What would you say was your most memorable case in 2020?

Por Yong Ming, FRCS(Ed), FRCS(Glasg), MMed(S’pore), MRCOphth
Consultant eye surgeon, Eye Surgeons @ Novena, Mount Elizabeth Novena Medical Centre, Singapore
"In late July, a gentleman in his 50s was referred for management of nonresolving, atypical keratitis that had been treated for 2 months as a possible herpetic/immune stromal keratitis with antivirals and topical steroids. The patient had initially presented with epithelial keratitis but was developing a white anterior stromal infiltrate (Figure 1A). He was treated with natamycin for early fungal keratitis. At 3 weeks, after an initial improvement in the keratitis, the frequency with which natamycin was dosed was reduced, after which the lesion appeared to progress and developed several adjacent satellite lesions (Figure 1B). Cultures were negative, but the clinical picture remained strongly suggestive of fungal keratitis. Oral voriconazole was prescribed but was subsequently changed to posaconazole due to disease progression.
A biopsy was taken from an inferior satellite lesion. All cultures and the histopathology of the biopsy were negative for microorganisms. The patient subsequently developed a hypersensitivity reaction to the natamycin, at which point compounded amphotericin B eye drops were substituted. A gradual improvement in the keratitis was observed over the course of 2 months. At the patient’s last visit, inactive scars were evident, and UCVA was 20/25 (Figure 1C).
When cultures and biopsies are negative, infectious keratitis—especially atypical keratitis—is challenging to diagnose. When a patient does not respond to empirical therapy, should the treating doctor persist with the working diagnosis or change the therapeutic approach? Whatever the outcome, this case and others similar to it remain etched in my mind. (Editor's note: For more on infectious keratitis, click here.)
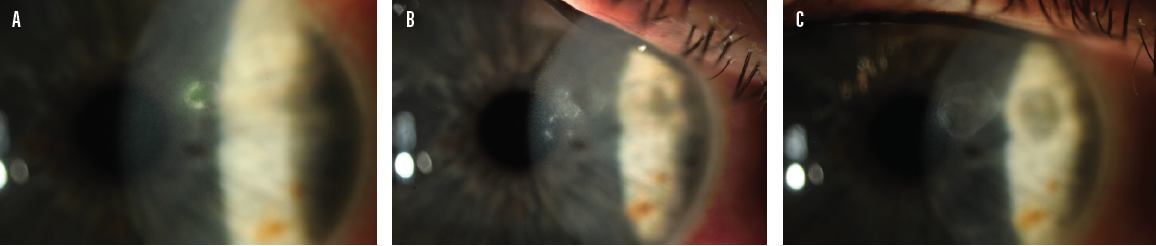
Figure 1. Presence of a curved anterior stromal infiltrate (A). Enlargement of the main infiltrate with satellites despite monotherapy with natamycin (B). Resolution of the keratitis with an inactive scar (C).

Brandon Ayres, MD
Surgeon on the Cornea Service, Wills Eye Hospital, Philadelphia
"As a tertiary referral surgeon for cornea and anterior segment surgery, I have the privilege of tackling complex cases daily. Many of these challenging cases are memorable, but my most memorable case of 2020 had nothing to do with subluxated lenses or capsular support systems. My most memorable case was a perforated corneal ulcer that had to be treated 1 week after the COVID-19 quarantine was put in place. I remember the quietness of the roads driving into the hospital. Once at the hospital, masks were on, temperatures checked, and hand sanitizer was everywhere. Although protocols were in place, nobody was quite sure if it was safe to borrow a pen to sign a consent form or if general anesthesia was safe. Surgeons were wearing multiple masks, goggles, face shields, and gloves. Nobody was quite sure if it was safe even to talk in the OR around the microscope. The OR was never so quiet.
The surgical case itself was pretty straightforward. A perforated corneal ulcer was removed, and a new cornea sutured in place, a relatively forgettable case done during an unforgettable time. As we left the OR, I recall saying goodbye to my friends and colleagues, whom I usually see on a daily basis, not knowing when I would see them in person again. Luckily, my patient has done well after surgery, and the OR is trending back toward normal. To date, this has been my most memorable case of 2020 and the most memorable case of my career.”

