

The idea for using corneal inlays to modify refraction has been around for almost 70 years. In 1949, Barraquer introduced his idea of keratophakia—shaping donor corneal tissue on a cryolathe, and implanting it in the cornea to alter a patient’s refraction.1 Since that time, there has been a long history of attempts to find biocompatible synthetic materials and implant designs that allow the cornea to maintain its physiologic function and also predictably improve refraction.2-6
After decades of refinement of the concept, a number of corneal inlays have in recent years reached the market, and each has amassed a significant quantity of clinical data demonstrating efficacy and safety. These inlays, rather than addressing myopia or hyperopia as Barraquer and others tried to do, are designed to improve near vision in presbyopic patients. Typically, a corneal inlay is implanted under a flap or in a stromal pocket in only the nondominant eye to boost near vision, leaving distance vision mostly unchanged. In patients who are not emmetropic, a corneal inlay can be combined with LASIK.
Commercially available corneal inlays include:
• The Kamra inlay (AcuFocus). This inlay, with an opaque ring surrounding a central aperture, operates on the pinhole optical principle, increasing the implanted eye’s depth of focus. Its diameter is 3.8 mm, with a central aperture of 1.6 mm and thickness of 5 µm. The Kamra was the first corneal inlay to receive both the CE Mark and US FDA approval.7
• The Raindrop Near Vision Inlay (formerly PresbyLens; ReVision Optics). Made of transparent hydrogel, this inlay is 1.5 to 2 mm in diameter, and its thickness ranges from 10 µm at the periphery to 32 µm in the center. Its index of refraction is similar to that of the cornea, and its effect comes from reshaping the center of the cornea.8 The Raindrop has both the CE Mark and FDA approval.9
• The Flexivue Microlens (Presbia). This hydrophilic acrylic implant is 3.2 mm in diameter and 15 µm thick at its edges. Central thickness varies with power, which ranges from 1.50 to 3.50 D, and there is a central opening 0.51 mm in diameter. It is a refractive implant, with a mechanism of action similar to that of a multifocal IOL. The Flexivue has received the CE Mark in Europe, but it is not approved by the US FDA.10 This past year, Presbia purchased the assets of Neoptics, a company that was developing another refractive corneal implant, the Icolens.11
INTRODUCING THE CONCEPT
Despite a long history and extensive clinical experience, corneal inlays are not widely known among the general public. In our refractive surgical practice, few patients ask specifically for corneal inlays. Therefore, we usually take it upon ourselves to introduce the idea of a presbyopia-correcting inlay when we see patients who we think might benefit from this technology.
In a typical case, for example, a patient may come in expressing interest in a more familiar refractive surgical procedure, such as LASIK, for his or her myopia or hyperopia. (We generally do not see emmetropic presbyopes, who tend to manage well with reading glasses and do not think often of refractive surgery. Patients who seek refractive surgery usually have a fairly significant refractive error that binds them to their glasses or contact lenses all day long.)
When a patient seeking LASIK is in the presbyopic age range—40 years and above—we point out that LASIK will address only his or her distance vision, meaning that he or she will still have to wear reading glasses after surgery. At this point, we would initiate discussion of ways to remedy that situation, and a corneal inlay would be one of the options.
Clearly, when patients express interest in any type of refractive surgery, this suggests that they are interested in getting rid of their glasses. For presbyopes, then, our discussion with them begins with the question, “Are you interested in reducing your need for spectacles for all ranges of vision postoperatively?”
