Monofocal IOLs
P. Dee Stephenson, MD, FACS

It is sometimes surprisingly difficult to pick the most appropriate lens for a patient. Many options are available—some with negative aberrations, some with positive aberrations, and some that are aberration-free (aspheric). The postoperative quality of vision attained makes IOL selection worth the hard work it requires.
The average spherical aberration of the anterior corneal surface is +0.27 µm. I achieve the best results for patients when the cornea has positive aberrations postoperatively. I believe that IOL material matters. Some IOLs have glistenings, some have ridges on the optic edge, and some rotate more than others. I have used almost every IOL platform, mixed and matched many of them, and have found the most success with monofocal IOLs—specifically, the enVista aspheric IOL and the enVista aspheric monofocal toric IOL (Bausch + Lomb).
A Strong Preference
The enVista lenses have the same power from their center to their edge, and they induce no spherical aberrations. In my hands, these IOLs are forgiving, with little in the way of dysphotopsias and increased depth of field postoperatively. In my practice, 86.4% of patients who have received these IOLs have achieved postoperative uncorrected intermediate visual acuity of 20/40 or better, and they have been able to use handheld devices and perform some near-vision tasks without glasses (Figure 1A). They have some uncorrected near visual acuity as well (Figure 1B). Because patients retain consistent uncorrected distance visual acuity across a wide range of manifest refraction spherical equivalent, they tolerate defocus well (Figure 2). In my experience, the enVista aspheric monofocal toric IOL is also a great choice for patients with aberrated corneas because this lens does not induce spherical aberration and offers a large range of cylinder correction (+0.77 to +4.53 D).
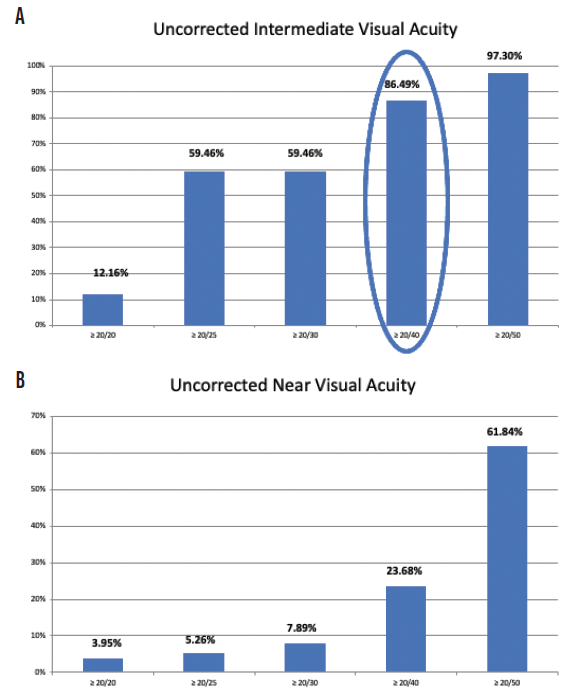
Figure 1. Postoperative uncorrected intermediate visual acuity (A) and postoperative uncorrected near visual acuity (B) among patients who received an enVista monofocal toric IOL in Dr. Stephenson’s practice.
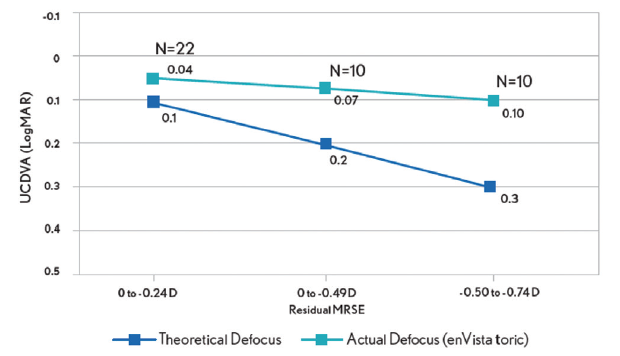
Figure 2. Postoperative tolerance of defocus among patients who received an enVista monofocal toric IOL in Dr. Stephenson’s practice.
When I compared my results with low-add toric IOLs and monofocal lenses, I found that using the former improved clinical outcomes and patient satisfaction and expanded the treatment options for cataract patients with a low amount of corneal astigmatism (Figure 3).
