I am the founder of the Toyos Clinic, which has offices in Memphis, Nashville, and New York City. I specialize in LASIK, cataract surgery, and dry eye disease (DED). I developed the use of intense pulsed light (IPL) for treating DED, and I have since trained many eyecare professionals, both nationally and internationally, on DED management and other ophthalmic therapies.
I am working with Lumibird Medical on various aspects of their DED products, such as the C.DIAG® and C.STIM® devices. We are developing unique features, clinical research, and physician education to assist clinicians with DED consultations. Here, I will describe my experience and the strategies I use to manage DED in my clinics, and the benefits to using C.DIAG® and C.STIM® in a dry eye consultation.
DEFINING DRY EYE DISEASE
To treat DED successfully, I believe we need to start by defining it accurately. I consider DED to be an inflammatory condition of the skin and glands, including the meibomian and lacrimal glands. Affected glands produce abnormal tears; it may be an isolated incident of inflammation, or it could be a sign of systemic disease such as rosacea, acne, rheumatoid arthritis, lupus, etc.
Approaching DED as a skin/glandular condition, instead of just an eye condition, broadens our approach to treatment. Rather than concentrating on finding the most effective artificial tears, we can start thinking of ways we might improve a patient’s systemic inflammatory condition. If we improve the skin, we will improve the glands. Thus, we must consider patients’ overall lifestyle, environment, and diet in our quest to get their glands working to produce their own natural tears.
IPL: MY STANDARD OF CARE FOR DED
When I opened an aesthetics clinic 26 years ago, dermatologists were using IPL to treat rosacea. I discovered that successive treatments of IPL successfully improved the symptoms of DED and also benefitted the surrounding skin. Although there are a variety of IPL devices available to treat DED, the one I have been developing with Lumibird Medical is the C.STIM®, which offers unique features to provide a safe and efficient treatment for most skin types (skin phototypes 1 through 5; Figure 1). An IPL device is crucial for my dry eye clinic, because making patients’ eyes look and feel better is paramount.

