Introduction
Cataract surgery is the most common ophthalmic surgery performed worldwide. More than 26 million cataract surgeries are performed annually. Driven by demographic changes and access to more medical services, procedure volume is growing at a compound annual rate of 3.1%.1
Phacoemulsification is the gold-standard treatment for cataract patients.2 The application of ultrasonic (US) energy during phacoemulsification can carry the risk of endothelial cell loss and tissue damage, especially in hard cataracts.3 In the conventional US mode, needle-tip movement is longitudinal, which can result in decreased cutting efficiency as the back-and-forth movement of the tip pushes away the nucleus.4
In 2006, torsional ultrasound (OZiL, INFINITI Vision System; Alcon Laboratories) was proposed.5 Torsional US mode uses rotary oscillations at US frequencies to emulsify cataractous lens material in a seamless cutting motion from a tip that oscillates laterally.5,6 The side-to-side movement of the phaco tip produces minimal repulsion of lens material, resulting in improved followability7 and more effective lens removal with torsional US in comparison to the conventional US mode.5-7 Torsional phacoemulsification produces less heat than longitudinal phacoemulsification and may provide thermal protection or reduce risk of wound burn.8,9 Torsional phacoemulsification's advantages, including improvements in energy delivery, thermal profiles, and machine fluidics, have been shown in laboratory studies.6,8-10 Experimental data were supported by clinical study results.2,7,11 Vasavada et al conducted a prospective, randomized, masked clinical trial to compare the intraoperative efficacy and postoperative outcomes of torsional ultrasound versus longitudinal ultrasound phacoemulsification procedures. Shorter surgical time (4.40 ± 1.37 and 6.65 ± 2.48 min, P < 0.05) and lower fluid volume (101 ± 40.44 mL and 125 ± 37.76 mL, P < 0.05) use with torsional US is a demonstration of improved surgical efficiency when compared to longitudinal phaco technology. The postoperative assessment showed significantly less increase in corneal thickness in the torsional group on the first postoperative day (67.2 ± 21.0 vs 83.6 ± 49.0, P < 0.01). The decrease in the endothelial cell density also favored the torsional group (3.3 ± 0.8 vs 5.6 ± 2.5, P < 0.001), indicating improved endothelium protection (Figure 1).7
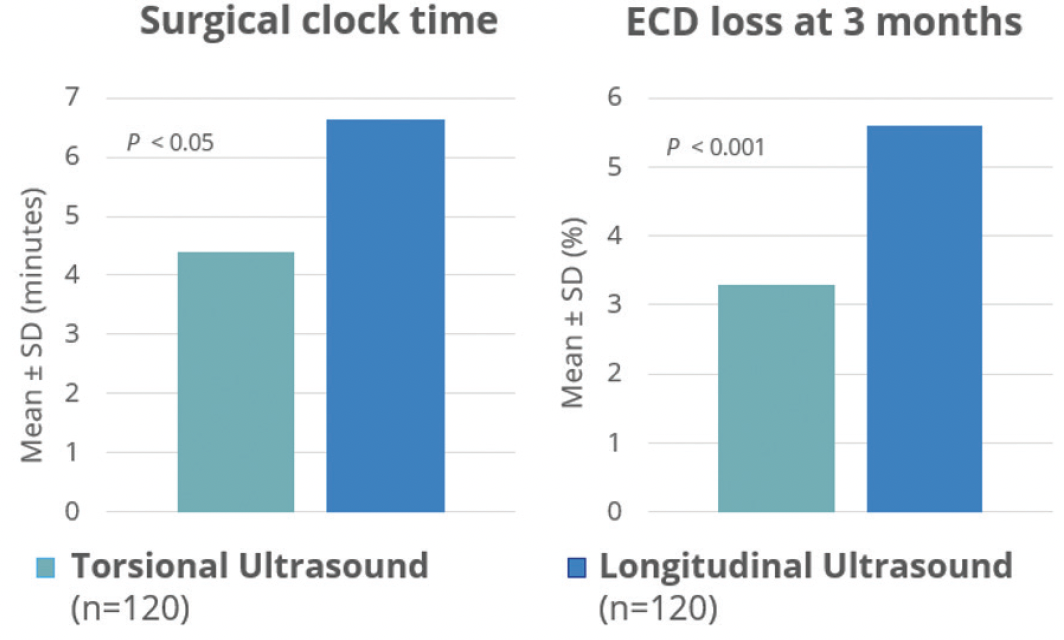
Figure 1. Surgical efficiency and patient outcomes (Vasavada et al, 2010).