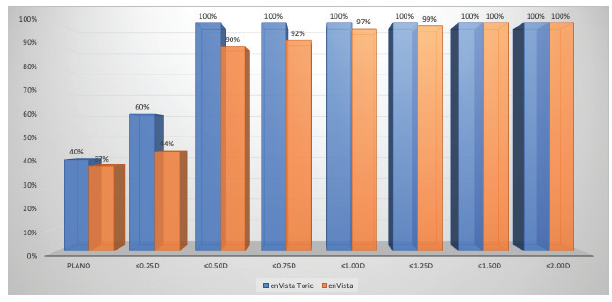
Figure 3. Dr. Stephenson’s comparison of postoperative refractive astigmatism in cataract patients with a low amount of corneal astigmatism after the implantation of an enVista toric IOL versus an enVista monofocal IOL.
Figures 1–3 courtesy of P. Dee Stephenson, MD, FACS
Conclusion
I work hard to optimize my surgical outcomes, honing my surgical skills and preoperative workups and doing everything from correcting dry eye disease and identifying preexisting ocular surface to addressing retinal disease. Monofocal IOLs, specifically the enVista aspheric and monofocal toric IOLs, allow me to enhance my patients’ lives with stable, predictable outcomes and great quality of vision.
EDOF Blended Vision
Detlev R.H. Breyer, MD, PhD; Lena Beckers, MD; and David Lücht



The standard procedure to treat cataract patients is currently to replace the crystalline lens with a monofocal posterior chamber IOL. Patients must decide preoperatively whether they prioritize good near, intermediate, or distance vision postoperatively. Over the past few years, numerous IOLs designed according to different optical principles have been developed to provide spectacle independence after lens surgery (Figure 4). Only 1% to 5% of patients, even in western industrialized countries, receive this advanced customized premium treatment from their surgeons.
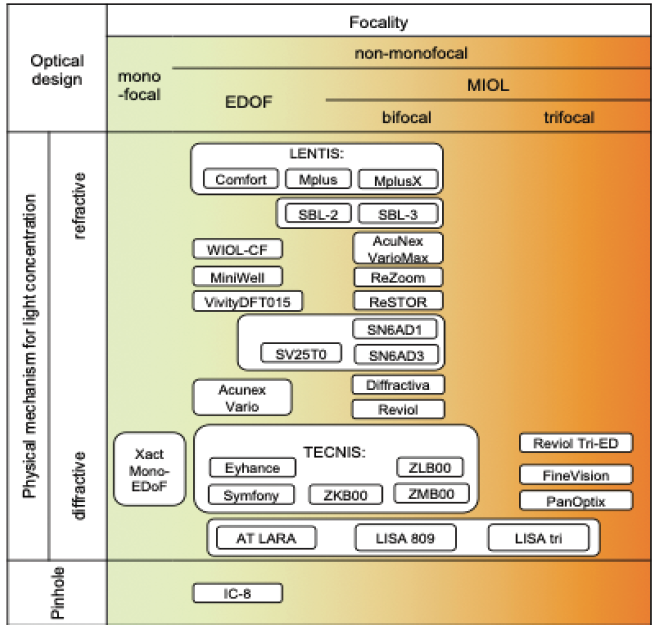
Figure 4. The most commonly used IOLs (organized by focality and optical design).
The Players: Advanced Optics for Spectacle Independence
Multifocal IOLs feature either refractive or diffractive optics and vary on the optical physics of how light is distributed and centered on the retina. Refractive IOLs function similarly to the natural lens by bending light once.
Another way to classify the optic of an IOL is by its focality. If the lens provides a single focal point, it is categorized as a monofocal. If the lens provides two or more focal points, it is categorized as a multifocal. Bifocal IOLs have two focal points, and trifocal IOLs have three focal points. An extended depth of focus (EDOF) IOL has a longitudinally extended focal point.