Figure 1. The C.STIM® IPL device is safe for skin phototypes 1 through 5.
The C.STIM®’s Unique, Patented Stim-ULI technology™
The C.STIM® represents next-generation IPL technology by integrating unique technical features to safely treat the skin around the eyes, which is the thinnest and most sensitive skin of the body. The handpiece of the C.STIM® device incorporates patented Stim-ULI™ (Uniform Light Intensity) technology, which ensures a perfectly even distribution of energy across the entire treatment window. The device delivers this energy in five regulated pulses (Figure 2). This “pulse train” technology is calibrated to give the skin thermal relaxation time (TRT) and prevent thermal damage, thereby minimizing any inflammatory reaction or burning on the skin (Figure 3). Combined, these features ensure a controlled energy accumulation for better results and a more comfortable treatment on the majority of skin types.
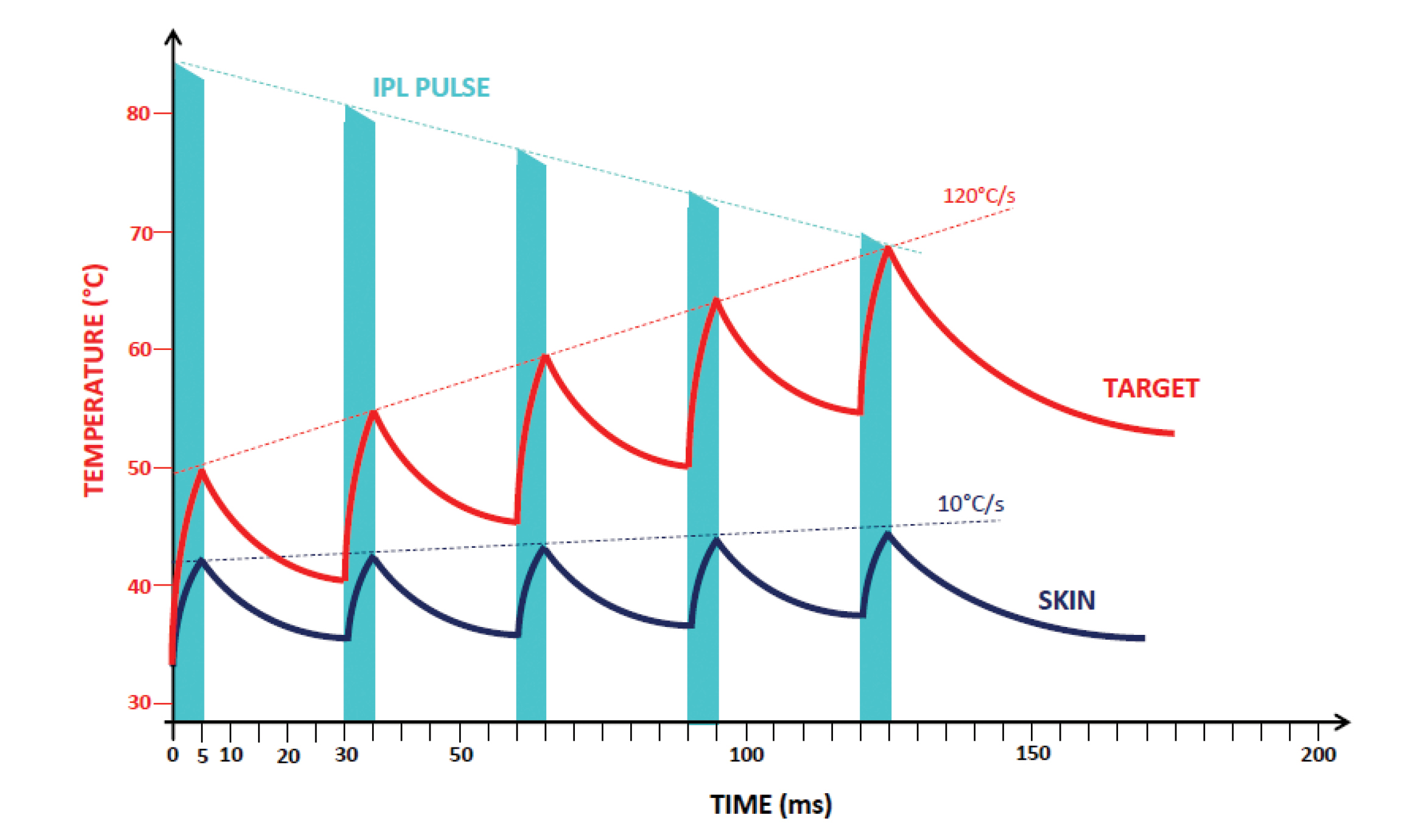
Figure 2. The handpiece of the C.STIM® device delivers a train of five spaced pulses to allow for thermal relaxation time that reduces the skin’s inflammatory reaction.

Figure 3. The patented Stim-ULI™ technology ensures a comfortable, safe, yet effective treatment.