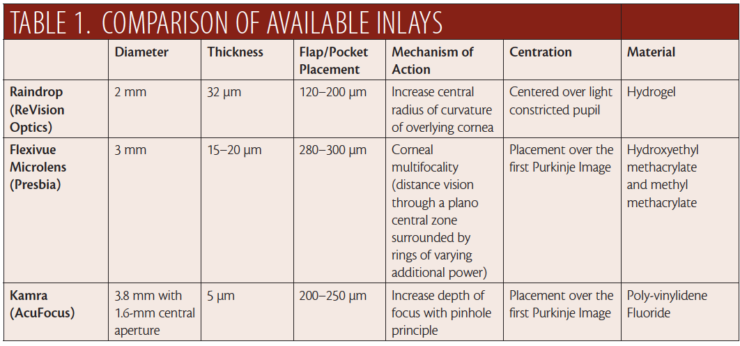
We always discuss all options for dealing with presbyopia, including bifocal and progressive spectacles in addition to surgical approaches. But, when patients answer that question positively, depending on their refractive error, we may present monovision laser refractive surgery and corneal inlays as options. Depending upon the patient’s age and level of refraction, we may also offer refractive lens exchange with either a multifocal or extended depth of focus lens. Because we are based in the United States, we note that the two types of inlays that are available to them are the Raindrop and the Kamra. Table 1 shows a comparison of these two inlays and the Flexivue Microlens, available now in Europe.
When a patient expresses interest in one of these corneal inlays, we proceed with our evaluation, making sure the eye and the patient are healthy, determining whether the patient qualifies for surgery, and assessing the patient’s refractive state. Doing this helps us to determine which inlay might be more appropriate.
Question No. 1: What is the difference between vision with An inlay and with monovision?
Drs. Moarefi and Bafna: Monovision is a strategy that is often employed to improve near vision for presbyopic patients such as yourself. Essentially, one eye is corrected for distance, one for near. Sometimes this causes problems for patients such as loss of stereo vision and depth perception. The inlay is different from monovision because you would not lose significant distance vision in the operated eye, which is your nondominant eye. You might lose 1 line of distance vision in that eye, but you would gain 5 or 6 lines of near vision, so it is not a one-to-one tradeoff. Plus you will still have good distance vision in your unoperated eye.
Google hit No. 1: Monovision LASIK and [corneal inlay surgery] are similar in the sense that one eye is treated for near vision while the other eye is used for distance. Both procedures treat the nondominant eye for near. As far as similarities go between the two, that is pretty much it. One advantage of the corneal inlay is that since the focusing power of the treated eye is not affected, the patient can continue to use both eyes for distance vision. This helps to preserve depth perception, which is important for activities like golf and tennis. Also, because both eyes work together for distance vision, patients often find the adjustment more tolerable than monovision. Some monovision patients find that having one eye focused on near and one eye focused on distance causes considerable discomfort and potential disorientation. (If you are considering monovision, it is best to test the condition with contact lenses first to see if you can tolerate the eyes being focused for different distances.) The advantage of monovision is that for most patients, it can create much better vision for near tasks than the [corneal] inlay. Also, there is a cost differential.1
1. http://www.bettervisionguide.com/monovision-lasik-versus-kamra-corneal-inlay/
Question No. 2: Will my eye look different or strange with the implant in place?
Drs. Moarefi and Bafna: The Raindrop is completely transparent, so it cannot be seen. The Kamra does have a pigmented ring, as you can see in the manufacturer’s picture (Figure 1). You might think that there would be a cosmetic concern, in that the ring would be visible to others. Strangely, though, it is almost impossible to tell that an eye has had an inlay and LASIK. Let me introduce you to our staff member who has a Kamra inlay. Can you tell which of her eyes the inlay is in (Figure 2)?
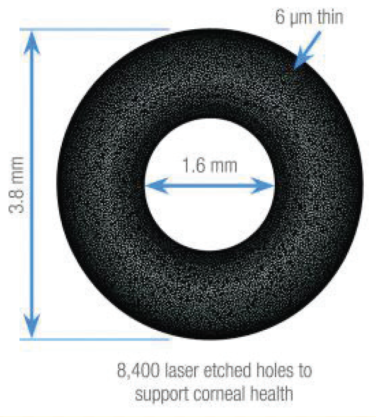
Figure 1. Specs of the Kamra inlay.

Figure 2. The Kamra inlay in situ.