The term multifocal lens is also often applied to EDOF IOLs. The AAO defines the depth of focus as the range at which the lens provides a mean acuity of at least 0.2 logMAR. We, however, agree with the scientific interpretation of Damien Gatinel, MD, PhD, that the IC-8 IOL (AcuFocus) is the only true EDOF IOL.1
Unavoidable Optical Side Effects With Multifocal IOLs
When counseling patients, the preoperative discussion of multifocal IOLs must address optical side effects such as photopic phenomena, reduced contrast sensitivity, changes to light distribution, and waxy vision. When light passes through a multifocal IOL, various mechanisms can disturb its distribution on the retina (Figures 5 and 6). Halos and glare are the most common forms of dysphotopsia. In general, photopic phenomena are more common and severe with diffractive than refractive optics. The Zernike decompensation defocus corresponds mathematically to the Zernike term Z(2,0) of the wavefront error. Higher-order aberrations include coefficients Z(n,m) with n greater than 2, such as coma Z(3,±1) or spherical aberrations Z(4,0). They can be important contributors to the presence of halos postoperatively. In our experience, halos are an inevitable side effect of multifocal and EDOF IOLs and increase with higher near addition powers.2,3
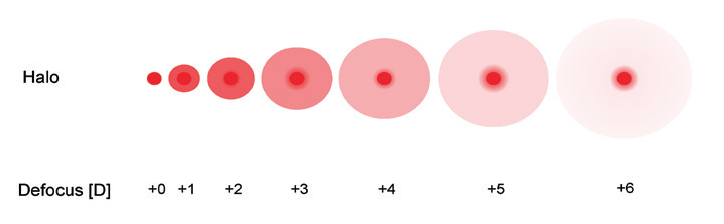
Figure 5. The intensity of IOL-induced halos increases with higher near additions of the optic.
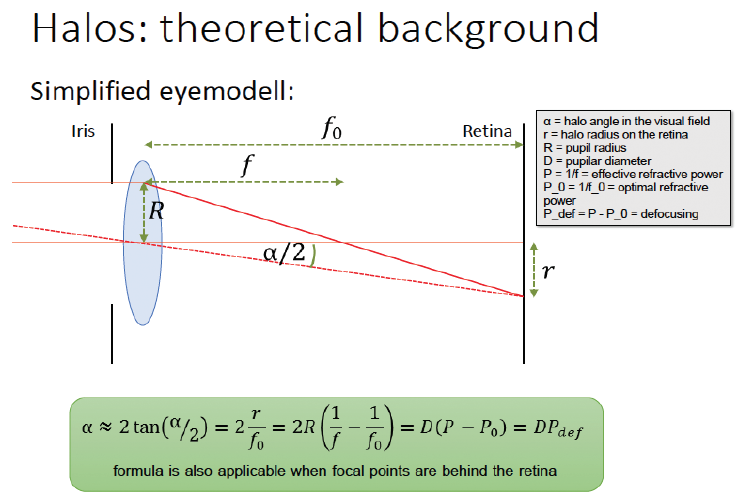
Figure 6. A simplified eye model to describe the theoretical background of halos.
On the other hand, a high degree of spectacle independence can be achieved with multifocal IOLs. Compared with monofocal optics, disadvantages of IOLs that feature diffractive and refractive optics include halos, glare, and reduced light transmission. Multifocal IOLs decrease contrast sensitivity and therefore impair vision under mesopic conditions.
The postoperative refractive error should not exceed 0.50 D of astigmatism and sphere. A refractive enhancement may be required to achieve this result.
Mix-and-Match and Blended Vision Strategies for Even Better Clinical Outcomes
When multifocal IOLs are implanted bilaterally, different lens types (ie, refractive and diffractive designs) and near addition powers (+1.50 to +2.00 D and +3.00 to +4.00 D) can be combined to achieve better binocular visual outcomes (Figures 7 and 8). This mix-and-match or blended vision approach can provide greater spectacle independence and less severe dysphotopsias than the bilateral implantation of one type of multifocal IOL with a high near add power (Figures 9 and 10).4,5
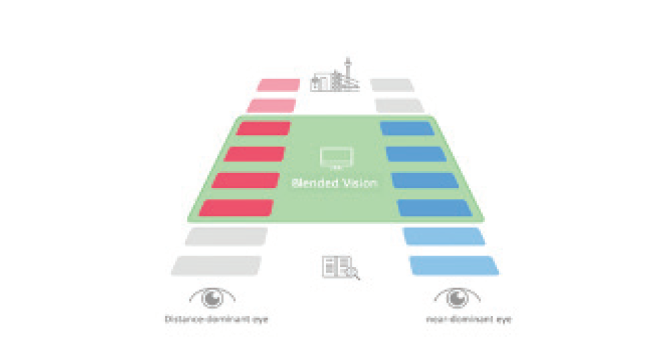
Figure 7. Blended vision according to the Düsseldorf formula shortens neural adaptation time.
