Advanced Eye Analysis
A wonderful opportunity for patient education.

By George O. Waring IV, MD, FACS
With the advent of advanced digital diagnostics comes a wonderful opportunity for patient education. My mentor Daniel S. Durrie, MD, taught me the value of an advanced eye exam with his advanced ocular analysis. At the Magill Vision Center, we use advanced diagnostic technology not only for clinical assessment but also to educate patients. Marketed as an advanced eye analysis, this exam takes patients on a digital tour of their eyes to create a truly visual experience. (Editor’s note: Watch an example of the advanced eye analysis on Eyetube: http://bit.ly/waring0416.)
AT A GLANCE
• Advanced eye exams should be a part of advanced eye clinics and a premium patient experience.
• Patients appreciate the high-tech, high-touch experience of an advanced eye anaylsis and associate it with state-of- the-art technology.
• Specific displays from diagnostic devices can help to clarify patient complaints or propose and explain certain surgical procedures.
Within minutes of checking in, every patient is escorted to our advanced eye analysis center, where he or she is essentially put on a digital diagnostic track in which our technicians explain what each machine does. This is important, as all patients appreciate the high-tech, high-touch experience. Furthermore, they associate the advanced eye analysis with state-of-the-art technology. All digital images are then imported into our electronic health record system while the patient is once again escorted, this time to the exam lane. While dilating, the patient reviews educational material explaining the benefits of laser-assisted lens surgery and advanced lens implant options on digital tablets.
At the outset of the exam, I explain to the patient that we will evaluate his or her overall ocular health with an advanced eye analysis that assesses the lids, lashes, lenses, nerves, vessels, and nutritional status. Once the biomicroscopic exam is completed, the patient is taken on a digital tour of his or her eye, using a camera as analogy and paying particular attention to the two lenses and the film of the camera. I begin with a discussion of the patient’s outer lens and show his or her level of astigmatism with topographic and tomographic images, including the ectasia risk screening maps for LASIK evaluations. This is followed by OCT images of the cornea.
The patient is then educated on the health of his or her internal focusing lens with a dilated Scheimpflug image of the lens correlated with the densitometry (both with the Pentacam; Oculus). This step is important in that patients can easily see the aging changes associated with lens opacity and the correlating light scatter.
Next, the patient is shown “how you are seeing” with a double-pass wavefront (HD Analyzer; Visiometrics), which “measures not only the amount but also the pattern of blur” (point spread function), as we explain. Although patients are generally thrilled postoperatively, images can be repeated and compared after lens replacement to demonstrate that their new clear lens has no light scatter or blur. The exam is augmented with slit-lamp video and photography as needed, as well as with macular OCTs or fundus images.
Additional diagnostics and imaging are performed for other conditions and procedures. For example, in patients with narrow angles, particularly hyperopes, we will image and measure their angles with anterior segment OCT and Scheimpflug imaging before and after lens replacement, and we can often correlate a drop in IOP with widening of the angle after lens replacement. Patients appreciate the procedure more when they can visualize why they have improved. We will perform similar imaging for patients implanted with the Visian ICL (STAAR Surgical) to measure their angles and vaults.
Use of our advanced internal lens analysis is paramount to properly educate patients with dysfunctional lens syndrome. This exam is often the first time patients have the opportunity to understand why they stopped driving at night and why their glasses no longer work despite multiple attempts. We discuss the nonsurgical and surgical treatment options for these patients, including dysfunctional lens replacement (DLR).
It is worth mentioning that DLR is different from clear or refractive lens exchange in many ways. Most important, these lenses are not clear, as demonstrated by the objective diagnostics described above. Even though these patients may not qualify for an insurance-based lens procedure, they came to our clinic looking for surgical options to reduce their dependence on glasses. Once we show them the sources of their blur, it is easier for patients to understand that they may be better served with a lens-based refractive procedure than with a cornea-based procedure. This is particularly true for patients older than 60 years. As with all surgical consultations, we outline all risks, benefits, and alternatives, including the relative risks associated with lens- and cornea-based procedures. However, patients like that DLR is a permanent, all-in-one solution that addresses both congenital and age-related causes of ametropia.
Advanced eye exams should be a part of advanced eye clinics and a premium patient experience. Things have changed since Herman Snellen first described the gold standard visual acuity measurement in 1862. We now have the technology to objectively measure and show patients their quality of vision with advanced diagnostics such as the HD Analyzer. These advances have enabled us to not only serve our patients with better options and outcomes but to better educate them as well.
Diagnostic Images Make Excellent Patient Education Tools
Pictures can be worth thousands of words.

By Fernando Faria-Correia, MD
Since I began performing refractive surgery, I have used a Scheimpflug imaging device (Pentacam HR; Oculus) and a wavefront analyzer (iTrace; Tracey Technologies) on a routine basis. Many patients in our clinic have dry eye disease, and use of the Keratograph 5M (Oculus) is essential for the study and follow-up of such patients.
