CASE PRESENTATION
A 49-year-old man presents for a cataract surgery consultation. The patient reports decreased visual acuity in each eye. He received a Verisyse phakic IOL (Johnson & Johnson Vision) through a superior incision in each eye 15 years ago.
Upon examination, BCVA is 20/25 with a manifest refraction of -1.75 +0.50 x 005º OD, and glare testing reduces visual acuity to 20/100 OD. In the left eye, BCVA is 20/30 with a manifest refraction of -3.50 +0.75 x 175º, and glare testing reduces visual acuity to 20/200.
A slit-lamp examination reveals a clear cornea and a well-centered phakic IOL in each eye (Figure). The right eye has a 1+ nuclear sclerotic cataract and a 1+ posterior subcapsular cataract. The left eye exhibits mild anterior capsular changes and has a 1+ nuclear sclerotic cataract and a 3+ posterior subcapsular cataract. A dilated fundus examination shows mild myopic degeneration but no holes, breaks, or tears. The endothelial cell count is 2,400 cells/mm2 in the right eye and 2,000 cells/mm2 in the left. An OCT scan of the retina is normal in each eye.
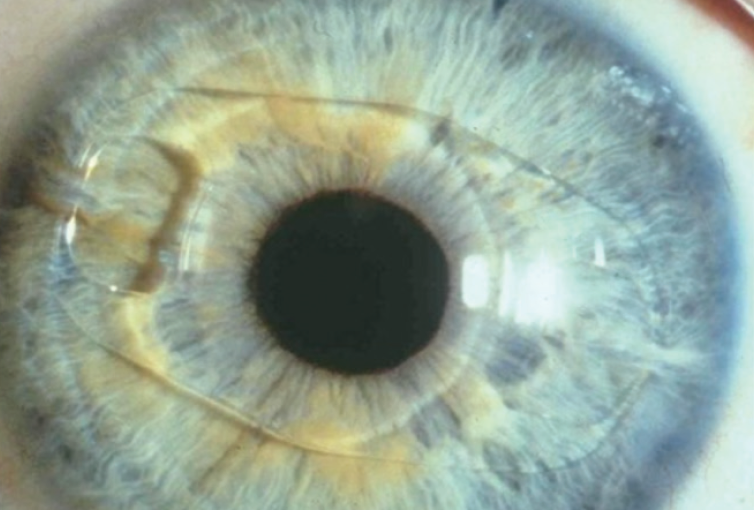
Figure. A Verisyse phakic IOL in situ in the left eye.
The patient is concerned about seeing glare at night. He expresses a desire for good midrange vision. He does not want monovision but would instead like the visual acuity in his left eye to be similar to that in his right.
How would you proceed? Would you offer laser cataract surgery? Where would you place the cataract incision, and which IOL would you offer to this patient? Are you concerned about the endothelial cell count?
—Case prepared by Audrey R. Talley Rostov, MD

RUPERT MENAPACE, MD, FEBO
Iris-fixated phakic IOLs are an effective and safe option for correcting myopia. Implantation of a nonfoldable PMMA Verisyse lens with a 5-mm optic requires a large incision that can induce significant astigmatism, particularly when the incision is created in clear cornea. I recommend against using a femtosecond laser for surgery in this case because the gas that accumulates between the IOL and the crystalline lens could cause a radial anterior capsular tear.
I would explant the phakic IOL through a superior frown incision and then perform cataract surgery using a temporal approach under topical and intracameral anesthesia. To begin the explantation, after asking the patient to look down, I would create a superior fornix-based conjunctival flap and a 4.5-mm scleral frown incision located as posteriorly as possible. Next, I would dissect a 5.5-mm sclerocorneal tunnel and create a 2.2-mm central corneal lip. After exchanging the aqueous for a cohesive OVD, I would use a pair of Artiflex implantation forceps (Ophtec) to grasp the haptic base and disenclavate the iris with a needle passed through paracenteses at the 10 and 2 clock positions. After enlargement of the corneal lip to 5.5 mm, the IOL would be rotated vertically and explanted while the endothelium was protected with a spatula.
Standard temporal-access 2.2-mm posterior-limbal cataract surgery would follow with a related use of a dispersive OVD during phacoemulsification.
The choice of replacement IOL depends on the quality of the patient’s preoperative corneal topography. Asymmetric bow tie astigmatism resulting from the implantation of a Verisyse lens through a superior corneal incision would decrease the optical performance of multifocal and extended depth of focus IOLs. The planned posteriorly positioned 5.5-mm frown incision would avoid inducing additional astigmatism during explantation of the phakic IOL. A toric trifocal lens could be considered. An excimer laser enhancement might be required to optimize the refractive result but should not be performed before 6 months have elapsed in case the cataract incision sags and induces a change in astigmatism.1

