
Vitreoretinal surgery requires delicately balancing the light source, providing enough illumination to aid visualization without inducing phototoxic exposure. On the one hand, full illumination with the complete light spectrum provides the best opportunity for the surgeon to see what he or she is doing. Yet, too much light may cause damage to the retina, especially with regard to certain light spectrums.
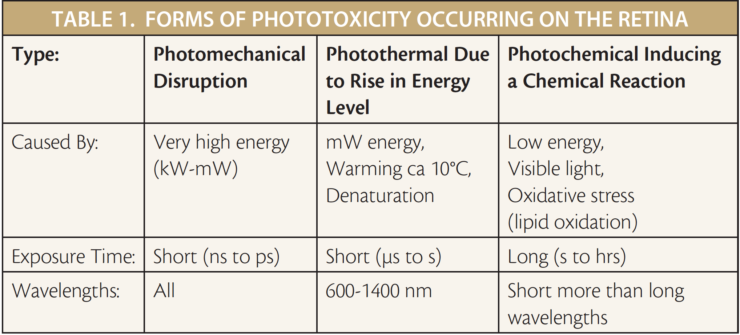
There are different forms of phototoxicity that can occur on the retina (Table 1 ). In vitreoretinal surgery, we are most concerned about phototoxicity due to nonionizing radiation to the retina, which depends on a number of factors, the most important of which are the wavelength of light used, exposure time, and the distance from the retina. Other factors, including the flux density of radiation, the character of the beam (i.e.: focused vs nonfocused), and radiance, also play a role.
The science of inducing damage to the retina is actually quite sophisticated and well characterized. What is less clear is how humans perceive light and why two different surgeons may see the same image differently.
Principles of Phototoxic Exposure
Phototoxicity is most associated with long exposure to blue light due to a photochemical process referred to as photoreversal bleaching. At a very fundamental level, the higher the energy used for illumination, the higher the energy of the photon beam, resulting in increased damage to the retina. Blue light causes chemical regeneration of rhodopsin; there are increased levels of rhodopsin following extended blue light exposure. Yet, as rhodopsin accumulates, it causes oxidative stress. Additionally, blue light inhibits the activity of essential chromophores, such as cytochromoxidase A2E, that play a central role in the visual cycle.
The human eye has developed several mechanisms to prevent or mitigate damage due to light exposure. Almost 90% of exposure is reduced by simple eye movements. In addition, the cornea, lens, and pupil function as filters to reduce the amount of blue light reaching the retina. However, during vitrectomy, the light source bypasses these natural defense mechanisms, leading to increased risk due to the surgery.
Long exposure to blue light, principally in the 400 to 550 nm range, can induce the photochemical injury described previously. However, in an aphakic eye, the relevant range for the blue light hazard widens to include wavelengths as short as 310 nm and all the way up to 550 nm. This becomes especially relevant for retinal surgery, because, as noted, we are bypassing the natural light filters of the eye—and so, whether or not the patient has a crystalline lens, the eye is essentially aphakic for purposes of the light source. The associations of potential aphakic hazard with toxicity in vitreoretinal surgery have been described in the literature as early as 1978.1
Several solutions have been proposed to counteract this phenomenon. According to the American National Standards Institute, photoexposure should not exceed 10 joules/cm2 with a maximum illumination time of 30 minutes.2 Many retinal surgeries might exceed that time frame, and it appears that the light emitting from most endoilluminators far exceeds these guidelines. According to the conclusion of one study looking at the absolute power and spectral distribution from various light sources and filter combinations, “Commercially available light sources for endoillumination during vitrectomy are not safe with respect to photochemical retinal damage. Even with maximal precautions macular phototoxic damage remains a factual danger during vitrectomy.”3
Avoiding Phototoxicity
While there is very real risk of inducing phototoxicity in retinal surgery, it is not an inevitability if certain precautions are taken. For example, shorter surgery and maintaining distance from the retina with the light source lower the potential exposure. I am currently involved in research to see if a chemical supplement can be introduced to prevent phototoxic effects in the retina. Another option would be to use different wavelengths of light, either for the whole procedure, or for certain functions, where in either case doing so reduces the exposure to blue light wavelengths.
Several different kinds of light sources are available for vitreoretinal surgery, including halogen, xenon, and metal halid. Each has advantages and disadvantages that have been described. The most recent innovation in light sources involves the use of light emitting diodes, or LED light. In terms of balancing the need for optimal illumination while reducing the potential to induce phototoxicity, perhaps the greatest advantage of LED endoilluminators is that its wavelengths can be split, thus allowing the operator to customize the spectral composition of the light.

Figure 1. The surgeon can change the color during surgery using the side switch of the wireless pedal.
