
Extracapsular cataract extraction (ECCE) is a technique that paved the way for modern cataract surgery, yet it remains relevant only as a plan B when the possibility of successfully executing phacoemulsification or small-incision cataract surgery (SICS) no longer seems likely intraoperatively.
All cataract procedures work on a principle of pressure gradients related to the size of the nucleus versus that of the incision, and nuclear fragments tend to exit the eye through the area of least resistance. During phacoemulsification, surgeons attempt to extract the cataract through the small port of the phaco probe. Because the phaco port is smaller than the size of the nucleus for most of the cataract procedure, a saline boost, influx of fluid, or irrigation is needed to draw the nucleus toward the phaco port (ie, followability), which makes the phaco probe the area of least resistance (with the addition of aspiration at the phase port). In ECCE, the nuclear fragment is smaller than the incision, which helps draw material toward the incision using a gradient of high to low pressure. This balance unfortunately changes drastically when the nucleus is located posterior to the iris, which has the potential to prevent the nucleus from being drawn from the posterior to the anterior chamber.
CONVERTING FROM PHACOEMULSIFICATION TO ECCE
Indications
There are three indications for converting from phacoemulsification to ECCE:
No. 1: Posterior capsular rupture or zonular dehiscence with or without a dropped nucleus when the nuclear fragment is larger than half the size of the cataract (> 5 mm);
No. 2: Errant capsulorhexis in an eye with a hard cataract; or
No. 3: Unexpectedly dense cataract for which standard phacoemulsification could lead to permanent corneal damage.
How to Make the Transition
Whenever conversion from phacoemulsification to ECCE is warranted, it is important first to ensure that the anterior chamber is well formed so as to prevent hypotony. Next, any nuclear pieces should be brought above the iris and into the anterior chamber. Otherwise, once the incision is enlarged, bringing the nucleus above the iris will become extremely difficult because the pressure gradient will not support it.
Step No. 1: Mark the planned corneal incision based on the size of the nucleus (Figure 1).
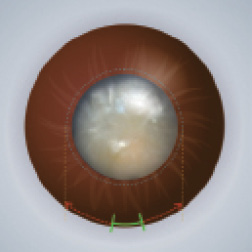
Figure 1. The planned corneal incision is marked based on the size of the nucleus.
Step No. 2: Using corneal scissors, enlarge the phaco incision as marked on the cornea (Figure 2).

Figure 2. The phaco incision is marked on the cornea using corneal scissors.
Step No. 3: Extract the nucleus using a traditional technique of pressure and counter-pressure (Figure 3). Alternatively, remove the nucleus by injecting OVD behind it while depressing the posterior lip of the incision (Figure 4).

Figure 3. The nucleus is extracted using a traditional technique of pressure and counter-pressure.

Figure 4. The nucleus can alternatively be removed by injecting OVD behind it while depressing the posterior lip of the incision.
Step No. 4: Inspect the anterior chamber for any vitreous prolapse (Figure 5). If vitreous has prolapsed, place a three-port trocar inside the eye (anterior or posterior), as shown in Figure 6. Doing so facilitates using a vitrectomy cutter. Cutting prolapsed vitreous via a pars plana approach will bring the vitreous from the anterior chamber back into the posterior chamber, thereby reducing the chance of posterior capsular rupture or zonular dehiscence (Figure 7).
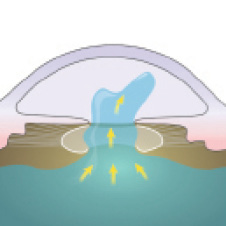
Figure 5. Inspect the anterior chamber for any vitreous prolapse.
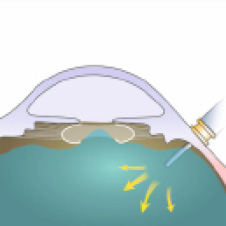
Figure 6. If vitreous has prolapsed, place a three-port trocar inside the eye (anterior or posterior).
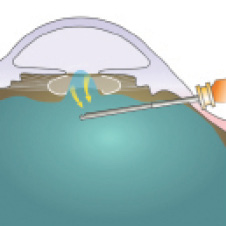
Figure 7. Cutting prolapsed vitreous via a pars plana approach will bring the vitreous back into the posterior chamber.
Step No. 5: Place the IOL in the bag if the capsulorhexis is complete and any posterior capsular rupture is small and roundish (Figure 8). If the capsulorhexis is complete but there is a large posterior capsular rupture or zonular dehiscence, then a secondary IOL may be implanted (Figure 9). Various techniques may be used for placing the lens implant, including a glued IOL, anterior chamber IOL, scleral-fixated IOL, or Yamane technique (Figure 10).

