
Physician burnout is a clinical syndrome characterized by emotional exhaustion and loss of enthusiasm for work, feelings of cynicism, and reduced performance. The symptoms of burnout can include feeling drained and overwhelmed; being physically exhausted; exercising poor judgment; suffering from a sense of detachment in relationships with coworkers and patients; and experiencing feelings of ineffectiveness.
The impact of burnout is extensive. Although its consequences to the physician are concerning, burnout has equally concerning effects on patients, patient safety, and quality of care. Research correlates burnout with disruptive behavior, increased medical errors, lower patient satisfaction scores, and increased malpractice risk. If unaddressed, burnout can result in dire consequences for the individual, both personally and professionally. In addition to job dissatisfaction, burnout can contribute to failed relationships, substance abuse, and worsening mental health for the physician.
Why Is Burnout on the Rise?
Practicing medicine has always been intellectually, physically, and emotionally demanding work. But, in addition to performing their clinical duties, today’s physicians are doing much more. The restructuring of health care, increased regulatory pressures, and even the introduction of technology has resulted in a tsunami of change and additional stressors.
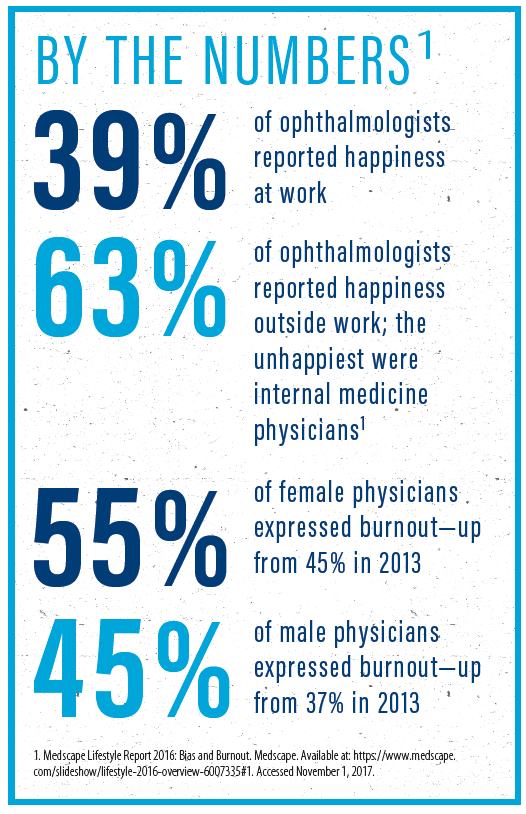
All these extra responsibilities detract from time spent with patients and threaten a healthy work-life balance. In the 2016 Medscape Physician Lifestyle report, which surveyed thousands of US physicians, respondents identified the top five causes of burnout as: (1) too many bureaucratic tasks, (2) too many hours at work, (3) insufficient income, (4) increasing computerization, and (5) the impact of the US Affordable Care Act.1
What Should Affected Doctors Do?
Those most directly responsible for health and healing tend to forego the very treatment they would recommend to any patient. Physicians must pay attention to their symptoms and do whatever it takes to restore work-life balance—including seeking professional help. Medicine’s culture of invincibility has made it difficult for physicians to attend to their basic mental health needs. The danger is, if unaddressed, there is a risk of severe depression and a host of other serious personal and professional sequelae.
Organizations concerned about physician health and well-being can adopt a proactive approach to identifying burnout among their medical staff by administering anonymous surveys and by investigating other telltale signs of struggle, including reports of behavioral changes or perhaps a decline in performance or patient satisfaction scores. Hospitals and medical groups can also promote wellness by offering education and resource information via their Physician Health and Wellbeing Committees, whose charter is to assist physicians struggling with behavioral issues, substance abuse, addiction, and mental health challenges.
A Message on Mindfulness
Meaningful connections help to decrease the key components of physician burnout.
By Jullia A. Rosdahl, MD, PhD; and Karen Kingsolver, PhD
Take a breath—not extra deep or slow, just a regular breath. Really feel the breath: Notice the air passing through your nose, how it might feel cooler going in and warmer coming out, and the movement of your belly or chest expanding against your clothes. Do not judge the way you breathe; just notice it. That is mindfulness, or a mindful breath. Mindfulness is a key intervention that has been shown to decrease physician burnout.
MINDFULNESS IN ACTION
Like mindful breathing, you can do just about anything in a more mindful way: walking, eating, sitting, listening. Mindfulness is about being present and paying attention to the present moment in a nonjudgmental way. This awareness can help you respond instead of react when difficulties arise.
Even a brief mindfulness practice, such as touching the door knob before entering the exam room and feeling the coolness or smoothness of the metal, can help you let go of your thoughts, concerns, and worries. This, in turn, can help you be more open to the patient waiting for you so that you can be more present with him or her, focus your attention, and connect. Meaningful connections with our patients, our staff, and each other help to combat and decrease the depersonalization and exhaustion that make up physician burnout.
A DEFENSE AGAINST BURNOUT
Burnout at the individual clinician level is characterized by emotional exhaustion, cynicism, and feeling ineffective. Each of those affective states has been shown to be responsive to mindfulness because mindfulness is accompanied by increased vitality and calm, a more positive outlook, and increased self-efficacy. Many of our colleagues report to us that mindfulness micro-practices (eg, feeling the hand on the door knob, noticing the breath) help them to feel more present and therefore less sluggish during their busy clinic and OR days.
SUMMARY
Practicing mindfulness gives you a chance to reconnect with yourself and with your own body; to pause the racing thoughts, the multitasking, and the intense busyness; and to remember why we became doctors in the first place and how what we do as ophthalmologists every day can have a powerful impact on our patients’ and our own lives.
Suggesting reading list:
Kabat-Zinn J. Full Catastrophe Living: Using the Wisdom of Your Body and Mind to Face Stress, Pain, and Illness. New York: Bantam Books; 2013.
Shanafelt TD, Hasan O, Dyrbye LN, et al. Changes in burnout and satisfaction with work-life balance in physicians and the general US working population between 2011 and 2016. Mayo Clinic Proc. 2015;90(12):1600-1613.
West CP, Dyrbye LN, Erwin PJ, Shanafelt TD. Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. Lancet. 2016;388(10057):2272-2281.
Ultimately, it is necessary to make workplace improvements to lighten or streamline physician workload. I recently spoke with an emergency department chief who was aware of the workplace challenges of his physician staff. In addition to caring for patients in an impacted emergency department, the physicians complained about the burdens of documenting in the electronic health record, which was adding extra hours and stress to an already-demanding shift. This chief is currently exploring the benefit of using scribes in the emergency department to free up physicians so that they can focus on their patients.
Being responsive to the sources of physician job dissatisfaction and identifying improvement opportunities is one way of advocating for physicians, preventing burnout, and ensuring that patients receive the best possible care from their providers.
1. Medscape Lifestyle Report 2016: Bias and Burnout. Medscape. Available at: https://www.medscape.com/slideshow/lifestyle-2016-overview-6007335#1. Accessed November 1, 2017.



