
Keratoconus is one of the most common corneal dystrophies worldwide. The previously established prevalence of keratoconus, approximately 1 in 2,000 in the general population,1 has been challenged, and we now believe rates in many parts of the world to be much higher than this.2
This condition, characterized by corneal thinning and progressive ectasia (Figure 1), is not an overtly inflammatory disorder, although the levels of some inflammatory mediators are elevated in the tears of individuals with keratoconus.3 The most common etiologic feature is excessive eye rubbing due to irritation, occurring in about two-thirds of people with keratoconus.4
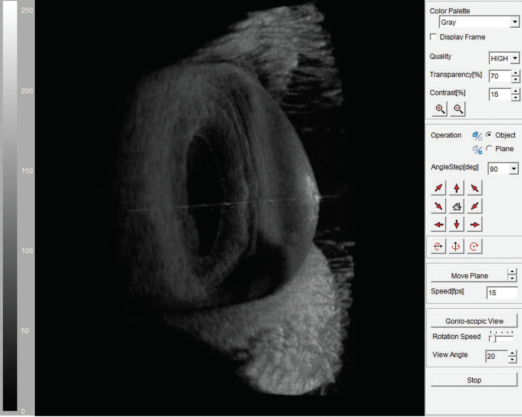
Figure 1. 3-D image of advanced keratoconus.
CXL is a technique in which UV-A light is combined with a photosensitizing chemical to strengthen the chemical bonds in the cornea with the aim of stopping progressive ectasia. Developed in the late 1990s, it was first used in humans in the early 2000s with promising results.5 It has since been refined, widely adopted, and commercialized. The most common indication for CXL is in the treatment of keratoconus, although it is also used often in individuals with iatrogenic corneal ectasia and other corneal dystrophies such as pellucid marginal degeneration.
Keratoconus is a disease of the young, with age of onset typically in the teen years,6 although the disease may be present for some time before becoming symptomatic. When a diagnosis is made, generally the patient knows nothing about the disease, so a thorough explanation is called for. Therefore, I always undertake a thorough discussion of keratoconus, its course, its implications for the patient, and the potential need for a treatment in the future, which may include CXL or, in advanced disease, a corneal transplant.
DESCRIBING KERATOCONUS AND CXL
With every new patient, I use a graphic presentation to explain what keratoconus is and how it progresses through stages. For these discussions, I have a Rendia (formerly Eyemaginations) video animation that shows the pathophysiology of the cone, including therapeutic options. I also have on hand the patient’s corneal topography maps. Using these tools, I explain what happens if we do CXL and what may happen if we do not do CXL.
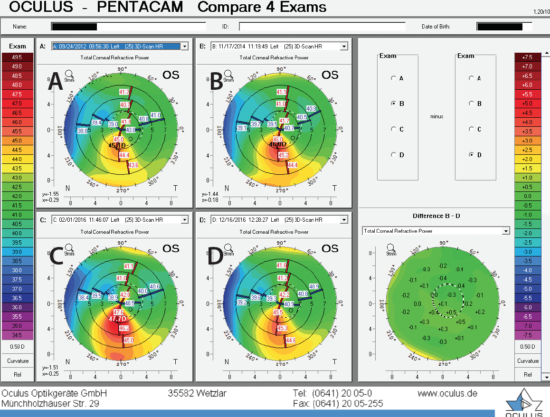
Figure 2. Disease progression: baseline (A), keratoconus worsening (B and C), and after epi-on iontophoresis CXL (D).
I may also use other patients’ topographical maps to illustrate these possibilities. When feasible, if a patient who already had CXL is present in the office, I try to arrange for him or her to meet with this new patient. This, of course, depends on the consent of both parties and their preferences regarding privacy.
After I have I described the stages of keratoconus, I then classify for the patient where he or she sits on this continuum. Then I detail what treatments are possible to do at this stage of the disease, and I discuss what the patient may want to do.
If the patient’s keratoconus is progressive, I explain that we can try to stop the progression with CXL. The ultimate goal of CXL is to avoid the need for a corneal transplant. In my practice, we do both epithelium-on (epi-on) CXL assisted by iontophoresis and epithelium-off (epi-off) CXL. Depending on which of these we do, the procedure can have a greater or smaller effect. Whether we choose epi-on or epi-off CXL depends on the state of progression of the cone and the risks for the patient. I prefer to use epi-on CXL for less cooperative patients, such as those with Down syndrome. It is also appropriate for patients who have difficulty managing contact lens wear. But, whichever technique we choose, I emphasize to patients that most people have an effect from CXL, and we can stop the progression of their keratoconus and avoid a transplant.