Thomas A. Oetting, MD
Rudy and Margaret Perez Professor of Ophthalmology and Director of the Ophthalmology Residency Program, University of Iowa, Iowa City
"My most memorable cases are not even my cases and not even real.
We were all closed down for COVID-19. We were doing no elective cases, and the ORs were empty. Our residents were losing precious time to learn the skills they needed to care for future patients. Fortunately, at the University of Iowa, we have a clever and persistent leader of surgical simulation—Jaclyn Haugsdal, MD. She worked with simulated eye companies like Phillips Studio Eye and our administration to keep a supply of artificial eyes. Dr. Haugsdal also coached our faculty on the use of simulation.
Now we get to the unreal cases. A. Tim Johnson, MD, chief of cataract surgery at the university, held numerous sessions using simulated eyes to continue his resident phaco training (Figure). This simulation, which took place in the empty COVID ORs, was very high-fidelity using a real OR microscope, a real OR phaco machine, and real OR instruments. This experience changed our perspective on simulation and took great advantage of our empty COVID ORs. Simulation in our ORs using artificial eyes opened our real eyes to the power of high-fidelity simulation without the need for a special simulation facility.
In June, our graduating residents Austin Fox, MD; Matthew Benage, MD; Heather Stiff, MD; Ben Janson, MD; and Tony Chung, MD, presented Dr. Johnson with the very real Resident Teaching award: Making the Most of a Bad COVID Situation—I am proud of Dr. Haugsdal, Dr. Johnson, and the Iowa simulation team.”
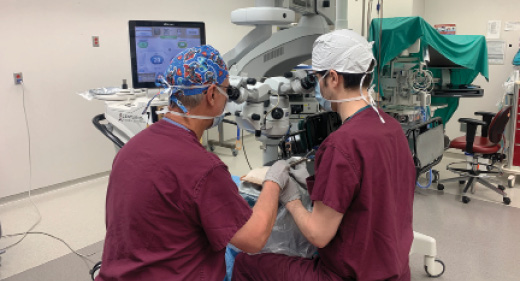
Figure 2. Dr. Johnson teaching Chris Fortenbach, MD, using simulated eyes (Kitaro) in the surgery center at University of Iowa.

Richard Mackool Sr, MD
Director, Mackool Eye Institute and Laser Center, Astoria, New York
"A 65-year-old woman presented in November 2018 with complaints of declining vision in both eyes for several years. Pertinent history included autoimmune disease with severe anxiety disorder and multiple phobias. BCVA was light perception in the right eye and 20/50 OS, with a hypermature white cataract in the right eye and moderate nuclear and posterior subcapsular cataracts in the left eye. The patient was scheduled for cataract surgery on the right eye but canceled the procedure 2 days before the date of surgery. She rescheduled and again canceled. This was followed by repeated weekly scheduling and canceling; at times, she would cancel from her car while on the way to the surgery center, and on a few occasions, she made it as far as our front door before fleeing. Psychiatric treatment and antianxiety medications were instituted, and these got her as far as walking into the OR on two occasions, looking around, and then immediately leaving the facility. Her name appeared on my surgery schedule every week, and every week it was canceled. In fact, she rescheduled and canceled more than 60 times over the next 16 months! During this time, gradually declining vision in her left eye made her nearly legally blind and totally dependent on her husband for her care.
In February, 16 months after her initial examination, she came to the surgery center where she was now, of course, on a first-name basis with every one of our employees and physicians. Several of them sat with her, encouraged her as they had been doing for more than a year, then walked her into the OR. With her husband by her side and holding her hand, I began the procedure. However, episodes of tearful and emotional outbursts required me to intermittently suspend the procedure (she refused sedation or any other medication but was given intravenous midazolam [Versed, Roche] after her health care proxy gave permission in advance for us to do whatever was needed for us to perform the surgery as safely as possible). The actual operating time was less than 10 minutes, but another 20 minutes were occupied by the delays necessary for her to become cooperative. I was able to perform the procedure uneventfully, and she immediately regained 20/20 vision in that eye. Within 1 month, the left eye progressed to a mature white cataract just before the COVID pandemic struck.
To be continued. Estimated time to surgery on the left eye, anyone?"



