As the battle rages between proponents of laser-assisted cataract surgery and those who think this is an expensive fad with little to no advantage for our patients, IOL technologies continue to advance. Although the majority of IOLs implanted worldwide are still monofocal lenses, there are interesting developments under way, particularly in IOL technologies that are postoperatively adjustable, allowing surgeons to change IOL power after implantation.
The idea of being able to correct the spherical and cylindrical power of an IOL after implantation has been with us for some years, and the Light Adjustable Lens (LAL; Calhoun Vision) is available commercially outside the United States already. However, a number of other approaches to postoperative adjustment are being investigated, ranging from use of magnets to femtosecond lasers to multicomponent IOLs. Let us look at some of these exciting developments, which are also described in further detail in the subsequent five articles in this cover focus.
MODIFIABLE IOLs: A SOLUTION FOR POSTOPERATIVE REFRACTIVE ERRORS
Even with improvements in our ability to measure axial length and corneal power with modern IOL power calculation formulas, refractive errors still occur postoperatively. There have been studies in the past in which only 45% of patients were within ±0.50 D of the expected refractive outcome.1 Although postoperative outcomes are improving, one of the commonest reasons for IOL exchange is still postoperative refractive error.2 In order to deal with this problem, there have been various attempts to produce adjustable IOLs, and these fall into seven categories.
Light adjustment. As already mentioned, a light-adjustable IOL technology has been available for several years; however, some concerns have presented hurdles to widespread adoption, including the need for UV protection between implantation and the lock-in procedure. Improvements to the LAL design have been made to address this drawback (see LAL Timeline in "Update on the LAL”). One change is that the adjustable part of the optic will now be a 100-μm posterior layer. The aim of this and other changes was to decrease the number of postoperative adjustment procedures needed and alleviate the necessity for UV protection. Published results to date are impressive, with achieved correction of up to 2.25 D of sphere and 2.75 D of cylinder.3
Multicomponent adjustment. Although the idea of a multicomponent IOL has been proposed for nearly 20 years, Infinite Vision Optics now has developed a hydrophilic acrylic foldable dual IOL system, the Precisight, consisting of a plate-haptic base that provides only spherical correction coupled with an anterior lens that provides spherical, cylindrical, and multifocal correction as required. The front component, which fits into slots etched in the base lens, can be changed as needed in a second procedure. The Precisight IOL has been implanted in humans in small numbers,4,5 but the IOL’s biocompatibility, efficacy, and reversibility need further work.
Clarvista Medical also has developed a multicomponent device, the Harmoni lens. Like the Precisight, this IOL also consists of a base and a separate optic (spherical, multifocal, or toric), both made of a hydrophobic acrylic material. The lens is intended for capsular bag implantation. A clinical trial is under way; no data are yet available.
Mechanical adjustment. Another approach to postoperative IOL power adjustment is a mechanically adjustable IOL. The Acri.Tec AR1 has been implanted in animals and humans. The device consists of a 5.5-mm PMMA optic with two 1-mm cylinders attached at the optic-haptic junction (Figure 1).6 When activated by an instrument that is passed from outside the eye, the optic can move along the optical axis, giving up to 2.50 D of adjustment. This technology has been stable over a median 18-month follow-up, albeit with higher need for Nd:YAG laser capsulotomy than controls.7
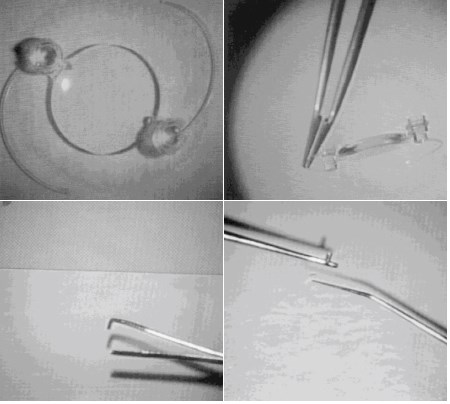
Figure 1. Power adjustment with the Acri.Tec AR1 is achieved by the piston (attached to the haptic) moving relative to the cylinder (attached to the optic).
