If you had €100,000 to invest in your practice, what would you do with it? What about €500,000? CRST Europe asked several influential ophthalmologists to weigh in on how they would spend these amounts to enhance their practices.
Did you know?
IntelliAxis
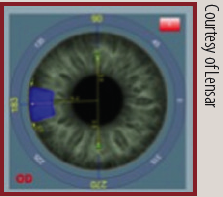
When implanting a toric IOL, surgeons can use the IntelliAxis feature of the Lensar Laser System to establish visible steep axis landmarks on the cornea.
Centurion Vision System

The Active Fluidics feature of the Centurion allows surgeons to work in a more consistent physiologic IOP range, improving control over ocular fluidics. It works in three steps: (1) the surgeon selects the target IOP, patient eye level, irrigation factor, and leakage flow rate, (2) the system monitors, detects, and compensates for changing pressure, and (3) the system automatically adjusts fluid compression to maintain the target IOP.
Investment in New Laser Technologies

Detlev R.H. Breyer, MD
I subspecialize in minimally invasive refractive premium cataract surgery, and I rely on a femtosecond laser to enhance the patient experience. If I had €100,000 to invest, I would put it toward making refractive lens exchange (RLE) even safer and more perfect for our patients than it already is. My most recent investment was in the IntelliAxis system (Lensar), which integrates with the Cassini Total Corneal Astigmatism device (i-Optics) to provide the best solution for toric IOL implantation with cyclotorsion control available at this time.
I now want to push the limits toward perfect removal of the nucleus. No machine is better right now to ensure a stable anterior chamber than the active fluidics system of the Centurion Vision System (Alcon). Combining this device with the Cetus nanosecond laser (A.R.C. Laser) would allow me to remove the laser-fragmented nucleus without ultrasound energy and induce almost no corneal endothelial loss; this would be another giant step toward perfect and safe cataract surgery. Other attractive features of the Cetus include reduction of posterior capsular opacification (PCO), hygienic single-use handpieces, and a low rate of iatrogenic posterior capsular breaks. Therefore, my €100,000 would be invested in the Cetus.
If I had €500,000 to invest, the choice would be easy: the all-in-one Femto LDV Z8 femtosecond laser (Ziemer Ophthalmic Systems). This transportable femtosecond laser is comparable to a Swiss Army knife: It can perform LASIK flaps, pockets for intrastromal corneal rings, corneal graft incisions, corneal incisions, cataract fragmentation, and—for study use only—even circular keratotomy. Can it get any better?
A Technology to Detect Backscatter

