SCHWIND ATOS is a new development in femtosecond laser technology that enables the generation of LASIK flaps and lenticules for SmartSight lenticule extraction. It received the CE Mark in July 2020, early in the COVID-19 pandemic. Since then, a steadily growing number of surgeons in and beyond Europe has performed SmartSight. In all treated patients, lenticule removal was reported to be performed without relevant intraoperative complications.
SCHWIND ATOS works in the plasma-mediated ablation range, which is well below the photodisruption range and slightly above the threshold for laser-induced optical breakdown. It generates only low-density plasma and pulses in the low-energy range, providing a gentle, tissue-friendly treatment. Most procedures are performed using pulse energies between 75 and 100 nJ with spot/track spacings from 2.5 to 5 µm. ATOS does not require a minimum lenticule thickness, potentially reducing the overall thickness of the lenticules.
FEATURES AND ASSOCIATED ADVANTAGES
The basic features of the SCHWIND ATOS and their associated advantages (Table) have enabled the development of tight nomograms, no perceived undercorrections for either sphere or cylinder, and fast cutting times. The compact system includes cyclotorsion compensation imported from SCHWIND diagnostic devices (SCHWIND SIRIUS+, SCHWIND PERAMIS, and SCHWIND MS-39)†, pupil recognition software, and objective treatment offset and cyclotorsion compensation during and after the docking procedure.
Compared to other lenticule extraction laser procedures and unlike excimer laser–based ablations, there is only a slight difference in cutting times depending on the planned correction. With the SCHWIND ATOS, flaps can be cut in about 8 to 10 seconds and lenticules in about 15 to 18 seconds.
SCHWIND’s application team accompanies surgeons on their first days of treatment in the clinic to support ATOS users as best as possible. The feedback from the ever-growing SCHWIND ATOS user family is that the flap edges are very clean, but they can require attention to separate them cleanly in a single pass. Users also have commented that the stromal bed is smooth and visual acuities on day 1 produce the typical "wow" effect patients experience after LASIK. Regarding lenticule creation, users mentioned that lenticules may be unexpectedly easier to approach than flaps initially. The smoothness cannot be truly qualified in this setting because the pocket remains closed. Visual acuities on day 1 are good; on average, patients achieve 20/25 to 20/20 with a few exceptions of 20/32. Some even achieve 20/16.
On postoperative day 1, topographies look wide and clean and the planned optical zone is achieved (Figure 1). The optical zone for SmartSight lenticules can be up to 7.5 mm; overall lenticule diameters are larger due to the included transition zone. As the lenticules get thicker (eg, for higher corrections or larger optical zones), they are easier to extract, but less residual stroma is left behind. The ATOS limits the maximum lenticule thickness to between 25 and 165 µm. Further, ATOS imposes a minimum 275 µm calculated residual stromal thickness.
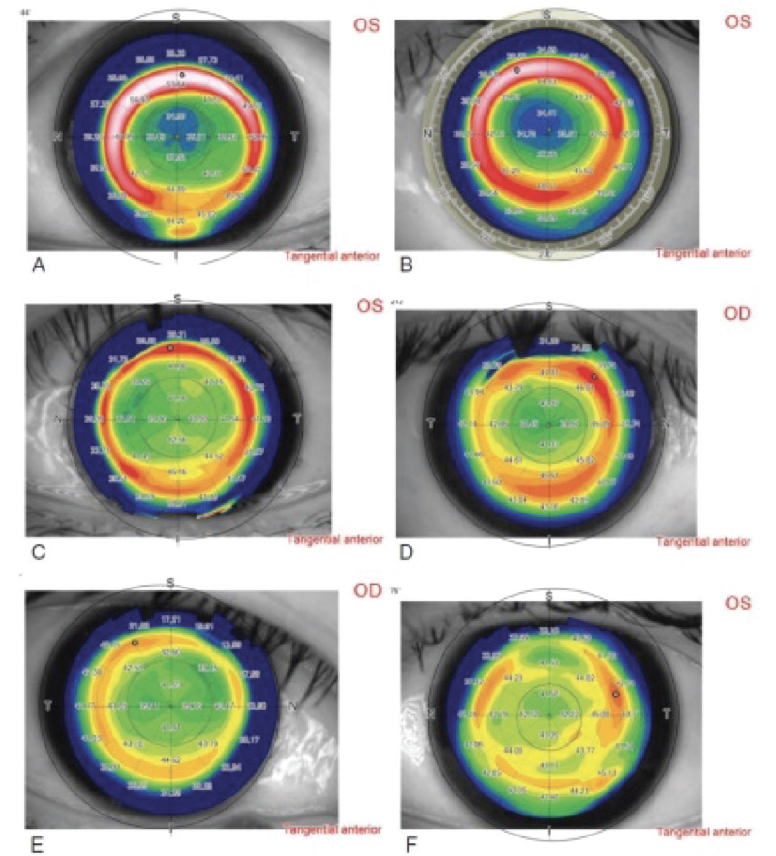
Figure 1. Postoperative day 1 topographies. In these cases, the planned optical zones were 6 mm.