THE IMPORTANCE OF A DIAGNOSTIC TOOL
Meibography for Diagnosis and Demonstration
The second most important purchase for a dry eye clinic is having a high-image-quality meibographer with transillumination that is simple to use and has print capabilities, so clinicians or their technicians can show patients what they mean when they’re talking about meibomian gland dysfunction (MGD) and DED. The C.DIAG® diagnostic aid platform is easy to use, and it provides five key measurements in 5 minutes: blinks, tear stability via noninvasive tear film breakup time (NIBUT), tear meniscus height, lipid analysis, and meibography.
The C.DIAG® uses standard infrared meibography to quantify the loss of meibomian glands (from the upper and lower eyelids), and it employs transillumination infrared meibography to produce a clear image that helps me qualify the functionality of the meibomian glands and see the telangiectasias that create inflammation (Figure 4). The infrared image is a powerful educational tool for me to explain a patient’s pathology and increase their treatment compliance.
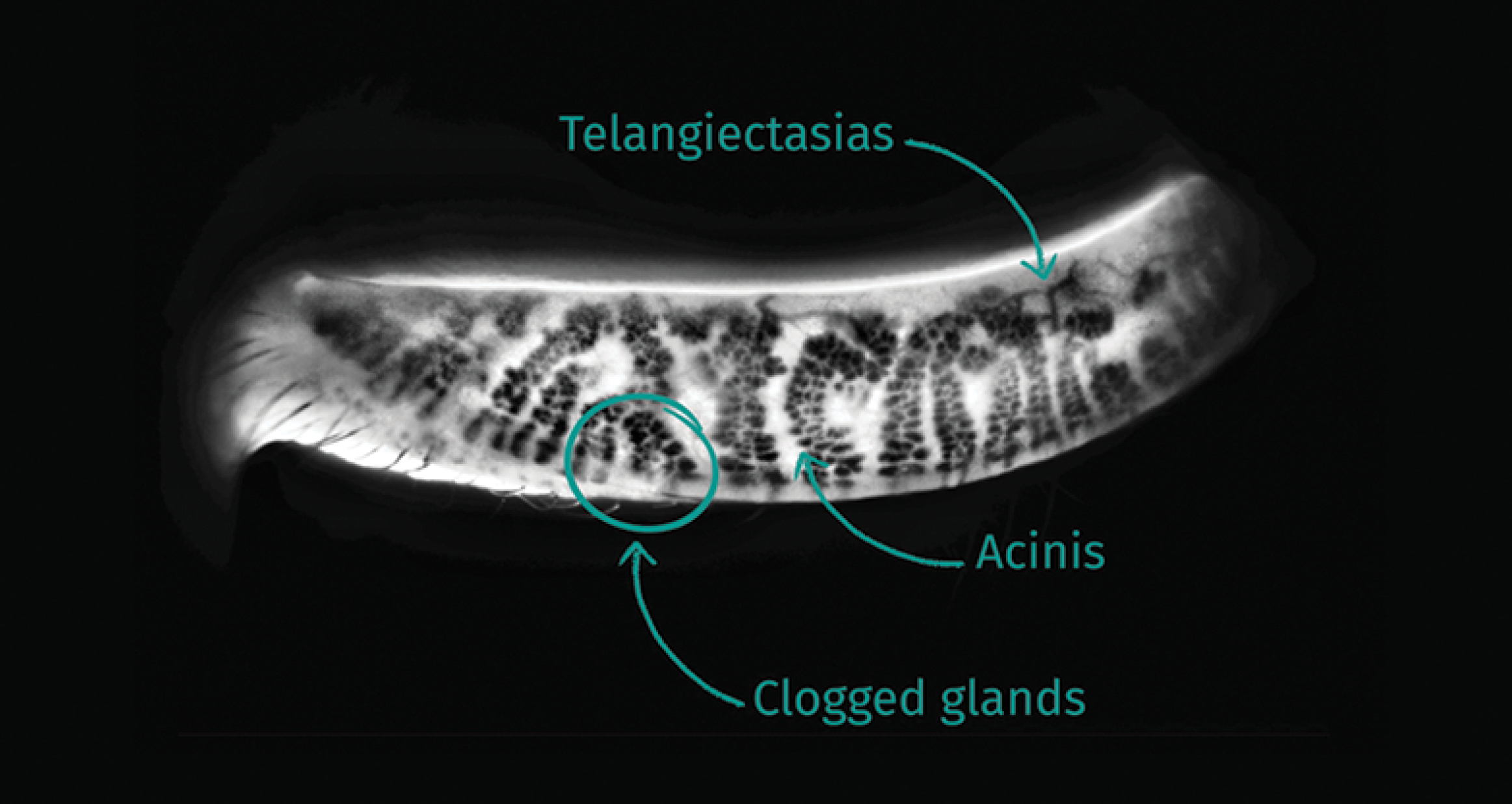
Figure 4. Transillumination infrared meibography performed with the C.DIAG®.
The C.DIAG® is a comprehensive and automated diagnostic platform with high-quality imaging that integrates the best advanced technologies, including a unique meibography, and all the essential ocular surface exams. I find this platform particularly useful when I am evaluating patients who have MGD and I’m trying to decide on what treatment paradigm to use.
Blinks, Tear Stability, and Tear Meniscus Height
Because an unstable tear film is part of the inflammatory cycle of DED, measuring the tear film’s stability with NIBUT is important. The blink analysis is another key examination to identify the source of DED, because insufficient blinks can lead to a lack of tears and ultimately MGD. The C.DIAG® evaluates the patient’s blink frequency and the percentage of the ocular surface not covered by blinks (Figure 5). The tear meniscus measurement helps me identify problems in the lacrimal glands. The C.DIAG® displays these readings in an easy-to-read report.

