



There are many laser vision correction (LVC) options available today, including a variety of lenticule extraction procedures, that expand the reach of refractive correction and increase the potential for patient satisfaction after surgery. Over the past decade, lenticule extraction has established itself as a viable alternative to LASIK and PRK for corneal refractive surgery. Lenticule extraction procedures, such as SmartSight (SCHWIND eye-tech-solutions), are an established LVC technique.
During the SmartSight procedure, the SCHWIND ATOS femtosecond laser, a platform designed to enable corneal cuts for a variety of indications, is used to create a predefined lenticule in the intrastromal tissue of the cornea and make small peripheral incisions in the topmost layer of the cornea for lenticular access. The procedure spares tissue by optimizing lenticular geometry. No lenticule sidecut is performed, and the lenticule is tapered outside the optical zone using a transition zone, much like with the SCHWIND AMARIS, toward the periphery to reduce epithelial remodeling and minimize regression.
Tight nomograms are possible with ATOS, decreasing the risk for undercorrection in either sphere or cylinder. The laser boasts fast cutting times, a compact design, static cyclotorsion compensation imported from the SCHWIND SIRIUS scheimpflug system†, pupil recognition, objective treatment offset, and cyclotorsion correction during and after the docking procedure.
This article details the clinical experience from three centers that have been using the ATOS since 2020: Matrika Eye Center in Kathmandu, Nepal; Svjetlost Clinic in Zagreb, Croatia; and EyeLaser in Vienna, Austria. Our practices were among the first in the world to use the ATOS femtosecond laser for both LASIK and lenticule extraction procedures. Collectively, as of July 2022, we have created more than 1,000 flaps and more than 1,000 SmartSight lenticules.
The outcomes with this new laser are promising and, in our opinion, point to a paradigm shift in refractive correction. In our experiences, the platform is helping to build a renaissance in corneal refractive surgery. For us to be involved with a technology so early in its lifecycle has been exciting.
LOWER LASER POWER
We use similar settings. Pulse energy ranges from 80 to 90 nJ, and spot and track distances range from 4 to 5 µm and 2.5 to 3.5 µm, respectively. These settings lead to an overall treatment dose of 0.8 J/cm2 or less.
Lenticules can be created with an energy level as low as 75 nJ per pulse (with tighter spacing) or with a track distance as large as 5 µm using higher energy per pulse. Oversizing the cap so that it is approximately 0.8 mm wider than the transition zone provides ample room for surgical maneuvers. The overall cap diameter ranges from 8.0 to 8.6 mm.
ADVANTAGES
The use of lower laser power levels at higher repetition rates. This can result in a more accurate treatment and cyclotorsion control during surgery, which can improve astigmatism correction and decrease vertical coma. The ATOS also creates a refractive transition zone at the edge of the lenticule, possibly improving quality of vision. Because the lenticule has a zero-thickness edge, it is easier to extract without leaving lenticule fragments behind and requires no minimum lenticule thickness.
Docking. Docking with the ATOS is seamless. This is key: A successful dock promotes successful surgery and the best chance for excellent postoperative outcomes. The docking process with ATOS is gentle, and there is no blackout phase, promoting a better patient experience and easing patient fears.
Eye tracker–guided centration and docking. We feel the biggest advantage of the ATOS compared to competing devices is the eye tracking and cyclotorsion compensation, which makes sure you are treating on the right axis. The eye tracker provides the operator with a coaxial view through the cone of the patient interface. It includes static overlays of the target pupil position surrounded by two concentric hot zones (target hot zone of 200 μm radius; maximum permissible hot zone of 700 μm radius; Figure). Once the patient is instructed to move the operating table, the operator centers the interface on the target pupil position, which is detected by a video-based eye tracker. Suction is then applied and pupil centration is confirmed to be in the target hot zone. A maximum permissible hot zone is also shown on the display (the red circle in the Figure). If the pupil is not in either zone, docking is reattempted.
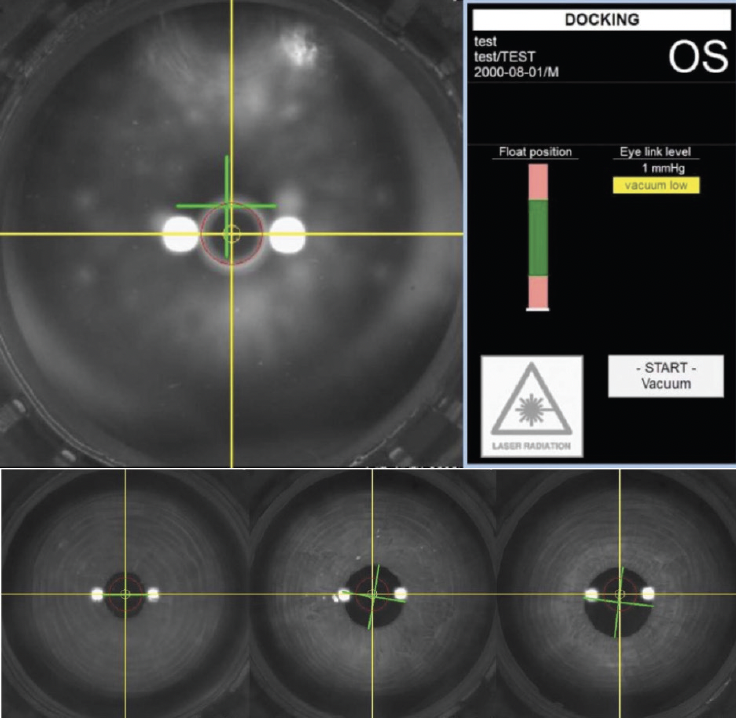
Figure. Static overlays of the target pupil position (yellow crosshairs) surrounded by two concentric hot zones (target hot zone of 200 μm radius, marked as a yellow circle; maximum permissible hot zone of 700 μm radius, marked as a red circle). The torsional deviation is displayed by the rotated green crosshairs.
