
The benefits of scleral contact lenses have been well established since descriptions of glass-blown shells appeared in the literature in the late 1800s.1 Scleral lenses are fit for therapeutic use, the improvement of vision, and the correction of refractive error.
The first successful fitting of scleral lenses made of PMMA was reported in 1939.2 Complications related to corneal hypoxia, including neovascularization and edema, however, limited the use of scleral lenses until the latter part of the 20th century.3,4 The development of materials with high oxygen permeability (Dk) renewed interest in scleral lenses. In 1983, Ezekiel first described the successful use of gas permeable scleral lenses, which significantly reduced complications from corneal hypoxia.5 Other pioneers reported the successful use of gas permeable scleral lenses for postoperative refractive correction and keratoconus.4,6-11 Since the 1990s, the indications for the use of scleral lenses have been improved and refined. This article describes modern uses of this therapeutic modality.
KNOW THE BASICS
How the lenses work. Scleral lenses provide a smooth anterior ocular surface and neutralize the irregularity of the ocular surface. They have a larger diameter than other contact lenses.
Scleral lenses do not rest on the cornea; they are supported by the conjunctival tissue overlying the sclera. In other words, a large diameter delivers the desired vision benefits without requiring the lens to sit on the cornea itself (Figures 1–3). Lenses that sit on the cornea are typically less comfortable than scleral lenses and are therefore problematic for patients with corneal irritation or irregularly shaped corneas. For eyes with highly irregular corneas, better lens centration and stability may be attained with scleral lenses than corneal lenses. A lack of contact between the scleral lens and the highly innervated cornea also generally decreases patient awareness of the lens on their eye, increases their comfort, and reduces their lens adaptation time.
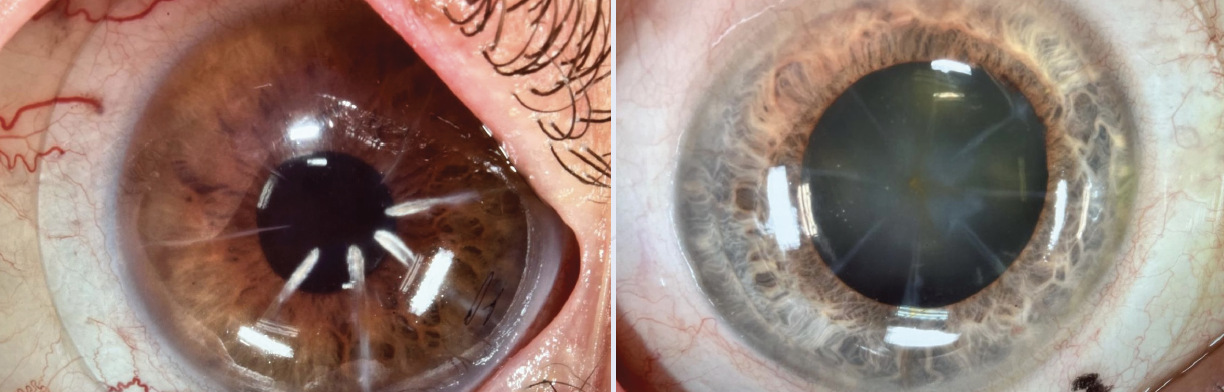
Figure 1. Scleral lenses over post–radial keratotomy eyes.
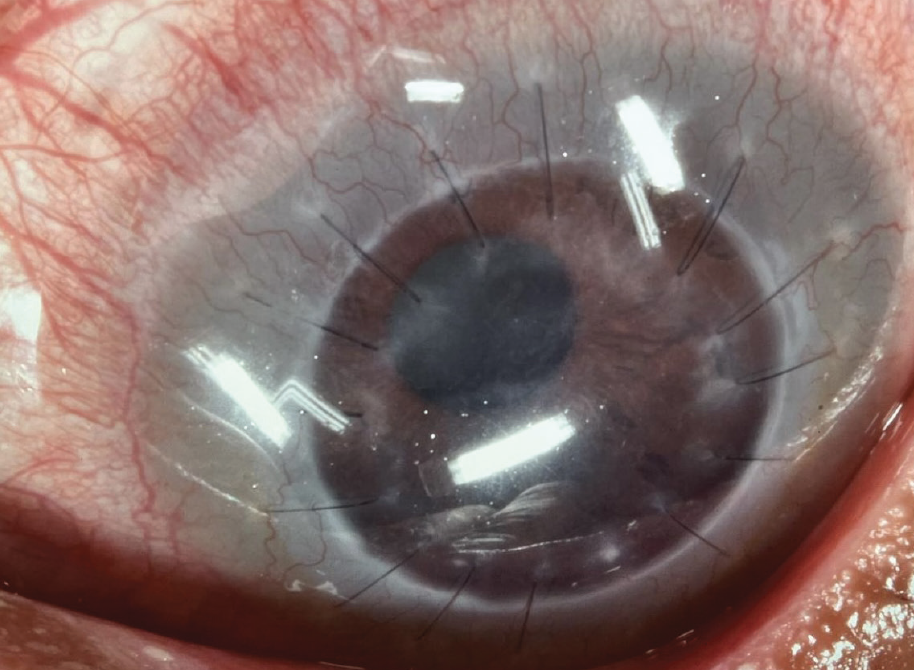
Figure 2. Scleral lens over a post-keratoplasty eye with interrupted sutures and a displaced pupil.
