
Refractive surgery has become massively popular worldwide. Laser vision correction (LVC) is an excellent option for the management of myopia, astigmatism, and hyperopia—particularly for individuals who have not yet developed presbyopia. Most of these patients achieve 20/20 UCVA after LVC. This group of procedures can also achieve similar uncorrected distance visual acuity (UDVA) for patients with presbyopia. The lack of excellent uncorrected near visual acuity after the refractive correction of presbyopia, however, is challenging in this population.
THE GRAVEYARD AND THE CURRENT LANDSCAPE
Failed methods of correction. Occasionally, refractive surgery procedures that hold promise initially for hyperopia and presbyopia are abandoned. Some examples include conductive keratoplasty and laser thermokeratoplasty, which surgeons stopped performing because patients experienced full regression of the procedures’ refractive effects, and the Raindrop Near Vision Inlay, which was withdrawn from the market because of an unacceptably high incidence of corneal haze and melting.
Current landscape: Laser vision correction. LVC can be a viable option for hyperopia correction for young individuals (40–60 years of age) with presbyopia. Lenticule extraction may also be an option in the future, if it becomes an approved indication (see Read It Now). For patients with presbyopia who are 50 years of age or older, lens replacement surgery is becoming an increasingly popular strategy owing to advances in IOL technology.
READ IT NOW
Related Content From the CRST Archives
Dan Z. Reinstein, MD, MA(Cantab), FRCSC, DABO, FRCOphth, FEBO, shares a review of research on SMILE for hyperopia.
The most challenging patients in my practice continue to be 40- to 52-year-olds with low hyperopia and presbyopia. These patients present to my clinic regularly in search of spectacle independence, especially for near visual activities. They often find it hard to understand the concept of presbyopia and why their vision has changed suddenly, the differences in the optical correction required for distance versus near visual acuity, and the progressive nature of presbyopia.
When monovision is a successful strategy for these individuals, LVC may be an appropriate option. Depending on their professional and leisure activities, some patients may do well with full bilateral refractive correction with LVC. The transition from using a mechanical microkeratome to a femtosecond laser to create the LASIK flap and improvements in excimer laser ablation profiles generally provide superior optical results, better UDVA, more stable postoperative refractions, and less regression of effect than was achieved in the early days of LVC.
Current landscape: Lens replacement surgery. Unless they have high hyperopia (> +5.00 D) or a smaller amount of hyperopia with shallow anterior chambers and 20/40 or worse UDVA, I tend to avoid lens replacement surgery for individuals who are 55 years old or younger. My choice of IOL depends on the patient’s lifestyle and occupation, corneal asphericity, pupil size, angle kappa, and chord mu (see Dr. Chayet’s General Approach to Lens Replacement Surgery).
Dr. Chayet’s General Approach to Lens Replacement Surgery
Treatment should be based on the patient’s lifestyle and occupation, corneal asphericity, pupil size, angle kappa, and chord mu.
- Patient lifestyle/occupation: Complete spectacle independence
Solution: Trifocal IOLs - Patient lifestyle/occupation: Good UDVA (if willing to wear +1.25 D readers to view very small print)
Solution: Light Adjustable Lens (LAL, RxSight; Figure) with extended depth of focus technology - Pupil size: Small photopic pupils
Solution: LAL with a blended vision strategy; avoid multifocal, trifocal, and extended depth of focus IOLs in this population - Chord mu: Greater than 0.4
Solution: LAL, trifocal IOL, or new-technology monofocal IOL for patients who cannot be available for the laser procedures required with the LAL or who cannot afford this lens or a trifocal IOL
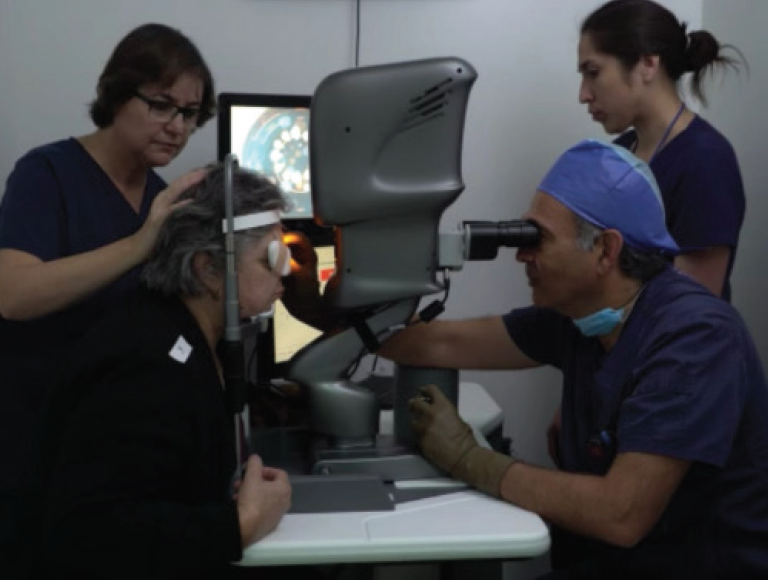
Figure. Light treatment with the LAL.
