Sponsored by Carl Zeiss

SOWWA ANATOLIY, MD
Ophthalmic Surgeon specializing in cataract,
glaucoma, and excimer laser surgery
Head of Center of Vision Rehabilitation of Anatoliy Sowwa
Honored Doctor of Ukraine
http://clinica-dr-sovva.com.ua; sowwa66@gmail.com
Case History
A 66-year-old retired female presented with closed-angle I glaucoma in her right eye and acute attack of closed-angle II glaucoma in her left eye. Both eyes showed pseudoexfoliation syndrome and weak cynic ligaments. The patient’s left eye was in remission from chronic uveitis, which was last aggravated 4 months prior to her presentation. Her left eye also had post uveitis, complicated cataract, posterior synechia, and a rigid narrow pupil. Both eyes presented with a high degree of hypermetropia and corneal astigmatism.
Therapeutic Strategy
I recommended ND YAG 1.44mkm laser (Rakot VI, Eye Microsurgery Complex, Russia) in both eyes, and phacoemulsification of the cataract in the left eye with implantation of the ZEISS CT LUCIA 601P IOL due to its biocompatibility. The patient’s preoperative visual acuity in the right eye was 0.5 / 0.7 with spherical + 6.0D, cylinder + 0.75D. The main incision and anti-incisions of the cornea were performed in a strong meridian of 175 degrees. The visual acuity in the left eye was 0.1 / 0.2 with spherical + 6.5D, cylinder + 0.75D, and an axis of 175. IOP with non-contact tonometry was 16.0 mm Hg in the right eye and 16.5 mm Hg in the left eye. In the right eye, the angle of the front chamber was closed all over. The angle of the front chamber in the left eye was also closed all over with the addition of goniosynechiae and glaucoma neuroopticopathy. The IOLMaster 500 revealed an axial length of 20.79 mm, ACD of 2.66 mm, and keratometry average of 46.84 D in the left eye. The calculation of the CT LUCIA 601P IOL for the left eye was 28.0 D; the estimated target refraction was -0.5D.
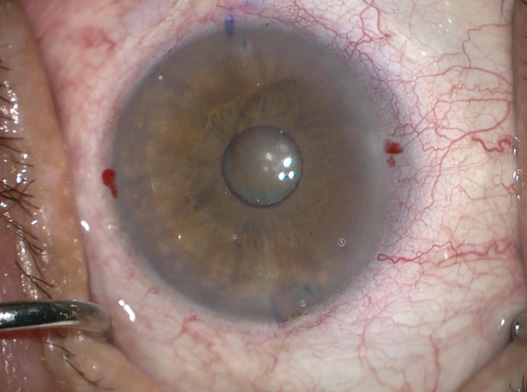
Before surgery.
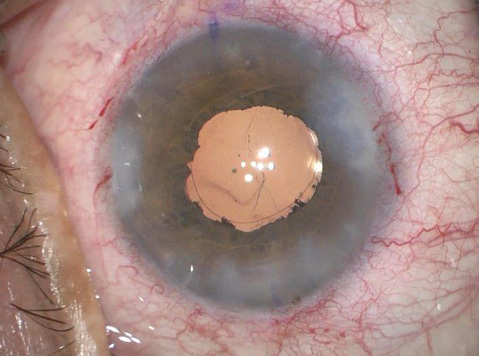
After surgery.
In the first stage of treatment, I performed YAG laser iridotomy on both eyes. In the second stage of treatment, I performed laser cataract phacoemulsification on the left eye with Rakot VI. During phacoemulsification, I created the main incision and anti-incision of the cornea in a strong meridian of 175 degrees. I then created a narrow rigid pupil and dissected the synched posterior with viscoelastic. I dilated the pupil with the help of four hooks of iris retractors superimposed on the iris, and I broke down the sphincter of the pupil. A continuous circular capsulorhexis revealed weakness of the cynical ligament at which point I shifted the hook Iris retractors with fixation beyond the anterior margin. I then facilitated capsulorhexis, hydrodissection, and rotation of the lens. I inserted an encapsulation bag into the capsular bag and performed laser phacoemulsification of the cataract followed by Intracapsular implantation of the CT LUCIA 601P IOL.

CT LUCIA 601P.
On the second postoperative day, the patient’s visual acuity in the left eye was 0.8 or 1.0 with spherical - 0.5D, cylinder + 0.25D, and an axis of 170. IOP with non-contact tonometry was 17.0 mm Hg. The angle of the anterior chamber was fully open. Glaucoma neuroopticopathy was present, and the central zone of the retina was unremarkable. Measurements with the IOLMaster 500 revealed an anterior chamber depth of 4.56 mm. The CT LUCIA 601P IOL was in the correct position, and there were minor tears of the sphincter of the pupil in the area where the iris retractors were used. There were no surgery complications.
On the fifth postoperative day, the visual acuity in the left eye was 0.9 – 1.0 / 1.0 clearer with spherical – 0.25 D, cylinder – 0.25D, and an axis of 80. IOP with non-contact tonometry was 14.0 mm Hg. The CT LUCIA 601P IOL position was correct and the postoperative course Oftaguixs (Santen Oy) and Medexol (World Medicine Ltd.) continued without complications.
BLUEJECT injector.
Conclusion
Biocompatibility and ease of use of are essential considerations that should be assessed prior to IOL selection and implantation, even in complicated cases. The CT LUCIA 601P IOL—a hydrophobic, aspheric monofocal IOL—showed good biocompatibility in the clinically complicated neovascular glaucoma eye with no recurrence of uveitis, despite the use of iris retractors. The IOL’s fully preloaded injection system and C-loop design optimize surgical workflow and visual outcomes.

