
Many patients with dry eye disease (DED) are searching for effective care. At Bowden Eye & Associates, nearly 80% of patients who enter our practice have at least one DED symptom, or they have metrics that demonstrate an early imbalance of the tear film. One way to strengthen the patient experience within your practice is therefore to consider adding DED services or enhancing the ones you currently offer. Patients with DED are extremely loyal to someone who listens to their concerns and addresses their needs. When cared for effectively, they become your patients for life. This article examines the lifecycle of a typical patient with DED and describes the care continuum (Figures 1 and 2).
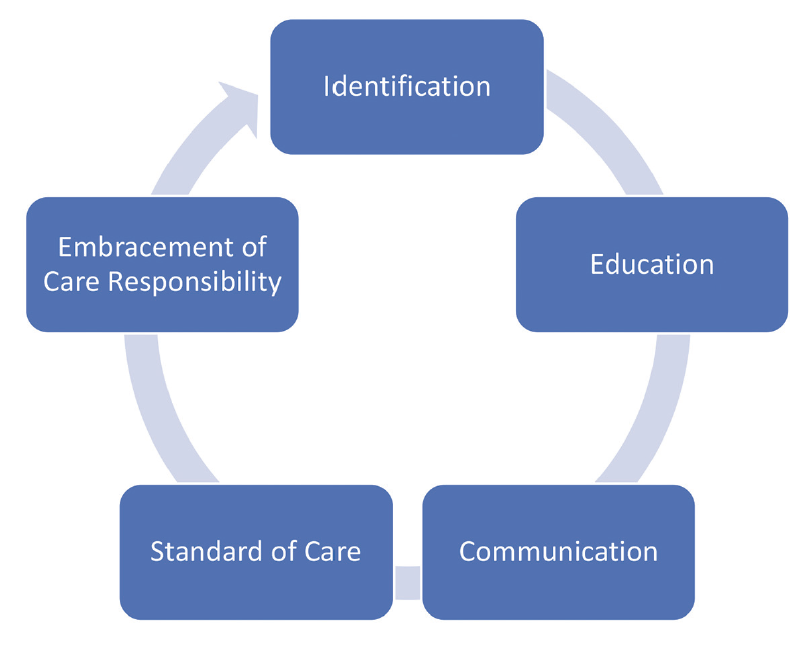
Figure 1. The lifecycle of a patient with DED.
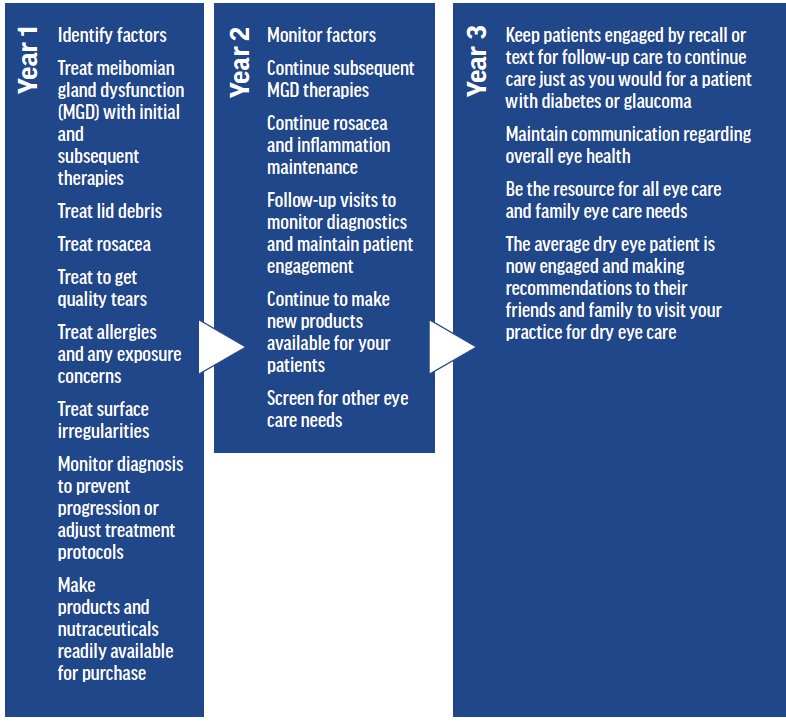
Figure 2. The care continuum for patients with DED.
