
In the past, to get the best performance out of a high-end supercar (Figure 1), you had to be an expert driver. Years of training went into developing the subtle skills of braking, clutching, steering, and accelerating. Over the past decade, however, technology to bring this performance to the average driver has been developed. Braking computers apply threshold and cadence braking. Electronic stability control applies different braking to each individual wheel to prevent skidding. Downshifting rev-matching technology adjusts engine speed to the selected gear, resulting in silky-smooth downshifts by novices. The result? A better driving experience for everyone, including the average driver.

Figure 1. Driving a supercar used to require years of training.
Image licensed from Adobe; Courtesy of Apfeweile
What would a high-performance patient-surgeon experience look like in LASIK? For starters, every patient would have an excellent outcome, defined as 20/20 or better UCVA. The quality of the patient’s 20/20 or 20/15 vision would be free of distortions and aberrations. Patients would have great day and nighttime vision. And they would be happy!
Happy patients love their vision and rave to their friends and family about their LASIK experience. This leads to happy surgeons in response to the smiling faces and the new referrals rolling in. Better yet, these surgeons are no longer stressed on surgery days because the planning of their surgery has become streamlined, efficient, predictable, and successful.
Sound like a dream? It has been until recently, when new technology made it a reality.
A LASIK SUPERCAR?
In November 2015, Alcon released Contoura Vision topography-guided LASIK into the US market. Using not simply the standard two keratometry (K) indices—steep K and flat K—Contoura brought more than 100,000 topographic data points to the excimer treatment of each eye. This was coupled with a fast eye tracker running at 1,050 Hz and synchronized to the laser frequency at 500 Hz, yielding a 2 msec latency time. The gaussian beam was ultrathin, with a 0.68-mm spot size.
This new LASIK supercar performed well in the study supporting FDA approval, with 92.6% of eyes achieving 20/20 UCVA or better and 64.8% experiencing 20/16 or better.1 Patients’ postoperative vision quality was also improved from preoperative vision with glasses and contacts, with statistically significant reductions in glare, light sensitivity, difficulty driving at night, and difficulty reading.1
When Contoura was released to the US market, however, it flopped. In the FDA study, no fewer than three cornea specialists evaluated every cornea and agreed that each one had perfect topography before it was allowed into the study. This was the equivalent of a professional race car driver piloting a supercar only on perfect roads under perfect conditions with no turns.
In the average clinic, however, life is real, and it is often messy. Most corneas (80% to 90%) are not perfect. Time is precious, and surgeons can’t spend hours on calculations for every single eye. The addition of topographic data led to greater complexity and difficulty determining the correct treatment. The WaveLight Allegretto Wave Eye-Q excimer laser (Alcon) may have had great power, speed, and potential, but it was wasted if the average surgeon driving it became frustrated trying to bring it all to bear.
A TECHNOLOGY ASSIST
What was needed was new technology to assist the surgeon driving that powerful topography-guided excimer laser. To meet this need, the Phorcides Analytic Engine (Phorcides) was developed. Phorcides uses geographic imaging software (GIS) to analyze the 2D corneal topographic treatment image produced by the Contoura planning laptop (Figure 2) and pull from it detailed information about the complex 3D cornea (Figure 3).
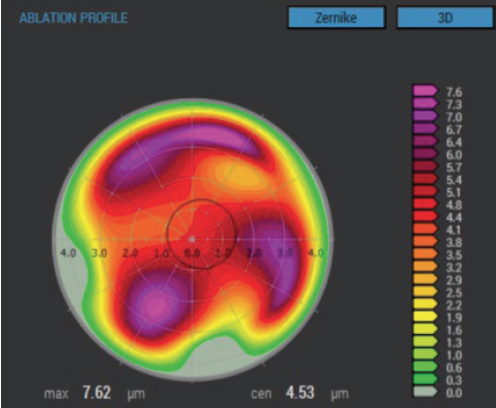
Figure 2. Topography-only corneal ablation profile from the Alcon planning laptop.