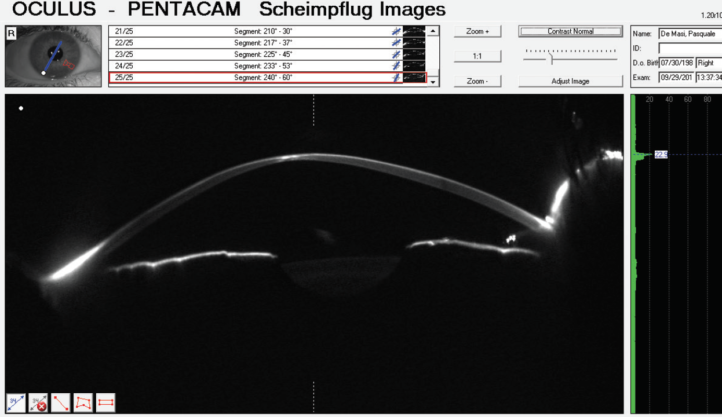
Figure 3. Scheimpflug image of an eye with advanced keratoconus with apical leucoma.
If the disease is relatively stable and the patient has a significant refractive error, I may lay out the possibilities for combining refractive correction with CXL. The options might include a bioptics procedure, with customized PRK (maximum 50-µm ablation to better regularize the cone), a phakic IOL, or perhaps intrastromal corneal ring segment (ICRS) implants. It depends on the state of the disease and varies from patient to patient. For patients older than 30 whose keratoconus is stable, CXL is not necessary, and additive refractive surgical procedures, such as IOL or ICRS implantation, can be done without combining them with CXL.
Bilateral CXL With A Mix-and-match approach
Sometimes, if a patient with bilateral keratoconus wants both eyes done on the same day, I suggest a mix-andmatch procedure, with epithelial-off (epi-off) CXL for the worse eye and epithelial-on (epi-on) CXL for the better eye. With this arrangement, the temporary blurring of vision in the worse eye is not so debilitating because vision is preserved in the better eye with the epi-on procedure. Therefore, patients can continue their work and other activities, and they do not have to come back again for a second CXL, also avoiding double follow-up visits. In my opinion, this is the best option when possible: The progressive keratoconus in the worse eye is halted with the standard epi-off procedure, and the eye with less progressive disease has the less-powerful procedure with no pain and less possibility of other problems in the healthier eye.
For informed consent, after explaining face-to-face all the risks and possible complications of the CXL procedure, I use the written forms prepared by our Italian ophthalmology society. The Italian Society of Ophthalmology (SOI) has produced forms for this purpose, and each is complete and explains all possible adverse outcomes, including opacifications and infections.
Question No. 1: Will I see better after CXL?
Dr. Gualdi: CXL itself is not a refractive procedure. Its goal is to stop the progression of the disease, not correct your vision. If you also want refractive correction, we can talk about your options and possibly incorporate a refractive treatment in conjunction with CXL. After initial worsening due to epithelium assestment, some patients experience a regression of the cone several months after CXL, so they can also see a little bit better. However, I cannot promise you that your vision will improve after CXL. Sometimes there is no improvement, and sometimes, in case of rare complications, vision gets worse instead of getting better.
Google hit No. 2: With the traditional CXL procedure, most patients find that immediately after the crosslinking treatment, their vision is actually worse than it was before the procedure. This usually goes on for roughly 3 to 6 weeks. Patients may start to notice positive effects 4 to 8 weeks after the procedure and may experience major improvement in vision at least 3 to 6 months after the investigational procedure. In some studies, patients’ vision and astigmatism were still continuing to improve 5 years after the crosslinking procedure so visual improvement is a long process. With the less invasive transepithelial CXL, some patients found their vision improved as early as several weeks after treatment.1
1. https://www.clevelandeyeclinic.com/cornea-ohio/corneal-cross-linking-cxl/
Question No. 2: Is CXL repeatable?
Dr. Gualdi: Yes, CXL treatment can be repeated. It is unusual to need CXL a second time because it is very effective. It might become more necessary if we do epithelial-on, or epi-on, CXL, as the effect of this procedure is less robust than the more conventional epithelial-off, or epi-off, CXL.
Google hit No. 2: In many studies, the vast majority of patients respond to a single CXL treatment and do not need to have the procedure repeated. For the occasional patient in whom this treatment is not successful, CXL can often be repeated.1
1. https://www.clearvieweyes.com/collagen-crosslinking/
Question No. 3: If I have CXL, can my eyes have other treatments?