Legion® System
The LEGION® System (Alcon) is a compact, advanced, gravity-based phacoemulsification platform. The LEGION® System uses OZil® torsional phacoemulsification technology (including OZil® Intelligent Phaco [IP] software; Alcon) and CENTURION®-based gravity fluidics (Alcon). The system is compatible with a range of accessories (Figure 2).12
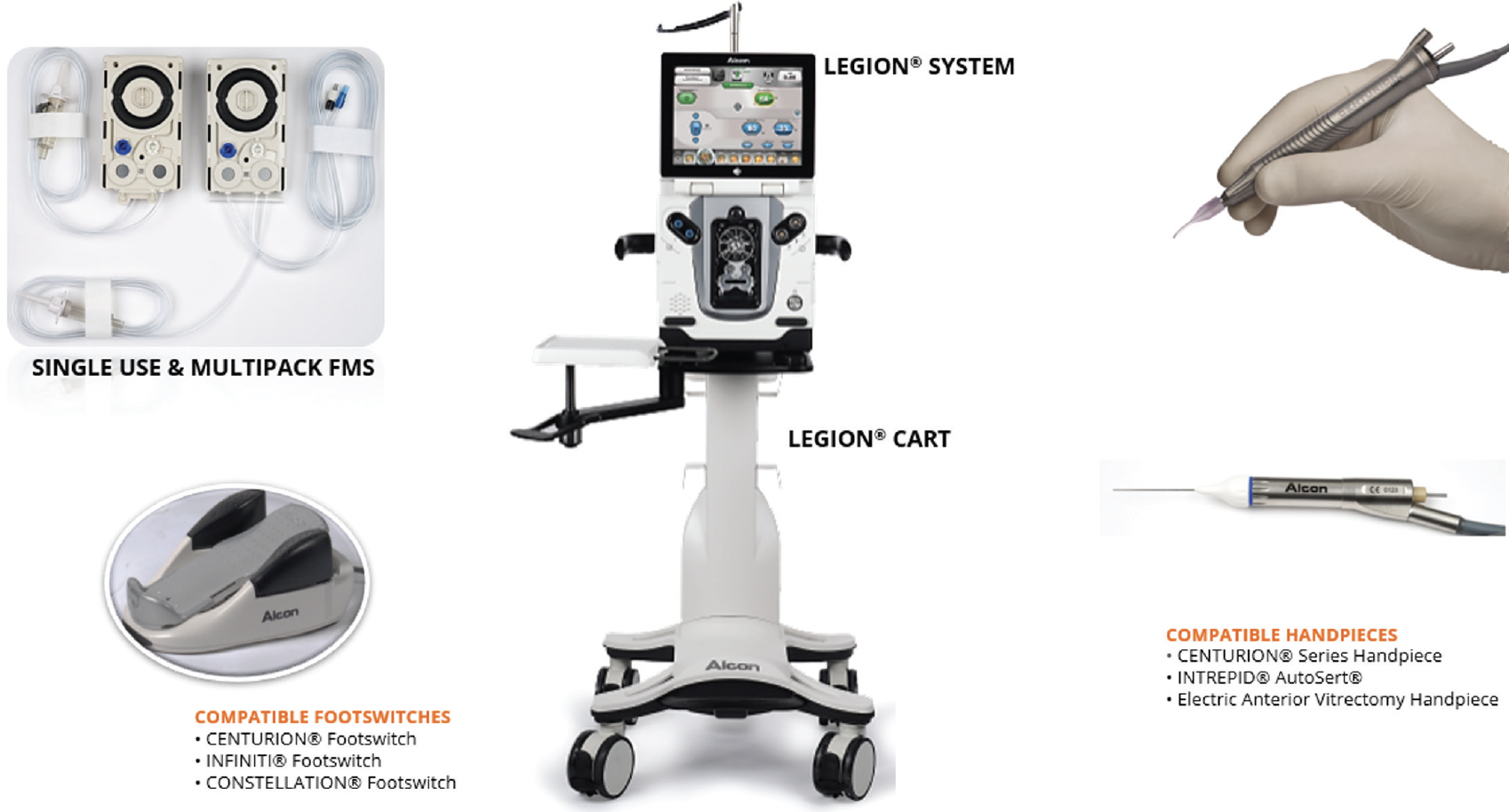
Figure 2. LEGION® System components.
