
This article describes a technique for implanting a foldable IOL in an eye with a large zonular dehiscence. This procedure can be helpful in eyes with ectopia lentis for any number of reasons, such as blunt trauma, Marfan syndrome, or Weill-Marchesani syndrome. The photos that accompany this article are from surgery on a patient who had experienced blunt trauma to the eye, resulting in a 180° zonular tear and posterior synechiae; however, the same technique would also work well in eyes with zonular dehiscence due to other causes.
POSSIBLE APPROACHES
Cataract surgery and IOL implantation in the presence of a subluxated lens with a large zonular dehiscence lends itself to a few possibilities, and a variety of methods have been described.1-8 The cataract can be removed by an intracapsular technique through a 150° limbal incision using a tumbling technique and a vectis. Alternatively, if the lens is relatively soft, it can be consumed with a 23-gauge vitrector using a three-port pars plana vitrectomy approach. Alternatively, phacoemulsification through a small capsulorrhexis can be used to remove the lens while the capsular bag is supported with capsule or iris hooks or a sutured-in Cionni capsular tension ring (Cionni CTR; Morcher).
After removal of the crystalline lens, the problem of IOL selection and fixation remains. If the capsular bag is sacrificed in an intracapsular method or inadvertently damaged during phacoemulsification, there are four options for implantation: (1) an anterior chamber IOL, (2) a posteriorly fixated iris-supported IOL, (3) a glued posterior chamber IOL, or (4) a posterior chamber IOL sutured into the sulcus or to the peripheral iris. If the bag is retained, an IOL can be sutured through the capsular bag itself, using what I have dubbed the bag-to-the-wall technique.
BAG-TO-THE-WALL TECHNIQUE
Following is a description of my personal technique for suturing a posterior chamber IOL through the capsular bag in eyes with extreme subluxation of the crystalline lens such as occurs in Marfan syndrome or after ocular trauma.
Anesthesia. Typically I use topical anesthesia consisting of 2% lidocaine jelly (Oculan; Sunways India Pvt) applied for 5 minutes before surgery begins. This is supplemented by intracameral 1% nonpreserved lidocaine in a 50/50 dilution with balanced saline solution.
At a Glance
• The bag-to-the-wall technique can be helpful in eyes with ectopia lentis for any number of reasons, such as blunt trauma, Marfan syndrome, or Weill-Marchesani syndrome.
• A small rhexis as central as possible is the cornerstone of this procedure.
• Because the technique is essentially an assisted in-thebag implantation, the lens is very stable. As a result, iris chafing and lens tilt are not seen.
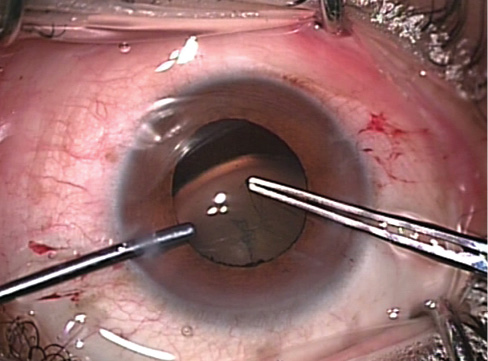
Figure 1. A sideport incision is created at the 8-o’clock position, opposite the area of maximum subluxation.
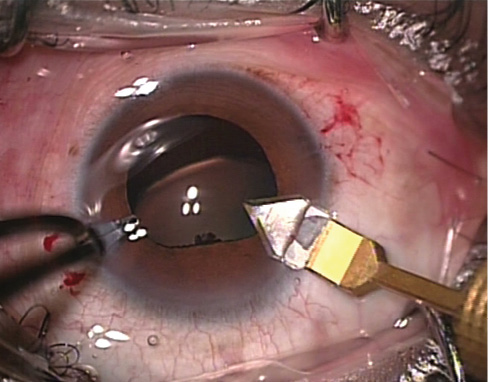
Figure 2. A clear corneal incision is created at the 10-o’clock position with a 2.5-mm diamond keratome.
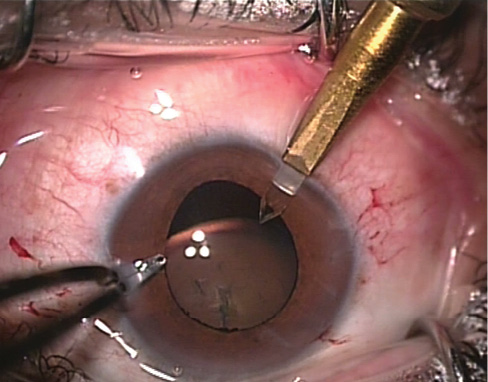
Figure 3. Posterior synechiae adhesions are swept with an iris repositor.