Google hit No. 1: No, you cannot see it at all when you look at me. Patients do not notice it, and neither do my friends. Outside in the sun, if I am not wearing sunglasses, the pupil that has the inlay in it looks larger because it maintains that 3.8-mm size, whereas the other one is constricted, but the inlay itself is not visible. In a person with light-colored eyes, from an angle, it may be visible. We have never had a patient want the inlay removed for cosmetic reasons.1
1. http://crstoday.com/articles/2015-jun/personal-experience-with-a-corneal-inlay/
Question No. 3: Will my vision return as quickly after the inlay as it does after LASIK?
Drs. Moarefi and Bafna: You may have read on the internet or heard from friends that good vision returns almost immediately after LASIK—what people refer to as the wow effect. The inlay is different from LASIK. There is a gradual neural adaptation that takes place while your eyes learn to use the reading add. It is like a journey in which, as every week goes by, vision continues to progressively improve. As long as you realize that the change is not instantaneous, but gradually improves, you will probably adapt well to it.
Google hit No. 5: Most patients experience improvement within the first 24 to 48 hours. However, optimal results are usually achieved between 1 and 3 months postoperatively. Visual recovery depends on personal healing patterns and compliance with your doctor’s postoperative instructions (follow-up visits, medications).1
1. http://www.clearsight.com/kamra/common-kamra-inlay-faqs/
Question No. 4: Is the implant removable?
Drs. Moarefi and Bafna: In refractive surgery, we make a distinction between subtractive technologies and additive technologies. LASIK is a subtractive technology, meaning that we remove tissue from the cornea and we cannot put it back. An inlay is an additive technology. We put the inlay under a flap in your eye, and, if necessary, we can take it out. At that time, your vision should return to its preoperative level.
Google hit No. 4: The Kamra inlay has been proven to be the safe and effective solution for reducing the need for reading glasses. However, if for some reason you are unsatisfied with your vision after treatment, it can be removed and your vision restored to its pre-Kamra state.1
1. http://www.clearsight.com/kamra/common-kamra-inlay-faqs/
Question No. 5: What are the risks?
Drs. Moarefi and Bafna: The risks with an inlay procedure are very low, similar to those of LASIK because we must create the flap or stromal pocket in which we will place the inlay. As I mentioned previously (Question No. 4), if there is a problem with the inlay, we can take it out. In our practice right now, about 98% of patients who receive inlays are very happy with them. We have explanted inlays from less than 2% of patients, which is a very low number. Most patients are accepting of the vision change. And in the few patients who have undergone explanation, all of them have had their vision return to baseline levels.
Google hit No. 1: Side effects:
1. Halos, glare, and disturbances in night vision.
2. Loss of contrast sensitivity: This is also due to reduction in light entering the eye.
3. Difficulty in reading in dim light. The aperture design inlays reduce the amount of light entering the eye. This effect is more noticeable in dim lighting, making reading difficult.
4. Effect of pupil size. Pupil size may affect vision in case of refractive inlays. In small pupils, most of the pupillary area is occupied by the inlay, making distance vision difficult. Conversely, in larger pupils, only a small part of the pupillary area is covered by the inlay making near vision blurry.
5. Corneal haze. This may develop after implantation of the Raindrop inlay. It generally resolves spontaneously, or following a course of topical steroids.
Complications:
1. Lens decentration. This can occur in the early postoperative period due to inadequate flap adhesion. Decentration degrades the quality of vision and specially affects distance vision.
2. Dry eyes. This can occur due to damage to the corneal nerves during flap creation, as in the LASIK procedure.
3. Keratolysis, vascularization, and opacification. These complications were more common with older inlay designs which were thicker, less biocompatible, and had low water content. Anterior placement or nonporous implants affected the movement and diffusion of aqueous, oxygen, glucose, and other nutrients to the anterior portion of the cornea, resulting in necrosis and tissue breakdown. However, today these complications are rare with the thinner profile, small-diameter, higher permeability, and better biocompatibility of inlays.