With the Oertli OS4 platform, the surgeon can change color during surgery using the pedal switching between three programmable presets for light color, thus permitting the ability to apply light according to specific situation (Figure 1).
But choosing the composition of light is about more than reducing the risk of phototoxicity. Studies are starting to show that different spectrums of light may be assistive in visualizing certain aspects of vitreoretinal surgery. For instance, amber or yellow light may amplify the appearance of Brilliant Blue staining, and other spectrums may be more relevant for other surgical steps (Figure 2).4 Despite concerns in this area, use of spectral filters does not appear to have any effect on contrast sensitivity.5
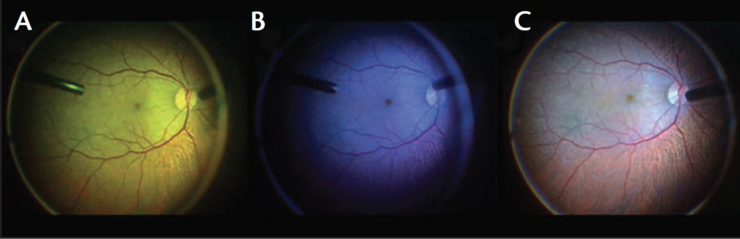
Figure 2. Different lighting options available: predominantly yellow (A), predominantly blue (B), and white lighting (C).
Interindividual Variability in Light Perception
An additional benefit for the ability to switch between different light compositions during vitreoretinal surgery is that every individual perceives light differently. This principle adds additional significance to the ability to change color composition using the footpedal while performing surgery with the Oertli OS4. Different parts of the retina, macula, and vitreous will appear differently to different surgeons using different compositions of light—especially if the tissues are differentiated using staining mediums.
There is another optical principle that comes into effect during retinal surgery that becomes relevant. Rayleigh scattering, named for British physicist Lord Rayleigh, describes the scattering of light when the particles are smaller than the wavelength. The shorter the wavelength, the more the light scatters. This phenomenon, which can be overcome by the potency of the wavelength, explains why the sky is seen as blue, but also why white light in the vitreous is only seen as a scatter effect. But we can take advantage of this principle if the diodes in the light source are adjustable; remnant vitreous is much easier to see with blue versus amber light, whereas amber light overcomes the reflections that are often apparent during fluid-air exchange. During membrane peeling, switching between different compositions of light changes what the surgeon sees, especially if epiretinal membrane, which has a wrinkled surface, is present.
Conclusion
How light is perceived is highly individualized, and, therefore, there is rationale for being able to adjust how light is used during a surgery (Table 2 ). The light can be adjusted by a number of factors, including the microscope used, the aperture, and the use of filters. But because every individual perceives light differently, it is important for every surgeon to be able to find his or her personal light settings (Figure 3). Of course, to be able to do that requires the advanced functionality built into the surgical platform enabling the operator to do so, and this feature is only available on the OS4 platform.

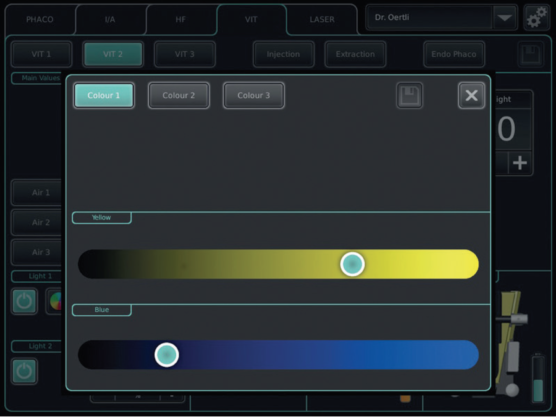
Figure 3. Yellow or blue can be added and mixed, the intensity increased or decreased.
1. Fuller D, Machemer R, Knighton RW. Retinal damage produced by intraocular fiber optic light. Am J Ophthalmol. 1978;85(4):519-537.
2. International Organization for Standardization. Ophthalmic instruments-Fundamental requirements and test methods-Part 2: Light hazard protection. ISO 15004-2:2007.
3. van den Biesen PR, Berenschot T, Verdaasdonk RM, et al. Endoillumination during vitrectomy and phototoxicity thresholds. Br J Ophthalmol. 2000;84(12):1372-1375.
4. Saxena S, Meyer CH; International Chromovitrectomy Collaboration. A trichrome RGB endoillumination prototype system: a novel application for chromovitrectomy. Ophthalmologica. 2013;230 Suppl 2:73-76.
5. Henrich PB, Valmaggia C, Lang C, Cattin PC. The price for reduced light toxicity: Do endoilluminator spectral filters decrease color contrast during Brilliant Blue G-assisted chromovitrectomy? Graefes Arch Clin Exp Ophthalmol. 2014;252(3):367-374.

