
From our patients’ perspective, two of the most significant negative events in their aging process are vision-related: (1) the development of presbyopia and (2) the development of cataracts. First, patients lose the flexibility in their vision, and then they lose the clarity. Historically, most surgeons focused solely on the latter, clarity, while feeling ill-equipped to bring back the flexibility and range of vision that patients enjoyed in their earlier years of life.
Now, with the emergence of improved preoperative analysis and advanced-technology IOLs, and with attentive postoperative care, more surgeons are delving into the world of refractive cataract surgery. Surgeons and patients are finding joy by addressing not only clarity of vision but also improving the range of vision that our patients experience.
Stepping into the world of refractive cataract surgery does not come without questions or concerns, however. This article highlights some of the top concerns that one faces in starting a refractive cataract program and offers some pearls for addressing these issues.
IS MY PREOPERATIVE ANALYSIS ADEQUATE?
One goal of the preoperative cataract consultation and associated testing is to prevent the unhappy refractive cataract patient. In our practice, we have found the use of corneal topography, wavefront analysis, and OCT of the macula and nerve to be invaluable tools for screening patients.
By identifying irregular astigmatism, high degrees of higher-order aberrations, large angle kappa, occult maculopathies, and optic neuropathies before surgery, we can steer patients who may be highly motivated to have refractive cataract surgery to a more traditional approach. Conversely, when patients are identified as good candidates, we can have high confidence that we will be able to deliver the outcomes they desire.
A strong focus on operational excellence in optical biometry assessment, with comparison of keratometry measures between multiple devices, can significantly improve IOL selection and outcomes.
DO I HAVE THE INTRAOPERATIVE ACUMEN NECESSARY?
Obtaining excellent results with refractive cataract surgery requires excellent surgery and attention to detail. Certain tools can help with this, including automated capsulotomy technology with a femtosecond laser or precision pulse capsulotomy (Figure) with the Zepto (Mynosys).
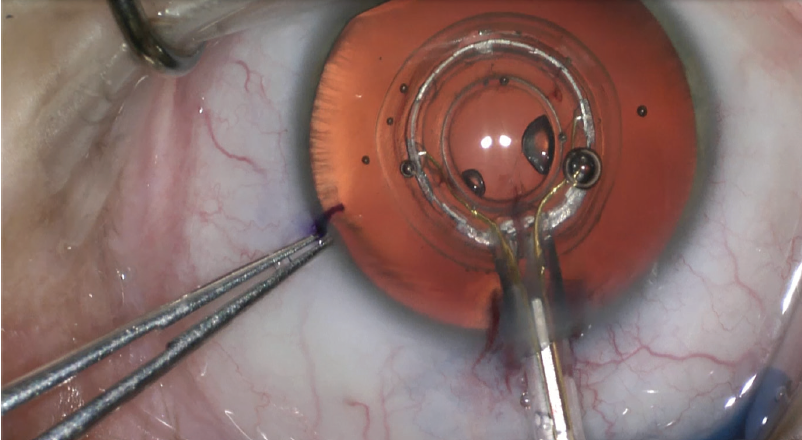
Figure. The clear round tip of the Zepto capsulotomy system allows positioning of the capsulotomy using light reflex. As the patient fixates, the capsulotomy can be specifically centered on the patient’s visual axis using the first and fourth Purkinje images. The device is aligned via patient fixation; if the patient cannot fixate, the surgeon can use a second instrument to perform manual alignment. This allows the surgeon to optimize 360° of anterior capsule overlap of the optic.
By paying attention to capsular overlap and centration of the IOL, we can improve the predictability of effective lens position (ELP), reduce lens tilt, and, hopefully, reduce the risk of induced higher-order aberrations such as coma.
The use of intraoperative aberrometry can also help reduce the likelihood of residual refractive error. For patients who have significant astigmatic error or who have undergone previous laser vision correction, aberrometry can be of particular benefit to reduce the risk of needing a laser enhancement after surgery.
DO I HAVE AN ENHANCEMENT PLAN?