Extensive hyperplasia may be one reason why some competing lenticule systems require overplanning of the nomogram. The amount of epithelial hyperplasia appears to be much less with the ATOS than with competing technologies.1 We believe that the use of a progressive refractive transition zone with the ATOS helps produce less hyperplasia, undercorrection, and regression and potentially reduces epithelial remodeling. In one study, central epithelial thickening with ATOS was only 3 ±2 µm at 12 months (Figure 2).2 Additionally, there were no reports of undercorrection for either sphere or cylinder and more than 90% of treatments were within ±0.50 D of intended correction at the same time point (Figure 3).
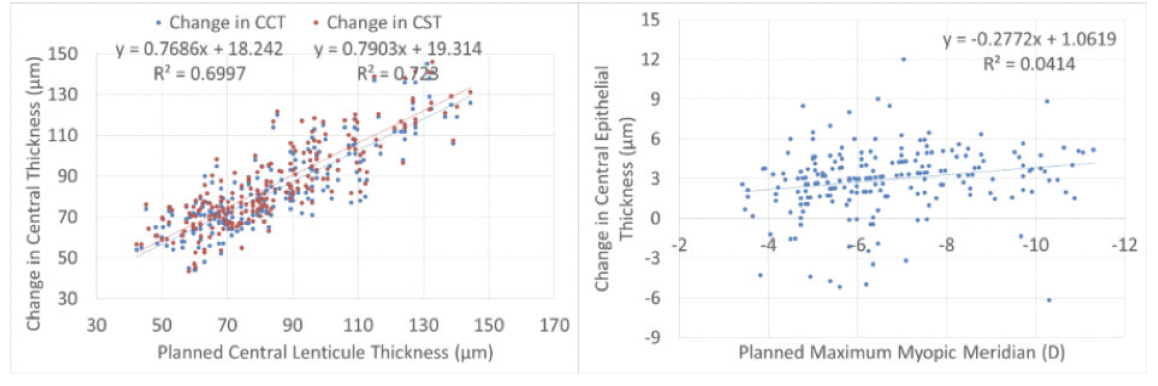
Figure 2. Change in central corneal thickness.
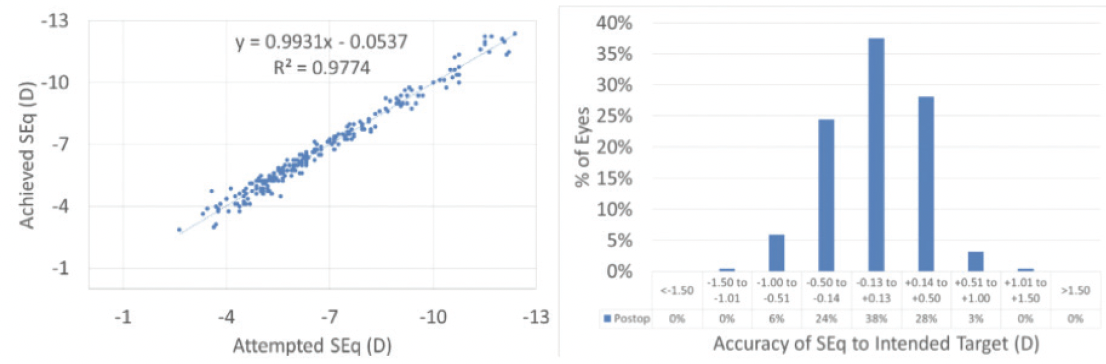
Figure 3. Accuracy of the spherical equivalent at 12 months postoperative.