Arthur B. Cummings, MB ChB, FCS(SA), MMed(Ophth), FRCS(Edin)
If I had €100,000 at my disposal for investment in capital equipment, I would acquire Visiometrics’ HD Analyzer (I know this is true because I recently did just that.) This device helps the surgeon make quick decisions about whether a patient is an appropriate candidate for corneal refractive surgery versus IOL surgery. In the past, when I detected early nuclear sclerosis changes in a patient’s lens, I would advise the patient to wait a year and return for a follow-up exam to monitor the condition. Most would not come back, as over the course of a year their priorities or circumstances would have changed, and my initial uncertainty may have spooked them a bit. With the HD Analyzer, if the patient’s lens is clear of backscatter, I feel confident offering corneal refractive surgery. If there are lens changes, I know that the best advice is to choose lens replacement. Remember, at the slit lamp we see forward scatter, but what the patient is aware of is backscatter. Before the availability of this technology, the examiner could not visualize that. The same device has an excellent mode for assessing the optical quality of the tear film, and this works extremely well for educating and motivating patients to work with us in improving their meibomian gland dysfunction.
Did you know?
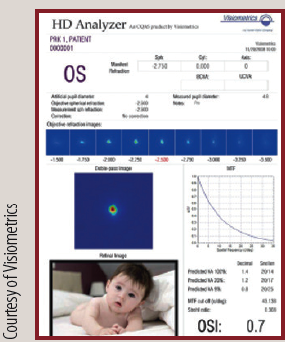
HD Analyzer
The Objective Scatter Index of the HD Analyzer can aid in suggesting the best time for lens replacement with an IOL.
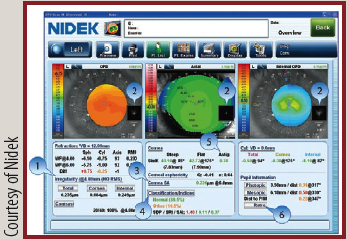
OPD-Scan III
The device’s overview summary provides essential measurements and analysis data, including corneal irregularities separated into total, corneal, and internal (1), point spread function images that simulate objective retinal visual quality from each component of the eye (2), corneal spherical aberrations (3), color-coded classification indices that help to identify post-LASIK ectasia and keratoconus (4), astigmatism index (5), and retroillumination image of cataracts captured during the exam (6).
After this investment there would still be funds free, and I would look to spend it on the MiBoFlo ThermoFlo (Mibo Medical Group) therapeutic device for dry eye disease (DED). Meibomian gland dysfunction is a common problem, especially with the number of hours that people now spend looking at computer, tablet, and smartphone display screens and, as a result, not blinking properly. Other alternatives are too expensive, and the MiBoFlo appears to offer a good alternative to help improve evaporative DED.
I have been slow to take up laser-assisted cataract surgery (LACS), but perhaps, if I had €500,000 available to invest, I might just do it now. LACS has been around long enough to have established itself as a safe and effective treatment for cataracts. I have not seen convincing data to suggest that it is any better than standard phacoemulsification in terms of vision and refractive outcomes, but there is no doubt that it increases the precision and repeatability of the capsulorrhexis procedure, providing reliable sizing and positioning. The lens fragmentation mode results in a lower use of phaco power during the lens extraction part of the procedure, leading to a lower incidence of ultrasound-related complications. Some patients like being treated with the latest technology, especially if it reduces the possibility of human error. With very low uptake of LACS in Ireland to date, the timing might be good now to achieve a marketing benefit from this investment.
Share the Risks by Investing in a Surgicenter

Sheraz M. Daya, MD, FACP, FACS, FRCS(Ed), FRCOphth
I have made considerable investments in my practice recently, which includes two surgical facilities and a satellite consultation facility. Any further investments right now would be in technology that would be nice to have but that would probably provide no additional revenue. I would rather not name these technologies for fear of offending the manufacturers. A better approach might be to put myself in the place of a surgeon newly in practice, one who wants to consider what will bring the best value for his or her monetary investment. I will make the assumption that this individual is a cataract and refractive surgeon and is establishing an office for the first time.
With €100,000 to invest, item No. 1 for a surgeon with a new practice would be the Refractive Power/Corneal Analyzer OPD-Scan III (Nidek; also see Figure 1, pg 44), a sophisticated device that provides a considerable amount of valuable diagnostic information including autorefraction, autokeratometry, corneal topography, ocular aberrometry, and internal aberrometry (derived by subtracting corneal aberrometry from overall aberrometry). Additionally, the device measures pupil size in photopic and mesopic conditions, average pupil power, white-to-white distance, and deviation of the line of sight from the pupil center. All of the above are useful for planning laser refractive surgery, phakic IOL implants, and RLE. The utility of the device itself could be the subject of numerous articles; however, suffice it to say that it provides a wealth of useful information.
Did you know?

Victus Femtosecond Laser Platform
The curved patient interface of the Victus can be docked two ways: the noncontact docking used in cataract surgery uses a thin liquid layer separating the cornea from the interface, and the full-contact docking used in corneal applications optimizes stability. Surgeons can change modalities during procedures.
Leica M720 OH5 and M525 OH4 surgical microscopes
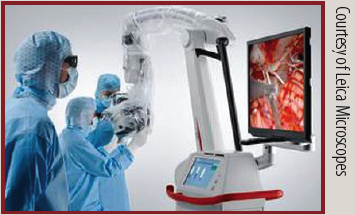
Visualization in 3-D can improve understanding, engagement, and knowledge retention.1 High-definition, 2-D and 3-D surgical video can be streamed to monitors in the operating room or over distance to enhance staff education.
1. 2010 Texas Instruments educational study.
Item No. 2 would be some means of performing biometry and lens calculations, preferably a device with built-in modern IOL formulas, especially the Holladay 2, which is my personal preference for the vast majority of patients. Devices that fit this description include the IOLMaster (Carl Zeiss Meditec), the AL Scan (Nidek), and the Lenstar (Haag-Streit).
Item No. 3 would be the Pentacam (Oculus) device for Scheimpflug tomography. This technology provides vital information about the cornea and bestows a phenomenal level of comfort when it comes to performing corneal procedures, specifically laser ablative surgery.
With these three technologies, the young practitioner would be able to comfortably and accurately plan surgery for more than 80% of his or her patients, and they would also provide good sources of revenue.
If I were in a similar position and had €500,000 to spend in addition to the above, I would seriously consider partnering with fellow ophthalmologists to establish a surgical facility. The capital requirement to establish a high-end, fully compliant operating room with appropriate ventilation, an operating microscope, phacoemulsification machine, monitoring equipment, surgical instruments, stock, and sundries is approximately €2.5 million. The €500,000 could be used as a down payment, with the balance taken as a loan. However, for an individual, this course of action could result in a lack of working capital and a high risk of cash-flow problems. These risks could be reduced considerably by sharing the investment with like-minded colleagues. If this were done, in no time, enhanced technologies such as a femtosecond laser for cataract surgery could be considered, along with an excimer laser. My personal choice would be the Victus femtosecond laser, as it has the ability of doing both cataract and refractive surgery, and the Teneo 317z excimer laser (both by Bausch + Lomb Technolas).
A New Microscope, a New Laser

Detlef Holland, MD
Recently I had the opportunity to test drive the heads-up TrueVision 3D Visualization System available on the M720 OH5 and M525 OH4 surgical microscopes (Leica Microscopes). This is a fascinating technology through which the surgeon and the entire surgical team can see anterior and posterior segment surgery with 3-D depth perception and without looking through the microscope oculars. Before testing it myself, I thought that the experience would be different from traditional microscopes and would require a long learning curve. When the tryout started, in the first two patients I did only the clear corneal incisions and capsulotomy using the heads-up display, but, by the third patient, I was confident enough to perform the whole cataract surgery without a large loss of time. The quality of the picture regarding the 3-D view is comparable to the view through a standard stereo microscope. The resolution of the picture is not as high as with traditional microscopy, but this will improve, as improvement occurs with all new technologies. This is a technology that might represent a worthwhile capital investment. I believe this mode of viewing will be important for the future training of young doctors and will provide a great opportunity for live surgery presentations, which is why I would use €100,000 to purchase either the M720 OH5 or the M525 OH4 microscope.
If I could invest €500,000 at this moment, I would acquire the technology for small incision lenticule extraction (SMILE). We have a Schwind eye-tech-solutions excimer laser system that provides excellent results in LASIK, PRK, and PTK. The VisuMax femtosecond laser system (Carl Zeiss Meditec) would provide an important tool that is currently lacking in our clinic. Patients are increasingly expressing interest in this surgical method, and it is a disadvantage for our clinic not to have the opportunity to offer it to them. The technique is safe and precise, and the ability to offer it would have a positive effect on our marketing efforts.
Tears and SMILEs

Michael Lawless, MBBS, FRANZCO, FRACS
If I had €100,000 to invest—or, in my case, 100,000 Australian dollars (AU$)—I would buy a Tear Osmolarity System (TearLab) and a LipiView II ocular surface interferometer (TearScience) for DED diagnosis and a LipiFlow Activator (TearScience) treatment device. Then I would invest in educating a key staff member to care for dry eye patients and would set this up as a standalone area within the practice dealing with DED.
If I had AU$500,000 to invest in the practice, I would buy a VisuMax femtosecond laser to allow me to perform SMILE. In fact, this is exactly what we did nearly 2 years ago. This has proven to be a clinical success, and good things always flow from that. Of my patients who are suitable for corneal laser refractive surgery, 60% now undergo SMILE, 30% LASIK, and 10% PRK. Our message is that all three are great procedures, and I select the one that is best for the individual patient.
New Ways of Seeing

Gilles Lesieur, MD
For an investment of less than €100,000, a practice can acquire a Pentacam for topographic analysis of the posterior cornea. This technology is key for diagnosis of keratoconus, for assessing spherical aberration to allow IOL customization in cataract surgery, and for measuring anterior and posterior astigmatism and total axis.
DID YOU KNOW?
AngioPlex
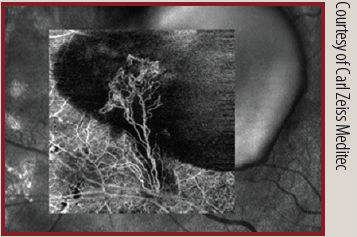
Available on the Cirrus 5000 HD-OCT platform, AngioPlex is powered by optical micro angiography algorithms, which use amplitude and phase OCT signal data to produce detailed images and to minimize scan acquisition times. It can be used to illustrate the presence of microaneurysms, areas of ischemia, and choroidal neovascularization, and it can delineate the location of retinal vein occulsions and affected areas of ischemia.
For posterior segment analysis, several technologies fit in this price range. The IOLMaster 700 (Carl Zeiss Meditec) with swept-source OCT technology provides accurate optical biometry, and I anticipate that new features will be introduced on this device in the near future. Or, for a little bit more than €100,000, a practice could purchase a device for OCT angiography, such as AngioPlex OCT (Carl Zeiss Meditec). This technology promises to usher in a new era of retinal analysis.
With an investment of less €50,000, a practice that has an existing Zeiss microscope in its operating room (OR) could buy an image-guided system such as the Callisto eye (Carl Zeiss Meditec). These are fantastic systems that can assist the surgeon in capsulorrhexis sizing and toric IOL orientation. With the Callisto system in my OR, I now perform 65% of my cataract surgeries with toric IOL implantation. Many developments will be forthcoming to improve the safety and accuracy of surgical results with these systems.
For an investment of €500,000 a practice can acquire a femtosecond laser for LACS; however, with a significant rate of capsulorrhexis tag formation, in my opinion, it would be smarter to wait for improvements in the technology before investing. The exception is if you want to establish yourself as a leader in a competitive area.
In my own practice, the most important acquisitions since 2006 have been our Scheimpflug and OCT imaging devices. Investments in capital equipment this year have included the Tonoref III autorefractor/autokeratometer/tonometer/pachymeter (Nidek), the AngioPlex, and the IOLMaster 700.
High-Quality Microscopes and Technologies That Enhance Surgical Precision

