When faced with a patient who has insufficient pupil dilation and is scheduled for cataract surgery, there are two major points to keep in mind: (1) pupil size and (2) rigidity, or biomechanical properties, of the iris tissue. What size pupil is considered small is controversial, as pupil size is relative and the definition of small small is greatly influenced by the experience of the surgeon, ocular comorbidities, and the intraoperative situation. Most welltrained surgeons would probably agree on using pupilexpansion devices—either iris hooks or pupil-expansion rings—in an eye with a rigid pupil smaller than 3.5 mm with a soft nucleus or smaller than 4.0 mm with a hard nucleus. Pupil size will have to be increased up to 4.5 to 5.5 mm for an inexperienced surgeon. Some surgical techniques of nucleus fragmentation, such as divide and conquer, require bigger pupils than others, such as phaco chop, for safe nucleus removal.
The pupil often dilates poorly in eyes with atrophic irises, and the significantly diminished iris tone in these eyes is unable to withstand the fluidic currents in the anterior chamber and maintain the correct position of the iris. In cases of intraoperative floppy iris syndrome (IFIS), loss of iris tissue rigidity, even in the presence of a moderately dilated pupil, will complicate the surgical procedure by increasing the risk for the iris to be aspirated and damaged by the ultrasound needle. 1 In these patients, in which the pupil tends to be large enough initially but then experiences progressive miosis during surgery, a mechanical pupil-enlargement strategy can be utilized during the earlier steps of the surgical procedure.
In many cases of IFIS, intracameral injection of epinephrine or phenylephrine can simplify preoperative patient preparation and enlarge and stabilize the iris tissue, reducing the risk of complications. 2,3A commonly used concentration of epinephrine is 1:1,000 mixed 1:3 with balanced saline solution.
In small pupils, iris tissue is located closer to the zone of high fluidic currents, which is why it is more likely to be aspirated into the ultrasound or I/A handpiece. Reducing flow parameters is an important factor in preventing iris damage during phacoemulsification. Maintaining a central position and employing minimal movements of the surgical handpiece are also important to prevent iris damage. Endocapsular nucleus fragmentation is much safer in these eyes because this locates the areas of the highest fluidics currents inside the capsular bag, away from the corneal endothelium and iris.
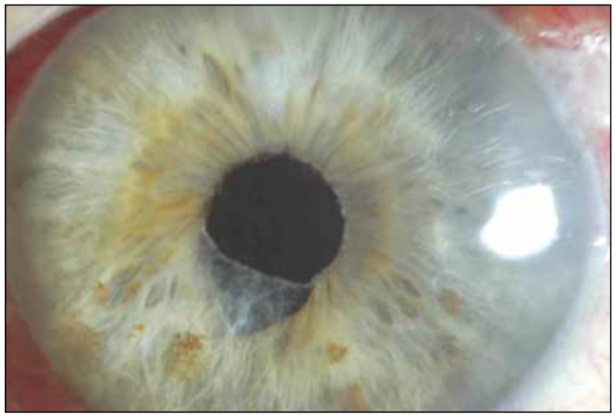
Figure 1. A relatively small pupil defect caused by iris aspiration.
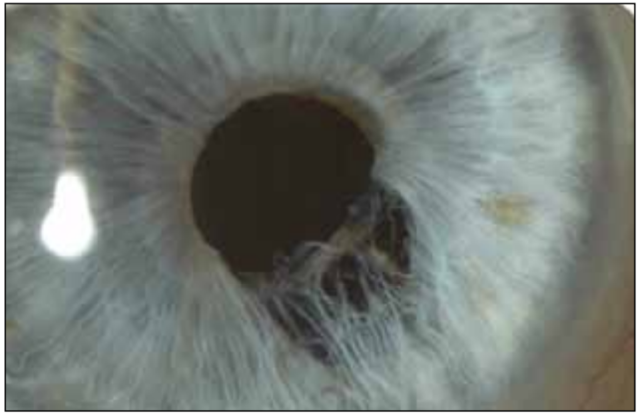
Figure 2. A significant pupil defect caused by a vibrating ultrasound needle, leading to formation of stromal fibrils.
