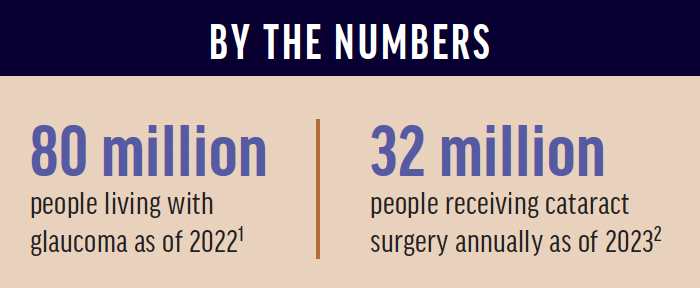
Glaucoma and cataract are prevalent conditions that will be of increasing concern as the population ages (see By the Numbers).1,2 Approximately 6 million patients with glaucoma or ocular hypertension undergo cataract surgery every year3; however, many do not receive the opportunity to address their glaucoma at the time of their cataract procedure.
Cataract surgery may yield some IOP lowering, but it is not enough to change the course of glaucoma. In the Ocular Hypertension Treatment Study,4 cataract surgery lowered IOP by 1.3 to 2.2 mm Hg, but this reduction was not significant at 1 year. The medication burden was reduced by only 0.4 medications at 2 years. Randomized controlled trials have shown that performing MIGS at the time of cataract surgery (phaco+MIGS) can yield better and longer IOP control, reduce the medication burden, and eliminate some patient-dependent aspects of care.5
Phaco+MIGS: Advantages and Lessons
Performing MIGS at the time of cataract surgery offers several advantages. Surgical control of IOP can minimize diurnal fluctuation, which may slow disease progression.6-8 Phaco+MIGS may also reduce the rate of functional deterioration and the need for secondary surgical interventions.5 Reduction of drops after phaco+MIGS can improve the ocular surface and increase tear film stability.9 In one study, 79% of patients reported an overall improvement in quality of life after phaco+MIGS.10
More than a decade of MIGS experience shows that achieving the same or lower IOP with a lower medication burden is a valid treatment goal. It has become clear that “phaco-like” safety is a must for glaucoma procedures performed at the time of cataract surgery. Low technical complexity broadens surgeon uptake and patient access. Further, avoiding retained devices may be advantageous. These insights can assist in the evaluation of emerging technologies and their potential in glaucoma care.

Phaco+MIGS With ELIOS
Excimer laser trabeculostomy (ELIOS) is a clinically validated MIGS procedure performed with the ELIOS excimer laser (Bausch & Lomb). The procedure creates 10 microchannels (210 µm) in the TM to facilitate aqueous outflow into Schlemm’s canal and reduce IOP. ELIOS preserves the TM, is implant-free, and is broadly adoptable by surgeons. Combined with phacoemulsification, ELIOS provides an opportunity to address cataract and glaucoma—a valuable pursuit in the effort to optimize quality of life.
1. Tham YC, Li X, Wong TY, et al. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121(11):2081-2090.
2. Data on file with Elios Vision.
3. Hughes R, Aristodemou P, Sparrow JM, et al. Surgeon effects on cataract refractive outcomes are minimal compared with patient comorbidity and gender: an analysis of 490 987 cases. Br J Ophthalmol. 2023;107(4):488-494.
4. Mansberger SL, Gardiner SK, Gordon M, et al. Cataract surgery lowers intraocular pressure and medication use in the medication group of the Ocular Hypertension Treatment Study. Am J Ophthalmol. 2022;236:53-62.
5. Montesano G, Ometto G, Ahmed IIK, et al. Five-year visual field outcomes of the HORIZON trial. Am J Ophthalmol. 2023;251:143-155.
6. Pyfer MF, Gallardo M, Campbell A, et al. Suppression of diurnal (9AM-4PM) IOP fluctuations with minimally invasive glaucoma surgery: an analysis of data from the prospective, multicenter, single-arm GEMINI study. Clin Ophthalmol. 2021;15:3931-3938.
7. Posarelli C, Ortenzio P, Ferreras A, et al. Twenty-four-hour contact lens sensor monitoring of aqueous humor dynamics in surgically or medically treated glaucoma patients. J Ophthalmol. 2019;2019:9890831.
8. Asrani S, Zeimer R, Wilensky J, et al. Large diurnal fluctuations in intraocular pressure are an independent risk factor in patients with glaucoma. J Glaucoma. 2000;9:134-142.
9. Jones L, Maes N, Qidwai U, et al. Impact of minimally invasive glaucoma surgery on the ocular surface and quality of life in patients with glaucoma. Ther Adv Ophthalmol. 2023;15:25158414231152765.
10. Al Habash A, Nagshbandi AA. Quality of life after combined cataract and minimally invasive glaucoma surgery in glaucoma patients. Clin Ophthalmol. 2020;14:3049-3056.