The last valid laser eye-tracker video frame is used for cyclotorsion control, and the torsional misalignment from the diagnostic image is determined and accounted for by the torsional deviation display (the green crosshairs in the Figure).
Astigmatism correction. The ATOS can potentially treat higher amounts of astigmatism with better precision than other femtosecond laser platforms. The device’s built-in torsion control compensates for rotation during the docking procedure. In our experience, results with SmartSight for astigmatism correction are excellent. We have also found that refractive correction with SmartSight is comparable to LASIK with less chance for regression.
Lenticule dissection and extraction. With ATOS, the edge of the lenticule is zero-thickess. This simplifies lenticule dissection and extraction on the periphery.
OUTCOMES
ATOS performance for LASIK and SmartSight is very good. Once the right settings for the device have been found, users may slightly refine their technique, and results are very convincing.
For flap creation. None of us experienced a long learning curve for flap creation with the ATOS. In fact, it was nearly nonexistent thanks to the intuitive user interface of the device, allowing us to dock the patient interface and achieve the same efficiency in flap creation as we had after years of experience with other femtosecond laser platforms. This was true regardless of the surgeons’ level of experience. After five or six procedures, all surgeons were able to complete the flap in just a few minutes.
The day 1 postoperative results with ATOS are impressive. The flap edge is smooth, similar to the quality achieved with a microKERATOM, and there is minimal to no inflammation. This is because of the low energy dose (and total energy) being delivered to the corneal lamella. Further, ATOS allows granular customization, including spot/track distances and energy fine-tuning, so that each surgeon can determine their own settings. With ATOS, it is possible to fine-tune the energy to ensure that every flap is easy to dissect. The level of adjustment is virtually infinite.
For SmartSight. All surgeons were comfortable performing SmartSight within a few weeks of experience with the ATOS. After a few lenticules, even the less-experienced surgeons felt secure enough to perform the procedure independently. SmartSight feels easy to perform almost instantaneously due to the device’s torsion control, eye tracking, pupil recognition/centration, and positioning technologies.
It is typical for patients who undergo SmartSight to experience about 90% to 95% visual recovery on the first day postoperatively. The smoothness of the bed makes visual recovery faster than any other laser system, and the different lenticule shape and composure requires less tissue removal. This is valuable in higher prescriptions. Contrast sensitivity may fluctuate within the first month.
Results with SmartSight have changed the outlook of lenticular surgery. It is becoming a procedure we perform more often, and we believe that lenticular surgery will become the procedure of the future.
Previously with lenticular surgery procedures, it took longer for patients to recover, and they did not see 20/20 or better on postoperative day 1. The wow factor was missing, and patients’ vision was hazy and blurry immediately postoperatively. With SmartSight, however, the time commitment of surgery and the postoperative day 1 results are comparable to femtosecond LASIK. In our opinion, this is an important point for the evolution of the procedure. Patients can experience the same wow factor as after LASIK with a fast visual recovery and minimal risk of inducing or exacerbating dry eye disease. Additionally, after SmartSight, patients are not bound by any safety limitations for their daily activities.
The difference in central epithelial thickness at 12 months postoperatively from preoperative baseline has little to no correlation with the refractive power of the correction. On average, the thickness of the central epithelium increased by about 3 μm, with maximum changes of 12 μm thicker to 6 μm thinner compared to the preoperative baseline. Most of the data points suggest a minimum change in central epithelial thickness between zero and 5 μm (see Figure 2 in the next article, “Enhancements to Lenticule Extraction”).
COMPLICATIONS
In our experience, there are no known complications that are unique to ATOS. An opaque bubble layer can occur regularly, whereas black spots occur more rarely, and areas of inaccurate laser pulse placement due to eye movement are seldom.
Specifically for SmartSight, in some treatments initially the posterior plane was entered. Generally, it was detected by the surgeon and the anterior plane was subsequently entered.
CONCLUSION
One of our jobs as surgeons is to individualize treatment plans for our patients, ensuring not only the best postoperative outcomes but also meeting their needs. An adjustable laser system like the ATOS increases the range of patients we can treat, such as those with large pupils, thin corneas, and dry eyes. In our opinion, the clinical results we have achieved with the ATOS support the expanded use of the laser for LASIK flaps and SmartSight lenticule extraction.
†Manufactured by CSO SRL