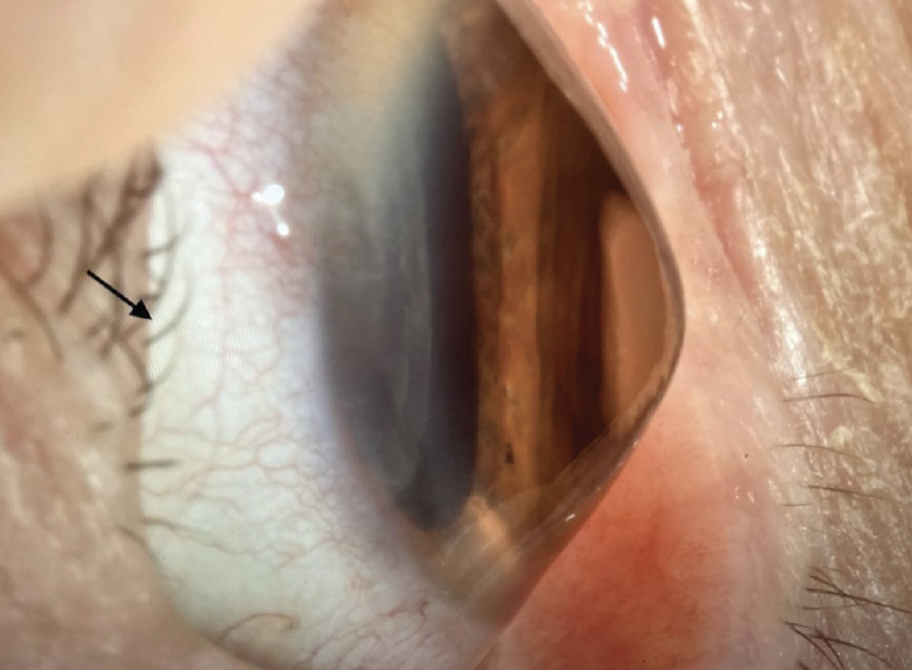
Figure 3. Side view of a scleral lens over an eye with advanced keratoconus.
Figures courtesy of Edward Boshnick, MD
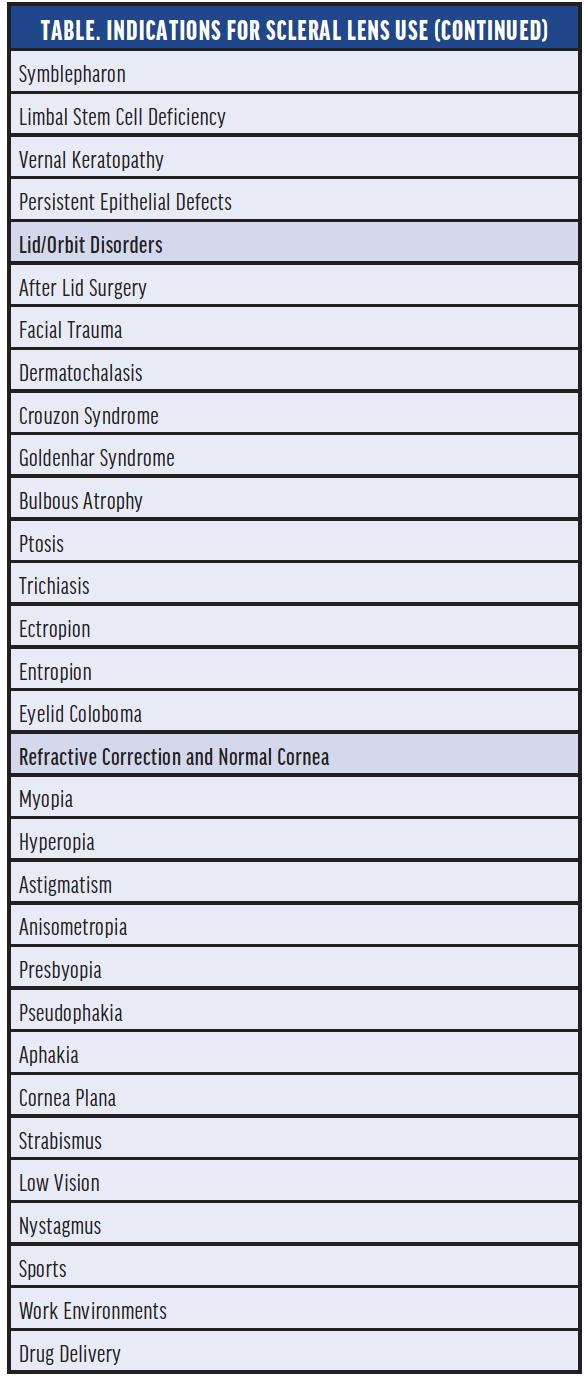
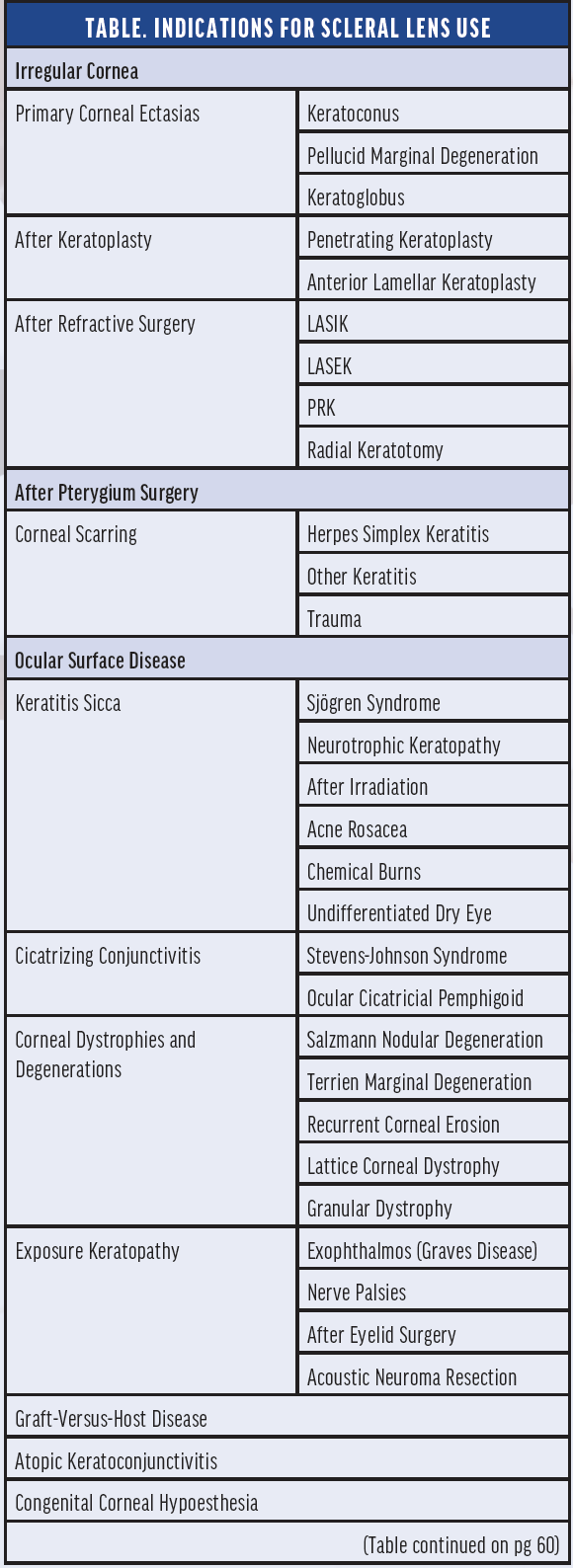
Indications. The main indication for scleral lenses is corneal irregularity.4,12 They can also help in managing ocular surface disease12-14 and are a good therapeutic option for lid or orbital disorders and refractive correction in otherwise normal, healthy eyes. The clinical indications for scleral lens wear are summarized in the Table.