ON THE HORIZON
Like many of my colleagues, I anxiously await the availability of new accommodating IOL designs. I have participated in several clinical trials for accommodating IOLs, including the Juvene IOL (LensGen; Figure 1). This multipiece IOL has two components—(1) a base lens that fills the capsule and thus should provide greater vitreous stability and reduce the formation of posterior capsular opacification and (2) a fluid-filled lens that fits into the base lens and mimics the crystalline lens (ie, offers accommodation). One benefit of this technology is the potential for interchangeability, as the main power lens can be removed and exchanged, even many years after implantation.
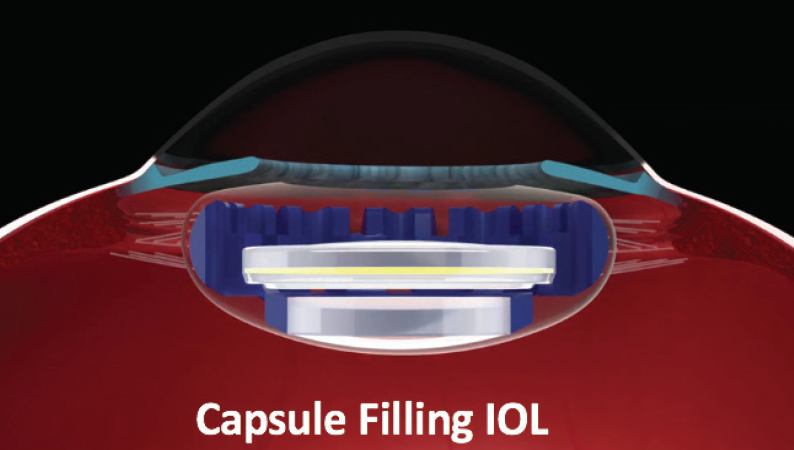
Figure 1. Placement of the Juvene IOL.
I have also participated in studies of the shape-changing Opira AIOL (ForSight Vision6; Figure 2). The main advantage of this lens is that it does not depend on capsular bag fibrosis because it is implanted in the sulcus outside the capsular bag and therefore does not affect accommodation. To achieve stability, two wings on the IOL are captured behind the capsulorhexis.

Figure 2. The Opira AIOL.
Both of these IOLs have provided excellent uncorrected distance, intermediate, and near visual acuity thus far in clinical trials. Other IOLs like the Omega Refractive Capsule (Omega Ophthalmics), a 3D implant that can hold any lens with a traditional C-arm haptic and keeps the capsular bag open to allow easy exchange of any IOL, are also on the horizon.
CONCLUSION
Twenty years after the approval of the excimer laser for the correction of hyperopia, LASIK remains a viable procedure for the treatment of low to moderate hyperopia, whereas several other refractive surgery procedures have been abandoned. As IOLs continue to evolve, the popularity and public acceptance of lens replacement surgery for presbyopia correction continue to grow. New treatments and lens technologies for refractive correction are on the horizon, and they hold much promise.
There is no question in my mind that now is a great time to be a refractive surgeon.


