I began using femtosecond laser-assisted cataract surgery (FLACS) regularly as soon as I entered clinical practice, where 80% to 90% of my cataract surgeries included some form of advanced technology. I quickly decided that the laser technique was superior to manual cataract surgery. Although I think I execute manual cataract surgery uniformly and efficiently, there is greater variability and more opportunity for a complication, however rare. To me, FLACS feels safer and more predictable than a manual cataract technique.
How the ALLY® Adaptive Cataract Treatment System Improves Surgery
I have used several different femtosecond lasers in my career, but I prefer the ALLY Adaptive Cataract Treatment System (Lensar). This laser offers specific advantages that I feel will help increase the adoption of femtosecond lasers in the market. The number of ophthalmic surgeons who have access to a femtosecond laser and use it on a regular basis still hovers around 4% in the global marketplace.1 Part of this low adoption rate may be the perception that FLACS is slower than manual cataract surgery. I think the ALLY addresses that concern in three ways: its speed, its workflow, and its astigmatism management.
Speed
The ALLY laser is exceptionally fast. I recently completed a case with less than 40 seconds of suction time, and my average is between 45 seconds and 1 minute 20 seconds, depending on the case. A skilled surgeon may be able to do the incisions, LRIs, and a manual capsulotomy in 1 minute 20 seconds, but not with pre-chopping the lens. The speed of a laser-assisted capsulotomy is a huge advantage.
Workflow
Having tried various configurations of the ALLY laser’s OR setup and observing how others do it, I am a huge proponent of using a sterile laser arrangement, meaning I use a dedicated femtosecond laser in each OR. My colleagues and I conducted a timed single-site study with ALLY, the endpoints being total surgeon case time and total patient case time.2 We found a significant time savings—approximately 7 minutes per case for the surgeon and approximately 14 minutes for the patient—by using two sterile ALLY lasers in two ORs (Figures 1 and 2). In contrast, using one laser between two ORs produces a gap between the laser and the phaco time, not including time for prepping and draping the patient and other setup tasks. I think that high-volume cataract surgeons in particular will benefit from the efficient workflow of the sterile setup.
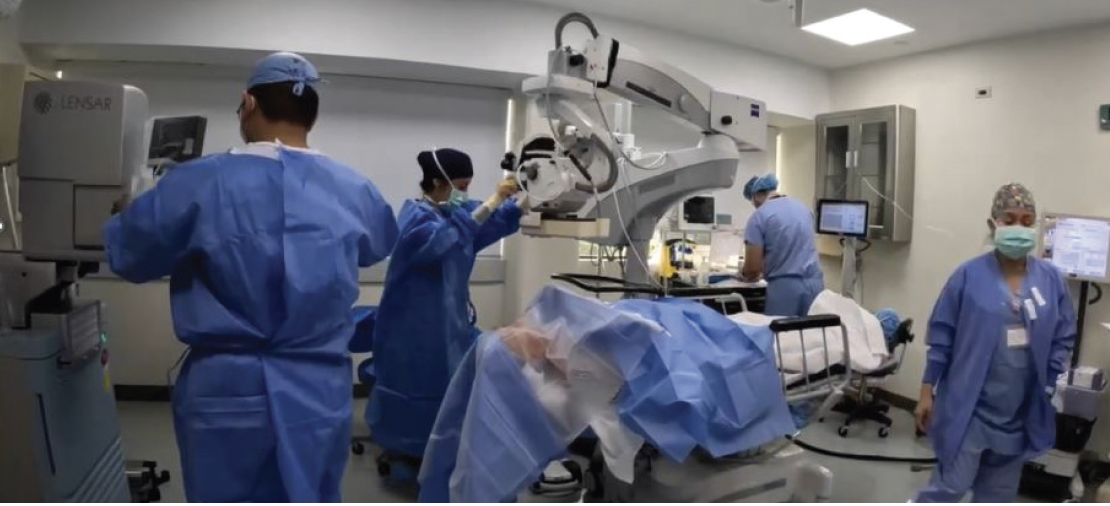
Figure 1. Dr. Nikpoor’s clinic has a dedicated LENSAR ALLY laser in each OR for a sterile setup.
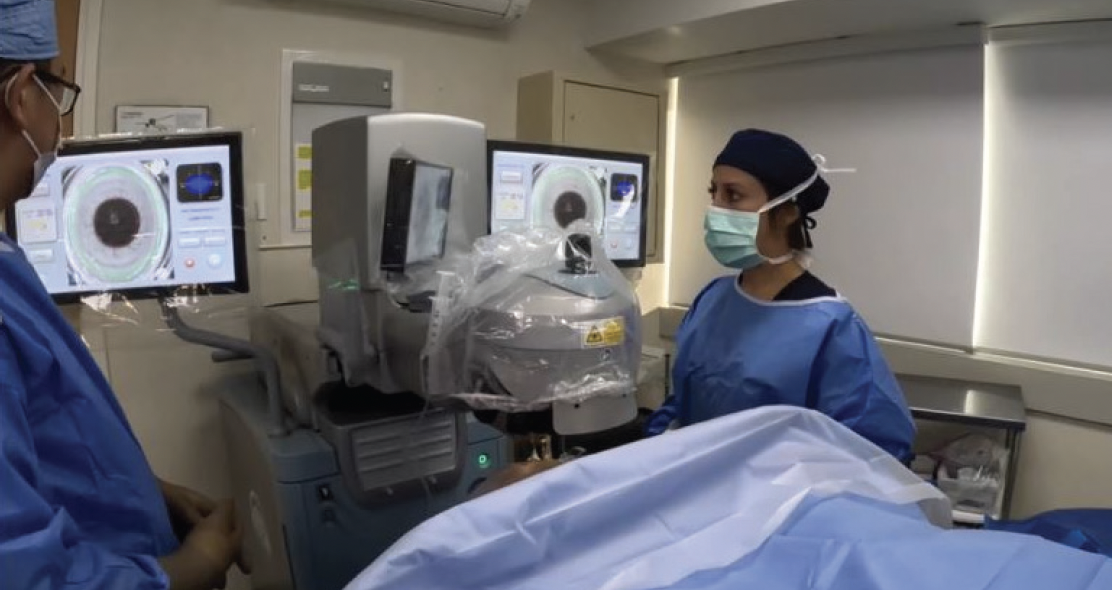
Figure 2. Dr. Nikpoor and her staff estimate saving 7 mins per case with a dedicated LENSAR laser.
