
I coauthored an article for CRST last year with David Lockington, MB BCh, BAO(Hons), FRCOphth, PhD, a consultant ophthalmologist in Glasgow, Scotland. In the piece, he described “avoiding detours rather than taking shortcuts.”1 The sentiment resonates with me and became the cornerstone of increasing efficiency at my clinic and improving the patient experience during the COVID-19 pandemic. Here I share myriad positive changes brought about by the worst pandemic in more than 100 years.2
No. 1: A QUIETER, MORE EFFICIENT CLINIC
Patients endure fewer postoperative visits today than were required before the pandemic.
Cataract surgery and refractive lens exchange. Before the pandemic began, my patients were seen at 1 day, 1 week, and 6 weeks postoperatively. The clinic was full of these patients, who were often seen by my optometric team. Now, patients undergo cataract surgery on their second eye 1 week after surgery on their first eye. The first postoperative follow-up visit for both eyes is scheduled 1 week after the second-eye surgery (ie, 2 weeks after the first eye). Their final visit is at 6 weeks. The updated schedule eliminated both the day 1 visit and one of the week 1 visits, resulting in three fewer visits to the clinic.
LASIK. These patients were seen at 1 day, 6 weeks, and 6 months postoperatively; the last visit was used to fine-tune our laser nomograms. During the pandemic, we attempted to eliminate the 6-week visit, but too many patients objected. It became a voluntary visit that most patients choose to attend.
Surface ablation. The major change in postoperative care scheduling occurred for patients who had PRK and other forms of surface treatment. Before the pandemic, they were seen at days 1 and 6 and months 1, 3, and 6. The updated schedule eliminates the day 1 visit, and patients now are seen on day 6 for bandage contact lens removal and at months 1 and 6. The visit at month 3 is voluntary, but most patients skip it.
The bottom line. Reducing the number of postoperative visits for patients has not compromised postoperative care but has resulted in a quieter, more relaxed clinic environment and greater patient satisfaction. Additional advantages are that the clinic schedule can accommodate more new patients. Revenue has therefore increased.
No. 2: MORE CONVENIENT COMMUNICATION AND PAYMENT METHODS
Text messaging and telemedicine appointments. Patients can check in with clinicians from the comfort of their homes or offices at any time of the day. The use of telemedicine also alleviates the burden on staff of seeing so many patients in person.
Electronic consent forms. We adopted and customized the DocuSign platform for our preoperative forms. Notes and sketches are now delivered to patients in a bundle with the informed consent form via email by DocuSign (Figure). Patients complete the required documents electronically at their convenience and then sign the informed consent form remotely. Those who prefer to sign the form in-person can do so digitally in the clinic.
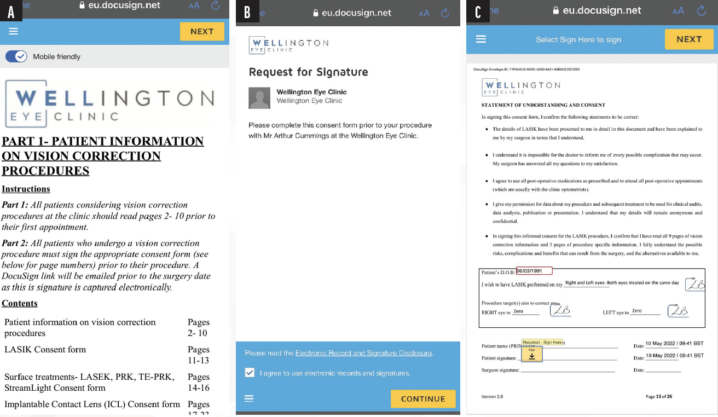
Figure. The patient information packet (A), request for signature notification (B), and statement of understanding and consent (C) are sent to patients via DocuSign.
Electronic medical history forms. We also incorporated a software platform from FormStack that is customized for our clinic. Documents include a thorough medical history form, a list of the reasons why patients are seeking surgery, and the patient’s wish list (ie, what they wish to achieve with surgery).
Electronic medical records. The clinic adopted an electronic medical records (EMR) system in 1999, but we used a hybrid approach. Diary and refractive data were entered into EMRs, and clinical notes were handwritten. Six months before the start of the COVID-19 pandemic, we switched entirely to EMRs. It subsequently took the staff approximately 18 months to scan 64,000 handwritten notes into our EMR system so old records are preserved and easily accessible. This is helpful now that we are experiencing a backlog of cataract surgeries due to the pandemic, especially for patients who had LASIK 20 years ago.
Electronic payments. Rather than pay with a credit or debit card at the reception area on their way out, most patients now pay before they even enter the clinic with payment platforms such as Stripe (Stripe). Some still pay in the clinic, but we now use contactless payment methods. Both electronic payment methods have thorough audit trails. Our patients and the front desk staff save time with the updated protocol.
No. 3: INCREASED DEMAND
As at many ophthalmology practices, we were pleasantly surprised by increased patient demand during the pandemic. Unanticipated effects of the pandemic, including foggy glasses while wearing a face mask, money saved on cancelled vacations, and an uptick in ocular surface disease and computer vision syndrome from more time spent viewing screens spurred interest in ophthalmic services.
Fortunately, we have not seen a drop in procedural and services demand despite war, skyrocketing inflation, disruptions to the supply chain, uncertainties in the energy market, and reductions in disposable income.
CONCLUSION
Most people are familiar with the saying every cloud has a silver lining. It encourages the adoption of a more positive mindset. The pandemic has brought much misfortune, but it has also led to changes in medical practice that have improved clinic efficiency and the patient experience.
1. Lockington D, Cummings AB. Cutting corners or avoiding detours? Cataract & Refractive Surgery Today Europe. 2021;16(6):19-23.
2. Rosenthal M. Fauci: COVID-19 worst pandemic in 100 years. Infectious Disease Special Edition. October 21, 2020. Accessed May 9, 2022. https://www.idse.net/Covid-19/Article/10-20/Fauci–COVID-19-Worst-Pandemic-in-100-Years/60937#:~:text=With%20more%20than%2041%20million,of%20the%20pandemic%20to%20date