DED is a chronic disease. Patients who experience DED require education to understand the chronic nature of their disease and their need for care to avoid progression. Patients therefore are essentially annuities for your practice. If engaged regularly, these patients appreciate your efforts and follow their treatment plans.
IDENTIFYING PATIENTS
There are several proven methods for identifying patients in your practice who have DED that don’t require advertising or expensive marketing dollars.
No. 1: Self identification. Patients call for an appointment to have a DED evaluation. These patients are symptomatic. Either they have researched new technologies and pharmacologic treatments for DED or they have a friend who has undergone treatment.
No. 2: Screening. We use the Standard Patient Evaluation of Eye Dryness questionnaire created by Donald Korb, OD, and at least one dry eye diagnostic tool (for a nonexhaustive listing of options, see DED Screening Devices). Patients who have a Standard Patient Evaluation of Eye Dryness score that is greater than 1 are automatically seen by the dry eye counselor before the physician encounter. This can also be done virtually.
Some DED Screening Devices
- TearScience LipiView Ocular Surface Interferometer (Johnson & Johnson Vision)
- Oculus Keratograph (Oculus Optikgeräte)
- Tearcheck (ESW Vision)
- Phoenix Meibography Workstation
(Marco Ophthalmic) - Visionix VX120 (Luneau)
- InflammaDry (Quidel)
- TearLab Osmolarity System (TearLab)
No. 3: Slit-lamp evaluation. Adding a meibomian gland evaluation, tear film breakup time, and a lid and lash examination to the slit-lamp evaluation is important. The Korb Meibomian Gland Evaluator (Tear Science) or quick expression with a cotton swab to assess the quality of the meibum can aid identification of DED.
EDUCATION
Before you can educate patients effectively, you must define your standard of care and share it with everyone on your staff. Consistency in the application of care helps with meeting patient expectations. It also helps your staff to be proactive with education, instructions, and the application of diagnostics. Your standard of care should include how and when each treatment, pharmaceutical, therapy, and product are used.
Consistency is key. Without it, patients may receive different recommendations from various providers, which can erode their trust in the treatment plan as well as in your practice. Consistent advice encourages compliance.
A clearly defined standard of care helps to create a framework for informing patients of their treatment options so that they can make educated choices. A wealth of DED education is available for your team and patients (see Educational Resources). Some patients come in for their appointments having researched their condition and treatment options. These patients will be sadly disappointed if you have nothing to offer. Other patients know nothing about their condition because no provider has taken the time to address their symptoms.
Educational Resources
- Dry Eye University
www.dryeyeuniversity.com - Dry Eye Access
www.dryeyeaccess.com - Dry Eye Coach
www.dryeyecoach.com
Whether they are educated on DED or not, patients are typically aware of the nature of their symptoms, and they want to have a higher-level conversation with you and the members of your practice about these symptoms. This is especially true of patients who have been to other providers before without experiencing relief.
COMMUNICATION
Patients with DED require an extra layer of communication because the disease state is often new to them. Developing scripts for your staff and providers facilitates patient engagement. Additionally, DED counselors can help educate patients about treatment options, medications, products, and even diagnostic tools.
Patients should be screened to identify signs of DED and provided with education before their examination to manage their time in the office effectively. In return, their visit will be significantly more productive.
If yours is a practice with multiple specialties and providers, it is important that every provider embrace the role of DED care by enforcing your treatment plans.
MOTIVATE PATIENTS
DED treatment requires patients to take responsibility for their care at home. This can include consistent application of drops and masks, continued use of nutraceuticals, and routine lid hygiene. Patients’ efforts affect their level of satisfaction with your care.
I recommend developing handouts and individualized plans for patients that include the dry eye products and medications they are prescribed. These should be discussed with patients at each visit. Patients should also be reminded about the effects of poor compliance. When they know that you are following up on their specific care, they tend to be more invested in their part of the journey.
CONCLUSION
Individuals with DED can become patients for life when they are cared for to their satisfaction. Meeting their needs requires understanding and addressing the chronic nature of DED.



