 Modern cataract surgery has become much more than a rehabilitative procedure—now it is also a refractive procedure. In this new era of cataract surgery, toric IOLs play a major role in helping patients with preexisting corneal astigmatism to achieve excellent postoperative outcomes.
Toric IOLs are becoming the standard of care; however, the results following implantation are not always predictable. We recently introduced a new regression formula that should help to improve the predictability of these results.
Modern cataract surgery has become much more than a rehabilitative procedure—now it is also a refractive procedure. In this new era of cataract surgery, toric IOLs play a major role in helping patients with preexisting corneal astigmatism to achieve excellent postoperative outcomes.
Toric IOLs are becoming the standard of care; however, the results following implantation are not always predictable. We recently introduced a new regression formula that should help to improve the predictability of these results.
DON’T FORGET THE POSTERIOR CURVATURE
Because standard keratometric and topographic devices only measure the anterior cornea and assume a fixed ratio between the anterior and posterior curvature, they tend to inaccurately assess the total corneal astigmatic power. Yet, as we know from Koch et al,1 the posterior cornea tends to be steepest along the vertical meridian, thus creating a net plus power along the horizontal meridian, or against-the-rule astigmatism. In translation, the posterior corneal curvature will decrease the net astigmatism in eyes that have with-the-rule astigmatism and will increase the net astigmatism in eyes that have against-the-rule astigmatism. Koch et al1 also found that, in eyes that had with-the-rule astigmatism, greater anterior steepening correlated to greater posterior steepening; on the other hand, there was no such correlation in magnitude of astigmatism in eyes that had against-the-rule astigmatism. The Baylor nomogram was the first step to addressing the issue of predictability.A NEW FORMULA
Since the Baylor nomogram was published, a great deal of work has been done to refine our understanding of posterior corneal astigmatism and to find more accurate ways to incorporate it into daily practice. Three popular solutions are intraoperative aberrometry, the use of a standard toric IOL calculator with either a nomogram or direct measurements of the posterior corneal astigmatism, and the use of a next-generation toric IOL calculator such as the Barrett Toric IOL calculator. The Abulafia-Koch formula, which is based on a regression model and has recently been incorporated into PhysIOL’s toric IOL calculator, compensates for the effect of posterior corneal astigmatism. Our formula takes anterior curvature–based corneal measurements and calculates a new net corneal astigmatism with a new magnitude and a new meridian. The usefulness of the Abulafia-Koch formula was verified during a retrospective case series2 comparing the accuracy of two toric IOL calculators (Alcon and Holladay calculators) with and without the Abulafia-Koch formula to the accuracy of the Barrett Toric IOL calculator, which uses a mathematical model to compensate for the posterior corneal astigmatism. For developing the Abulafia-Koch formula, we used biometry data from the Ein-Tal eye center in Israel, and for validation we used biometry measurements data from the Lion Eye Institute in Australia.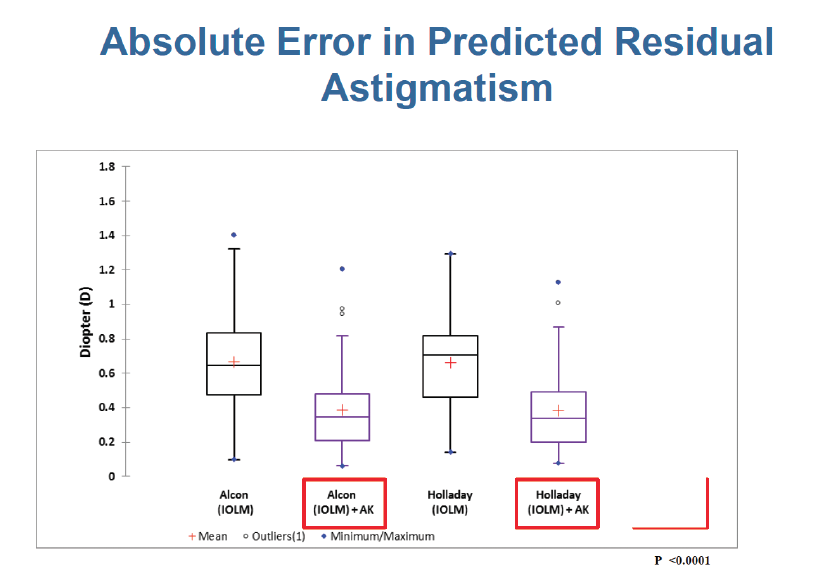
Figure 1. Absolute error in predicted residual astigmatism.
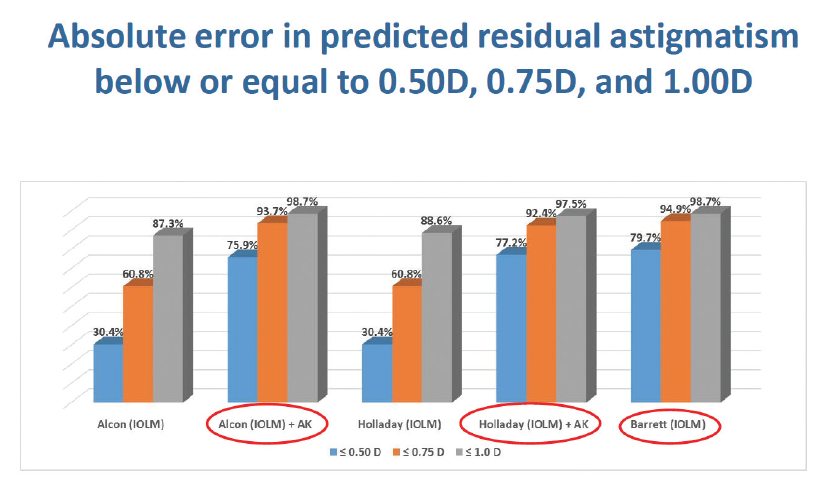
Figure 2. Absolute error in predicted residual astigmatism below or equal to 0.50, 0.75, and 1.00 D.

Figure 3. Errors in predicted residual astigmatism with the Alcon and Holladay formulas alone (top row) and the formulas modified with the Abulafia-Koch nomogram (bottom row).
CONCLUSION
The prediction of postoperative astigmatic outcomes can be optimized by adjusting standard toric IOL calculators with the Abulafia-Koch formula. I congratulate PhysIOL for this new and wonderful calculator update, which takes into account the effective lens position in order to calculate the IOL cylinder power at the corneal plane and incorporates the Abulafia-Koch formula, which can be toggled on and off by the user.
1. Koch, DD, et al. Contribution of posterior corneal astigmatism to total corneal astigmatism. J Cataract Refract Surg, 2012;38(12):2080-2087.
2. Abulafia A, Koch DD, Wang L, et al. New regression formula for toric intraocular lens calculations. J Cataract Refract Surg. 2016.
