
The most influential examination in modern laser refractive surgery measures manifest refraction and, astonishingly, is still performed in essentially the same manner as 30 years ago. A widely accepted review1 found minimal uncertainty with this method and showed that the typical uncertainty (±1 standard deviation [SD]) is about 0.30 D in refractive error measurement and about 0.04 in logMAR visual acuity. Aberrometric refraction has been proposed as an alternative to overcome some of the problems associated with manifest refraction, but its repeatability remains at the level of 0.25 D.2
My colleagues and I studied the repeatability and reproducibility of manifest refraction and corrected distance visual acuity (CDVA) in normal preoperative patients under standardized conditions when a systematic protocol was followed in our refractive surgery practice.
PATIENT POPULATION, EXAMINATIONS, AND STANDARD WORKFLOW
Patient population. We searched our electronic database and included 1,000 consecutive eyes with myopia or myopic astigmatism on which at least two manifest refractions had been performed during the preoperative period. Exclusion criteria for this study were medical conditions or medication that might affect the refractive power or visual acuity.
Examinations. The time interval between the two visits was at least 48 hours but not longer than 3 months. Each refraction was performed by one of four experienced optometrists.
Standard workflow. For adult patients seeking vision correction, our workflow includes at least two evaluations conducted on two different days. Soft and rigid contact lens wear must be discontinued at least 2 weeks and 4 weeks, respectively, before the initial examination. Great attention is paid to optimizing the ocular surface. The manifest refraction is performed at the initial visit and repeated, at minimum, at one separate visit before surgery to determine the final refraction to plan the treatment.
MANIFEST REFRACTION PROTOCOL
Standardized conditions. Our process of measuring refractive error and visual acuity is based on a standardized protocol I devised specifying the International Organization of Standardization recommendations3 for our setting.
The same room (lane) was used for performing the preoperative manifest refraction with a constant distance of 6 m from the phoropter (Visutron, Möller-Wedel Optical) to the optotype screen and constant lighting conditions with no natural daylight. Randomly generated normed optotypes (Landolt rings, no numbers) with a constant contrast level were presented on a computer screen (MultiVisus, bon Optic). A cross-cylinder method was used. The process concluded with fine-tuning the cylinder magnitude and axis by displaying a sun dial on the screen to check for homogeneous vision (Figure).
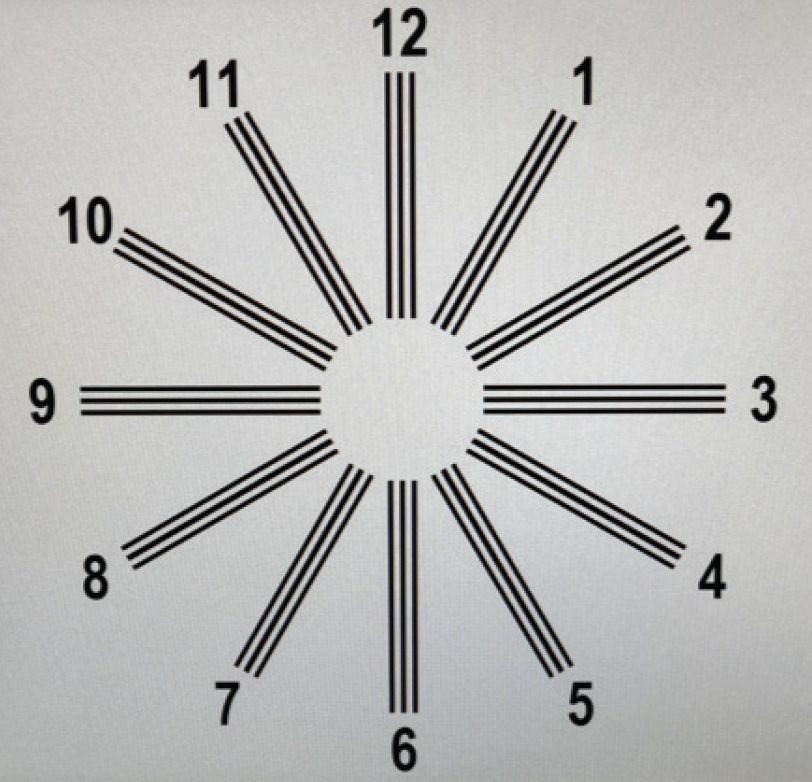
Figure. Fine-tuning of cylinder magnitude and axis by displaying a sun dial to check for homogeneous vision.