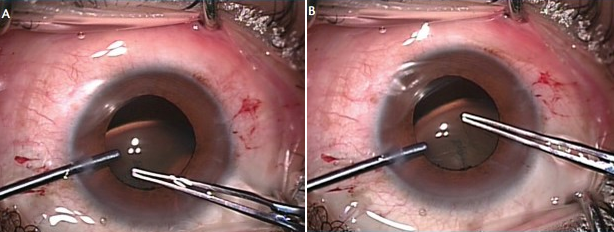
Figure 4. The capsulorrhexis is initiated by pinching with sharp forceps (A). The rhexis is extended around the lens capsule (B).
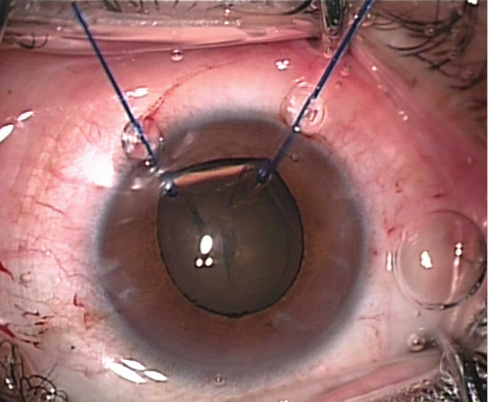
Figure 5. The capsular bag is supported by two iris hooks.
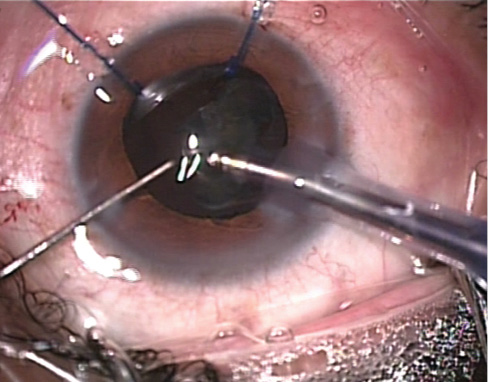
Figure 6. Phacoemulsification is performed with torsional energy and reduced vacuum.
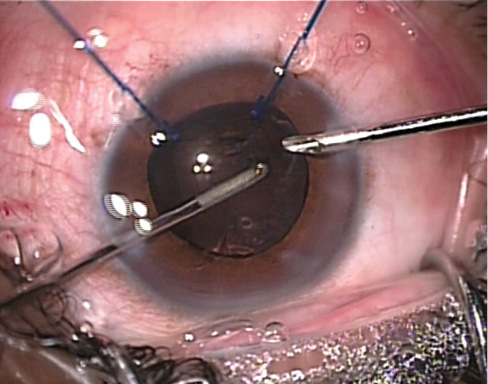
Figure 7. Bimanual irrigation and aspiration is performed carefully because of the loose zonules.
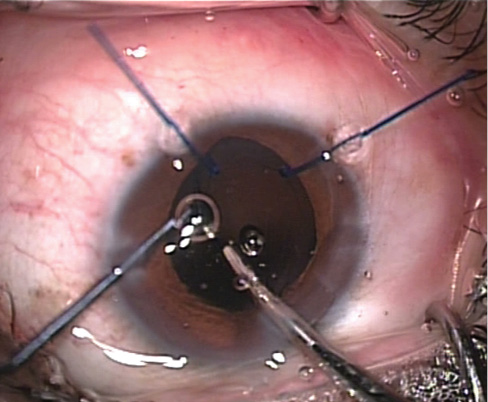
Figure 8. The CTR is injected.
Incision creation. Two stab incisions are created first, at 90° and 180°, with a 0.9-mm diamond keratome (Meyco). The eye is tightened by injecting a moderate quantity of OVD (Viscoat; Alcon). Then two more stab incisions are created at the 4- and 8-o’clock positions (Figure 1). Finally, a 2.5-mm clear corneal tunnel is fashioned at the limbus at the 10-o’clock position with a diamond keratome (Figure 2), regardless of which eye is to be operated. