Case Presentation

A 27-year-old woman with high myopia and thick corneas expressed interest in refractive surgery. She wore soft contact lenses but was unhappy with them, and she was motivated to undergo surgery. The refraction in her right eye was -8.50 -2.25 X 180º, and in her left it was -12.25 -3.00 X 180º. CDVA was 20/20 in both eyes. Central pachymetry was 614 µm in her right eye and 595 µm in her left, and the topography looked good in both eyes (Figures 1 and 2).
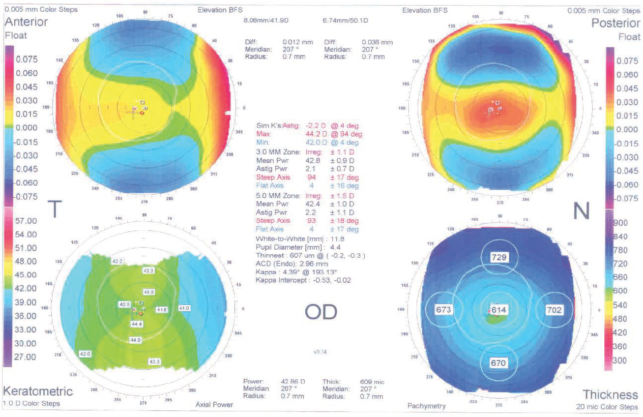
Figure 1. Preoperative topography in the patient’s right eye, with normal findings.
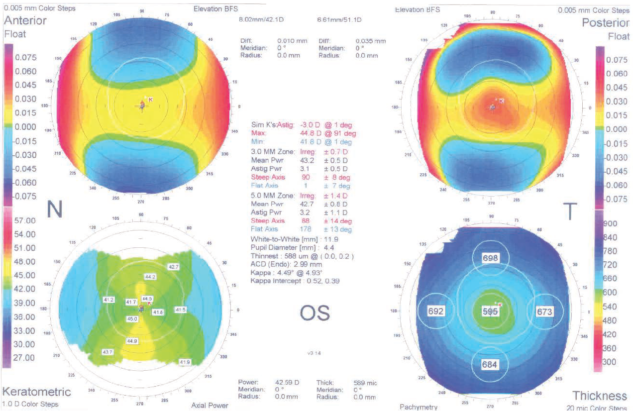
Figure 2. Preoperative topography in the patient’s left eye, with normal findings.
This patient was relatively well educated about refractive surgery options. She had heard about the Evo Visian ICL (STAAR Surgical) and about LASIK. She had a number of questions:
- What was the safest option for her?
- What procedure has the best results?
- How many of these procedures had I done?
- What procedure leaves her with the most future options? (ie, Will the proposed procedure mess up her eyes for IOLs or some other procedure in the future?)
- What procedure has the fewest complications?
- What about cost?
Contestants, please tell me:
- What procedure or procedures would you recommend for this patient?
- Why would you recommend this treatment?

Contestant No. 1
This patient reminds me of a comment Kenneth J. Hoffer, MD, once made: If any patient has more than three questions, fire ‘em. And if he or she starts directing the therapy, really fire ‘em.
In all seriousness, Steve, this is a fairly tough case because of the degree of myopia in the patient’s left eye. I would not feel comfortable performing LASIK for the entire amount of her myopia in that eye. That would probably mean doing a bioptics procedure, implanting a phakic IOL in combination with LASIK. If her left eye was more like her right, then I would feel more comfortable with bilateral LASIK; but -12.25 -3.00 X 180º is pushing the limit. If this were my patient, I would recommend LASIK alone in her right eye and LASIK plus the Evo Visian ICL in her left.
If I were asked this question 10 or 15 years ago, I might have chosen bilateral LASIK with no ICL. But, with a spherical equivalent of -13.75 D in the patient’s left eye, I do not think I would sleep well. Granted, this is just one case, not a series, but I think over time doing those kinds of high ablations routinely can lead to bad results that become a problem for one’s practice.

Contestant No. 2
Steve, the patient you just described is a typical patient I see in my practice. In the similar cases that I have treated, I often implant an ICL, followed
1 to 2 months later by PRK to treat the residual astigmatism. Alternatively, LASIK or PRK with mitomycin-C (MMC) may be an option for the right eye. I personally prefer PRK over LASIK for the level of myopia present in the right eye. The left eye is too myopic in my opinion for LASIK or PRK.
Although some surgeons use MMC on every PRK case, I am more selective. When performing a PRK enhancement after ICL implantation, I do not use MMC, as the ablation depth for the astigmatism is low. My cutoff for the use of MMC for haze prophylaxis is for ablations of around 60 to 75 µm. Where I am located, in South Florida, there could be worries about sun exposure causing haze if MMC was not used with PRK. With a small levels of correction, as with the PRK enhancement following the ICL procedure, there should be minimal risk of postoperative haze.
Some might ask why choose PRK instead of LASIK to enhance the residual refractive error after the ICL procedure? First, I like PRK, and, generally speaking, I think it is a safe procedure. The key is that PRK is less invasive than LASIK. In combination with the ICL, the refractive error treated with PRK will be low, so it will be a thin ablation with a low risk profile. The risk for complications with PRK after ICLs in my experience has been very low.
Returning to choosing LASIK versus PRK over an ICL for the right eye, both LASIK and PRK are appropriate options. One reason I favor PRK slightly over LASIK for high myopia is related to quality of vision. When deep ablations are performed, there is a small risk that the LASIK flap will not fit smoothly, resulting in microstriae. Microstriae can significantly affect the quality of vision. I have noticed that, on some associations’ discussion boards, some surgeons set their limit for LASIK at about -9.00 D.
Just to mention, it is a shame that the Evo Visian Toric ICL is not available in the United States, as that would eliminate both the high myopia and astigmatism in one procedure.