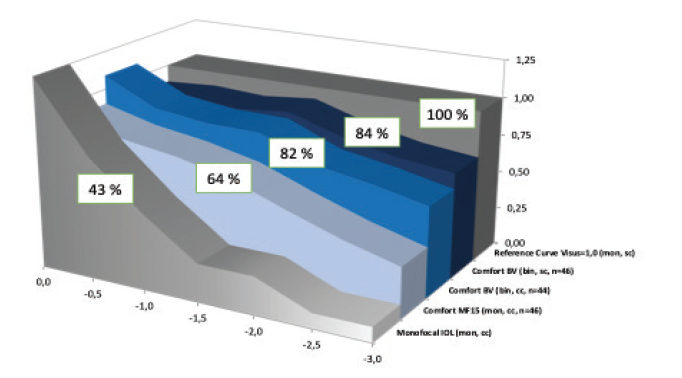
Figure 8. Defocus curve of the Düsseldorf formula, a comfortable way to offer a high range of spectacle independence with a minor increase in photopic phenomena.
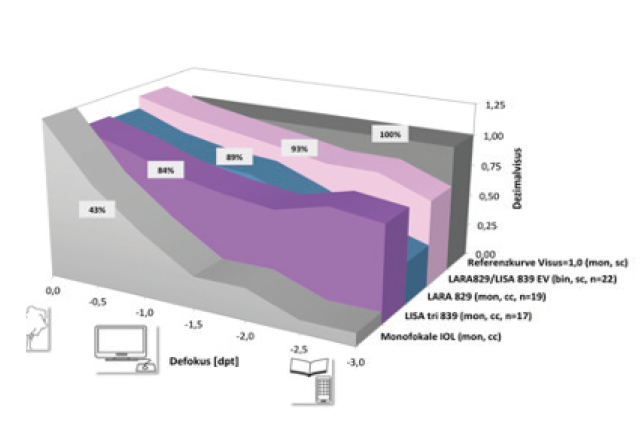
Figure 9. Defocus curves of diffractive blended vision.
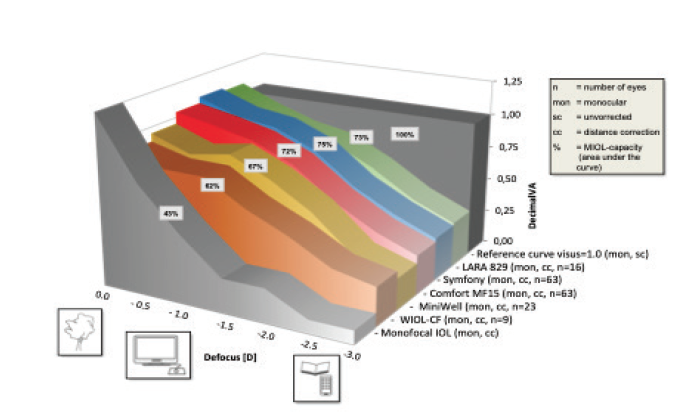
Figure 10. Defocus curves for various EDOF IOLs.
Customized Surgery
When deciding which IOL to implant, it is important to consider the patient’s visual needs, including their occupation and leisure activities. Often underestimated and of even greater importance is knowing the extent to which a patient is willing to accept optical side effects such as photopic phenomena. A knowledge of defocus curves and lens design capacities and halo and glare incidence and gravity is mandatory for every refractive surgeon, and this information has to be made understandable to the patient (Figure 11).

Figure 11. The preoperative use of display boards is important when explaining the possible side effects of multifocal IOLs to patients.
Figures 4–11 courtesy of Detlev R.H. Breyer, MD, PhD
If the patient cannot tolerate halos and glare and is willing to accept glasses for reading, micromonovision of -0.75 D anisometropia is another option. In our experience, patients who do not tolerate photopic phenomena may achieve a high rate of spectacle independence with a refractive low-add EDOF IOL such as the Lentis Comfort, MF15, or Acunex Vario (all from Teleon Surgical) with a blended vision strategy. We have created a technique called the Düsseldorf Strategy. In general, these patients have a continuous broad range of vision from far to near, excluding small print reading, and report photopic phenomena comparable to in the general population.
We are currently studying this EDOF blended vision model with the AcrySof IQ Vivity EDOF IOL (Alcon). The results are promising and close to the Düsseldorf strategy with the Lentis Comfort EDOF IOL.