Similar to what we know from the world of laser vision correction, residual refractive error is a major driver of patient satisfaction after refractive cataract surgery. Despite all our preoperative measurements and attention to detail during surgery, our patients still go through their own independent, and sometimes unpredictable, healing response.
With traditional cataract surgery, we are all comfortable with this fact and understand that a fine-tuning with a pair of glasses will be necessary. For refractive cataract surgery, this fine-tuning is often completed with a laser at present. In the future, the emergence of light-adjustable lens technologies and refractive index shaping may allow this fine-tuning to be completed without disruption of the ocular surface.
WHAT TECHNOLOGIES DO I NEED TO INVEST IN?
Each piece of technology you invest in comes with a price, and deciding which technologies to invest in can be challenging—particularly if you are in solo practice. I encourage surgeons to find a group of trusted colleagues to help in evaluating new technologies as they enter the market and determine which is a fit for your practice.
In its simplest form, undertaking astigmatic management by performing limbal relaxing incisions and developing comfort with toric IOLs can provide an easy entry into the space with minimal investment.
WHAT WILL MY MENTORS THINK?
As trainees, many of us had mentors who shaped our views of our beloved profession. Some of these role models may have expressed concerns about the refractive side of ophthalmology. It is important to remember your own core values. For me, that means always doing what’s right. It means educating patients—but not overselling them—on the options they have, and allowing patients to make educated decisions about what is best for them.
HOW DO I EDUCATE MY STAFF?
Our staff—our work family—spends more time with patients than we do. Every interaction matters in the customer experience cycle:
- The phone call with the patient to set up an appointment;
- The before-visit phone call or video with the team and doctor to review the appointment;
- The greeting that patients experience when they enter our clinic;
- The testing experiences they have with our technicians;
- The consultation time with the doctor;
- The coordination of surgery and aftercare by the surgery counselor;
- The departure after the clinic visit; and
- The extension of their visit that we undertake by connecting with referring doctors and their teams.
Each of these steps is crucial to the patient experience, and, notably, the surgeon is heavily involved in only one of those steps. Ensuring that your staff is empowered to answer patients’ questions and meet them in their moments of vulnerability helps to ensure that each patient has a tremendous experience.
HOW DO I EDUCATE MY PATIENTS?
It is vital to educate patients about all their options at the time of cataract surgery. A 65-year-old patient can be expected to live 20 years after cataract surgery. Helping these patients realize that they are making a 20-year decision about their vision is helpful.
I try to keep it simple. If we determine that a patient has a cataract, the question that should follow is: “Does the cataract bother you enough to have surgery?” If the answer is yes, then the next question is: “Do you want to do a lot with glasses or without glasses?”
Helping patients understand that their natural lens has lost its flexibility (presbyopia) and clarity (cataract) and that we can correct one (the clarity only) or both (the clarity and the flexibility) is a useful approach. I do not talk a lot about the technology. I do not talk about corneal topography, wavefront mapping, measuring angle kappa, OCT, intraoperative aberrometry, automated capsulotomy, extended aftercare, or laser fine-tuning. What patients care about is how they are going to use their eyes after surgery.
DO I HAVE A WORLD-CLASS CUSTOMER EXPERIENCE?
My partner, Vance Thompson, MD, FACS, has shaped my understanding of this important topic. When people consider this question, they often overlook the importance of the staff. It might be helpful to ask: “Do I have a world-class work family experience?”
I believe it is impossible to have a world-class customer experience without a world-class work family experience. Our management team spends countless hours considering how to improve our team experience. This allows our team to focus solely on our patients and find ways to surprise and delight them on a daily basis.
SUMMARY
There has been no better time in history to be a cataract surgeon than now.
Continued investment and innovation in technology will propel our field forward and allow us to build upon an already great procedure. I often tell patients that the perfect IOL would act like the human lens at age 21 and allow the patient to regain his or her ability to see at all distances without undue complications or visual compromise. Although we are not there yet, we have wonderful options that provide great opportunities for our patients to experience improvement in both the clarity and the flexibility of their vision.