First evaluation. Manifest refraction and CDVA were assessed by protocol, starting with spectacles.
Second evaluation. On a different day, a second manifest refraction starting by first refraction, CDVA, a cycloplegic autorefraction with the use of tropicamide, a cycloplegic refraction, and cycloplegic CDVA were assessed. All details from the first evaluation and the wavefront refraction were considered at this evaluation.
Third evaluation. If a significant discrepancy was found either between the first and second manifest refractions or the manifest refraction and another examination, then a third evaluation was performed. This evaluation included at least manifest refraction and CDVA. If the discrepancy was not resolved, further evaluations could be scheduled to allow more time for optimizing the ocular surface. Only the most recent two refractions after stabilization were evaluated for this study, however.
RESULTS
The most recent 1,000 consecutive eyes of 510 patients fulfilling the inclusion criteria were included in the analyses.
Overall results. The mean difference in absolute value of the entire cohort was 0.15 ±0.19 D for sphere, 0.12 ±0.18 D for cylinder, 0.05 ±0.25 D for spherical equivalent, 0.05 ±0.06 logMAR for CDVA, and 5.1º ±9.8º for astigmatic axis. Of note, 0.25 D is the typical step used for manifest refraction, and 15º malposition of the cylinder axis results in 50% residual cylinder magnitude.
The difference in absolute value increased statistically but not clinically significantly with the measured magnitude for sphere, cylinder, and spherical equivalent. The 95% limit of agreement (LOA) remained within 0.50 D for sphere, cylinder, and spherical equivalent and within 22º for astigmatism axis. Interestingly, the difference in axis decreased significantly with the measured cylinder magnitude. We assume that the greater influence on visual quality of an axis change with higher astigmatism values may be the main reason for a more reliable measurement. The difference in CDVA significantly increased with worse measured CDVA values, and the 95% LOA remained within 1.5 Snellen lines.
Of note, one amblyopic eye showed deviations that were clearly out of the normal distribution (a difference of 1.75 D in sphere and cylinder magnitude). This may be explained by more intense pushing of the cylinder at the second refraction after the wavefront refraction had revealed high cylinder.
Comparison of same versus different optometrists. The comparative analyses of measurements by the same versus two different optometrists revealed a statistically significant but not clinically meaningful difference in CDVA. Spherical equivalent and cylinder magnitude measurements did not differ between groups.
DISCUSSION
Despite substantial advances in the objective evaluation of the individual eye and its refractive error, subjective manifest refraction is still the most influential parameter in every refractive treatment performed today except for refractive lens exchange.4,5
Great attention must be given to optimizing the ocular surface before obtaining the manifest refraction that may be used for planning a refractive treatment. A poor ocular surface can compromise the entire evaluation.6-9 Only the latest two refraction measurements with an acceptable ocular surface were therefore evaluated in this study. (If more than the latest two refractions had been evaluated, the differences had been greater; data not shown.)
Measuring the refraction remains challenging even under optimized conditions because the refractive error fluctuates. Factors affecting refractive status include accommodation, stress level, fatigue, ambient illumination conditions, and long-term drifts.10-12 For our study, as many parameters as possible were kept constant, and a large sample size was used.
Overall, our findings are comparable to or slightly better than previously reported values, which may be attributable in part to our patient selection process and the additional information from objective examinations in our setting.13-17
The retrospective nature of this chart review better represents the real values in our setting (a refractive surgery clinic) than a prospective study could. The former avoids a significant potential bias, namely that examiners would be consciously participating in a study.
It may be interpreted as a major limitation that the two separate refractions were not truly independent and that, in cases of large disparities, a third refraction measurement was scheduled. The aim of this study, however, was to evaluate the refraction in refractive surgery patients under real-world conditions, which include a standardized approach under constant conditions that naturally reduce the variability of the measurements compared to truly unbiased independent refractions. Care therefore must be taken not to generalize our results to less-controlled settings.
Limitations of our study include that the time interval between the two manifest refractions was not identical for all patients and that not all examinations were performed at the same time of day. Because the actual manifest refraction fluctuates within a small diurnal range and may drift over time, some pseudo-errors might have been introduced.