The low pulse energy (sub-100 nJ) of the ATOS provides better resolution and reduces corneal reactions.3 The asymmetric spacings leads to more homogeneous cuts with less pulse energy. Additionally, a slight overbending of the cap is a protective measure against slight decentrations.
SMARTSIGHT OUTCOMES
Pradhan et al found that, at 12 months, 93% of eyes that underwent SmartSight achieved a UDVA of 20/20 or better.2 In all eyes, UDVA remained within 1 line of the preoperative distance-corrected visual acuity (CDVA), and no eyes lost more than 1 line of CDVA. Refractive correction of the spherical equivalent (SEQ) and refractive astigmatism were both excellent, with 90% and 100% of eyes, respectively, within ±0.50 D of the target. In 89% of eyes, the axis of the refractive astigmatism was within 15º from the planned treatment.
Pradhan found that, for eyes with moderate to severe astigmatism (1.00 D or greater) preoperatively, 81% had 0.50 D or less of residual astigmatism postoperatively.4 The correlation between target-induced and surgically induced astigmatism for manifest refraction was relatively good, but it was lower than for SEQ. Almost all eyes (96%) showed an angle of error between -15° and +15°.
There is a short learning curve with SmartSight lenticule extraction.5 In one study, the first 16 treatments were performed without astigmatism correction, followed by 52 treatments to optimize the laser’s settings and refine the technique. Thereafter, the treatments (>100) have been performed with the optimized settings and technique. The UDVA outcomes are shown in Figure 4.
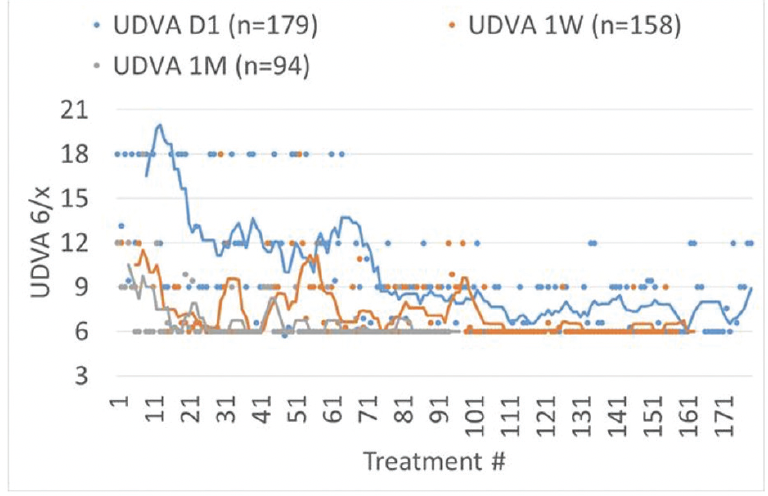
Figure 4. UDVA outcomes after SmartSight.
SmartSight does not yet have customized treatments. Data show that, above -5.00 D, 93% to 96% of eyes achieved a UDVA of 20/20 or at least equal to the preoperative CDVA.2
At ESCRS 2021, Maja Bohac, MD, PhD, reported that higher-order aberrations (HOAs) after SmartSight, especially spherical aberration and coma, remained essentially unchanged (Figure 5).6 Whole-eye ocular wavefront (OW) scans did not show changes from preoperative to 3 months postoperative for coma or spherical aberration, whereas HOA root mean square (RMS) increased by 0.14 ±0.15 μm. Corneal wavefront (CW) measurements increased from preoperative to 3 months postoperative for coma (0.22 ±0.21 μm), spherical aberration (0.17 ±0.19 μm), and HOA RMS (0.32 ±0.26 μm). From preoperative to 3 months postoperative, HOAs changed for OW (0.1 ±0.1 μm), coma (0.2 ±0.2 μm), and spherical aberrations (0.2 ±0.2 μm) and HOA-RMS changed for CW (0.3 ±0.3 μm).
