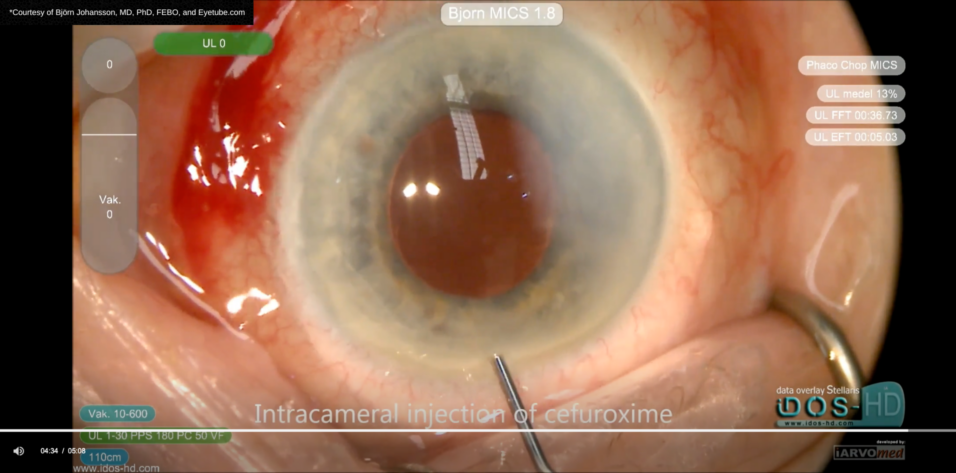
Nothing strikes more fear into the heart of a cataract surgeon than the prospect of a suprachoroidal hemorrhage. Suprachoroidal hemorrhages are statistically rare, but they can occur without warning. Every cataract surgeon must be equipped to recognize and deal with them intraoperatively. The aftermath of a suprachoroidal hemorrhage often involves close coordination with a posterior segment surgeon.
It’s a pleasure to have Jessica Randolph, MD, MPH, and Melissa Suggs, MD, share their vitreoretinal perspective on principles for managing suprachoroidal hemorrhages in this iteration of Fundamentals in Five.
— Kavitha R. Sivaraman, MD


Suprachoroidal hemorrhage is a rare but serious complication of intraocular surgery. It can be difficult to manage and often causes patients to experience a significant decrease in visual acuity. Suprachoroidal hemorrhage results from the rupture of the short or long posterior ciliary arteries, vortex veins, or their tributaries during an acute change in IOP. The complication can also result from choroidal vasculature congestion following peribulbar or retrobulbar anesthesia.
Both glaucoma and cataract surgery carry the risk of suprachoroidal hemorrhage, but it is more often associated with glaucoma surgery. The reported occurrence of suprachoroidal hemorrhage during cataract surgery is less than 0.1% per year. When they occur, suprachoroidal hemorrhages are usually a postoperative complication of glaucoma surgery. They more typically occur intraoperatively with cataract surgery, however, and most commonly during phacoemulsification of the nucleus, nuclear expression, or right after the nucleus is removed.1
1. RISK FACTORS
The risk factors for suprachoroidal hemorrhage can be divided into four categories.2
No. 1: Systemic. Systemic risk factors for suprachoroidal hemorrhage include advanced age, use of anticoagulant or antiplatelet medication, poorly controlled hypertension, atherosclerotic disease, and diabetes.
No. 2: Ocular. Ocular risk factors include a history of glaucoma, high myopia, aphakia, ocular trauma, intraocular surgery, prior suprachoroidal hemorrhage, choroidal hemangioma, and a preoperative elevation in IOP.
No. 3: Intraoperative. General, retrobulbar, or peribulbar anesthesia; Valsalva-type maneuvers; hypotony or an acute drop in IOP; and prolonged or complicated surgery (eg, vitreous loss during cataract surgery) are associated with an increased risk of suprachoroidal hemorrhage.
No. 4: Postoperative. Risk factors in the postoperative period include hypotony, emesis, and Valsalva-type maneuvers.