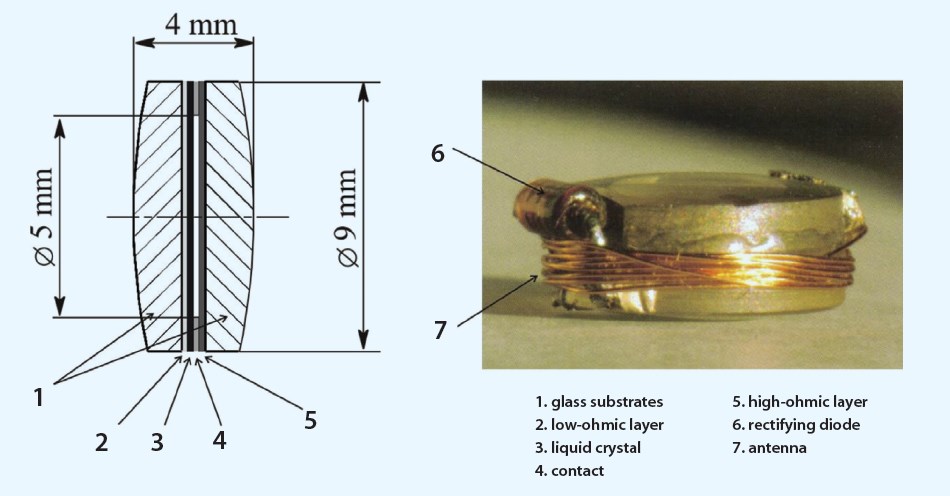
Figure 2. Schematic of the liquid crystal IOL (A). Image of the liquid crystal IOL and the outer surface of the lens (B).
Magnetic adjustment. A lens that started out requiring manual rotation of the optic to change lens power now has a rare earth magnet incorporated into its base unit and optic. Studies are currently under way to assess leaching and toxicity before any human trial is considered.8
Liquid crystal optic. A new type of lens optic material, liquid crystal, is also being investigated as a means to achieve postoperative power adjustments. Theoretically, the liquid crystal optic would be adjusted wirelessly to create an adaptive lens technology that could provide up to 3.00 D of accommodative amplitude. The challenge will be to find a biocompatible liquid crystal and isolate the receiving antenna and rectifier (Figure 2). There is currently one company with a prototype autofocal accommodating IOL (Sapphire AutoFocal IOL; Elenza). If successfully developed, this IOL would be capable of monitoring the patient’s pupillary dynamics associated with accommodation.9
Laser adjustment. Alcon and Perfect Lens are investigating femtosecond laser adjustments of lens power and toricity.10-12 Both companies are working to incorporate thin layers of shape-altering material into their lens optics. When activated by femtosecond laser pulses, these materials would change shape and cause the optic to change power. The treatment time is estimated to be between 20 and 60 seconds.13
Chemical adjustment. The last type of modifiable IOL currently under investigation would achieve power adjustment by embedding photoactive derivatized coumarins into the lens optic. When exposed to two photons of either identical or different frequencies, the refractive index, and, thus, the focusing power of the lens, could be altered for spherical and toric correction. Because these changes would be immediate, they could easily be fine-tuned. Unlike the LAL, natural sunlight and UV light should have no effect on this material.14,15
AT A GLANCE
• Several new IOL technologies may allow one to correct the spherical and cylindrical power of an IOL after implantation.
• Although standard monofocal IOLs and multifocal and accommodating IOLs will continue to dominate the market share in the next few years, modifiable IOLs are expected to take center stage over time.
CONCLUSION
With more cataract surgery patients than ever before expecting perfect vision after lens implantation, the desire for modifiable IOL technologies is gaining momentum. Also adding to the appeal of this kind of lens is the increasing number of patients who have undergone laser refractive surgery, as they are more inclined to encounter postoperative refractive surprises after cataract surgery.