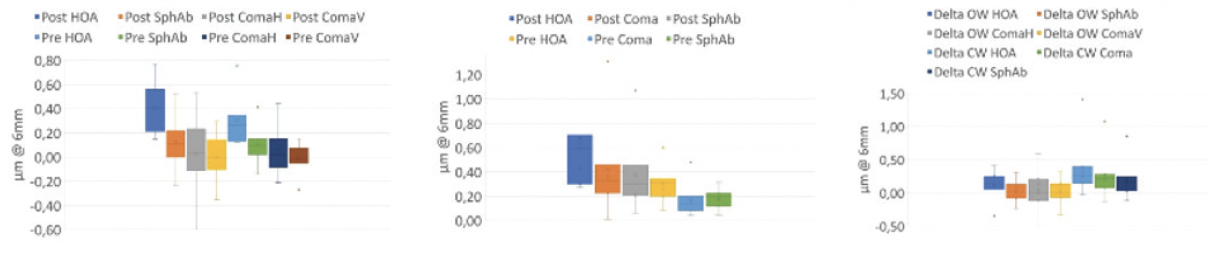
Figure 5. HOAs after SmartSight as measured by OW and CW.
FUTURE OUTLOOK
In the future, the following advancements and features will be released for the SCHWIND ATOS:
- Easier flap transition;
- Conversion of a cap (lenticule) to a LASIK flap;
- Inclusion of intrastromal corneal ring segment function;
- Inclusion of a keratoplasty function; and
- Optimized centration with an asymmetric transition zone concept.
Furthermore, treatment options such as custom lenticules for myopia, hyperopic lenticules, and presbyopia-correcting lenticules are being considered to broaden the ATOS application range in the future.
CONCLUSION
The SmartSight lenticule extraction procedure will continue to undergo enhancements with the SCHWIND ATOS. The innovative laser system incorporates properties of the successful and proven SCHWIND AMARIS technology.
The ATOS works in an optimized but minimum pulse energy range and spaces the laser pulses asymmetrically. Of the many advantages, the eye tracking–guided centration and static cyclotorsion control seem to be relevant for the clinical success of the lenticule extraction procedure (ie, SmartSight in the SCHWIND nomenclature), paving the way for future customizations in lenticule profiles.
The concept for the SmartSight lenticule profiles were derived from the vast experience with the SCHWIND AMARIS and do not require any minimum thickness levels. The profiles incorporate a progressive refractive transition zone, possibly reducing the overall thickness of the lenticules and providing a true transition zone that causes less remodeling of the epithelium and less regression.
Both the current ATOS laser system and future developments can help surgeons stay on the cutting edge of laser vision correction.
1. Reinstein DZ, Archer TJ, Gobbe M. Lenticule thickness readout for small incision lenticule extraction compared to artemis three-dimensional very high-frequency digital ultrasound stromal measurements. J Refract Surg. 2014;30(5):304-309.
2. Pradhan KR, Arba Mosquera S. Twelve-month outcomes of a new refractive lenticular extraction procedure. J Optom. 2021;S1888-4296(21)00085-6.
3. Arba-Mosquera S, Naubereit P, Sobutas S, Verma S. Analytical optimization of the cutting efficiency for generic cavitation bubbles. Biomed Opt Express. 2021;12:3819-3835.
4. Pradhan KR, Arba Mosquera S. Three-month outcomes of myopic astigmatism correction with small incision guided human-cornea treatment. J Refract Surg. 2021;37(5):304-311.
5. Pradhan KR, Arba Mosquera S. Initial experience with the SCHWIND ATOS and SmartSight Lenticule Extraction. J Clin Res Med. 2020;3(4):1-5.
6. Bohac M. First European results of a new refractive lenticular extraction procedure – SmartSight by Schwind Eye Tech Solutions. Paper presented at the: ESCRS Annual Meeting; 2021.
†Manufactured by CSO SRL