2. CLINICAL SIGNS
There are commonalities among the clinical symptoms of suprachoroidal hemorrhage in the pre- and intraoperative periods, but signs can also be seen postoperatively. Common intraoperative signs include anterior chamber shallowing, loss of the red reflex, an increase in IOP, bulging of the posterior capsule, and extrusion or prolapse of intraocular contents. Postoperative signs include severe eye pain, headache, nausea with or without vomiting, significantly decreased visual acuity, vitreous prolapse into the anterior chamber, and choroidal elevation.3
3. DIAGNOSIS
Intraoperatively, the diagnosis of suprachoroidal hemorrhage can be confirmed with examination and observation of the clinical signs. Suprachoroidal hemorrhage can be challenging to diagnose in the postoperative period secondary to inflammation, corneal edema, or poor pupillary dilation. Several modalities can aid the diagnosis of suprachoroidal hemorrhage, but the most helpful initial imaging modality is ultrasonography (A- and B-scan). The initial B-scan of a suprachoroidal hemorrhage shows an irregular shape with hyperechoic clots. Over time, as the clot dissolves, the irregular shape becomes more hypoechoic, homogenous, and dome-shaped in appearance. A-scan ultrasonography can show changes in the clot’s density over time.
4. MANAGEMENT
The initial best step for managing a suprachoroidal hemorrhage is early detection. Once a hemorrhage is suspected, it is important to close the wound immediately. This can help tamponade bleeding vessels and prevent the prolapse of intraocular materials. If necessary, an OVD can be injected to deepen the anterior chamber, prevent extrusion of the intraocular contents temporally, and provide more room for wound suturing when necessary.4,5
IOP control is important during the postoperative period. This can be accomplished initially with topical beta blockers and, if necessary, the addition of an oral carbonic anhydrase inhibitor. Ocular inflammation is typically managed with topical steroids. Cycloplegics can be used to prevent lens-cornea or iris-cornea touch, which can help relieve one source of pain.3 NSAIDs and aspirin are contraindicated because their antiplatelet function increases the risk of bleeding, but other oral analgesics can be used.
Reoperation or drainage can be considered if conservative measures do not resolve the hemorrhage. Reoperation may also be considered if appositional choroidals, uncontrolled IOP, persistently high levels of pain, or retinal detachment occur and do not resolve with medical management. Typically, the two surgeries are timed about 14 days apart to allow liquification of the suprachoroidal hemorrhage and dissolution of the clot.6
5. Timing
The timing for drainage of a suprachoroidal hemorrhage varies among studies. One approach is to wait weeks after the initial development to allow sufficient time for clot lysis. Immediate intraoperative drainage increases the risk of further bleeding if the clot is dislodged. More conservative management is generally favored, and patients are closely observed in the postoperative period. Traditionally, a suprachoroidal hemorrhage is drained via a posterior sclerotomy, but alternative surgical options with transscleral trocars can be used. Use of trocars or posterior sclerotomy may avoid the need for more invasive procedures such as pars plana vitrectomy.7
CONCLUSION
Suprachoroidal hemorrhage is a rare complication that can cause significant vision loss. Suprachoroidal hemorrhages most often occur after glaucoma surgery, which can produce an acute change in IOP that tears vessels in the choroid. If a suprachoroidal hemorrhage occurs intraoperatively, it is imperative to secure the wounds and restore a closed system. Postoperative management should focus on pain and IOP control, and the patient should be monitored closely for sequelae such as retinal detachment.
1. Roa T, De La Rosa S, Netland P. Five pointers on choroidal effusion and suprachoroidal hemorrhage. Glaucoma Today. 2019;17(4):37-39.
2. Chu TG, Green RL. Suprachoroidal hemorrhage. Surv Ophthalmol. 1999;43(6):471-486.
3. Koksaldi S, Utine CA, Kayabasi M. Management of suprachoroidal hemorrhage during cataract surgery: a case report. Beyoglu Eye J. 2022;7(1):66-70.
4. Foo R, Tsai A, Lim L. Management of suprachoroidal hemorrhage. EyeNet Magazine. May 2018. Accessed January 16, 2023. https://www.aao.org/eyenet/article/management-of-suprachoroidal-hemorrhage
5. Wolter JR, Garfinkel RA. Ciliochoroidal effusion as precursor of suprachoroidal hemorrhage: a pathologic study. Ophthalmic Surg. 1988;19(5):344-349.
6. Learned D, Eliott D. Management of delayed suprachoroidal hemorrhage after glaucoma surgery. Semin Ophthalmol. 2018;33(1):59-63.
7. Rezende FA, Kickinger MC, Li G, Prado RF, Regis LG. Transconjunctival drainage of serous and hemorrhagic choroidal detachment. Retina. 2012;32(2):242-249.