
The climate crisis is a health emergency, and it’s accelerating faster than anticipated.1 Human health is already being harmed, and the impact will become more severe without immediate and concerted action.1 In early September, more than 200 medical journals released a joint statement in collaboration with The Global Alliance on Climate Change and Health calling for physicians to address this issue, especially with political leaders.2 The US Department of Health and Human Services has recognized the urgency of the crisis and recently created an office that will treat climate change as a public health issue.
The incidence of illness, injury, and death from extreme weather events is increasing. Rising sea levels, floods, and the accumulation of greenhouse gases affect water and food supplies and their quality. There are changes in vector ecology and thus the locations and incidences of infectious diseases. Increases in air pollution and pollen are leading to an increased incidence of asthma, allergies, and respiratory and cardiovascular diseases. Forced migration related to climate change/desertification is now occurring worldwide. Mental health is being affected both acutely and chronically.3 Everyone’s health is threatened. The most vulnerable, however, are children, senior citizens, pregnant women, outdoor workers, individuals with chronic illnesses, and people living in disadvantaged communities.
THE CLIMATE CRISIS AND OPHTHALMOLOGY
Though it may not be as obvious as in other medical specialties, the effects of climate change on ophthalmology are many.
Elevated pollen counts. An increasing number of patients come to me with itchy eyes. “But, Doctor, I never had allergies before,” many of my elderly patients say. Warming temperatures can increase pollen production, prolong allergy seasons, and worsen air pollution, leading to more allergic conjunctivitis.4,5
Severe weather. The incidence of eye injuries increases in extreme weather events, but there are also many less obvious ophthalmic sequelae of climate change. As the intensity of storms increases, ozone in the stratosphere decreases, allowing more UV radiation to reach people.6 Cataracts, pterygia, certain corneal lesions, eyelid skin cancers, and uveal melanoma have all been associated with increased UV radiation exposure.7,8
Pollution. Air pollution—a contributor to and a result of climate change—affects multiple organs.9 In one study, a small increase in exposure to tiny pollution particles raised the risk of developing age-related macular degeneration by 8%, and small changes in larger pollution particles and nitrogen dioxide were linked to a 12% higher risk of adverse retinal changes.10 Another recent study found that people living in areas with high amounts of fine particulate matter pollution were at least 6% more likely to report having glaucoma than people in the least polluted areas.11 Globally, increased incidences of trachoma, onchocerciasis, and nutritional deficiencies due to climate change have been predicted.8
In addition to the direct effects of climate change on the health of our patients, eye care services can be disrupted by climate-related effects on supply chains. Climate change can affect raw material extraction, manufacturing capabilities, competition/product availability, logistic supply lines, and costs.12 Ophthalmologists must also recognize that the carbon footprint of their specialty contributes to climate change to the detriment of their patients.
AN EMERGENCY AND AN OPPORTUNITY
Ophthalmologists are working to mitigate and adapt to the health threats posed by climate change. The International Agency for the Prevention of Blindness Climate Action Working Group has released a Call to Action and a Guide for Environmentally Sustainable Practices in the Eye Care Sector (Figure).13 In North America, the Ophthalmic Instrument Cleaning and Sterilization and OR Waste Task Force, which is cochaired by David F. Chang, MD, and Cathleen M. McCabe, MD, has representatives from multiple organizations. Its goal is to advocate on behalf of constituent society members for the reduction of needless surgical waste. (For more on the Ophthalmic Instrument Cleaning and Sterilization and OR Waste Task Force, see “Environmentally Sustainable Practices in the Eye Health Sector.”).
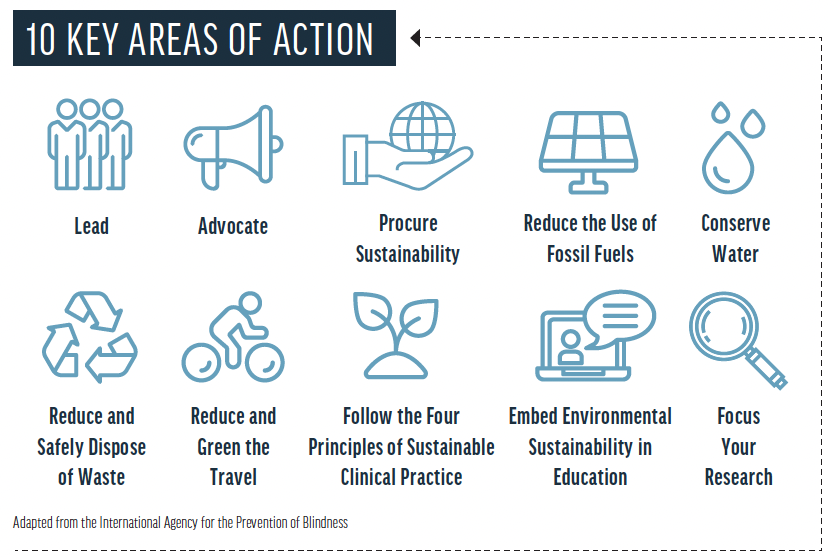
Figure. The International Agency for the Prevention of Blindness Climate Action Working Group’s 10 key areas of action to address climate change.
Medical Society Consortium on Climate and Health. The AAO and ASCRS have joined the Medical Society Consortium on Climate and Health. The mission of the Consortium, launched in 2016, is to organize, empower, mobilize, and amplify the voices of US doctors. In partnership with public health experts and fellow health professionals, the Consortium advocates for equitable climate solutions that protect and promote the health of all people. Membership in the organization has grown rapidly to include 36 national medical societies, representing well over 600,000 physicians—more than 60% of US doctors. The Consortium partners with 61 organizations from across the spectrum of health care and public health. The organization has developed a variety of resources to help inform the public about climate change and its impact on health and to provide physicians and other health professionals with useful tools such as posters on the health benefits of climate action, advocacy guides, and Health Voices for Climate Action videos.
