Femtosecond laser treatment of the phakic lens is a procedure intended to restore accommodation or to improve distance corrected near visual acuity (DCNVA) in presbyopes. The theory behind the treatment is to use the femtosecond laser to cut predefined ablation patterns into the phakic lens as a means to increase the bulk flexibility of the lens.1 The primary goal of this procedure is to allow the stiffened, presbyopic lens to regain some flexibility, thus enabling the natural accommodative mechanism via the capsule, zonular fibers, and ciliary muscle contraction to produce some functional accommodative optical change in power to the presbyopic eye.
AT A GLANCE
• Lens stiffening is the root cause of the age-related decline in accommodative amplitude that characterizes the progression of presbyopia.
• Femtosecond laser treatment of the lens is not intended to reverse or undo the age-related molecular structural changes but rather to provide an alternative means of reducing overall bulk stiffness of the presbyopic lens.
• A fundamental prerequisite for the success of this approach is that the femtosecond laser treatment does not induce cataract or reduce visual acuity.
With increasing age, the lens gets stiffer, and accommodative amplitude is lost. This progressive stiffening of the lens is due to structural changes in crystallins (ie, water-soluable proteins), and it results in aggregation of crystallins as well as crosslinking and precipitation of the proteins out of solution as insoluble aggregates.2
Femtosecond laser treatment of the lens is not intended to reverse or undo the age-related molecular structural changes in the lens, but rather to provide an alternative means to reduce the overall bulk stiffness of the presbyopic lens. After using the femtosecond laser to cut into the lens, the expectation is that, with accommodation, the capsule will be able to mold the modified lens to such an extent that it can alter lens shape, increasing the lens surface curvatures and thereby optical power. Prior studies have shown that laser treatment can reduce overall bulk stiffness of the lens.3,4
Because the laser procedure does not involve entering the eye manually and does not cut the lens capsule, the possibility exists that laser softening of the lens could also alter the lens shape and thus change the resting refraction or aberrations of the eye. If the laser treatment patterns can be implemented to modify the shape of the lens in predefined and controlled ways, this procedure may also improve DCNVA through increasing the depth of focus of the eye. This would be achieved by altering the natural aberration structure of the lens. In this way, femtosecond laser treatment of the lens could produce beneficial effects by changing the spherical aberration of the eye, for example.
Extensive finite element analysis and optical modeling has been used by Lensar to aid in the design of its laser treatment patterns for presbyopia correction in an effort to optimize the predictability and outcomes of these treatments. Rowiak is another company investigating this technique.
PRELIMINARY STUDY
Lensar conducted a preliminary study using the Lensar Laser System in 80 eyes of 80 patients scheduled for cataract surgery.5 The protocol called for all patients who had undergone laser lens softening to complete a 1-month follow-up study before electing to proceed with lens removal during cataract surgery. Follow-up testing included objective accommodation measurements with a Grand-Seiko autorefractor, subjective accommodation testing with the push-down method, and testing of DCNVA.
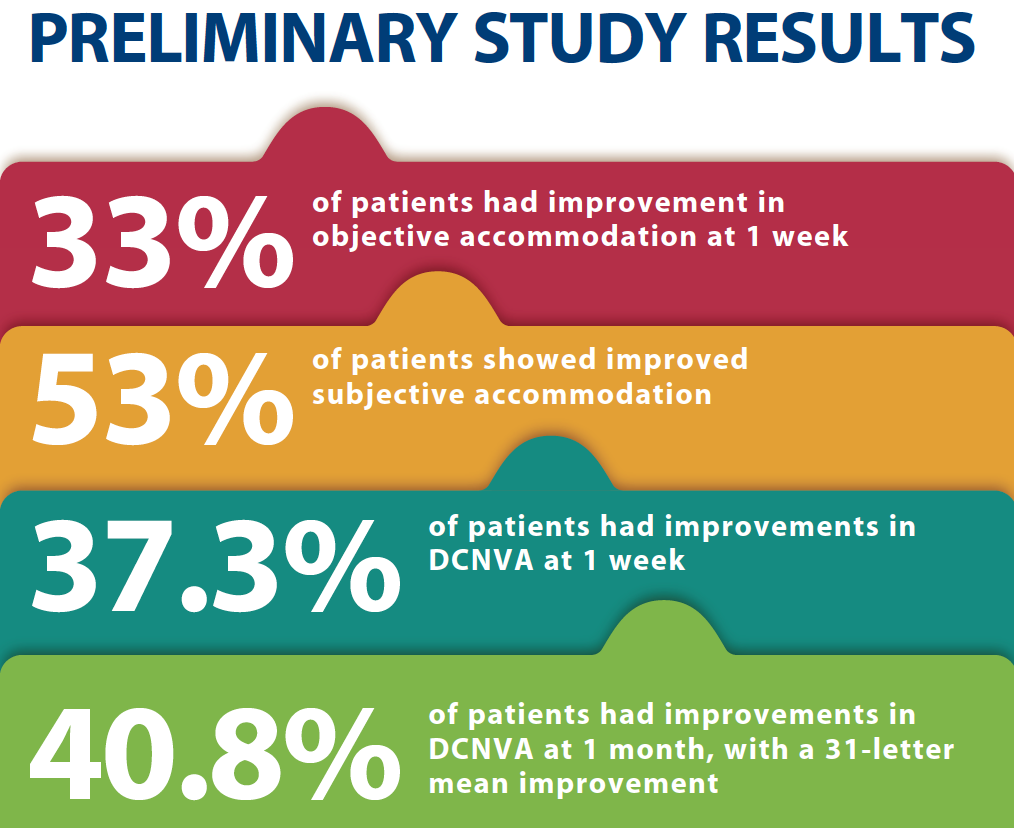
Improvement in objective accommodation was observed in 33.3% of patients at 1 week. Fifty-three percent showed improved subjective accommodation. Improvement in DCNVA was observed in 37.3% of patients at 1 week and 40.8% at 1 month, with a 31-letter mean improvement.