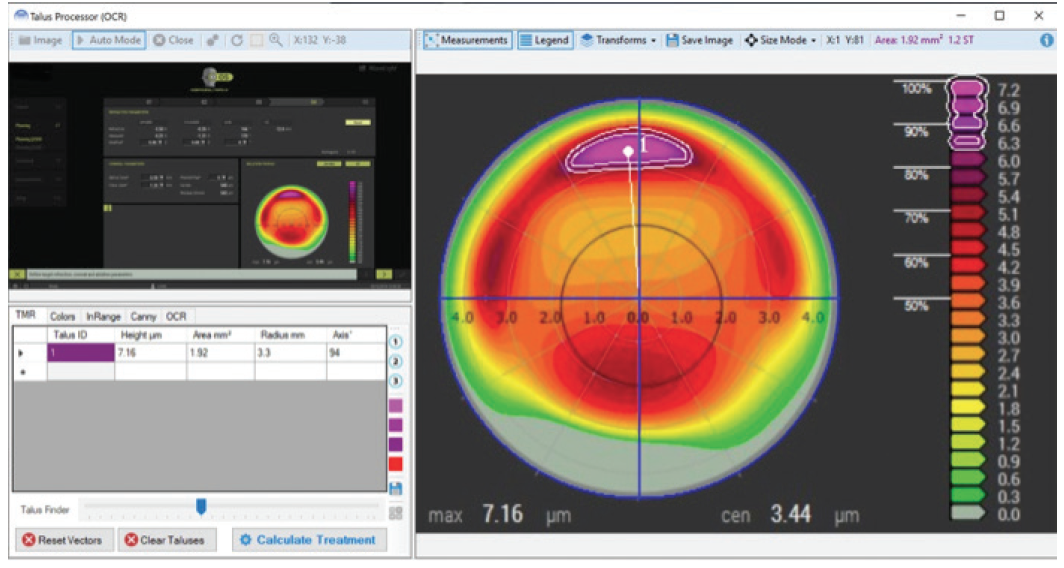
Figure 3. Phorcides GIS topography refractive analysis of an Alcon planning image.
The software then compiles a series of refractive vectors: one vector for each raised topographic feature on the corneal surface, one for the anterior corneal astigmatism, one for the posterior corneal astigmatism, and one for any internal lenticular astigmatism. Finally, it uses a series of advanced computer algorithms to determine the best treatment for each eye (Figure 4).
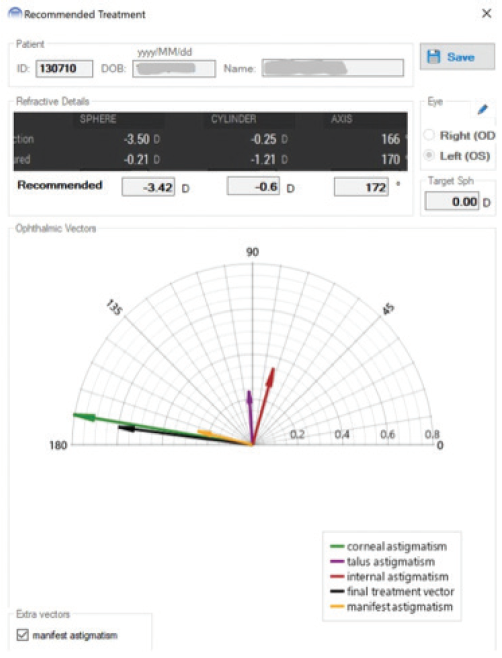
Figure 4. Phorcides vector analysis and treatment recommendation.
Although the analysis is complex, the surgeon experience is fast and seamless, with treatments calculated in less than 10 sec. What are the results? Exceptional patient experiences with beautiful vision. Figure 5 shows a comparison of Phorcides Contoura outcomes with other current refractive surgery techniques.1-5
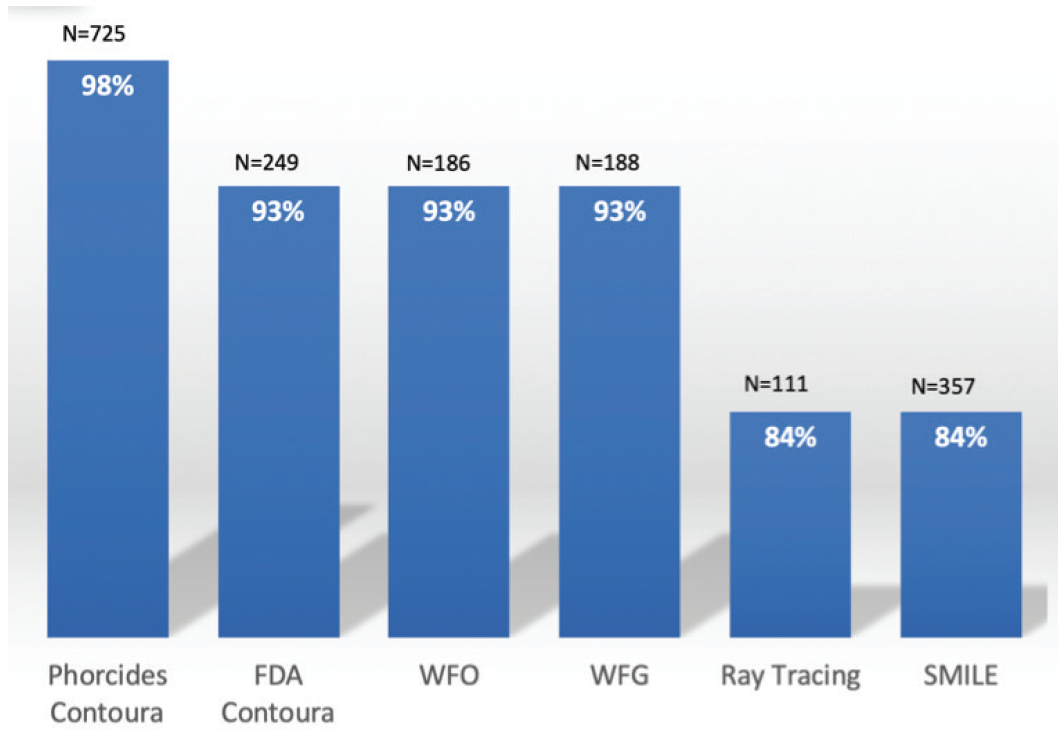
Figure 5. Eyes achieving UCVA of 20/20 or better with several refractive surgery platforms. Data for Phorcides Contoura,2 FDA trial for Contoura approval,1 wavefront-optimized (WFO) ablation,3 wavefront-guided (WFG) ablation,3 and ray tracing4 are from 3-month postoperative assessments. Data for SMILE5 are from 6-month postoperative assessments.
The data for the Phorcides Contoura group comes from a retrospective analysis of five US clinics including 725 eyes.2 At 3 months postoperative, 100% achieved 20/25 or better, 98.3% achieved 20/20 or better, and 60.1% achieved 20/15 or better UCVA. Of note, more than half of the eyes achieved 20/15 or better, which means we can move the new normal to beyond 20/20 in 2020.
One finding in the study is that the results in the Phorcides Contoura group were better than those in the FDA study, even though the FDA study restricted entry to only so-called perfect corneas and the Phorcides Contoura cohort included all clinic patients, even the 80% to 90% of eyes with mildly abnormal corneal topographies that caused the manifest astigmatism to differ from the measured anterior corneal astigmatism. Even more surprising, Phorcides Contoura delivered results superior to those of ray-tracing LASIK, a technology that has been forecast by some to supplant topography-guided LASIK in the future.4
QUALITY OF VISION
But great patient outcomes from LASIK go beyond just achieving 20/20 or 20/15 UCVA. Not all 20/20 vision is the same quality. Two patients can read the same 20/20 line on a Snellen chart, but they may not be seeing the same crisp outline of each letter. Figure 6 shows a Snellen chart as viewed by a patient with no aberrations (bottom left) and with a small amount of coma (bottom right). Contoura allows the correction of topographic irregularities on the corneal surface that generate higher-order aberrations such as coma. When these are eliminated, the result is a higher quality of vision.
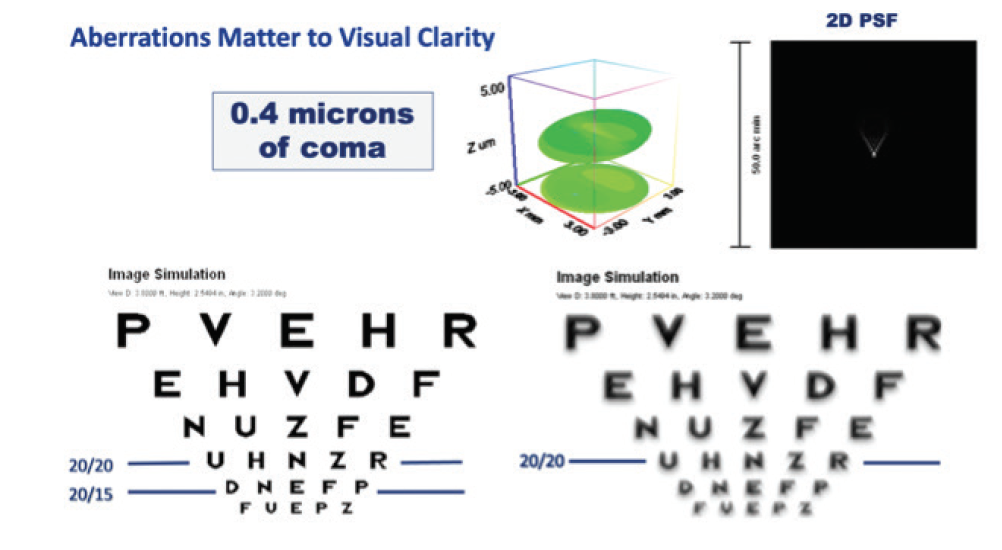
Figure 6. Image quality with no aberrations (bottom left) and with a small amount of coma (bottom right).
