The fourth industrial revolution is inevitable. The construction of new systems in health care is being spurred by the growing popularity of telemedicine during the COVID-19 pandemic and an unprecedented increase in data collection and analysis. This article summarizes how we can use big data and standardized protocols to improve our results for the benefit of our patients.
AN INSEPARABLE RELATIONSHIP
The use of big data entails collecting various types of data from both inside and outside medical institutions, processing the data, and extracting meaningful values and incorporating them into strategic diagnostic decisions to achieve optimal results. Initially, big data were characterized by the three Vs—volume, variety, and velocity. Value creation through big data is becoming more important, and now the three Vs have expanded to five with the addition of veracity and value. The change recognizes that big data are an information resource that can be specified in terms of scale, variety, speed, accuracy, and value and that big data are meaningful only when value can be obtained through usage. Big data, if not used properly, can consume a lot of storage space unnecessarily. The analysis and use of big data with unstructured diversity are therefore often performed with AI. This creates an inseparable relationship between big data and AI.
In ophthalmology—particularly cataract and refractive surgery—a new type of protocol using big data and AI has been tested multiple times and is gradually becoming a part of the clinical setting. Two examples are the use of lifestyle information for multifocal IOL selection and pre- and postoperative clinical data for laser vision correction.
MULTIFOCAL IOLS
Surgeons can choose from various types of multifocal IOLs to maximize patient satisfaction. The most suitable IOL is selected by taking the patient’s characteristics (standardized data and nonstandardized data such as lifestyle) into account. Because we rely on subjective statements from patients, the results of surgery sometimes do not meet their expectations. This can occur because we were unaware of certain lifestyle information or because accurate information was not provided to us.
The Vivior Monitor (Vivior; Figure 1) can improve surgical results with big data and AI. The device is affixed to the patient’s glasses and collects nonstandardized lifestyle information such as their near and distance life habits and the corresponding changes in pupil size. By processing these data using an AI algorithm, the device can recommend the optimal multifocal IOL.
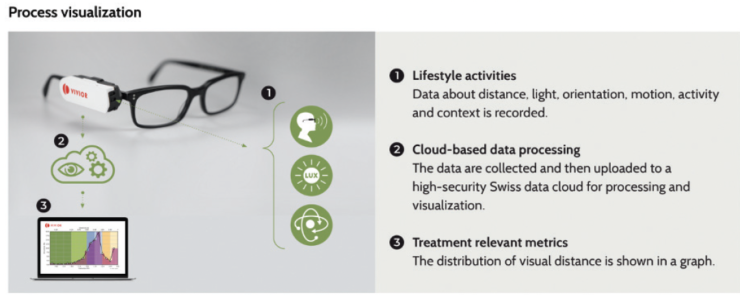
Figure 1. The concept of the Vivior Monitor technology.
Figure 1 courtesy of Vivior
The device provides an example of how big data and a standardized protocol can change the clinical setting, which has conventionally relied solely on patients’ subjective statements. This sort of change could drastically improve surgical outcomes and increase patient satisfaction.
LASER VISION CORRECTION
The Loocus-Vision program (Visuworks; Figure 2) recommends the most suitable form of laser vision correction for each eye based on pre- and postoperative clinical data from 18,480 eyes collected at a medical institution specializing in vision correction and nonstandardized data collected before surgery.1
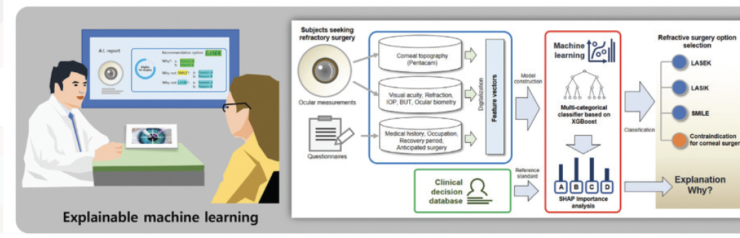
Figure 2. Architecture of the proposed machine learning models for corneal laser refractive surgery procedures.
Reprinted with permission from TK Yoo, IH Ryu, HN Choi, et al. Explainable machine learning approach as a tool to
understand factors used to select the refractive surgery technique on the expert level. Trans Vis Sci Tech. 2020;9(2):8.
The program provides a big data–based standardized protocol rather than a surgical method based on the preference of the patient or surgeon. Use of the Loocus-Vision program can reduce selection bias and improve patient satisfaction by providing objective indicators such as postoperative visual acuity.
CONCLUSION
The need for standardized protocols and big data in the clinical setting will grow. I believe that it is critical for us to prepare for the coming changes. A better clinical setting can be achieved by using existing patient data from electronic medical records and picture archiving communication systems.
Compliance with regulations on the use of big data, including disease information, and legal requirements must be maintained. The use of data for purposes other than originally intended and the unauthorized distribution or trading of data will adversely affect the transition to digital health care. An adherence to medical ethics can expand opportunities to use quality data and build the medical environment of the future.
1. Yoo TK, Ryu IH, Choi H, et al. Explainable machine learning approach as a tool to understand factors used to select the refractive surgery technique on the expert level. Transl Vis Sci Technol. 2020;9(2):8.