Iris damage during surgery can range from a relatively small iris defect, as the result of iris aspiration without ultrasound activation (Figure 1), to more extensive iris tissue damage with ultrasound engaged. Contact with the activated ultrasound probe can lead to stromal chafing and the formation of tissue fibrils (Figure 2). Once created, these fibrils have a tendency to be repeatedly aspirated into the ultrasound needle or I/A handpiece, aggravating the condition.
My personal strategy in the presence of mild iris defects is to use a second instrument to retract the iris margin away from the orifice of the aspiration needle. If they have not already been deployed, use of iris hooks or pupilexpansion rings can be considered at this point to prevent further iris damage. In cases of severe damage, I prefer to use radiofrequency endodiathermy (Oertli Instrumente AG) to coagulate the fibrils and strengthen the rigidity of the iris tissue.
TECHNIQUES FOR PUPIL ENLARGEMENT
A number of techniques can be used to mechanically enlarge the pupil during cataract surgery. Most surgical maneuvers for pupil expansion and prevention of intraoperative constriction are less than ideally safe. They can lead to increased risks of iris sphincter tears, bleeding, iris damage, posterior capsular tears, and vitreous loss.
Mechanical stretching with two instruments such as microhooks and microforks or a special iris dilator such as the Beehler Pupil Dilator (Moria Surgical) is a relatively simple and effective maneuver. It is extremely helpful in managing surgery in small pupils associated with increased rigidity of the iris sphincter. This maneuver creates microtears in the iris to enlarge the pupillary aperture. The drawback of iris stretching is that it permanently damages the iris sphincter. Microscopic tears of the sphincter muscle are usually clinically asymptomatic but sometimes result in bleeding and pigment dispersion postoperatively.
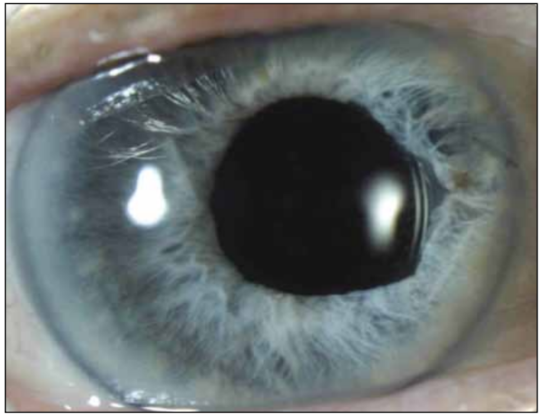
Figure 3. A fixed dilated pupil due to subincisional iridocapsular adhesions in the temporal quadrant following excessive intraoperative tissue trauma.
Small degrees of pupil dysfunction are not uncommon after cataract surgery with and without iris manipulation, usually causing no subjective symptoms (Figure 3). Halpern and coauthors4 found an incidence of postoperative atonic pupil of 1.1% after phacoemulsification, with pupil diameters ranging from 6.0 to 8.0 mm. In a study of stretch pupilloplasty in small pupil cases by Dinsmore,5 10% of 50 patients developed an enlarged atonic pupil postoperatively. All patients had a history of injury or inflammatory disease.
The use of iris hooks may also damage the pupillary margin intraoperatively, producing a semimydriatic nonreactive pupil postoperatively. Birhall 6 assessed the effect of various flexible iris hook positions on pupil shape and circumference. He confirmed that malpositioned iris hooks increase pupil stretching, with possible deleterious effects on postoperative pupil function. Masket 7 and Yuguchi 8 recommended that the pupil not be stretched by hooks to an area larger than 5.0 mm2because postoperative irregular atonic pupils can result from overstretching.