Figure 8. Place the IOL in the bag if the capsulorhexis is complete and any posterior capsular rupture is small and roundish.

Figure 9. If the capsulorhexis is complete but there is a large posterior capsular rupture or zonular dehiscence, a secondary IOL may be implanted.

Figure 10. Various techniques may be used for placing the IOL, including a glued IOL, anterior chamber IOL, scleral-fixated IOL, or Yamane technique.
Bonus Tips
The ECCE incision should be large. If the incision is small and pressure is high enough, the nuclear fragment may drop into the posterior chamber.
CONVERTING FROM SICS TO ECCE
Indications
There are two indications for converting from SICS to ECCE:
No. 1: The sizes of the incision and nucleus are mismatched; or
No. 2: During SICS on a nanophthalmic eye, a deformed nucleus is encountered.
How to Make the Transition
Successful conversion from SICS to ECCE requires an understanding of wound architecture. The SICS incision is a valvular opening. Its horizontal (temporal to nasal) length is smaller on the outside (scleral side) and larger on the inside (corneal side). When opened to express the nucleus, a SICS incision is more shallow than an ECCE incision based on the principle of volume. For this reason, horizontally large nuclei are easily expressed via the SICS technique, whereas thick nuclei are difficult to express via the SICS technique and can cause trauma.
Step No. 1: Inject OVD into the eye to push the nucleus away from the incision.
Step No. 2: Create a V incision. Place corneal scissors at the external edge of the SICS wound and slide one blade inside the eye while the other stays out (Figure 11).

Figure 11. Create a V incision by placing corneal scissors at the external edge of the SICS wound and sliding one blade inside the eye while the other stays out.
Step No. 3: Make a fine cut all the way to the inside of the eye.
Step No. 4: Repeat steps No. 2 and 3 on the other side to form an ECCE type of incision.
Step No. 5: Express the nucleus with a traditional technique of pressure and counter-pressure (Figure 12). Alternatively, viscoexpression may be used as described earlier. The latter technique can be particularly useful if the capsule has broken. An OVD cannula, placed under the nucleus but over the iris, can behave like a scaffold and prevent downward descent of the nucleus; the instrument pushes the nucleus in the direction of the wound and eventually out of the eye (Figure 13).
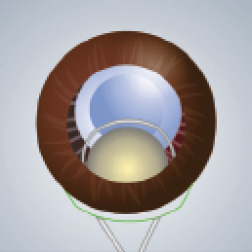
Figure 12. Express the nucleus with a traditional technique of pressure and counter-pressure.

Figure 13. A visco cannula pushes the nucleus in the direction of the wound and eventually out of the eye.
Step No. 6: Implant the IOL. If a can-opener capsulotomy was made, implantation of the lens inside the bag will be challenging, so placement in the sulcus may be warranted (Figure 14). If vitreous involvement is observed, switching to secondary IOL implantation is prudent (Figure 15).
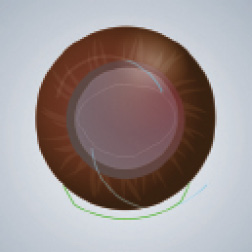
Figure 14. If a can-opener capsulotomy was made, implantation of the lens inside the bag will be challenging, so placement in the sulcus may be warranted.

Figure 15. If vitreous involvement is observed, switching to secondary IOL implantation is prudent.
CONCLUSION
A plan B allows surgeons to deal with hurdles when they arise, but such a technique is only as good as its timing. In other words, delaying conversion to ECCE could put your case in the hands of a retina colleague.



