Spectacles, contact lenses, CXL, intrastromal corneal ring segments (ICRSs), intrastromal corneal continuous rings (ICCRs), and PKP are all treatment options for corneal ectasia.1-3 Although the most popular treatment in severe cases is PKP, this eye-penetrating procedure has potentially serious complications such as infection, epithelial ingrowth, endothelial deterioration, graft rejection, induced astigmatism, and suture complications.2
WATCH IT NOW: MYORING INSERTION
A corneal pocket is created at a depth of 250 to 300 μm and the device is implanted to treat high myopia, advanced keratoconus, and post-LASIK ectasia in certain cases.
ICRSs VERSUS ICCRs
Implantation of ICRSs in the mid periphery of the cornea can reshape the cornea to a more regular (flatter) surface,4,5 and this approach is used as a substitute for keratoplasty in some cases. These segmented devices are available in multiple styles from several manufacturers, and they have long track records of reported safety and efficacy. One advantage of the ICRS treatment modality is reversibility with explantation.5-7
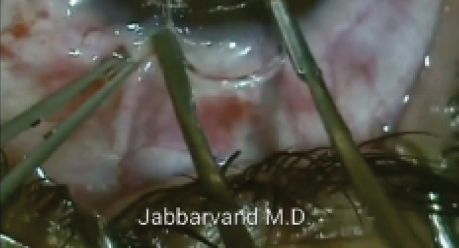
More recently, an ICCR (MyoRing; Dioptex) inserted into a corneal pocket (Figure 1) has been introduced for the treatment of high myopia, advanced keratoconus,4,8-11 and, in certain cases, post-LASIK ectasia. The pocket can be created at a depth of 250 to 300 µm with a specifically designed microkeratome (PocketMaker Ultrakeratome; Dioptex)9 or a femtosecond laser.10
The MyoRing has convex anterior and concave posterior surfaces with a radius of curvature of 8 mm. The material is flexible enough to accommodate implantation through a 4.5-mm wide tunnel, yet sufficiently rigid to stabilize the corneal shape after implantation. A limiting factor is pupil size; the pupillary opening must be smaller than the inner diameter of the ICCR.
In our experience, myopia reduction and corneal flattening are significantly greater after MyoRing implantation than after implantation of ICRSs. The flattening effect with ICRSs has been reported to be directly correlated with the thickness of the implant, but the ICCR has more of an arc-shortening effect.4 Our group has reported the correction of residual myopia after Intacs (Addition Technology) implantation by implantation of the MyoRing between the two Intacs segments.12

Figure 1. Slit-lamp photograph of the MyoRing implanted in a corneal pocket.
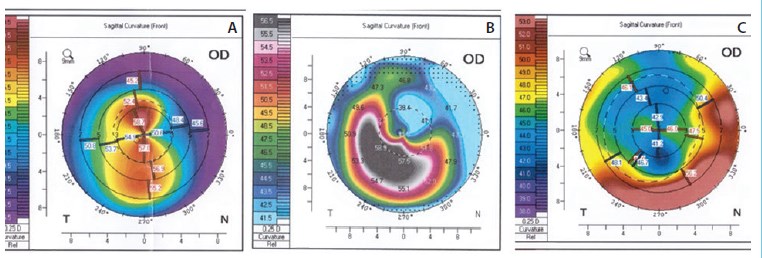
Figure 2. Topographic map of a patient with corneal ectasia before (A) and after (B) MyoRing implantation. The topographic map after adjustment of MyoRing position 0.5 mm downward (C). In A, refraction is -5.00 -6.00 X 12° (distance BCVA: 4/10); in B, refraction is +1.00 -7.00 X 12° (distance BCVA: 4/10); in C, refraction is +1.00 -3.00 X 90° (BCVA: 7/10).