The CENTURION®-based Fluidic Management System (FMS; Alcon) used for the LEGION® contains a rotary vent valve that is designed to provide precise venting control versus the INFINITI® system's (Alcon) non-adjustable on-off vent valve. Also, the CENTURION®-based FMS contains the optical vacuum pressure sensor that is designed to increase precision in vacuum detection versus the INFINITI® mechanical sensor (Figure 3).12,13

Figure 3. The Fluidic Management System (FMS) includes a rotary vent valve (1a), on-off vent valve (1b), optical vacuum pressure sensor (2a), and mechanical sensor (2b).
Legion® System clinical data
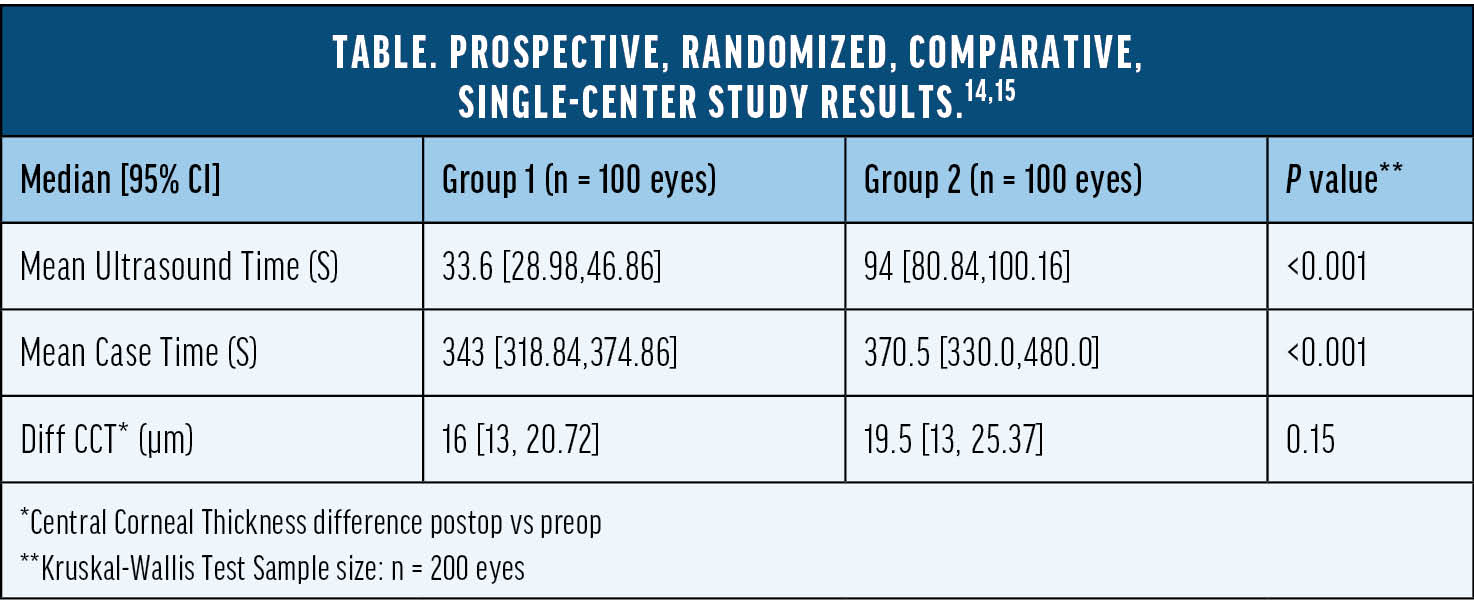
LEGION® system clinical performance data has been recently presented at international congresses.14-16 Shetty et al conducted a prospective, randomized, single-center study to compare surgical efficiencies and outcomes between torsional and transversal phacoemulsification. Two hundred eyes (all grades of cataract) of 200 patients were randomized into torsional (OZil® technology LEGION® system: group 1, n = 100) and transversal phacoemulsification (Ellips FX Technology Sovereign Compact: group 2, n = 100) study groups. Two experienced surgeons performed phacoemulsification using either torsional or transversal technologies as per randomization. The recorded surgical video was assessed for various parameters such as chatter, followability, chamber stability, etc., by a third independent surgeon using the questionnaire grading of surgical video recording. Mean US time and mean case time were significantly less in group 1. The postoperative versus preoperative central corneal thickness (CCT) difference was more in group 2 when compared to group 1, but was not significantly different (Table). Better followability, ease of chopping, and reduced chatter was noted in group 1 based on the surgical video assessment.14,15


Conclusions
Advances in phacoemulsification technologies may lead to better clinical outcomes in patients undergoing cataract surgery. The LEGION® system, with its torsional ultrasound capability and advanced surge protection, enables surgical efficiency and good postoperative outcomes.