Additionally, during engagement of the pupillary edge, iris hooks may catch the capsulorrhexis and damage the capsule, leading to an anterior capsular tear that may extend to the periphery. To avoid this problem, a drop of OVD should be injected between the iris and the capsule before the hook is inserted. Another useful technique is to keep the hook parallel with the iris plane during insertion and to tilt it slightly posterior, right near the pupillary edge, to engage only the iris. Iris hooks may become loose during surgery, and their tips may become dislocated, no longer holding the pupillary edge. This can cause problems such as iris aspiration.
One of the most attractive benefits of mechanical pupil expanders and pupil-expansion rings is the ability to avoid the multiple additional incisions of the eye that are required for iris hook implantation. Pupil-expansion rings are introduced and removed through the main phaco incision. Most of them have grooves on the outer surface for iris capture. Several pupil-expansion rings are currently available, including the Perfect Pupil (Milvella), Morcher Pupil Dilator (Morcher GmbH), Siepser Iris Protector (EagleVision), and Graether Pupil Expander (EagleVision).
The use of pupil-expansion rings can avoid or reduce complications in comparison with surgical enlargement. Most create round, expanded pupils, as opposed to the square pupils produced by the placement of four iris hooks. Given the geometric fact that the perimeter of the circle is smaller than the perimeter of the square, placement of a pupilexpansion ring is more tissue-friendly than use of hooks.
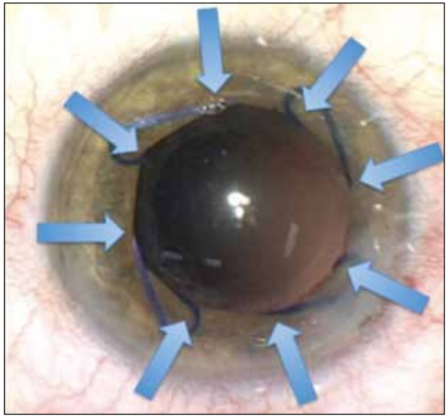
Figure 4. Eight retraction points of the pupillary margin (blue arrows) with the Malyugin Ring create a round, enlarged pupil.
Specific devices that help to mechanically dilate the pupil vary in design and handling. My preference in most cases is for the Malyugin Ring (MicroSurgical Technology), which helps effectively enlarge the pupil and protect the iris from damage. 9,10 The main advantage of this device is that it does not create a square pupil, as one may assume given its rectangular shape, but rather a round one (Figure 4). My technique for Malygun Ring implantation and removal is described in Useful Tips for the Mayugin Ring.
Patients with poorly dilated pupils are prone to more intense postoperative inflammatory response due to ocular comorbidity and extra manipulations of the iris tissue. For that reason, one should consider closer followup and intensive and prolonged postoperative pharmacotherapy combining steroids and NSAIDs.11
CONCLUSION
Most surgical maneuvers for enlarging the pupil and preventing its intraoperative constriction are not absolutely safe. They can lead to increased risks of iris sphincter tear, bleeding, iris damage, and severe postoperative fibrinoid reaction, especially in patients with pseudoexfoliation syndrome, chronic uveitis, glaucoma, or diabetes.
Consequently, cataract surgery in the presence of a small pupil remains one of the most difficult and challenging procedures. Use of minimally invasive approaches to reduce surgical trauma allows the surgeon to effectively minimize the risk of complications and provide patients with the best possible visual and anatomic outcomes.
Useful Tips for the Malyugin Ring
From time to time, I am asked about my approach to using the Malyugin Ring (MicroSurgical Technology) in smallpupil
cataract surgery. Below are some useful tips and tricks born from my clinical experience.
Implantation of the Malyugin Ring:
- Operating under topical anesthesia, inject lidocaine intracamerally, to prevent patient sensations during iris tissue
manipulations, followed by phenylephrine 1.5%, to enhance pupil dilation and strengthen the rigidity of the iris tissue
by contracting the dilator muscle. - Do not overfill the anterior chamber with ophthalmic viscosurgical device, as this will cause closer apposition of the
iris to the lens capsule and make engagement of the pupil edge more difficult. - Insert the injector and position its tip close to the iris margin.
