Sponsored by Oculentis

Every once in a while, a patient comes in for an evaluation and you aren’t quite sure what the best course of action will be to ensure that the patient has the best possible visual outcomes. The following scenario was one of those cases. It highlights the importance of taking time to diagnose the patient properly and also the benefit to combining procedures when warranted to achieve optimal results.
BACKGROUND
A service technician at Teleon, the European distributor of the LENSAR Laser System (Lensar), came to our clinic requesting refractive surgery to treat his myopia and astigmatism. At 56 years old, he had not had a proper ophthalmic checkup in the past 20 years. On preoperative examination, subjective refraction in his right and left eyes was -2.25 -1.00 x 21° (best corrected distance visual acuity [BDVA], 0.1 logMAR) and -2.00 -1.50 x 170° (BDVA, 0.0 logMAR), respectively. Upon further preoperative testing, it was determined that the patient also had concomitant glaucoma; IOP in his right and left eyes was 21 and 24 mm Hg, respectively, on the Humphrey Visual Analyzer (Carl Zeiss Meditec; Figure 1).
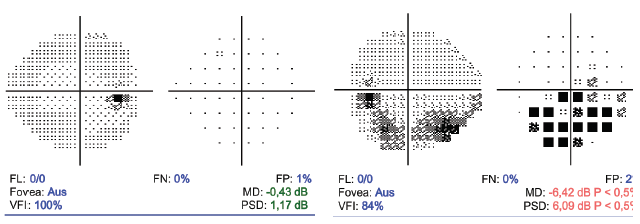
Figure 1. Preoperatively, the patient’s IOP was 21 mm Hg OD and 24 mm Hg OS.
A closer look at the optic nerve (Figure 2) revealed an elevated cup-to-disc ratio of 0.5 on the patient’s right eye and 0.8 on his left, with slight reduction of the retinal nerve fiber layer on the left eye. This corresponded with the findings in the patient’s visual field analysis. There was no decrease in contrast sensitivity or in the adaptation time.
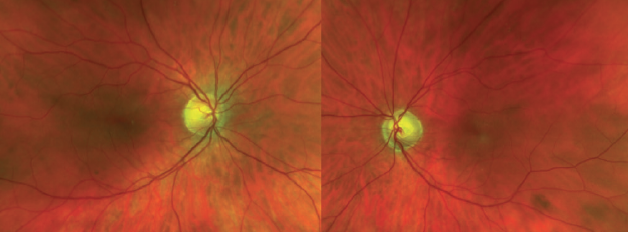
Figure 2. Fundus photographs of the patient’s eyes.
DECISION TIME
With all of this information, it was time to decide what refractive surgical procedure would most benefit the patient. Choosing between LASIK and refractive lens exchange (RLE), the patient elected for a RLE procedure. We then together decided that, rather than a monofocal, bifocal, or trifocal IOL, we would implant an extended depth of focus (EDOF) IOL in order to ensure that the patient had the best opportunity for improved, continuous quality of vision across all distances.
The major benefits of EDOF IOLs include that they do not split light rays like a multifocal lens does, that they improve intermediate and near vision while maintaining comparable distance vision, and that they mitigate the effects of presbyopia by extending depth of focus. Our EDOF IOL of choice is the LENTIS Comfort MF15 (Oculentis) with a blended vision (BV) procedure. In this case, we planned to implant a LENTIS Comfort, which has an add of 1.50 D, bilaterally and target emmetropia in the patient’s right eye and -1.50 D myopia in his left (Figure 3).
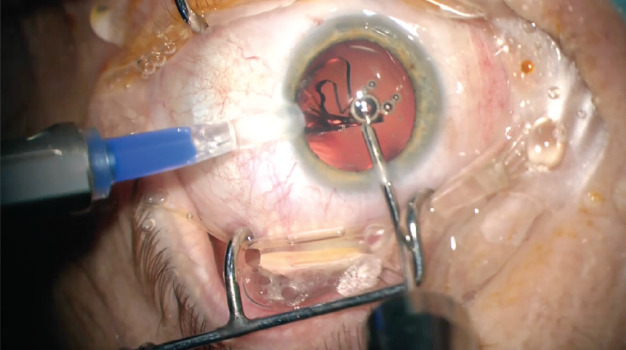
Figure 3. The LENTIS Comfort MF15 BV is implanted.
The LENTIS Comfort line of IOLs is based on the company’s Mplus IOL technology, which has a patient satisfaction rate of more than 96% (data on file with the company). The Comfort IOLs have a single, blended vision transitional zone that provides excellent intermediate and distance vision that is comparative to a monofocal, with excellent contrast sensitivity and optimized depth of focus. We thought it would be an excellent choice in this case.
We also opted to perform the procedure as a laser cataract surgery procedure with the LENSAR femtosecond laser (Figure 4), also creating arcuate incisions to treat the patient’s astigmatism. After creating a laser capsulotomy and softening the nucleus with the LENSAR, we performed gentle phacoemulsification to remove the nucleus. Due to the use of the laser, there was no need for ultrasonic power during phacoemulsification. Thereafter, we implanted the LENTIS Comfort MF15 BV in combination with a capsular tension ring to achieve the best positioning of the IOL and to prevent capsular bag shrinkage.
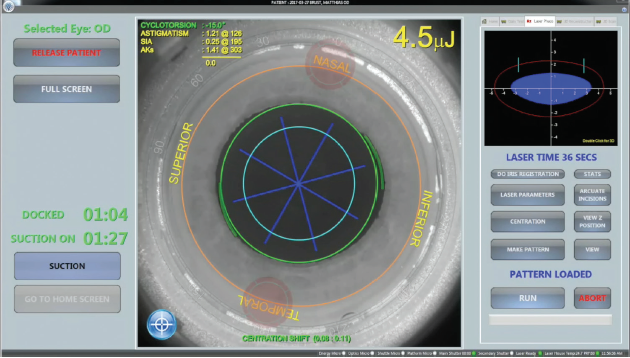
Figure 4. Laser cataract surgery was performed with the LENSAR Laser System.