1. Rampat R, Gatinel D. Multifocal and extended depth-of-focus intraocular lenses in 2020. Ophthalmology. 2020;S0161-6420(20)30931-30933.
2. Breyer DRH, Kaymak H, Ax T, Kretz FTA, Auffarth GU, Hagen PR. Intraocular lenses and extended depth of focus intraocular lenses. Asia Pac J Ophthalmol (Phila). 2017;6(4):339-349.
3. Breyer DRH, Hagen PR. Monovision vs. Multifokallinsen-Pro und Contra. DOC Nürnberg: International Congress of German Ophthalmic Surgeons. 2019.
4. Tarib I, Kasier I, Herbers C, et al. Comparison of visual outcomes and patient satisfaction after bilateral implantation of an EDOF IOL and a mix-and-match approach. J Refract Surg. 2019;35(7):408-416.
5. Kretz FTA, Tarib I, Teisch S, et al. Clinical evaluation of a novel intraocular lens with enhanced depth of focus (EDOF) to increase visual acuity for intermediate distances. Klin Monbl Augenheilkd. 2018;235(8):874-880.
Multifocal IOLs
By Hirotaka Tanabe, MD, PhD

There are three basic representative design concepts for IOLs: monofocal, multifocal, and EDOF. Multifocal IOLs provide not only good distance and near functional vision but also intermediate vision without the use of corrective lenses in new types of IOLs with more than two foci or EDOF mixtures. Currently, for this and several reasons described herein, multifocal and EDOF lenses are my preference for a majority of patients, but I consider a broad range of factors when customizing IOL selection to each patient.
Rarely Used in Japan to Date
Concerns remain about compromised contrast sensitivity and problems driving at night because of unwanted subjective phenomena (halos, glares, and/or starbursts) associated with multifocal IOLs. These disturbances may affect the patient’s visual performance and overall postoperative satisfaction. These are several reasons that, in Japan, many doctors and patients are unlikely to choose a multifocal lens. National surveys from 2019 and 2020 reported that the rates of multifocal and EDOF IOL use in cataract surgery were just 3.9% and 5.1%, respectively.2,3
Moreover, as of this writing, multifocal and EDOF IOLs are not supported by the regular national medical insurance in Japan (with the exception of the Lentis Comfort LS-313 MF15 and Lentis Comfort Toric LS-313 MF15 T1-3; Figure 12). The advanced medical insurance services that provided insurance contractors with full financial support through insurance companies to use the registered multifocal and EDOF IOLs ended in March 2020. Thus, there are financial barriers to the use of these IOLs.
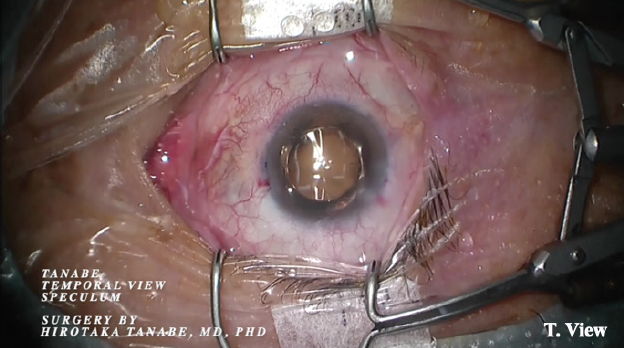
Figure 12. Lentis Comfort Toric LS-313 MF15 T1 IOL at cataract surgery. The eye is held open with the Tanabe Temporal View Speculum (Eye Technology [UK] and M.E. Technica [Japan]) to achieve a maximum view of the temporal surgical field.
Figure 12 courtesy of M.E. Technica
Monofocal Versus Multifocal: Comparing Postoperative Visual Performance
A large-scale retrospective study conducted at Tsukazaki Hospital and based on approximately a decade of practice from December 13, 2010, to July 29, 2019, compared visual performance with a monofocal and a multifocal IOL made of the same material and using the same basic design, the ZCB00 and ZMB00 models, respectively, of the Tecnis IOL (Johnson & Johnson Vision).1 Over the course of approximately 10 years, 904 eyes of 452 patients received the monofocal lens, and 1,326 eyes of 663 patients received the multifocal lens.