Contestant No. 3
In making a decision on treatment course, the truth is always in the complaints of the patient. It is important to listen for clues. For me, in the information you presented, Steve, what lights up is that she is unhappy with her contact lenses. I would like to know more about why that is. It may be that this patient has giant papillary conjunctivitis and her main complaint is discomfort, in which case she might be happy with any surgical approach. On the other hand, she might have complaints about night vision, in which case the best solution might be a more pupil-dependent approach, like a phakic IOL.
Young patients with high myopia can be overcorrected by contact lenses and spectacles. In my opinion, proper red-green refraction and also confirmation with true cycloplegia must be obtained so that a young myope does not become a hyperope. I like to take the time and explain this particular aspect to patients extensively, as they may return a year later complaining that they see better with their friend’s -1.00 D spectacles than they do their own.
Another red flag in this case, Steve, is the thickness of the patient’s corneas. In my practice, everyone who has a pachymetry of 600 µm or greater gets a thorough endothelial cell evaluation by slit lamp. She might have early Fuchs dystrophy, and thicknesses of 570 µm, and that may change the whole story.
Additionally, I would like to know who in her circle of friends has had vision correction. What procedures have they had, and what have they said about it? Did they have LASIK, PRK, or a phakic IOL, and were they satisfied with their results?
Finally, when you operate on a very high myope, there is a chance for future complications related to the high myopia that are not necessarily related to the patient’s vision correction intervention. The patient may have a peripheral retinal degeneration, a tear, or even a lingering partial limited retinal detachment. Once you operate on this patient, if there is such a complication, it is your complication. Because of a higher chance of an early cataract, I believe that a proper peripheral retinal examination, a candid conversation with the patient, and proper informed consent and documentation are in order.
As for treatment choice, if all of the above were uneventful, I would offer both LASIK and ICL. Most of my patients choose bilateral LASIK. In years past, I would have completely avoided the Evo Visian ICL in a young patient such as this because implantation would have required a peripheral iridotomy (PI)—something that is not trivial in a 27-year-old with a long axial length. In speaking to my retina colleagues, I have learned that a PI may build condensation of the vitreous posterior to the PI, increasing the risk for a retinal tear in the long term. Now that the Evo Visian ICL is available internationally, with its central hole to allow aqueous flow, I have gone back to using it. The PI is no longer required.
The Resolution
One detail that I withheld earlier is that this patient works in our office. That is one reason why she was so well educated about her choices and asked so many questions.
As for treatment, we decided to enroll her in the small incision lenticule extraction (SMILE) randomized clinical trial in which our center was participating. (Editor’s Note: The US FDA approved the VisuMax Femtosecond Laser [Carl Zeiss Meditec] for SMILE for myopia in September 2016.) That eliminated her concern about costs.
The SMILE study was randomized so that one eye of each patient received SMILE and the other eye received LASIK. As luck would have it, she was randomized to have LASIK in the eye with the higher correction and SMILE in the eye with the lower correction.
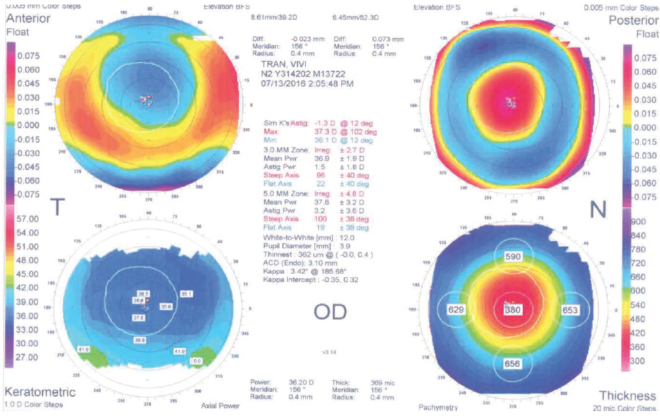
Figure 3. Topography in the patient’s right eye at 2 months postoperative.
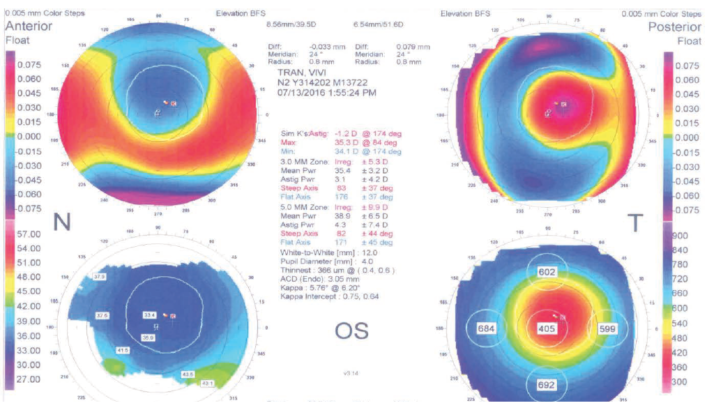
Figure 4. Topography in the patient’s left eye at 2 months postoperative.
Nonetheless, we proceeded to treat both eyes, and, at 2 months postoperative, results in both eyes were excellent: -0.50 D in her right eye, yielding 20/25-2 CDVA; and -0.25 D in her left, yielding 20/25+2 CDVA. Topographies in both eyes look good (Figures 3 and 4), and both corneas are nice and clear (Figure 5).
Figure 5. At 2 months postoperative, the patient’s corneas were clear.
She reports equal quality of vision and comfort in both eyes, which continue to improve. She initially preferred her right eye, the SMILE eye, because it was more comfortable. She currently prefers the left eye, after 2 months, because the vision is a little better.
She tells us that the SMILE eye continues to improve, and our experience in the clinical trial is that patients eventually prefer their SMILE eye after longer follow-up.
AND THE WINNER IS...
Three excellent, thoughtful comments! All the treatments described by the contestants would have been appropriate choices for the patient. Interestingly, the treatments selected by the contestants are all different: LASIK and ICL/LASIK, bilateral ICL/PRK, and bilateral LASIK.
Although we did SMILE/LASIK, none of the contestants mentioned SMILE as a treatment that they would have used. With the recent US FDA approval, that will change.
Contestant No. 2 laid out an excellent treatment plan with the patient’s safety first, and I was impressed with the breadth of consideration of the patient by this contestant. If I had not had SMILE available as a treatment option, though, I would have done LASIK and ICL/LASIK—the treatment selected by Contestant No. 1. Therefore, in the end, I choose Contestant No. 1 as the winner.
GET TO KNOW THE CONTESTANTS

WINNER
Contestant No. 1
John F. Doane, MD
• Private practice, Discover Vision Centers, Kansas City, Missouri
• Clinical Assistant Professor, Department of Ophthalmology, Kansas University Medical Center, Kansas City, Kansas
• Member, CRST Europe Global Advisory Board
• jdoane@discovervision.com
• Financial disclosure: None acknowledged

Contestant No. 2
William B. Trattler, MD
• Director of Cornea, Center for Excellence in Eye Care, Miami
• wtrattler@earthlink.net; Twitter @wtrattler
• Financial disclosure: Investor (CXL Ophthalmics)

Contestant No. 3
A. John Kanellopoulos, MD
• Medical Director, The Laservision.gr Research & Clinical Eye Institute, Athens, Greece
• Clinical Professor of Ophthalmology, NYU Medical School, New York
• Associate Chief Medical Editor, CRST Europe
• ajkmd@mac.com
• Financial disclosure: None acknowledged