CONCLUSION
In our study, the SD of refraction was better than 0.25 D—the minimum measurement increment of refraction itself—and the 95% LOA was within 0.50 D for sphere, cylinder, and spherical equivalent. The SD of the astigmatism axis was approximately 10º, and the 95% LOA was within 22º. The difference in axis decreased significantly with the measured cylinder magnitude. The SD for CDVA was 0.5 Snellen lines, and the 95% LOA was within 1.5 lines. There was increasing deviation with worse vision.
Our results suggest that, when using a guided standardized protocol in a controlled environment, the repeatability and reproducibility of manifest refraction in a select group of eyes of refractive surgery patients are better than the typical step used for manifest refraction (0.25 D). There were no clinically relevant differences in manifest refraction when the results obtained by the same optometrist versus two optometrists were used, which may be interpreted as a benefit of standardizing the process of refraction measurement.
Obtaining multiple refractions preoperatively may increase the predictability of refractive surgery and thus decrease the enhancement rate.
1. Smith G. Refraction and visual acuity measurements: what are their measurement uncertainties? Clin Exp Optom. 2006;89(2):66-72.
2. Piñero DP, López-Navarro A, Cabezos I, de Fez D, Caballero MT, Camps VJ. Intrasession repeatability of refractive and ocular aberrometric measurements obtained using a multidiagnostic device in healthy eyes. Clin Optom (Auckl). 2017;9:91-96.
3. ISO 13666:2019(en), Ophthalmic optics —spectacle lenses — vocabulary. ISO online browsing platform. Accessed March 31, 2020. https://www.iso.org/obp/ui/#iso:std:iso:13666:ed-3:v1:en
4. Perches S, Collados MV, Ares J. Repeatability and reproducibility of virtual subjective refraction. Optom Vis Sci. 2016;93(10):1243-1253.
5. Taneri S, Arba-Mosquera, Rost A, Kießler S, Dick HB. Repeatability of manifest refraction. J Cataract Refract Surg. 2020;46(12):1659-1666.
6. Montés-Micó R, Cerviño A, Ferrer-Blasco T, García-Lázaro S, Ortí-Navarro S. Optical quality after instillation of eyedrops in dry-eye syndrome. J Cataract Refract Surg. 2010;36(6):935-940.
7. Montés-Micó R, Cáliz A, Alió JL. Wavefront analysis of higher order aberrations in dry eye patients. J Refract Surg. 2004;20(3):243-247.
8. Epitropoulos AT, Matossian C, Berdy GJ, Malhotra RP, Potvin R. Effect of tear osmolarity on repeatability of keratometry for cataract surgery planning. J Cataract Refract Surg. 2015;41(8):1672-1677.
9. Çakır B, Doğan E, Çelik E, Babashli T, Uçak T, Alagöz G. Effects of artificial tear treatment on corneal epithelial thickness and corneal topography findings in dry eye patients. J Fr Ophtalmol. 2018;41(5):407-411.
10. Chen A-H, Ahmad A, Kearney S, Strang N. The influence of age, refractive error, visual demand and lighting conditions on accommodative ability in Malay children and adults. Graefes Arch Clin Exp Ophthalmol. 2019;257(9):1997-2004.
11. Taneri S, Oehler S, Azar DT. Influence of mydriatic eye drops on wavefront sensing with the Zywave aberrometer. J Refract Surg. 2011;27(9):678-685.
12. Michael R, Pareja-Aricò L, Rauscher FG, Barraquer RI. Cortical cataract and refractive error. Ophthalmic Res. 2019;62(3):157-165.
13. MacKenzie GE. Reproducibility of sphero-cylindrical prescriptions. Ophthalmic Physiol Opt. 2008;28(2):143-150.
14. Rosenfield M, Chiu NN. Repeatability of subjective and objective refraction. Optom Vis Sci. 1995;72(8):577-579.
15. Raasch TW, Schechtman KB, Davis LJ, Zadnik K; CLEK Study Group. Collaborative Longitudinal Evaluation of Keratoconus Study. Repeatability of subjective refraction in myopic and keratoconic subjects: results of vector analysis. Ophthalmic Physiol Opt. 2001;21(5):376-383.
16. Shah R, Edgar DF, Rabbetts R, Harle DE, Evans BJW. Standardized patient methodology to assess refractive error reproducibility. Optom Vis Sci. 2009;86(5):517-528.
17. Reinstein DZ, Yap TE, Carp GI, Archer TJ, Gobbe M; London Vision Clinic optometric group. Reproducibility of manifest refraction between surgeons and optometrists in a clinical refractive surgery practice. J Cataract Refract Surg. 2014;40:450-459.