© 2023 Alcon Inc. 12/23 IMG-LGN-2300004
1. Xinyi Chen, Jingjie Xu, Xiangjun Chen, Ke Yao. Cataract: Advances in surgery and whether surgery remains the only treatment in future. Advances in Ophthalmology Practice and Research. 2021;1(1):100008.
2. Leon P, Umari I, Mangogna A, Zanei A, Tognetto D. An evaluation of intraoperative and postoperative outcomes of torsional mode versus longitudinal ultrasound mode phacoemulsification: a meta-analysis. Int J Ophthalmol. 2016;9(6):890-897.
3. Kim DH, Wee WR, Lee JH, Kim MK. The comparison between torsional and conventional mode phacoemulsification in moderate and hard cataracts. Korean J Ophthalmol. 2010;24(6):336-340.
4. Zacharias J. Role of cavitation in the phacoemulsification process. J Cataract Refract Surg. 2008;34(5):846–852.
5. Liu Y, Zeng M, Liu X, et al. Torsional mode versus conventional ultrasound mode phacoemulsification: randomized comparative clinical study. J Cataract Refract Surg. 2007;33(2):287-292.
6. Davison JA. Cumulative tip travel and implied followability of longitudinal and torsional phacoemulsification. J Cataract Refract Surg. 2008;34(6):986-990.
7. Vasavada AR, Raj SM, Patel U, Vasavada V, Vasavada V. Comparison of torsional and microburst longitudinal phacoemulsification: a prospective randomized, masked clinical trial. Ophthalmic Surg Lasers Imaging. 2010;41(1):109-114.
8. Han JK, Miller KM. Heat production: longitudinal versus torsional phacoemulsification. J Cataract Refract Surg. 2009;35(10):1799–1805.
9. Jun B, Berdahl JP, Kim T. Thermal study of longitudinal and torsional ultrasound phacoemulsification; tracking the temperature of the corneal surface, incision, and handpiece. J Cataract Refract Surg. 2010;36:832–837.
10. Ryoo NK, Kwon JW, Wee WR, Miller KM, Han YK. Thermal imaging comparison of Signature, Infiniti, and Stellaris phacoemulsification systems. BMC Ophthalmology. 2013;13:53.
11. Christakis PG, Braga-Mele RM. Intraoperative performance and postoperative outcome comparison of longitudinal, torsional, and transversal phacoemulsification machines. J Cataract Refract Surg. 2012;38:234–241.
12. LEGION® System Operator’s Manual.
13. INFINITI® Vision System Operator’s Manual.
14. Shetty N. Comparison of Intraoperative Efficiencies and Surgical Outcomes Between Two Operating Systems: Torsional (Ozil Technology) Versus Transversal (EllipsFx Technology) Ultrasound Systems. The 38th Asia-Pacific Academy of Ophthalmology Congress, February 2023.
15. Srinath H, Shetty N. Comparing Surgical Efficiencies and Outcomes between Torsional and Transversal Phacoemulsification. The 35th Annual Meeting of the Asia-Pacific Association of Cataract and Refractive Surgeons, June 2023.
Refer to Operator's manual for the list of indications, warnings and precautions. Market-specific safety information may be required.