Although standard monofocal IOLs and multifocal and accommodating IOLs will continue to dominate the market share in the next few years, we can expect modifiable IOLs to take center stage over time, as means for surgeons to adjust IOL power after implantation and for patients to achieve emmetropia. n
Richard Packard, MD, DO, FRCS, FRCOphth
- Director of Arnott Eye Associates, London
- Practices at Prince Charles Eye Unit, King Edward VII Hospital, Windsor, UK
- mail@eyequack.vossnet.co.uk
- Financial disclosure: Consultant, Lecture Fees (Alcon)
1. Brandser R, Haaskjold E. Drolsum L. Accuracy of IOL calculation in cataract surgery. Acta Ophthalmol Scand. 1997; 75:162-165.
2. Mamalis N, Brubaker J, Davis D, Espandar L,Werner L. Complications of foldable intraocular lenses requiring explantation or secondary intervention–2007 survey update. J Cataract Refract Surg. 2008; 34:1584-1591.
3. Hengerer FH, Hutz WW, Dick HB, Conrad-Hengerer I. Combined correction of axial hyperopia and astigmatism using the light adjustable intraocular lens. Ophthalmology. 2011;118:1236-1241.
4. Fuchs HA, Frohn A, Dean K, Werblin TP. Multiple component intraocular lens: first human implantation. J Refract Surg. 2009;25:390-393.
5. Portaliou DM, Grentzelos MA, Pallikaris IG. Multicomponent-intraocular lens implantation: two-year follow-up. J Cataract Refract Surg. 2013; 39:578-584.
6. Jahn CE, Jahn MA, Kreiner CF, et al. Intraocular lens with reversibly adjustable optical power; pilot study of concept and safety. J Cataract Refract Surg. 2003;29:1795-1799.
7. Jahn CE, Schöpfer DC. Cataract surgery with implantation of a mechanically and reversibly adjustable intraocular lens. Arch Ophthalmol. 2007;125(7):936-939.
8. Matthews MW, Eggleston HC, Pekarek SD, Hilmas GE. Magnetically adjustable intraocular lens. J Cataract Refract Surg. 2003;29:2211-2216.
9. Simonov AN, Vdovin G, Loktev M. Liquid-crystal intraocular adaptive lens with wireless control. Opt Express. 2007;15:7468-7478.
10. Sacharoff A, Karakelle M, inventors; Novartis AG, assignee. Non-invasive power adjustable intraocular lens. U.S. Patent 12/434,237. May 1, 2009. Available at: http://patft.uspto.gov/netacgi/nph-Parser?Sect1ZPTO2&Sect2ZHITOFF&pZ1&uZ%2Fnetahtml%2FPTO%2Fsearch-bool.html&rZ1&fZG&lZ50&co1ZAND&dZPTXT&s1Zsacharoff.INNM.&OSZIN/sacharoff&RSZIN/sacharoff. Accessed November 4, 2014.
11. Bille JF, inventor; Perfect IP, LLC, assignee. System for forming and modifying lenses and lenses formed thereby. U.S.Patent 13/030,958. February 18, 2011. Available at: http://patft.uspto.gov/netacgi/nph-Parser?Sect1ZPTO2&Sect2ZHITOFF&pZ1&uZ%2Fnetahtml%2FPTO%2Fsearch-bool.html&rZ3&fZG&lZ50&co1ZAND&dZPTXT&s1ZBille.INNM.&OSZIN/Bille&RSZIN/Bille. Accessed November 4, 2014.
12. Bille JF. Generation and in situ modification of customized IOLs. Paper presented at: the ASCRS Symposium on Cataract, IOL and Refractive Surgery; March 2011; San Diego, California.
13. Ding L, Blackwell R, Kunzler JF, Knox WH. Large refractive index change in silicone-based and non-silicone-based hydrogel polymers induced by femtosecond laser micro-machining. Opt Express. 2006;14:11901-11909.
14. Trager J, Heinzer J, Kim H-C, Hampp N. Polymers for in vivo tuning of refractive properties in intraocular lenses. Macromol Biosci. 2008; 8:177-183.
15. Trager J, Kim H-C, Hampp N. Ophthalmology: two-photon treatment. Nat Photonics. 2007;1:509-511.