FURTHER STUDY
Following this preliminary investigation, another study was initiated in January 2015 at the Pacific Eye and Laser Institute in Makati City, Philippines. This study included 37 eyes of 37 patients, aged 45 to 60 years, who had elected to undergo cataract surgery with IOL implantation. Follow-up was a maximum of 6 months, and the contralateral eye served as a control eye for all post-procedure testing.
Several promising laser patterns were used in this study. The treatment parameters included variations in laser power, laser patterns, and placement of the laser incisions in the lens. All patterns included sparing of the lens optical axis to ensure that the laser treatments did not cause an increase in light scatter or reduction of visual acuity along the optical axis. A fundamental prerequisite for the success of this kind of procedure is that the femtosecond laser treatment does not induce cataract or reduce visual acuity.
The protocol included two pre- and postoperative measures of DCNVA, subjective accommodation using the push-down test, objective accommodation and wavefront measurements with the iTrace aberrometer (Tracey Technologies), and defocus curve testing. A comprehensive analysis of the data is under way, including objectively measured accommodative amplitude from the iTrace aberrometer, subjective accommodation, improvements in DCNVA, and wavefront analysis of factors that may improve accommodation or DCNVA through alterations to the aberrations of the eye. Two preoperative test days allow same-eye pre- and postoperative comparisons, and the untreated eye serves as a control eye for repeat testing.
CONCLUSION
Lens stiffening is the root cause of the age-related decline in accommodative amplitude that characterizes the progression of presbyopia. Procedures aimed at reducing the stiffness of the lens to allow the natural accommodative mechanism to function again or to increase the depth of focus of the eye may hold promise for restoring accommodation or improving DCNVA in presbyopic eyes. Femtosecond laser treatment of the presbyopic lens offers a promising, noninvasive approach to reduce lens stiffness, restore accommodation, and improve DCNVA.
1. Myers RI, Krueger RR. Novel approaches to correction of presbyopia with laser modification of the crystalline lens. J Refract Surg. 1998;14(2):136-139.
2. Hanson SR, Hasan A, Smith DL, Smith JB. The major in vivo modifications of the human water insoluble lens crystallins are disulfide bonds, deamidation, methionine oxidation and backbone cleavage. Exp Eye Res. 2000;71:195-207.
3. Krueger RR, Sun XK, Stroh J, Myers R. Experimental increase in accommodative potential after neodymium: yttrium-aluminum-garnet laser photodisruption of paired cadaver lenses. Ophthalmology. 2001;108(11):2122-2129.
4. Schumacher S, Oberheide U, Fromm M, et al. Femtosecond laser induced flexibility change of human donor lenses. Vision Res. 2009;49(14):1853-1859.
5. Gil-Cazorla R, Naroo S, Uy H; Shah S. Lens softening with a femtosecond laser. Cataract & Refractive Surgery Today Europe. July/August 2014.
Adrian Glasser, PhD
• Adrian Glasser Consulting Services
• adrianglasser@gmail.com
• Financial disclosure: Consultant (Lensar)
Sunil Shah, MBBS, FRCOphth, FRCS(Ed)
• Midland Eye, Solihull, West Midlands, United Kingdom
• Birmingham & Midland Eye Centre, Birmingham,
United Kingdom
• sunilshah@doctors.net.uk
• Financial disclosure: Investigator (Lensar)
Harvey S. Uy, MD
• Private practice, Peregrine Eye and Laser Institute, Makati, Philippines
• harveyuy@yahoo.com
• Financial disclosure: Principal investigator (Lensar)