Used with permission from Alcon; Courtesy of Lisa Boggs
All of this translates into a better experience for the patient and the surgeon. When patients have excellent UCVA with high-quality resolution, they don’t need enhancements. At the 2019 ESCRS Annual Meeting, Karl G. Stonecipher, MD, shared that, among a population of 2,038 patients who underwent some form of laser vision correction at his clinic, not one treated with Phorcides Contoura required enhancement (Figure 7).6 Data from my clinic show similar results, with only one eye requiring an enhancement out of 1,466 Phorcides Contoura treatments.
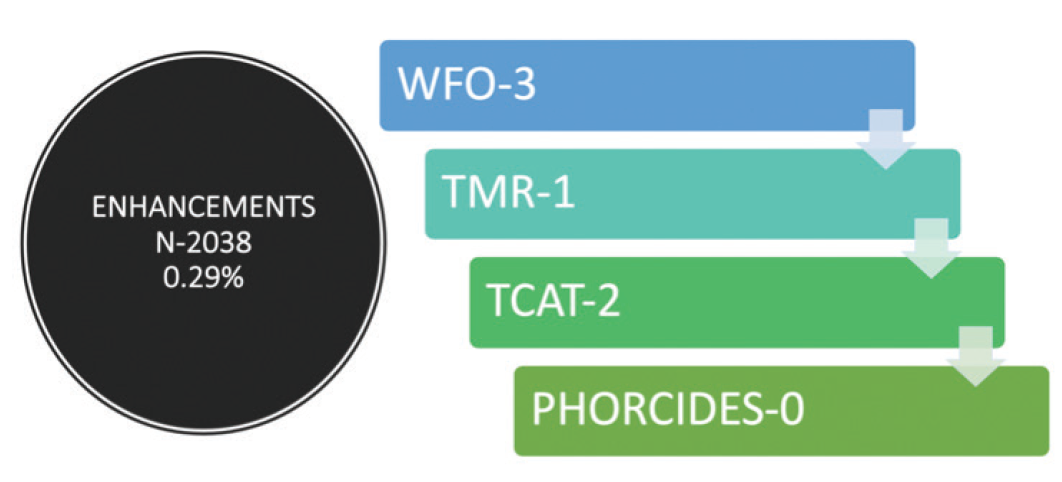
Figure 7. Enhancement data, courtesy Karl G. Stonecipher, MD.6 (Abbreviations: TCAT, topography-guided custom ablation treatment; TMR, topography modified refraction; WFO, wavefront-optimized)
FUTURE APPLICATIONS
AI can help us to better predict IOL spherical powers and toric choices for cataract surgery. Phorcides is currently developing patented software that can pull epithelial thickness maps into the GIS analytic engine and determine the refractive effects of removing epithelium of varying thicknesses. The hope is that this will lead to hyperaccurate PRK results.
It is my belief that much of the improvement in patient outcomes and surgeon satisfaction over the next few years will not come from new hardware. Rather, these gains will be made via software—AI and advanced computer analytics that make our current tools better. These smart software programs will never replace the surgeon, but they should make him or her better, augmenting existing abilities much like the high technology in supercars allows all drivers always to perform at their best.
1. US FDA. Allegretto Wave Eye-Q addendum procedure manual T-CAT topography-guided treatments. http://www.accessdata.fda.gov/cdrh_docs/pdf2/P020050S012d.pdf. Accessed December 5, 2019.
2. Lobanoff M, Mann M, Stonecipher K, Tooma T, Wexler S. Clinical outcomes after topography-guided LASIK calculated with new topography analysis algorithm: retrospective results from 5 US clinics. Clin Ophthalmol. In press.
3. Stonecipher K, Kezirian G. Wavefront-optimized versus wavefront-guided LASIK for myopic astigmatism with the Allegretto Wave: three-month results of a prospective FDA trial. J Refract Surg. 2008;24(4):S424-S430.
4. Schumacher S, Seiler T, Cummings A, Maus M, Mrochen M. Optical ray tracing-guided laser in situ keratomileusis for moderate to high myopic astigmatism. J Cataract Refract Surg. 2012;38(1):28-34.
5. Sekundo W, Kunert K, Blum M. Small incision corneal refractive surgery using the small incision lenticule extraction (SMILE) procedure for the correction of myopia and myopic astigmatism: results of a 6 month prospective study. Br J Ophthalmol. 2011;95(3):335-339.
6. Stonecipher K. Topography guided laser outcomes using a new vector software program (Phorcides). Paper presented at: the ESCRS Annual Meeting; September 14-18, 2019; Paris.