- Push on the thumb button and engage the pupil edge with the distal scroll.
- Continuing to push on the thumb button, slowly withdraw the inserter while expelling the ring.
- Usually two side scrolls are engaged with the pupil margin automatically. In rare cases in which the pupil is too small or
the anterior lens surface is excessively prolate, it can be hard to engage both lateral scrolls while injecting the ring. This
step can be facilitated with a sideport instrument (Osher/Malyugin Ring Manipulator [MicroSurgical Technology], Lester
[Katena Products, Inc.] or Kuglen hooks). Avoid using a Sinskey hook because there is an increased risk of puncturing the
anterior capsule with its tip. - To disengage the proximal scroll from the injector hook, use the sideport instrument and displace the ring away from the
incision or to the side (counterclockwise). - Retract the injector hook by pushing backward on the thumb button, being careful not to catch the proximal scroll again.
Removal of the Malyugin Ring:
- With the sideport instrument, disengage the distal scroll from the iris first and displace the whole ring slightly away
from the main incision, then disengage the contralateral (proximal) scroll. - Insert the injector into the anterior chamber and push the thumb button all the way forward.
- Position the injector tip footplate under the proximal scroll and engage it with the injector hook by pressing
backward on the thumb button. - Start retracting the ring. When both lateral scrolls join together, press on the upper one from above with the sideport
instrument to help them both enter the injector tube. - Retract the injector from the eye.
Boris Malyugin, MD, PhD, is a Professor of Ophthalmology and Chief of the Department of Cataract and Implant Surgery at S. Fyodorov Eye Microsurgery Complex, Moscow, Russia. Professor Malyugin is a member of the CRST Europe Editorial Board. He states that he is a consultant to Bausch + Lomb, MicroSurgical Technology, and Morcher GmbH. He may be reached at e-mail: boris.malyugin@gmail.com.
Chang DF, Campbell JR. Intraoperative floppy iris syndrome associated with tamsulosin. J Cataract Refract Surg. 2005;31:664-673.
Lundberg B, Behndig A. Intracameral mydriatics in phacoemulsification cataract surgery. J Cataract Refract Surg. 2003;29:2366-2371.
Lorente R, de Rojas V, Vázquez de Parga P, et al. Intracameral phenylephrine 1.5% for prophylaxis against intraoperative floppy iris syndrome: prospective, randomized fellow eye study. Ophthalmology. 2012;119:2053-2058.
Halpern BL, Pavilack MA, Gallagher SP. The incidence of atonic pupil following cataract surgery. Arch Ophthalmol. 1995;113:448-450.
Dinsmore SC. Modified stretch technique for small pupil phacoemulsification with topical anesthesia. J Cataract Refract Surg. 1996;22:27-30.
Birchall W, Spencer AF. Misalignment of flexible iris hook retractors for small pupil cataract surgery: effects on pupil circumference. J Cataract Refract Surg. 2001;27:20-24.
Masket S. Avoiding complications associated with iris retractor use in small pupil cataract extraction. J Cataract Refract Surg. 1996;22:168-171.
Yuguchi T, Oshika T, Sawaguchi S, Kaiya T. Pupillary functions after cataract surgery using flexible iris retractor in patients with small pupil. Jpn J Ophthalmol. 1999;43:20-24.
Malyugin B. Small pupil phaco surgery: a new technique. Ann Ophthalmol. 2007;39:185-193.
Chang D. Use of Malyugin pupil expansion device for intraoperative floppy-iris syndrome: Results in 30 consecutive cases. J Cataract Refract Surg. 2008;34(5):835-841.
Chang DF. Phaco strategies for complicated cataracts. In: Chang DF, ed. Phaco Chop; Mastering Techniques, Optimizing Technology, and Avoiding Complications. Thorofare, NJ: Slack; 2004: 173-198.

