Arthur B. Cummings, MB ChB, FCS(SA), MMed (Ophth), FRCS(Edin)
I perform cataract surgery in at least one or two eyes that have previously undergone refractive surgery every week now, and it is certainly a growing part of my practice. Without doubt, these eyes present the biggest challenge to achieve emmetropia postoperatively, and these are the very patients who want accurate outcomes.
I find the American Society of Cataract and Refractive Surgery (ASCRS) online IOL Calculator (iolcalc.org) works well most of the time. Typically I use the average IOL power calculated, but I also find myself leaning toward the Haigis-L and modified Masket formulas. I often end up with an IOL choice somewhere between the average and the Haigis-L and Masket suggestions.
This very area of postrefractive surgery IOL power calculation is an unmet clinical need at this point in time, in my opinion. This is the reason that I became involved in a project called ClearSight, which has as its mission to provide LASIK-like outcomes for cataract surgery, including eyes that have undergone previous refractive surgery. I now run any postrefractive cataract case through our ClearSight work-up, which entails new hardware, software, and some ray tracing elements. (Editor’s note: For more information on ray tracing, read Ray Tracing for IOL Power Calculations, page 46.)
Arthur B. Cummings, MB ChB, FCS(SA), MMed (Ophth), FRCS(Edin), practices at the Wellington Eye Clinic & UPMC Beacon Hospital, Dublin, Ireland. Dr. Cummings is an Associate Chief Medical Editor of CRST Europe. He states that he has no financial interest in the products or companies mentioned. Dr. Cummings may be reached at tel: +353 1 2930470; fax: +353 1 2935978; e-mail: abc@wellingtoneyeclinic. com.
Laurie K. Brown, COMT, OSA, COE, OCS, CPSS (for I. Howard Fine, MD)
Beside meticulous surgical technique, one of the most important elements for a successful outcome of cataract surgery is the preoperative measurement of eye length. At our private practice in Eugene, Oregon, we have both optical coherence and ultrasound immersion biometry units available to ensure the most precise preoperative measurements for IOL power calculations. Our results are constantly evaluated and refined to maximize accuracy; specifically, we update our lens power calculations by analyzing postoperative outcomes and making fine alterations in our formulas’ personalized lens constants.
Instruments crucial to our success are the IOLMaster (Carl Zeiss Meditec) partial coherence interferometer, the Holladay IOL Consultant Software (Holladay Consulting), the OPD-Scan III Refractive Power/Corneal Analyzer (Marco), and the Optiwave Refractive Analysis System (ORA System; WaveTec Vision). It is because of these continued refinements and precise measurements before and during surgery that we are able to offer accurate lens power determinations.
CUSTOMIZE THE IOL SELECTION
Rather than utilizing only one IOL design at our practice, we customize the IOL selection for each patient, choosing not only the lens power but also the lens design and the biocompatible material based on each patient’s unique ophthalmic anatomy, pathology, and postoperative visual requirements. We take extra effort to perfect the postoperative refractive error so that the majority of our patients have, at a minimum, the best possible distance vision without glasses.
Our highly skilled technicians recurrently train for higher levels of certification, and many have achieved the highest level of training for ophthalmic technicians in the world. They play a significant role in the IOL calculation process for our patients. They vigorously evaluate each measurement they take for accuracy and effect on IOL power calculation, and their perspective is no different in the postrefractive surgery patient than it is in the virgin eye. Our technicians take an active role in evaluating each patient’s history, exam, and test findings.
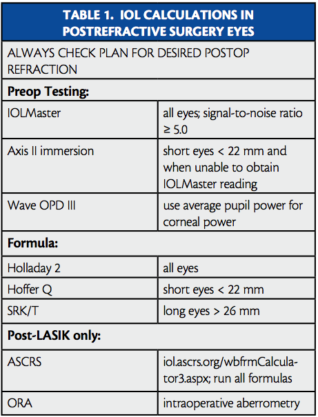
Due to the myriad available IOL power calculation formulas, an effective protocol is key to our success. With surgeons and technicians working together, we have established a protocol to obtain as accurate a preliminary calculation as possible. This protocol facilitates the surgeon’s final selection of IOL power (Table 1).
Laurie K. Brown, COMT, OSA, COE, OCS, CPSS, is an Administrator at Drs. Fine, Hoffman, Packer & Sims, Eugene, Oregon, and Dr. Fine is a member of the CRST Europe Editorial Board. Ms. Brown can be reached at tel: +1 541 687 2110; fax: +1 541 484 3883; e-mail: lkbrown@finemd.com.
John S.M. Chang, MD
To calculate IOL power in regular cataract patients, I use the following formulas: SRK/T, Haigis, Holladay II, and Hoffer Q. The latter is preferable when the patient’s axial length (AL) is less than 22 mm, and the Holladay II and SRK/T (personalized) formulas are more accurate if the patient’s axial length is greater than 27 mm. For eyes between 22 and 27 mm, SRK/T appears to be very accurate. In post-LASIK cases, my power calculation strategy is similar: Once corneal curvature is determined using keratometry (K), I apply the K reading to the formula the same way without any additional adjustment. For patients who have had LASIK, I mainly base my calculations on the clinical history method (CHM). The concept is as follows:
Post-LASIK K = Pre-LASIK K ( Preoperative Spherical Equivalent -Postoperative Spherical Equivalent).