Abhay R. Vasavada, MS, FRCS
Today, every specialty of medicine, and especially ophthalmology, is dominated by technology. With the variety of options at our disposal, it often becomes difficult to decide which of these technologies is best for our practices. However, there are certain basics that have to be kept in mind when investing in new technologies. With a capital investment of €100,000, a practice could acquire an excellent operating microscope or a top-notch phacoemulsification device.
My top priority when I invest is to make sure I have a good operating microscope. My criteria include a good red reflex and good depth perception. Nowadays, it is important not only to have a good view for the surgeon but also to be able to produce high-quality video displays and then record those videos. Therefore, when I procure a microscope, I prefer one with a beam-splitter with a ratio of 50/50, in which 50% of the light goes to the surgeon and 50% to the camera.
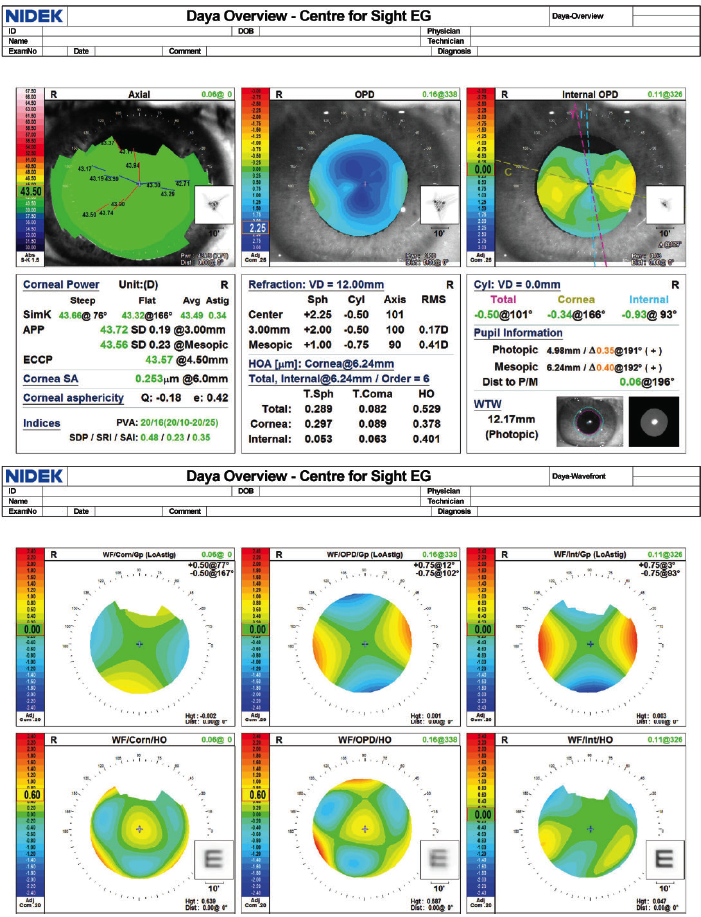
Figure 1. Overview screen of the OPD-Scan III.
Courtesy of Sheraz M. Daya, MD, FACP, FACS, FRCS(Ed), FRCOphth
After the microscope, as an anterior segment surgeon, I prioritize a good phacoemulsification system. Ultrasound efficiency and fluidics are equally important for the good performance of a phaco system. My personal preference is the Centurion Vision System. The reason is that it gives me a great combination: torsional ultrasound and active fluidics. The torsional modality increases the efficiency of ultrasound energy, reduces chatter, and makes lower aspiration parameters more effective. The active fluidics feature allows the surgeon to preset a desired IOP during cataract surgery, thus minimizing IOP-related damage in the eye. Whatever system you choose, always look for efficiency as well as safety in terms of surge protection.
If I had at my disposal a larger budget of €500,000, my investment would go toward better diagnostics. In particular, OCT, optical or swept-source biometry, and aberrometry are tools that can enhance cataract practice for every surgeon, particularly in this era when cataract surgery is being equated with refractive surgery. Precision in IOL calculations and the ability to detect subtle retinal or other ocular problems are important for decision-making with advanced technology IOLs, as well as for counseling patients and managing their expectations.
If I already had all of these diagnostic tools and still had €500,000 at my disposal, I would invest in femtosecond laser technology for both cataract and refractive surgery. n
Detlev R.H. Breyer, MD
• Head, Breyer.Kaymak.Klabe Eye Surgery, Düsseldorf, Germany
• Member, CRST Europe Editorial Board
• detlev.breyer@web.de
• Financial interest: None acknowledged
Arthur B. Cummings, MB ChB, FCS(SA), MMed(Ophth), FRCS(Edin)
• Consultant Ophthalmologist, Wellington Eye Clinic and Beacon Hospital, Dublin, Ireland
• Associate Chief Medical Editor, CRST Europe
• abc@wellingtoneyeclinic.com
• Financial disclosure: Consultant (Alcon, WaveLight)
Sheraz M. Daya, MD, FACP, FACS, FRCS(Ed), FRCOphth
• Director and Consultant Surgeon, Centre for Sight, East Grinstead, United Kingdom
• Chief Medical Editor, CRST Europe
• sdaya@centreforsight.com
• Financial disclosure: Consultant (Nidek, Bausch + Lomb)
Detlef Holland, MD
• nordBLICK Augenklinik Bellevue, Kiel, Germany
• Member, CRST Europe Editorial Board
• d.holland@nordblick.de
• Financial disclosure: Consultant (Lensar)
Michael Lawless, MBBS, FRANZCO, FRACS
• Vision Eye Institute, Chatswood, New South Wales, Australia
• Clinical Associate Professor, Sydney Medical School, University of Sydney, New South Wales, Australia
• Member, CRST Europe Global Advisory Board
• michael.lawless@visioneyeinstitute.com.au
• Financial interest: None acknowledged
Gilles Lesieur, MD
• Ophthalmologic Center Iridis, Albi, France
• Member, CRST Europe Editorial Board
• g.lesieur@centre-iridis.fr
• Financial disclosure: Consultant (PhysIOL), Investigator (Bausch + Lomb, Carl Zeiss Meditec), Recipient of royalties (PhysIOL ophthalmic knives, Rumex instruments)
Abhay R. Vasavada, MS, FRCS
• Director, Raghudeep Eye Clinic, Iladevi Cataract & IOL Research Centre, Gujarat, India
• Member, CRST Europe Global Advisory Board
• icirc@abhayvasavada.com
• Financial disclosure: Research support (Alcon)



