

When asked about the most challenging cases we have to operate upon, a special group of patients immediately comes to mind. These are individuals who will live an entire life with the consequences of our interventions. How skilled we are during surgery and how well we provide postoperative management will determine their visual function for—given today’s life expectancy figures—80, 90, or more years. These are our youngest patients: infants with cataract formation. It is absolutely crucial to provide these young patients with the best we can offer them.
AT A GLANCE
• Laser cataract surgery in pediatric cases is currently an off-label procedure; however, the authors have seen a clear improvement in surgical capabilities and options with this technology in this population.
• The surgeon faces a number of anatomic challenges in these youngest patients including small pupils and tight palpebral fissures.
• The Bochum correction formula helps the surgeon to achieve the exact precalculated anterior and posterior capsulotomy diameters in pediatric eyes undergoing laser cataract surgery.
• Frequent administration of topical steroids is still recommended to reduce the risk of complications such as fibrinous membrane formation, synechiae formation, inflammatory deposit formation on the IOL, and cystoid macular edema.
There are indications—some may call it proof—that the femtosecond laser can contribute to achieving these goals for these young patients.1 We have taken only the first steps, but our experience in treating the cataracts of babies, children, and teenagers with this technology is growing and has, to date, been undoubtedly encouraging. It must be pointed out that this is an off-label procedure, as is so often the case when doctors treat children, whether in ophthalmology or in other medical disciplines.
SPECIAL REQUIREMENTS
There are a number of requirements for the setting and the surgical team when it comes to performing laser-assisted cataract surgery in infants. (For the record, I prefer the term laser cataract surgery,2 and I will therefore use this terminology for the rest of this article.)
Operating room conditions. We consider it a prerequisite to have the laser system in the operating room; we treat it as one tool in a completely sterile procedure.3 This is an essential condition, particularly if redocking of the patient to the laser becomes necessary during the procedure. The climate control system of the room also must be sufficient, and there must be enough space for an addition to the usual surgical team: an anesthesiologist and his or her pediatric anesthesia equipment.
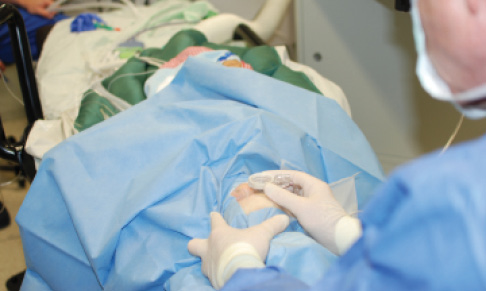
Figure 1. Sterile docking in pediatric laser cataract surgery.
Size-appropriate equipment. The surgeon faces a number of anatomic challenges in these youngest patients and must deal with, for instance, small pupils and tight palpebral fissures; this is an intervention in which every millimeter counts. Because no available femtosecond laser system was created for the treatment of small children, placing the fluid-filled interface used in our system between the laser and the small globe (compared with the size of an adult’s) is challenging in children under the age of 3 years. Fortunately, at least one system so far (Catalys; Abbott Medical Optics) has made available a smaller liquid optic interface that works for children, with a diameter of 12 mm compared with the standard 14.1 mm (Figure 1).
Selected applications. Unlike in adults, we do not perform lens fragmentation with the laser in children, and we are also reluctant to use the laser for corneal incisions in these patients.
SETTINGS AND OTHER CONSIDERATIONS
We started using laser cataract surgery in pediatric patients in December 2011 and have operated on 56 eyes to date. We always use the laser to perform anterior capsulotomy and often also posterior capsulotomy. Our settings are found on the following page.
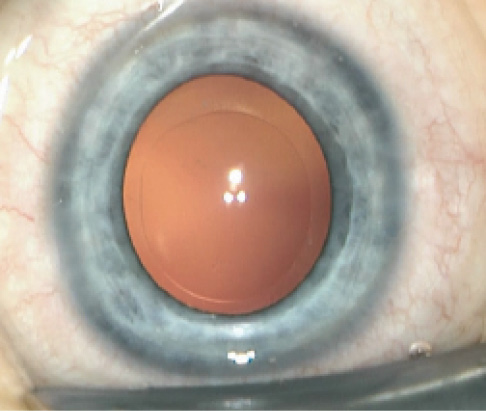
Figure 2. A perfectly sized circular anterior laser capsulotomy.
Every case is documented on high-definition video. Every removed capsulotomy disc undergoes histopathologic evaluation, which has shown that the edge quality is superb—better even than in adults.
Although anterior and posterior capsulotomies have been precisely centered and of perfect circularity, the capsulotomy diameter was at first larger than intended in all of our pediatric cases. This enlargement appears to depend on age: The younger the patient, the more pronounced the enlargement. We have computed a capsulotomy enlargement factor, which is 1.34 + (-0.009 X age in years). As a consequence, we have developed the Bochum correction formula, which is a valuable tool to achieve the exact precalculated anterior and posterior capsulotomy diameters (Figure 2).4
LASER SETTINGS IN PEDIATRIC CASES
• Pulse energy: 4 to 10μJ
• Anterior capsulotomy: 400 to 1,000μm incision depth, 3.3 to 5 mm intended diameter
• Posterior capsulotomy: 600 to 1,000μm incision depth, 3.2 to 4.7 mm intended diameter
We usually shy away from IOL implantation in children younger than 1 year old. If an IOL is implanted, the primary posterior laser capsulotomy helps to keep the anterior vitreous hyaloid intact. We have not encountered anterior or posterior capsular tears. In a limited number of eyes, minimal tissue bridges remained after anterior capsulotomy, but these were easy to break manually. There was no contraction syndrome, vitreous prolapse, or uncommon degree of inflammation.
POSTOPERATIVE CARE
In the immediate postoperative stage, the patient’s parents must take care to administer pharmacologic therapy as recommended by the surgeon or the ophthalmologist in charge of follow-up. Normally up to three kinds of drugs are instilled as eye drops: antibiotics, antiinflammatory agents, and maybe a mydriatic or cycloplegic agent. Because the inflammatory response to cataract surgery can be quite intense in children, the frequent administration of topical and rarely even systemic steroids is crucial to reduce the risk of complications such as fibrinous membrane formation, synechiae formation, inflammatory deposit formation on the IOL, and cystoid macular edema.
CONCLUSION
After having dedicated more than 15 years to pediatric cataract surgery before the advent of the femtosecond laser (HBD), we see a clear improvement in surgical capabilities and options with this technology. It gives the surgeon a great degree of pleasure to assume that the good we do with a successful intervention in a child with cataract will last far beyond our postoperative follow-up.
1. Dick HB, Schultz T. Femtosecond laser-assisted cataract surgery in infants. J Cataract Refract Surg. 2013; 39:665-668.
2. Dick HB. Bladeless custom femtosecond laser-assisted refractive cataract surgery? let’s give our latest breakthrough surgical technique a name that fits. J Refract Surg. 2015;31(5):346.
3. Dick HB, Gerste RD. Plea for femtosecond laser pre-treatment and cataract surgery in the same room. J Cataract Refract Surg. 2014; 40:499-500.
4. Dick HB, Schelenz D, Schultz T. Femtosecond laser-assisted pediatric cataract surgery: Bochum formula. J Cataract Refract Surg. 2015; 41:821-826.
H. Burkhard Dick, MD, PhD
• Director and Chairman, University Eye Hospital, Bochum, Germany
• Member, CRST Europee Editorial Board
• burkhard.dick@kk-bochum.de
• Financial disclosure: None
Tim Schultz, MD
• Physician, University Eye Hospital Bochum, Bochum, Germany
• Financial disclosure: None