DIAGNOSTICS AS VISUAL AIDS
Not only do I integrate these advanced digital diagnostics routinely as part of my clinical examinations, but I also use these instruments to provide visual aids for patients. Generally, I select specific displays from each device that will help me to clarify the patient’s complaints or to propose and explain certain surgical procedures. The types of displays that I select depend on the patient’s age and type of complaint or desire.
For example, if a patient with mild to moderate myopia is interested in laser vision correction (LVC), I usually look at the four-map display and the Belin/Ambrósio enhanced ectasia display on the Pentacam to ensure that femtosecond LASIK is appropriate. Integration of clinical data with corneal tomography data is useful to analyze the patient’s susceptibility to ectasia after LVC.
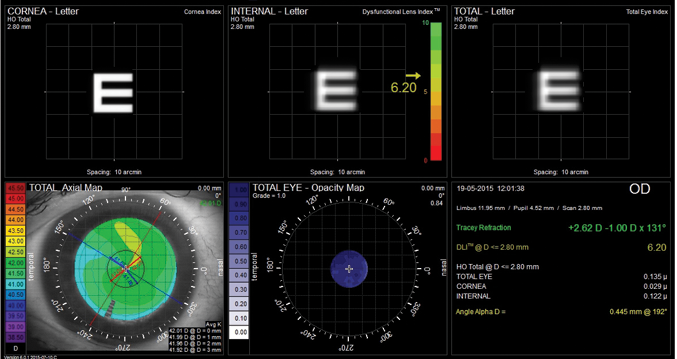
Figure 1. The iTrace dysfunctional lens display demonstrates the contributions of cornea and crystalline lens and total eye vision simulation using Snellen E. This display also illustrates the dysfunctional lens index score on a color scale.
For presbyopic and post-LASIK patients, I usually check the Scheimpflug-based lens densitometry from the Pentacam and the dysfunctional lens index (DLI) on the iTrace (Figure 1). Combining these devices is essential in order to identify where the problem is: in the cornea or in the lens. Some patients are more suitable for refractive lens exchange with a multifocal IOL rather than LASIK because the problem is in their crystalline lens. In this type of patient, I also select the cataract preop display on the Pentacam (Figure 2), as this helps us to check the magnitude of higher-order aberrations and assess whether a toric IOL may be appropriate.
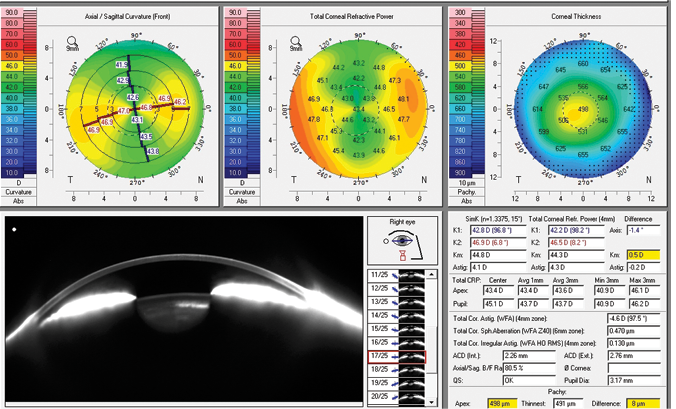
Figure 2. The Pentacam cataract preoperative display.
ELUCIDATE COMPLAINTS
Explaining the data presented on these displays in a routine examination helps me to elucidate the patient’s visual complaints and propose an appropriate treatment. Patients respond well to the visual information. I find that patient satisfaction is enhanced when patients are able to visualize their problems. It also motivates patients to seek more knowledge about their disease, particularly the pathophysiologic mechanisms, clinical signs and symptoms, and treatment options.
Sometimes patients in the examination room are reluctant to ask questions. They may feel that they are wasting the doctor’s time or are afraid of looking ridiculous or poorly informed. Having these imaging outputs as visual support enables a more open conversation with these patients. It allows the physician to better clarify any doubts and relieve anxieties, as well as present the best treatment or surgery options available. These interactions are helpful to establish more confidence in patients regarding the doctor and his or her team.
CONCLUSION
The integration of advanced digital diagnostics undoubtedly improves the level of patient care. For the physician, it helps with differential diagnosis and selection of the most appropriate treatment option. For patients, these visual aids help to objectify their problems and understand the causes and the therapeutic modalities available. The interaction between physician and patient in presentation of the diagnostic images also improves patient confidence regarding the treatment or procedure proposed. These tools can also help to obtain informed consent for surgery.
George O. Waring IV, MD, FACS
• Director of Refractive Surgery and Assistant Professor of Ophthalmology, Storm Eye Institute, Medical University of South Carolina
• Medical Director, Magill Vision Center, Mt. Pleasant, South Carolina
• Member, CRST Europe Global Advisory Board
• waringg@musc.edu
• Financial disclosure: Consultant (Abbott Medical Optics)
Fernando Faria-Correia, MD
• Cornea and Refractive Surgery Department, Instituto CUF, Porto, Portugal
• Cornea and Refractive Surgery Department, Hospital de Braga, Braga, Portugal
• Research Associate, Life and Health Sciences Research Institute, School of Health Sciences, University of Minho, Braga, Portugal
• f.faria.correia@gmail.com
• Financial disclosure: None