DECIPHER THE CAUSE OF ERROR
Post-LASIK refractive errors can be the result of cataract formation (ie, myopic shift) or a change in corneal curvature (ie, myopic regression after LASIK). To determine how much of the postoperative refractive error is caused by the change in corneal curvature after LASIK, we use the postoperative refractive error up to the time the BCVA matches the preoperative BCVA for calculations.
Measurements in the contralateral eye also provide helpful data, as cataract formation is often faster in one eye than the other. Therefore, if the current visual acuity in the contralateral eye is comparable to the visual acuity in the operated eye before LASIK, the refraction in the contralateral eye will most likely reflect the amount of myopic regression from the cornea.
For example, Patient A had a plano refraction and 20/20 visual acuity in both eyes after LASIK. Five years postoperatively, Patient A presented with a cataract in the right eye. BCVA in this eye was 20/40 with a refraction of -4.00 D; BCVA was 20/20 in the left eye with a refraction of -1.00 D. We assume that the -1.00 D refraction in the left eye was from regression, and therefore, if we assume the same -1.00 D of regression took place in the right eye, then -3.00 D of the error in the right eye is due to cataract formation.
If a patient does not have available preoperative K readings, my next option is to use Sim K on the Orbscan (Bausch + Lomb). This reading is similar to the preoperative manual K and therefore can be used for CHM calculation. My final check comes from the ASCRS online calculator, which does not necessarily require preoperative K readings. This tool calculates IOL power based on pre- LASIK refractive error, pre-LASIK K, post-LASIK refractive error, and post-LASIK IOLMaster K. The modified Masket formula appears to be the most accurate; I use this Web site as a reference for the IOL power calculated by CHM.
TOUCH-UPS
I compare the corneal astigmatism from the pre- LASIK K reading with the amount of LASIK cylinder correction. If they differ, I tell the patient that he or she will most likely need a LASIK touch-up after cataract surgery to correct residual astigmatism.
This would be the case, for example, if Patient B’s corneal astigmatism (from pre-LASIK K reading) was 3.00 D while his manifest astigmatism (corneal astigmatism plus lenticular astigmatism) was only 1.00 D (LASIK cylinder correction). With monofocal IOL implantation, the manifest residual corneal astigmatism in Patient B will be approximately 2.00 D, which can be corrected with a LASIK touch-up.
John S. M. Chang, MD, is Director of the GHC Refractive Surgery Centre, the Hong Kong Sanatorium and Hospital, Happy Valley, Hong Kong. Dr. Chang is a member of the CRST Europe Global Advisory Board. He states that he has no financial interest in the products or companies mentioned. He may be reached at tel: +852 2835 8885; fax: +852 2835 8887; e-mail: johnchang@hksh.com.
H. Burkhard Dick, MD
My use of IOL power calculations has decreased, as I prefer to implant the Light Adjustable Lens (LAL; Calhoun Vision). With this IOL, the refractive properties of the lens are customized and adjusted postoperatively, allowing me to precisely correct residual refractive errors after the cataract is removed and the eye is stable, even in patients who have previously undergone laser vision correction with LASIK or PRK.
When I implant a standard monofocal, multifocal, or accommodating IOL, however, I use the Okulix ray tracing program (Tedics Peric & Jöher GbR) to calculate the IOL power individually. (For more information on ray tracing, read Ray Tracing for IOL Power Calculations, page 46.)
H. Burkhard Dick, MD, is the Chairman of the University Eye Hospital, Bochum, Germany. Professor Dick is a member of the CRST Europe Editorial Board. He states that he has consulted for, served on the speakers’ board of, or receieved research funding from the following: AcuFocus, ARC Laser, Bausch + Lomb, Abbott Medical Optics Inc., Alcon Laboratories, Inc., Allergan, Aquesys, Calhoun Vision, Domilens, Glaukos, Hoya Surgical, Morcher GmbH, Neovista, Novartis Pharma, Ophtec, Optos, Oculus, Rayner Intraocular Lenses Ltd., SMO, Transcenor, Optical Express, and Carl Zeiss Meditec. He may be reached at tel: +49 234 299 3101; e-mail: burkhard.dick@kk-bochum.de.
Erik L. Mertens, MD, FEBOphth
Calculation of the correct IOL power after previous refractive surgery is still a burden for cataract surgeons. One useful tool is the formulas incorporated into the ASCRS IOL power calculation software. The user can choose between calculations for eyes with previous myopic LASIK or PRK, previous hyperopic LASIK or PRK, and previous radial keratotomy (RK). The more data that can be plugged into these formulas, the more accurate the calculation of final IOL power can be.