4. Epithelial ingrowth. Epithelial cells may accidently get implanted in the interface and grow around the corneal implant. The ingrowth opacifies the interface and may cause blurry vision, photophobia, and star bursts.1
1. http://eyewiki.aao.org/Corneal_inlays#Side_effects
MAKING A RECOMMENDATION
We usually describe both corneal implants to the patient but make sure to offer a sound recommendation for one or the other. As Barry Schwartz pointed out in The Paradox of Choice,12 having too many choices makes things more complicated for patients—it can paralyze the patient and make moving forward with a decision more challenging. To avoid this, we try to listen to the patient, gauge his or her needs, and make a suggestion with the aim of meeting those needs.
If the patient is slightly hyperopic, we may recommend the Raindrop. Because the hyperprolate shape that the Raindrop produces may theoretically function better in someone with a potentially flatter cornea, the so-called sweet spot for the Raindrop is 0.50 D. For someone with a slight myopic refractive error, we lean toward the Kamra. The sweet spot for this inlay is -0.75 to -1.00 D. We have information on both inlays on our practice website, and we offer patients pamphlets from the manufacturers if they are interested in learning more about the devices. By far the greatest educational resource we have, however, is the six staff members in our practice who have had a Kamra inlay placed in their own eyes. When patients are interested in getting an inlay, we let them talk directly to someone who has had the procedure, so they get a first-hand description of what the experience was like. This personal touch is far more valuable to patients than any website or promotional material that we can provide.
With that said, however, undoubtedly when patients decide on pursuing surgery with a corneal inlay, they will have questions. In the accompanying sidebar, we answer the five most common questions we receive from patients regarding inlay surgery, followed by answers pulled from the first page of hits on a Google search.
1. Barraquer JI. Modification of refraction by means of intracorneal inclusions. Int Ophthalmol Clin. 1966;6(1):53-78.
2. Lane SL, Lindstrom RL, Cameron JD, et al. Polysulfone corneal lenses. J Cataract Refract Surg. 1986;12(1):50-60.
3. Knowles WF. Effect of intralamellar plastic membranes on corneal physiology. Am J Ophthalmol. 1961;51:1146-1156.
4. Dohlman CH, Refojo MF, Rose J. Synthetic polymers in corneal surgery. I. Glycerylmethacrylate. Arch Ophthalmol. 1967;77(2):252-257.
5. Werblin TP, Peiffer RL, Binder PS, McCarey BE, Patel AS. Eight years experience with Permalens intracorneal lenses in nonhuman primates. Refract Corneal Surg.1992;8(1):12-22.
6. McDonald MB, McCarey BE, Storie B, et al. Assessment of the long-term corneal response to hydrogel intrastromal lenses implanted in monkey eyes for up to five years. J Cataract Refract Surg. 1993;19(3):213-222.
7. FDA approves first-of-its-kind corneal implant to improve near vision in certain patients [press release]. US Food and Drug Administration. April 17, 2015. https://www.fda.gov/newsevents/newsroom/pressannouncements/ucm443471.htm. Accessed May 30, 2017.
8. Raindrop Near Vision Inlay Professional Use Information. Revision Optics. March 2017. http://www.revisionoptics.com/wp-content/uploads/sites/5/2016/09/710-0015-Rev-6-Artwork-FDA-Professional-Information-Brochure-US.pdf. Accessed May 30, 2017.
9. ReVision Optics receives FDA approval for the Raindrop Near Vision Inlay [press release]. ReVision Optics. June 29, 2016. http://www.revisionoptics.com/raindrop-near-vision-inlay-fda-approval/. Accessed May 30, 2017.
10. The Presbia Flexivue Microlens. Presbia. https://presbia.com/surgeons/. Accessed May 30, 2017.
11. Presbia acquires comprehensive patent portfolio for the Presbia Flexivue Microlens [press release]. Presbia. August 22, 2016. http://investors.presbia.com/releasedetail.cfm?ReleaseID=985078. Accessed May 30, 2017.
12. Schwartz B. The Paradox of Choice. New York: HarperCollins; 2004.