SURGICAL PROCEDURE
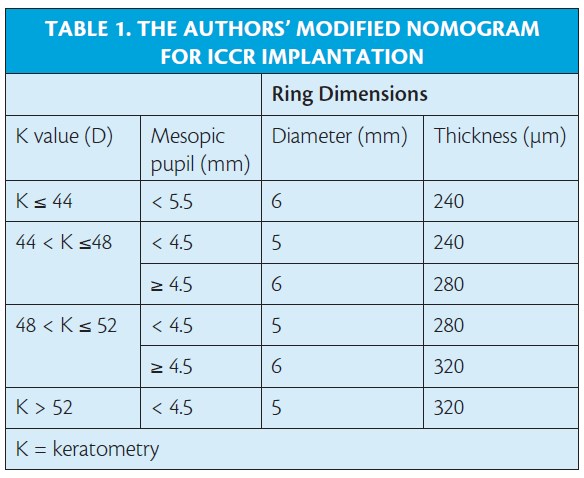
According to the factory nomogram, CXL is an optional pretreatment when the patient’s mean keratometry is greater than 50.00 D and is recommended when the number is higher than 55.00 D. We used an adapted nomogram to calculate MyoRing size (Table 1) and performed CXL only if the disease progressed after ICCR implantation.
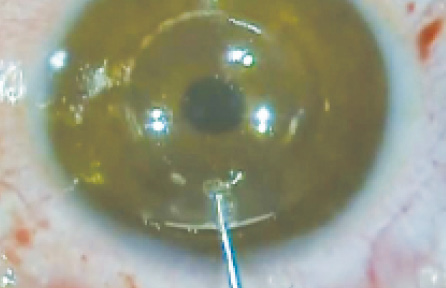
The stromal pocket is created with a femtosecond laser (Victus; Bausch + Lomb Technolas) using 1.05 μJ of energy, a spot size of 5 μm, and spot and line spacing of 3 and 5 μm, respectively. The pupil center is marked with a Sinskey hook before applanation, and this mark is used as a reference point to position the incision and to center the MyoRing after implantation. The laser makes a temporal corneal incision (70º arc length), followed by a 9-mm intrastromal pocket at a depth of 300 µm. The MyoRing is then inserted into the pocket and centered. A bandage contact lens is applied, and topical chloramphenicol is administered every 6 hours for 1 week and topical lubricant and betamethasone for 1 month (eyetube.net/?v=itelo).
EXPLANTATION AND ADJUSTMENTS
If the postoperative result is unsatisfactory, a spatula and reverse Sinskey hook can be used to reopen the tunnel and explant the MyoRing. The pocket closes rapidly, and a bandage contact lens is applied for 24 hours. If explantation is required after a long period (about 2 months or more), a clinically insignificant demarcation line as a result of debris and scarring may be seen at the position of the implant after its removal. Irrigating the pocket after implantation and explantation may reduce debris collection in the pocket.12
Placing the implant in a pocket allows adjustment of the ring position according to postoperative results.13 To reposition the ring, the pocket should be reopened and the ring should be shifted 0.5 mm toward the apex with the reverse Sinskey hook. This distance is equal to the width of the MyoRing (500 µm). Because the tangential keratometric map represents local curvature accurately, sharp power transitions are more easily recognized, and this map is more appropriately used to judge ring position than an axial map (Figure 2). Repositioning may be repeated as long as needed to achieve the desired refractive result (see When to Reposition the MyoRing).
WHEN TO REPOSITION THE MYORING
• UCVA < 20/40
• To push the cone further toward the center
• If the patient is dissatisfied with his or her present
We also have begun implanting the MyoRing in eyes with post-LASIK ectasia (see Five Characteristics of Post-LASIK Ectasia), and we have seen improvements in both distance UCVA and BCVA in patients postoperatively;1 the same favorable results have been shown in previous studies of MyoRing implantation in keratoconus.9-11 Primary coma, higher-order aberrations, and trefoil also reduced after the procedure, and primary spherical aberration is significantly increased.
FIVE CHARACTERISTICS OF POST-LASIK ECTASIA
Post-LASIK ectasia is characterized by the presence of all of the following:
1. Progressive corneal steepening and myopia
2. Loss of distance BCVA
3. Inferior-superior asymmetry index more than 1.2 on corneal topography
4. Highest elevation value more than 0.042 and 0.071 mm for anterior and posterior best fit spheres, respectively, on elevation map
5. Progressive corneal thinning
OTHER CONSIDERATIONS
Corneal parameters. A recent report3 found no statistically significant difference in corneal parameters between implantation depths of 250 and 300 µm. This finding is especially valuable in eyes with thin corneas, as the surgeon must keep the laser treatment a safe distance from the endothelium in order to avoid presumed harmful effects.