POSTERIOR CORNEAL POWER
With that said, the accuracy of postrefractive surgery IOL power calculations is lacking in comparison with the calculations available for virgin eyes. In eyes that previously have undergone laser vision correction, the lack of accurate measurement of posterior corneal power is the main cause of residual refractive error; direct measurement of posterior corneal power is potentially the optimal solution.1 For this reason, I always choose an IOL power calculation formula that incorporates corneal power and pachymetry data. This information is derived from imaging with a proprietary Fourier-domain optical coherence tomography (FD-OCT) device such as the RTVue (Optovue), offering a predictive accuracy that is equal to or better than current standard methods for IOL power calculation in eyes with a history of laser vision correction.
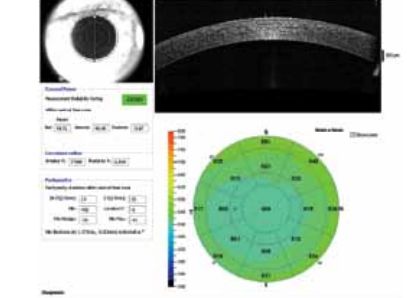
Figure 1. OCT can measure anterior and posterior corneal curvature and power in postrefractive surgery eyes.
Using conventional K readings for determining corneal power in postrefractive surgery eyes is problematic, as it incorrectly assumes a fixed relationship between anterior and posterior corneal curvature. For these eyes, a method is needed that can measure anterior and posterior corneal curvature and power, and OCT is one such modality (Figure 1). Compared with other techniques, OCT has very high spatial resolution and, now with FD-OCT technology, it also takes high-speed measurements.
A NEW FORMULA
Conventional IOL power calculation formulas cannot make use of FD-OCT corneal power values, as the measurement of net corneal power is approximately 1.00 D lower than the power determined by conventional keratometry, even in normal eyes. Because existing IOL power formulas are calibrated for conventional keratometry, a new formula, the FD-OCT IOL power calculation formula, is designed to accurately use the FD-derived corneal power value to determine IOL power. This formula is based on vergence calculations; a special formula for the effective lens position is calibrated to use the FD-OCT net corneal power value.
Inputs for the new formula include FD-OCT–measured net corneal power, anterior and posterior corneal powers, and central corneal thickness. Traditional parameters (ACD and AL determined using partial coherence or A-scan ultrasound biometry) are also included in the formula. This OCT-based IOL power calculation is accessible for free online through the Center for Ophthalmic Optics and Lasers (COOL) Web site at coollab.net/index. php?id=calculatordownload.
In my experience, the accuracy of the FD-OCT IOL power calculation method is higher than with any other tool available, making it an integral part of my preoperative diagnostic testing in cataract eyes that have previously undergone refractive laser surgery.
Erik L. Mertens, MD, FEBOphth, is Medical Director of Medipolis, Antwerp, Belgium. Dr. Mertens is a Co-Chief Medical Editor of CRST Europe. He states that he has no financial interest in the material presented in this article. Dr. Mertens may be reached at tel: +32 3 828 29 49; e-mail: e.mertens@medipolis.be.
Tang M, Wang L, Koch DD, et al. Intraocular lens power calculation after myopic and hyperopic laser vision correction using optical coherence tomography. Saudi Journal of Ophthalmology. 2012;26:19-24.
Kjell U. Sandvig, MD, PhD
The number of cataract patients who have previously undergone excimer laser surgery is increasing. If the refractive procedure was done in my own center, I have all the information needed for a reasonably accurate IOL calculation, such as preoperative K values and achieved change of refraction. In these cases, I use the CHM in addition to specially designed IOL power calculation formulas. My preference is the Haigis-L formula.
If the excimer surgery was performed elsewhere, which often is the case, my experience is that it is difficult to obtain preoperative data. Thus, I rely on only my own data. Upon examination, I routinely gather data needed for the Haigis-L formula, as it is included in the IOLMaster software. Usually I also perform calculations using the ASCRS online calculator. If these sets of results are inconsistent, I may even do further calculations using Orbscan K values from the central 2-mm zone.
INFORM THE PATIENT
The patient should also be informed before the excimer laser procedure as well as before cataract surgery that an excimer laser ablation decreases the accuracy of any IOL power calculation. I always perform sequential cataract surgery, starting with the nondominant eye, and usually aim for mini-monovision (eg, -0.75 D). Thus, the result will be acceptable, even with a slight over- or under-correction. I can also use the result to increase the probability of hitting emmetropia in the dominant eye.
I have not mentioned IOL power calculations for cataract patients with previous RK, as these cases do not represent a significant problem in my practice and RK (luckily) never became widespread in Norway. In the few RK cases I have had, however, I relied on the ASCRS online calculator.
Kjell U. Sandvig, MD, PhD, practices at Oslo Eye Center, Norway. Dr. Sandvig states that he is a paid lecturer for Alcon Laboratories, Inc., but has no financial interest in the products or companies mentioned. He is a member of the CRST Europe Editorial Board. Dr. Sandvig may be reached at tel: +47 22 93 12 60; fax +47 22 93 12 70; e-mail: kusandvig@gmail.com.