Figure 5. A Placido disk grid on the C.DIAG® is used to analyze tear film stability and blinks.
Lipid Analysis
Performing a lipid analysis allows me to assess the quality and quantity of the tear lipid layer, which provides even more detailed information on the health of the meibomian glands than may be visible on meibography or at the slit lamp. It is rare to find this function included in a meibographer. Lipid analysis can show the telltale “sausaging” of the glands that is often the first sign of MGD, as well as the quality of the secretions the eye is producing. The C.DIAG® evaluates the thickness of the lipid layer on a gradient scale based on Dr. JP Guillon’s international lipid grading scale.1
Ergonomics
Something else that impressed me about the C.DIAG® is its ergonomic features. It integrates a large HD screen and a powerful camera for an excellent image quality and better visualization of the eye and the eyelids. One feature I love is that the operator can zoom in on an image to examine the eyelashes and the surrounding area for signs of Demodex, blepharitis, or telangiectasias that will impact the treatment protocol.
The device is compact and can be easily integrated into a clinical environment. It features a highly user-friendly interface with a fast and efficient examination workflow. C.DIAG® is a unique platform whose operation can be easily delegated to the clinic’s staff.
The C.DIAG® Assists in Patient Education and Follow-Up
C.DIAG® and C.STIM® represent the perfect combination of diagnostics and treatment to fit a DED clinic’s needs. They play a crucial role in each step of managing DED patients. After completing all the examination functions on the C.DIAG®, I like to have a complete printout of the images and results, including the patient’s blink analysis, tear film stability, lipid analysis, tear meniscus, meibography, and eyelids/eyelashes in hand before I walk into the examination room. Patients are reassured by having a visual representation of my findings that explain the symptoms they experience daily with DED.

After diagnosing a patient with DED and then educating them on their treatment options, we need an imaging platform like C.DIAG® to follow the progression of their signs and symptoms over time. In my DED consultations, I perform a patient’s preliminary diagnosis, complete my IPL treatment protocol, and then bring the patient back a couple of months later to do a post-treatment analysis and compare the results. This is the final step in the patient’s treatment, and it gets the entire clinic involved in their healing journey. When patients can see the value of a treatment, they feel good about the investment they’ve made and will recommend it to others.
DED devices represent a vital investment for a DED clinic, both in terms of diagnostic accuracy and in educating and demonstrating to patients the severity of their disease and their treatment progress.
C.SUITE & PATIENT COMMUNICATION TOOLS
Lumibird Medical has developed C.SUITE (Figure 6), a comprehensive solution dedicated to DED management. This includes everything from diagnostics with C.DIAG® to IPL treatment using C.STIM®, along with patient education tools designed to enhance communication (Figure 7). These educational resources are invaluable in helping my staff and me inform our patients about chronic DED and the available treatment options.

Figure 6. The C.SUITE includes the C.DIAG® diagnostic aid platform (left), C.STIM® IPL system (right), and patient communication tools (see Figure 7).

Figure 7. Lumibird Medical makes a patient education kit for dry eye practitioners to use clinically.
Lumibird Medical supports us with printed materials such as flyers and videos for the waiting room, as well as IPL consent forms. In addition, they have developed digital tools to assist both patients and eyecare professionals. This includes the patient-centric website, www.mydryeyedisease.com, where patients can access information on DED, daily home care tips, tutorials, and monthly updates. The website also features a “Find a Specialist” page, enabling eyecare providers using the devices to create a profile with their office details, making it easier for patients to find nearby dry eye specialists.
The above mentioned resources are available by visiting www.mydryeyedisease.com
1. Guillon J.P. Non-invasive Tearscope Plus routine for contact lens fitting. Cont Lens Anterior Eye. 1998;21(Suppl. 1):S31–S40.