Contrast sensitivity (4.0º, 2.5º, 1.6º, 1.0º, 0.7º), contrast sensitivity with glare (1.6º, 1.0º, 0.7º), and the National Eye Institute Visual Function Questionnaire-25 (NEI VFQ-25) score for driving at night were significantly better in the monofocal group (P < .00068, Wald test), as were the NEI VFQ-25 scores for mental health, driving in general, driving during the day, and driving under adverse conditions (P < .05, Wald test). Uncorrected intermediate visual acuity, uncorrected near visual acuity, and spectacle independence at near were significantly better in the multifocal group (P < .00068, Wald test), as were the NEI VFQ-25 scores for general health and spectacle independence at distance (P < .05, Wald test).1
EDOF IOLs
Although EDOF IOLs were developed to overcome the drawbacks of mono- and multifocal IOLs, in most cases, the rate of spectacle independence with EDOF IOLs is lower than in patients who receive multifocal IOLs. The Lentis Comfort IOLs are rotationally asymmetric IOLs with a refractive design, combining an aspheric aberration-free distance vision zone with a sector-shaped near vision zone with +1.50 D added power in the IOL plane (+1.06 D in the corneal plane).4
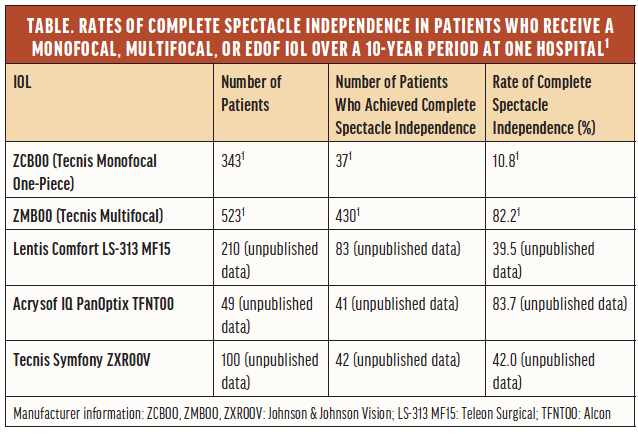
Unpublished data from a retrospective comparison of the postoperative visual performance with the Lentis Comfort LS-313 MF15 and with monofocal (Tecnis Monofocal ZCB00, Johnson & Johnson Vision), bifocal multifocal (Tecnis Multifocal ZMB00, Johnson & Johnson Vision), trifocal multifocal (AcrySof IQ PanOptix, Alcon), and EDOF IOLs (Tecnis Symfony ZXR00V, Johnson & Johnson Vision) in patients operated on over a 10-year period at Tsukazaki Hospital indicated not only that the Lentis Comfort IOLs were associated with greater higher-order aberrations but also that the lenses provided high contrast sensitivity with and without glare and high VFQ-25 scores for driving at night or driving under adverse conditions. Because the Lentis Comfort LS-313 MF15 has a mild added power that helps suppress light scattering, the rate of postoperative spectacle independence in this group was lower than in the bifocal and trifocal multifocal IOL groups (postoperative spectacle independence rates for each IOL included in the study are included in the Table).
Conclusion
Many reports have demonstrated that the most unsatisfactory subjective phenomena experienced by patients who receive multifocal IOLs result from factors unrelated to the lens itself. For patients who wish to be completely spectacle independent without monovision postoperatively, opting for multifocals or employing a mix-and-match approach is, in most cases, the best option at this time.
1. Tanabe H, Tabuchi H, Shojo T, Yamauchi T, Takase K. Comparison of visual performance between monofocal and multifocal intraocular lenses of the same material and basic design. Sci Rep. 2020; 10:15490.
2. Sato M, Kamiya K, Kojima T, et al. Clinical survey of the Japanese society of cataract and refractive surgery. IOL&RS. 2019;33:453–473.
3. Sato M, Kamiya K, Kojima T, et al. Clinical survey of the Japanese society of cataract and refractive surgery. IOL&RS. 2020;34:412-432.
4. Oshika T, Arai H, Fujita Y, et al. One-year clinical evaluation of rotationally asymmetric multifocalfocal intraocular lens with +1.5 diopters near addition. Sci Rep. 2019;9:13117.
QR codes make accessing digital exclusive content easier than ever. Simply open your smartphone’s camera, aim it at a code like the one below, and view your content.
Try it now!