Scleral lenses can enhance visual quality and comfort15,16 and thus quality of life.17,18 In a retrospective review, 18.7% of patients who underwent corneal transplantation between 1999 and 2003 achieved 20/20 or 20/25 VA with scleral lenses.15 According to DeLoss et al, even eyes with advanced keratoconus may benefit from scleral lenses, and visual outcomes were better and visual recovery was more rapid for patients with stage 4 ectasia who received scleral lenses versus keratoplasty.17 Koppen et al recently demonstrated the successful long-term treatment of severe keratoconus with scleral lenses in patients who otherwise would have needed corneal transplantation.19
Patients with poor vision due to an irregular corneal surface and irregular astigmatism can present a treatment challenge. Corneal gas permeable lenses may provide these individuals with excellent visual acuity. If lens centration, stability, or adaptation is insufficient, however, scleral lenses may be a better option.
CONCLUSION
Modern scleral lenses can eliminate blurred and distorted vision, promote healing of the ocular surface, and protect the cornea from the surrounding environment and the eyelids. Careful documentation and baseline measurements, photography, and other ocular assessments can help improve success with scleral lenses. Frequent follow-up visits are recommended. Lens designs may require fenestration, notches, localized vault, or impression techniques.
1. Müller F, Müller A. Das künstliche Auge. Bergmann; 1910.
2. Thier PFX. Contactglazen, vervaardigd van harsproducten. Ned Tijdschr Geneeskd. 1939;83:4161.
3. Dallos J. Sattler’s veil. Br J Opthalmol. 1946;30:607-613.
4. Tan DT, Pullum KW, Buckley RJ. Medical applications of scleral contact lenses: 1. A retrospective analysis of 343 cases. Cornea. 1995;14(2):121-129.
5. Ezekiel D. Gas permeable haptic lenses. J Br Contact Lens Assoc. 1983;6:158-161.
6. Visser R. Een nieuwe toekomst voor hoog-zuurstofdoorlatende scleralenzen bij verschillende pathologie. Visus. 1990;3:11-16.
7. Schein OD, Rosenthal P, Ducharme C. A gas-permeable scleral contact lens for visual rehabilitation. Am J Ophthalmol. 1990;109(3):318-322.
8. Rosenthal P, Cotter JM, Ducharme C. Gas permeable scleral contact lenses for irregular corneas. Contact Lens Association of Ophthalmologists. 1990;5:3.
9. Barr J, Rosenthal P. Scleral/haptic RGPs: the potential of these contact lenses for difficult cases is great. Contact Lens Spectrum. 1991;12:21-23.
10. Kok JH, Visser R. Treatment of ocular surface disorders and dry eyes with high gas-permeable scleral lenses. Cornea. 1992;11(6):518-522.
11. Rosenthal P, Cotter JM, Baum J. Treatment of persistent corneal epithelial defect with extended wear of a fluid-ventilated gas-permeable scleral contact lens. Am J Ophthalmol. 2000;130(1):33-41.
12. Rosenthal P, Croteau A. Fluid-ventilated, gas-permeable scleral contact lens is an effective option for managing severe ocular surface disease and many corneal disorders that would otherwise require penetrating keratoplasty. Eye Contact Lens. 2005;31(3):130-134.
13. Harthan J, Nau CB, Barr J, et al. Scleral lens prescription and management practices: The SCOPE Study. Eye Contact Lens. 2018;44(suppl 1):S228-S232.
14.Nau CB, Harthan J, Shorter E, et al. Demographic characteristics and prescribing patterns of scleral lens fitters: The SCOPE Study. Eye Contact Lens. 2018;44(suppl 1):S265-S272.
15. Pullum KW, Whiting MA, Buckley RJ. Scleral contact lenses. the expanding role. Cornea. 2005;24(3):269-277.
16. Montalt JC, Porcar E, España-Gregori E, Peris-Martínez C. Visual quality with corneo-scleral contact lenses for keratoconus management. Cont Lens Anterior Eye. 2018;41(4):351-356.
17. DeLoss KS, Fatteh NH, Hood CT. Prosthetic replacement of the ocular surface ecosystem (PROSE) scleral device compared to keratoplasty for the treatment of corneal ectasia. Am J Ophthalmol. 2014;158(5):974-982.
18.Picot C, Gauthier AS, Campolmi N, Delbosc B. Quality of life in patients wearing scleral lenses. Article in French. J Fr Ophtalmol. 2015;38(7):615-619.
19. Koppen C, Kreps EO, Anthonissen L, Van Hoey M, Dhubhghaill SN, Vermeulen L. Scleral lenses reduce the need for corneal transplants in severe keratoconus. Am J Ophthalmol. 2018;185:43-47.



