediate sequential bilateral cataract surgery (ISBCS) in a public health care setting before and after COVID-19: a prospective patient questionnaire survey. BMJ Open Ophthalmology. 2020;5(1):e000554.
2. Royal College of Ophthalmologists. Immediate sequential bilateral cataract surgery (ISBCS) during COVID recovery: RCOphth/UKISCRS rapid advice document. Accessed November 30, 2020. https://www.rcophth.ac.uk/wp-content/uploads/2020/07/Immediate-Sequetial-Bilateral-Cataract-Surgery-Guidance-2.pdf
3. Demystifying immediately sequential bilateral cataract surgery – a practical guide for beginners [webinar]. July 6, 2020. Accessed January 5, 2020. https://www.youtube.com/watch?v=eFPWFjWn4E0
4. Mavrikakis I, Georgiou T, Paul B, Liu CS. Cataract surgery by appointment—a pilot study. BMC Ophthalmol. 2006;6:18.
ISBCS Could Be Easier for Patients, But Is It Truly Better?
Michael Patterson, DO
Tennessee, United States

Aren’t we all fiduciaries to some degree? If the current pandemic has taught me one thing, it is that the Eagles’ hit song “Get Over It” is as relevant today as when it was released in 1994. By and large, doctors like to feel important—and for understandable reasons—but aren’t the lives of their staff and patients even more important? As the father of three (soon to be four), I feel a desire to do better for others than for myself. This is my main reason for not regularly offering ISBCS.
MY STAFF
Perhaps the most undervalued factor in a medical practice’s success is a competent and driven staff. I co-own a practice with more than 140 employees across eight locations. During the current pandemic, my fiduciary responsibility to my staff is greater than ever. When the COVID-19 pandemic started, I watched practices around mine crumble as they laid off employees and did everything they could to protect and serve the owners of those companies. We refused to buckle and have made it our priority to continue supporting and providing for our staff and 13 doctors.
In the United States, ISBCS involves a financial hit to the practice so that surgery on the first and second eyes may be performed on the same day. That alone raises an eyebrow. The investments in technology to become a premium practice, in staffing, and in supplies for the second eye remain the same with ISBCS as with routine DSBCS. Surely no one is performing a cataract procedure on a second eye with the same surgical equipment as was used on the first.
When occasionally it is necessary for one of my patients to undergo cataract surgery on both eyes on the same day, that patient is taken out of the OR between surgeries and the entire room is changed over before surgery on the second eye is performed. No shortcuts are taken. The costs incurred are therefore the same as with DSBCS, and the practice receives 50% of the revenue.
A practice’s staff presumably depends on their paychecks, so they will appreciate it if the owners take their fiduciary responsibility to the practice seriously. The staff would also probably like the profit margin to be as high as possible so that their jobs are secure at a time when job security is difficult to maintain. I am uncertain how anyone who wants to provide for their staff and their staff members’ families can reasonably say that ISBCS is in the best interest of their company. Without cash on hand to pay the staff, no cataract surgery will occur in the first place.
MY PATIENTS
The following is a true story. A patient I will call John in this article was referred to me for cataract surgery. He underwent successful surgery on the first eye, and UCVA was 20/20 at the 1-week follow-up. By day 9, UCVA was hand motion. The anterior chamber was full of cell, and the diagnosis was endophthalmitis.
A retina specialist operated on the patient. After a 4-week recovery period, UCVA was 20/30. The retina doctor cleared the patient to undergo cataract surgery on his contralateral eye. Preoperatively, I explained the risks and benefits of the procedure to the patient. Although I typically prescribe no antibiotic drops pre- or postoperatively, I instructed this patient to administer oral antibiotics preoperatively and topical antibiotic drops pre- and postoperatively. Additionally, antibiotics were administered intraoperatively by intracameral injection. In colloquial English, I threw the kitchen sink at John.
UCVA was 20/20 at his 1-week follow-up. I patted myself on the back and told John that I thought we’d gotten lucky. On postoperative day 9, I received a note from a retina specialist informing me that one of my patients had developed endophthalmitis. It was John. He’d known the routine and had gone straight to the retina specialist without even calling me.
I couldn’t believe my eyes when I read that note. At first, I thought the note on John’s first eye must have been sent to me again by mistake. On closer inspection, I realized the note was indeed about his second eye. Lightning had struck twice, so to speak! Occam’s razor says that a person can have only one diagnosis, but Hickam’s dictum says, “Patients can have as many diseases as they damn well please.”
This case was enough for me. Had this bilateral complication occurred after ISBCS, it would have debilitated the patient for at least a month. I can’t imagine that a retina surgeon would perform bilateral vitrectomies for endophthalmitis. One of the eyes probably would have been neglected—or possibly worse.
I understand the rationale that ISBCS could be easier for patients because, for example, it requires less travel, but is ISBCS truly better for patients?
CONCLUSION
ISBCS simply is not an option I prefer. Do I perform same-day bilateral cataract surgery occasionally? Sure. But for the benefit of my patients and staff, I will not be adopting ISBCS into routine practice anytime soon.