Dr. Gualdi: The answer, in a word, is yes. But this is a complex issue, as the aim of CXL is to stop progression of ectasia, not to provide a refractive surgical correction. If your progression can be arrested, then you can have another treatment done on your eyes.
Google hit No. 7: It has no effect on any future surgery as far [as] has been determined until now.1
1. http://kcglobal.org/content/view/11/25/
Question No. 4: What type of CXL do you suggest for me?
Dr. Gualdi: The choice of epi-on or epi-off CXL depends on your age and the status of your disease. Normally when there is evidence of progression, I use routine epi-off CXL because it is the gold-standard of CXL, with the most evidence of efficacy. In some cases, especially with patients older than 26 years or with less chance of progression, I may suggest an iontophoresis-assisted epi-on treatment.
Google hit No. 2: Epi-off is the classic and proven technique, and it specifically is this technique that has been [US] FDA approved at this point in time. The purposes of removing the epithelial layer are to allow for easier and fuller absorption of riboflavin into the stromal collagen fibers and to remove a possible barrier to UV-A irradiation.1
1. http://www.newgradoptometry.com/everything-need-know-corneal-collagen-cross-linking-cxl/
Question No. 5: Can I have both eyes done on the same day?
Dr. Gualdi’s answer for bilateral epi-off: Both can be done the same day, but you must be prepared to experience more pain, and you will not be able to go to work for a period of time because vision can be blurry or foggy for some weeks after the procedure. However, this is highly dependent on your reaction to the procedure. Some patients are fully recovered after 2 weeks, but some take more time. Since you will be undergoing epi-off CXL, I would advise that it is best to have CXL in your worse eye first and then wait 1 or 2 months for stabilization of visual acuity before doing your other eye.
Dr. Gualdi’s answer for bilateral epi-on CXL: Both eyes can be done on the same day because there is no blurred vision or pain from epithelial debridement. You can return to work and normal activity the day after the procedure with no problem. In general, I suggest the bilateral procedure because it is more convenient for you, the postoperative therapy is more manageable for you, and it requires fewer postoperative follow-ups at the office.
Google hit No. 2: As someone who just had CXL performed last month, I would definitely recommend one eye at a time (I’m assuming your doctor suggested epi-off technique?). If you are getting epi-off, expect to be out of commission 3 to 5 days at least. Healing time is different for everyone and the amount of discomfort also varies. You will be sleeping a lot the first few days and having your good eye still intact will be crucial for your ability to function and return to work more quickly. Having both eyes done at once might sound more convenient, but I think you will wish you had only done your worst eye. The other thing is that you will need to take a lot of eyes drops for the weeks following your procedure (steroid, antibiotic, lubrication drops), so having both eyes done would only make this more of a hassle. This is just my opinion so other people might have different thoughts.1
1. http://www.kcfreedom.org/t60264920/one-eye-or-both-eyes/
CONCLUSION
Because CXL is a new concept for many with keratoconus, patients have many questions when they come to the office. It is important to take the time with every patient to thoroughly discuss keratoconus; its course; its implications; and its treatment options, which must be tailored to the patient based on age, type of progression (Figures 2 and 3), and lifestyle. In the accompanying sidebar, I share the top 5 questions that I hear from keratoconus patients and how I answer them. Then, for comparison, one of the responses found on the first page of a Google search of the same questions is presented.
1. Rabinowitz YS. Keratoconus. Surv Ophthalmol. 1998;42(4):297-319.
2. Gomes JAP, Tan D, Rapuano CJ, Belin MW, et al; Group of Panelists for the Global Delphi Panel of Keratoconus and Ectatic Diseases. Global consensus on keratoconus and ectatic diseases. Cornea. 2015;34:359-369.
3. Balasubramanian SA, Mohan S, Pye DC, Willcox MD. Proteases, proteolysis and inflammatory molecules in the tears of people with keratoconus. Acta Ophthalmol. 2012;90(4):e303-309.
4. Karseras AG, Ruben M. Aetiology of keratoconus. Br J Ophthalmol. 1976;60(7):522-525.
5. Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-A-induced collagen crosslinking for the treatment of keratoconus.Am J Ophthalmol. 2003;135(5):620-627.
6. Olivares Jiménez JL, Guerrero Jurado JC, Bermudez Rodriguez FJ, Serrano Laborda D. Keratoconus: age of onset and natural history. Optom Vis Sci. 1997;74(3):147-151.