Lastly, as another adjunct to the RLE, we decided to address the patient’s glaucoma by placing two iStent injects (Glaukos) in each eye. This microinvasive glaucoma surgery procedure is straightforward and, in my hands, produces excellent IOP-lowering results. A video of the procedure can be viewed at bit.ly/klabe1118.
POSTOPERATIVE RESULTS
At 6 and 12 months postoperative, the patient was extremely thrilled with his vision, and visual results were perfect. Refraction in his right and left eyes had improved to 0.00 -0.25 x 110° (BDVA, 0.0 logMAR) and -1.50 -0.25 x 140° (BDVA, 0.0 logMAR), respectively. His IOP had also improved significantly, to 12 to 16 mm Hg in his right eye and 12 to 15 mm Hg in his left. Further, what is also impressive was the obvious improvement of the patient’s visual field rating over time, especially in his left eye (Figure 5).
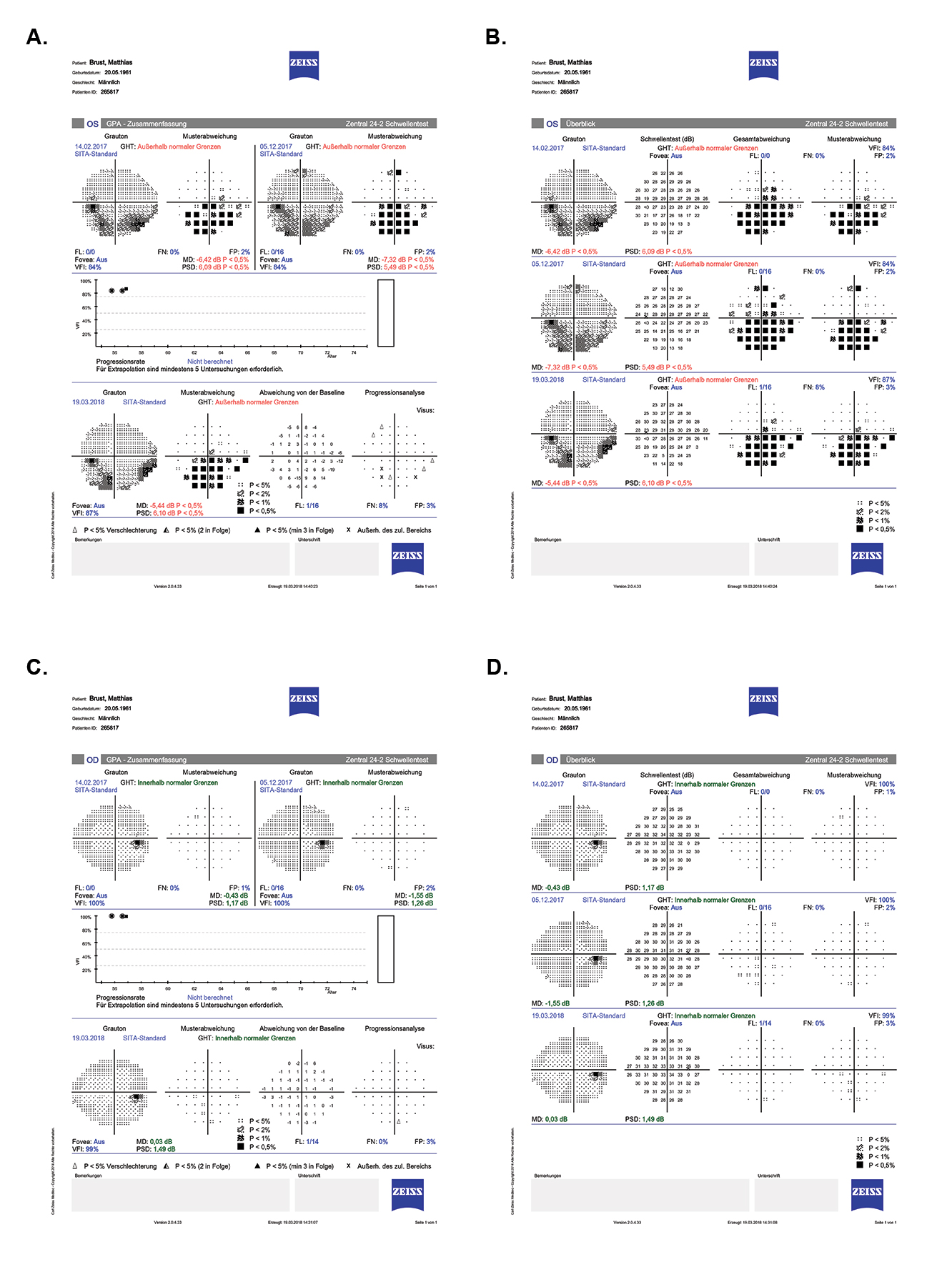
Figure 5. Visual field ratings in the patient’s left (A,B) and right (C,D) eyes.
This case was so interesting because I was able to treat someone in the ophthalmology industry, who had not had an ophthalmic examination in more than 20 years, with exceptional outcomes. This case demonstrates the excellent postoperative results that can occur after combined procedures. It also highlights the usefulness of a state-of-the-art EDOF IOL technology, the LENTIS Comfort MF15 BV, even in the presence of mild to moderate glaucoma and elevated IOP.