Trusted health professionals can be highly effective at conveying the message that climate change is real, that it is harming public health, and that climate solutions can benefit public health. The Consortium trains advocates who visit Congressional Representatives to share data and stories about climate change and health. The US Call to Action on Climate, Health & Equity: A Policy Action Agenda is endorsed by 168 organizations and schools of medicine, nursing, and public health as well as 500 hospitals.14
A commitment to do no harm. The US health care system contributes more than 10% of US greenhouse gas emissions and is responsible for one quarter of all global health care greenhouse gas emissions, which is more than the health care system of any other nation.15 Seventy-one percent of the cataract surgery carbon footprint is from the supply chain.16 Sustainable procurement takes into consideration social and environmental impacts as well as increasing profit. Morris et al estimated that the carbon footprint of phacoemulsification in the United Kingdom is 30 times greater than that of the Aravind eye care system in India. At the same time, the endophthalmitis rate at Aravind is lower than in the United Kingdom and United States.17,18 Changing practices to release fewer greenhouse gases has the potential to decrease costs and improve the quality of care.19
CLIMATE SOLUTIONS ARE HEALTH SOLUTIONS
Climate solutions could rapidly improve public health and equity. Physicians have trusted voices in their communities. In order to “first, do no harm,” ophthalmologists have a duty to act to limit climate change and protect human health.
1. Allan RP, Arias PA, Berger S, et al. Climate change 2021: the physical science basis, the working group I contribution to the sixth assessment report. IPCC. August 7, 2021. Accessed September 10, 2021. https://www.ipcc.ch/report/ar6/wg1/downloads/report/IPCC_AR6_WGI_Full_Report.pdf
2. Climate change is the greatest threat to public health, top medical journals warn. NPR. September 7, 2021. Accessed September 10, 2021. https://www.npr.org/2021/09/07/1034670549/climate-change-is-the-greatest-threat-to-public-health-top-medical-journals-warn
3. Preparing for the regional health impacts of climate change in the United States. Centers for Disease Control. July 2020. Accessed September 10, 2021. https://www.cdc.gov/climateandhealth/docs/Health_Impacts_Climate_Change-508_final.pdf
4. Hong J, Zhong T, Li H, et al. Ambient air pollution, weather changes, and outpatient visits for allergic conjunctivitis: a retrospective registry study. Sci Rep. 2016; 6:23858.
5. Das A, Basu S. Environmental and air pollution factors affecting allergic eye disease in children and adolescents in India. Int J Environ Res Public Health. 2021;18(11):5611.
6. Anderson JG, Wilmouth DM, Smith JB, Sayres DS. UV dosage levels in summer: increased risk of ozone loss from convectively injected water vapor. Science. 2021;337(6096):835-839.
7. Johnson GJ. The environment and the eye. Eye (Lond). 2004;18(12):1235-1250.
8. Jaggernath Jyoti, Naido KS. Climate change: impact of increased ultraviolet radiation and water changes on eye health. Health. 2013;05:921-930.
9. Schraufnagel DE, Balmes, JR, Cowl CT, et al. Air pollution and noncommunicable diseases: a review by the forum of international respiratory societies’ environmental committee, part 2: air pollution and organ systems. Chest. 2019;155(2):417-426.
10. Chua Syl, Warwick A, Peto Tunde, et al. Association of ambient air pollution with age-related macular degeneration and retinal thickness in UK Biobank. Br J Ophthalmol. Published online January 25, 2021. doi: 10.1136/bjophthalmol-2020-316218
11. Chua S, Khawaja AP, Morgan J, et al. The relationship between ambient atmospheric fine particulate matter (PM2.5) and glaucoma in a large community cohort. Invest Ophthalmol Vis Sci. 2019;60(14):4915-4923.
12. Mazer-Amirshahi M, Fox ER. Saline shortages – many causes, no simple solution. N Engl J Med. 2018;378(16):1472-1474.
13. Call to action and a guide for environmentally sustainable practices in the eye care sector. International Agency for the Prevention of Blindness. Accessed September 10, 2021. https://www.iapb.org/wp-content/uploads/2021/04/IAPB_CAWG_CTA-document.pdf
14. US Call to Action on Climate, Health, and Equity: A Policy Action Agenda. Climate Health Action. 2019. Accessed September 10, 2021. https://climatehealthaction.org
15. Eckelman M, Huang K, Lagasse R, Senay E, Dubrow R, Sherman JD. Health care pollution and public health damage in the United States: an update. Health Aff (Millwood). 2020;39(12):2071-2079.
16. Sherman J, Slutzman J, Thiel C. Clinical sustainability: environmental stewardship at the bedside. Presented at: Clean Med Virtual Series; October 29, 2020; online.
17. Morris DS, Wright T, Somner JEA, Connor A. The carbon footprint of cataract surgery. Eye (Lond). 2013;27(4):495-501.
18. Thiel CL, Schehlein E, Ravilla T, et al. Cataract surgery and environmental sustainability: waste and lifecycle assessment of phacoemulsification at a private healthcare facility. J Cataract Refract Surg. 2017;43(11):1391-1398.
19. My Green Doctor. Ten reasons to go green. Accessed September 21, 2021. https://mygreendoctor.org/welcome-to-my-green-doctor/ten-reasons-to-go-green