Femtosecond-assisted approach. Intraoperative complications including posterior corneal perforation have been reported after manual dissection of the tunnel for ICRS implantation.14 By contrast, previous studies with femtosecond laser channel creation for Intacs ICRSs have demonstrated rapidity, precision, safety, minimal induced stromal edema, good centration of the pocket, and easier channel creation.5
Haze. Most eyes develop mild haze around the ICRS or ICCR, especially in the first 3 months; however, in our experience this did not affect the visual axis. Subconjunctival hemorrhage also may develop in some eyes, probably due to the suction applied during docking of the femtosecond laser. It dissolves spontaneously and completely in less than 1 week.
CONCLUSION
MyoRing implantation is a reliable option to reduce myopia and regularize the corneal surface in patients with keratoconus and post-LASIK ectasia and can be considered an acceptable method to achieve corneal remodeling.
Corneal rings with larger diameters or eyes with smaller pupils should be selected for surgery when a minimal change in corneal asphericity is desired.
- Jabbarvand M, Hashemian M, Hashemian H, et al. Femtosecond laser-assisted MyoRing implantation in postoperative LASIK ectasia. J Refract Surg. 2014;30(7):462-466.
- Tan BU, Purcell TL, Torres LF, et al. New surgical approaches to the management of keratoconus and post-LASIK ectasia. Trans Am Ophthalmol Soc. 2006;104:212-220.
- Jabbarvand M, Hashemi H, Mohammadpour M, et al. Implantation of a complete intrastromal corneal ring at 2 different stromal depths in keratoconus. Cornea. 2014;33(2):141-144.
- Alio JL, Pinero DP, Daxer A. Clinical outcomes after complete ring implantation in corneal ectasia using the femtosecond technology: A pilot study. Ophthalmology. 2011;118(7):1282-1290.
- Carrasquillo KG, Rand J, Talamo JH. Intacs for keratoconus and post-LASIK ectasia: Mechanical versus femtosecond laser-assisted channel creation. Cornea. 2007;26(8):956-962.
- Alio JL, Shabayek MH, Belda JI, et al. Analysis of results related to good and bad outcomes of Intacs implantation for keratoconus correction. J Cataract Refract Surg. 2006;32(5):756-761.
- Alio J, Salem T, Artola A, et al. Intracorneal rings to correct corneal ectasia after laser in situ keratomileusis. J Cataract Refract Surg. 2002;28(9):1568-1574.
- Mahmood H, Venkateswaran RS, Daxer A. Implantation of a complete corneal ring in an intrastromal pocket for keratoconus. J Refract Surg. 2011;27(1):63-68.
- Daxer A, Mahmoud H, Venkateswaran RS. Intracorneal continuous ring implantation for keratoconus: One-year follow-up. J Cataract Refract Surg. 2010;36(8):1296-1302.
- Jabbarvand M, Salamatrad A, Hashemian H, et al. Continuous intracorneal ring implantation for keratoconus using a femtosecond laser. J Cataract Refract Surg. 2013; 39(7):1081-1087.
- Jabbarvand M, Salamatrad A, Hashemian H, et al. Continuous corneal intrastromal ring implantation for treatment of keratoconus in an Iranian population. Am J Ophthalmol. 2013;155(5):837-842.
- Behrouz MJ, Hashemian H, Khodaparast M, et al. Intacs followed by MyoRing implantation in severe keratoconus. J Refract Surg. 2013;29(5):364-366.
- Daxer A. Adjustable intracorneal ring in a lamellar pocket for keratoconus. J Refract Surg. 2010;26(3):217-221.
- Kanellopoulos AJ, Pe LH, Perry HD, et al. Modified intracorneal ring segment implantations (INTACS) for the management of moderate to advanced keratoconus: Efficacy and complications. Cornea. 2006;25(1):29-33.
Hesam Hashemian, MD
- Assistant Professor of Ophthalmology, Ophthalmology Research Center, Farabi Eye Hospital, Tehran University of Medical Sciences, Tehran, Iran
- h-hashemian@tums.ac.ir
- Financial disclosure: None
Mahmoud Jabbarvand, MD
- Professor of Ophthalmology, Ophthalmology Research Center, Farabi Eye Hospital, Tehran University of Medical Sciences, Tehran, Iran
- mahmoodjabbarvand@yahoo.com
- Financial disclosure: None
Mehdi Khodaparast, MD
- Assistant Professor of Ophthalmology, Ophthalmology Research Center, Farabi Eye Hospital, Tehran University of Medical Sciences, Tehran, Iran
- dr_mkhz@yahoo.com
- Financial disclosure: None