SIMONETTA MORSELLI, MD
I would counsel this patient on his low endothelial cell counts and his possible future need for an endothelial cell transplant. I would offer to perform cataract surgery and implant a monofocal IOL. When performing the IOL power calculation, I would target -2.00 D to obtain the same postoperative refraction as the right eye.
The pupil would not be dilated before surgery. After the conjunctiva had been opened from the 11 to the 2 clock position, a 4.5-mm scleral frown incision would be created at the 12 clock position, and a 2.2-mm temporal corneal sideport incision would be created. Under a cohesive OVD, the phakic IOL would be disenclavated with special forceps and a manipulator. After explantation of the IOL, the scleral incision would be closed with a 10-0 nylon suture, and the conjunctiva would be closed with an 8-0 polyglactin suture.
A mydriatic solution would be administered through the 2.2-mm temporal clear corneal incision created for disenclavation of the phakic IOL. Cataract surgery would be performed through this same incision under a cohesive OVD. I would perform phacoemulsification according to my usual technique and insert a monofocal IOL into the capsular bag. I would not suture the incision at the conclusion of surgery.

WHAT I DID: AUDREY R. TALLEY ROSTOV, MD
I decided to perform laser cataract surgery using the Lensar Laser System (Lensar) in an effort to minimize endothelial cell loss. The laser capsulotomy and phacofragmentation were executed without complication. I then created a 6-mm temporal incision, injected a dispersive OVD (Viscoat, Johnson & Johnson Vision), disenclavated the Verisyse lens with an enclavation needle, and explanted the IOL.
After hydrodelineation and hydrodissection of the fragmented cataract, the pieces were easily removed with irrigation as part of a modified technique of small-incision cataract surgery. Two sutures were placed in the temporal incision, and the cortex was removed with bimanual irrigation and aspiration using a low infusion pressure. A three-piece SofPort lens (LI61AO, Bausch + Lomb) was implanted; the targeted postoperative refraction was -1.50 D. The patient was pleased with the outcome.
1. Menapace R, Vass C, Hirsch U, Strenn K. A simple, safe and stable alternative to the frown incision for implantation of PMMA intraocular lenses with a large optic diameter. Spektrum Augenheilkd. 1996;10:237-240.
2. Galgauskas S, Norvydaite D, Krasauskaite D, Stech S, Stanislovas Ašoklis R. Age-related changes in corneal thickness and endothelial characteristics. Clin Interv Aging. 2013;8:1445-1450.
3. Moshirfar M, Imbornoni LM, Ostler EM, Valliammai M. Incidence rate and occurrence of visually significant cataract formation and corneal decompensation after implantation of Verisyse/Artisan phakic intraocular lens. Clin Ophthalmol. 2014;8:711-716.
4. Ohno-Matsui K, Kawasaki R, Jonas JB, et al; META-analysis for Pathologic Myopia (META-PM) Study Group. International photographic classification and grading system for myopic maculopathy. Am J Ophthalmol. 2015;159(5):877-883.e7.


