
What is your overall impression of the OPD-Scan III?
For me, the OPD-Scan III is a must-have for refractive corneal and lens surgery because the device collects a considerable amount of data from the optical system of each eye. Finding the software useful but too complicated, I collaborated with Nidek over a period of 18 months to produce a new report, the Daya Overview, which I explain below.
I incorporate the OPD-Scan III into every patient visit, and, at this stage, I would be lost without the information it provides.
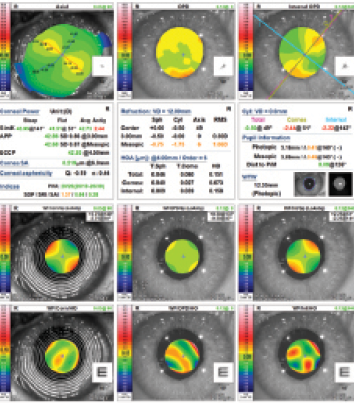
Figure 1. The Daya Overview assists the surgeon in understanding the eye’s optics.
How do you use the OPD-Scan III in clinical practice?
Collectively, the Daya Overview provides useful information to the refractive surgeon in terms of surgical planning, patient counseling, and postoperative evaluation. It divides information into three columns: Overall OPD data and aberrations are placed in the central column, corneal information in the left-hand column, and internal data in the right-hand column (Figure 1). In this manner, the portrayal of qualitative data can assist the surgeon in understanding the eye’s optics—including the influence of the cornea and internal structures (lens or corneal back surface)—at a glance. Quantitative data including refractive, keratometric, visually significant higher-order aberrations (coma and spherical aberration), and pupillometry can then be evaluated in more detail. Specific areas in which information is provided at a glance include the following:
Corneal versus lenticular astigmatism. Corneal and internal (combined lenticular and back surface cornea) components indicate each individual axis: corneal, internal, and total. This is useful when planning cataract surgery with toric IOLs.
Choosing the correct astigmatic axis with wavefront-derived data. Wavefront-derived astigmatism data (Zernike S2) are provided for the overall eye, cornea, and internal components. This information is particularly useful in corneas that have nonorthogonal astigmatism or an asymmetric bowtie (eg, forme fruste keratoconus). Internal wavefront astigmatic information is useful for verifying correct toric IOL alignment postoperatively, and there is no need for pupil dilation.
Pupil information. Pupil size and deviation of the visual axis from the pupil center are also displayed. This is useful for laser refractive surgery and, in particular, lens surgery when the magnitude and direction of lens decentration must be determined during surgery.
Point spread function (PSF) and simulated E. The overall, corneal, and internal PSFs and simulated E help the surgeon to objectively evaluate visual quality and the source of a visual problem (eg, dysfunctional lens syndrome; DLS). The term DLS is gaining traction in ophthalmology to describe a crystalline lens that may not yet be cataractous but is causing visual problems for the patient; the Daya Overview provides useful information to document this condition.
What are the advantages of the OPD-Scan III compared with other ocular biometry technologies?
Only two other devices, to the best of my knowledge, provide the same type of information: the KR1W (Topcon) and iTrace (Tracey Technologies). I also have these devices in my practice, and I find the OPD-Scan III with the new report much more useful.
Sheraz M. Daya, MD, FACP, FACS, FRCS(Ed), FRCOphth
• Director and Consultant Surgeon, Centre for Sight, East Grinstead, United Kingdom
• Chief Medical Editor, CRST Europe
• sdaya@centreforsight.com
• FFinancial disclosure: Consultant (Nidek)