Astigmatism Management
I consider the ALLY platform superior to other lasers in its astigmatism correction, thanks to the accuracy of its IntelliAxis capsule marks and iris registration. It performs these calculations automatically, thereby removing user bias or error. I estimate that I achieve good registration with the ALLY laser 98% of the time. While I was becoming familiar with this platform, I was simultaneously using other alignment and registration devices in the OR. Every time, the IntelliAxis capsule marks were the most accurate. Without the IntelliAxis capsule marks, I got cylinder, but with them, my outcomes were so much better. I have come to trust that these marks are highly accurate.
Advantages for Premium Cataract Procedures
Especially for toric, EDOF, and multifocal IOLs, it is important to use a femtosecond laser that makes careful arcuate incisions and performs optical axis centration of the capsulotomy. Interestingly, whereas every other laser makes arcuate incisions perpendicular to the tangent of the cornea, the ALLY makes them perpendicular to the coronal plane, so they are designed to slip instead of gape. Constructed this way, the incisions are less likely to regress. Robert Weinstock, MD, has published a good study showing the impressive stability of ALLY arcuate incisions at 1 year.3
CASE STUDY
Cataract Surgery in a Commercial Pilot With an Intrastromal Corneal Ring
A commercial pilot who required 20/20 BCVA bilaterally to continue working presented to me for cataract evaluation. His UCVA was 20/25 and his BCVA was 20/20-1 in the worse eye (sometimes he could make out the 20/20 line with correction, but not reliably), and his other eye was uninvolved. At this point, he was still passing his medical exams, but he was worried about his prescription changing or his vision worsening.
He had a previous diagnosis of keratoconus in the affected eye, for which he had undergone corneal cross-linking and received a Keraring intrastromal corneal ring (Mediphacos) outside the US. Despite the irregular topography, his UCVA was still 20/25, maybe 20/30 in that eye. In consulting with the optometrist in my practice, we were concerned that cataract surgery could worsen this patient’s prescription. He was just barely bothered by glare. I had a long conversation with the patient about the pros and cons of doing the surgery, and whether to implant an LAL or a toric IOL. He elected the surgery. During the examination, I found that the eye had significant scarring around the corneal ring, which was within the treatment zone for the LAL, so we decided against that lens and chose the toric option.
I wanted to use the IntelliAxis capsule marks, but I was concerned that the corneal ring and its surrounding scarring was within the ALLY laser’s firing zone and may block its passage, potentially causing an incomplete capsulotomy. So, in addition to the capsule marks, I placed tiny intrastromal marks on the cornea, 5º apart (the ALLY laser requires a 5º minimum).
Once the laser capsulorhexis was completed, I stained the cornea with trypan blue. Sure enough, an area of the capsulorhexis was incomplete, although it was just barely outside of the IntelliAxis capsule marks. I completed this part manually, and I was able to implant the lens on axis and use the capsulotomy marks and the corneal marks to help align the lens. I find that, because the IntelliAxis capsule marks are right next to the lens, there’s no parallax error, and so I am able to reliably place the lens where I want it. Ink marks on the cornea are simply less accurate, in my experience.
At the 1-week postoperative visit, this patient’s eye was seeing 20/25 UCVA, and at 1 month it was 20/15 -2 UCVA. He really had a “wow” reaction. He was very impressed that his vision was so much better than he thought it was going to be, given the irregularity of his cornea. I feel this outcome is a testament to the accuracy of the registration on the ALLY laser.
Device Collaboration and Saved Nomograms
There are two other benefits of the ALLY laser that I appreciate. First, it works with almost all topographers and biometers, which is very convenient. Second, it reduces the preplanning I have to do for premium cataract surgeries. I have saved my arcuate nomograms in the laser’s software, so I don’t have to preplan those incisions. I can simply click one button on the laser, and the arcuate incisions are planned according to my nomogram, accounting for age as well as astigmatism measurements. I can even toggle between TK and anterior astigmatism values from my biometer.
1. Market Scope: phaco and FLACS upgrades to drive expansion in cataract equipment market. Eyewire. Available at https://eyewire.news/articles/market-scope-phaco-and-flacs-upgrades-to-drive-expansion-in-cataract-equipment-market/?c4src=article:infinite-scroll. Accessed June 10, 2024.
2. Nikpoor N. Prospective analysis of time workflow and cost savings utilizing an all sterile femtosecond laser-assisted cataract surgery and phaco model. Presented at the annual meeting of the ASCRS. April 5-8, 2024; Boston, MA.
3. Weinstock RJ, et al. Comparison of regression of femtosecond laser arcuate incisions for astigmatism correction at the time of cataract surgery. Abstract presented at the annual meeting of the ASCRS; April 22-26, 2022; Washington, DC.


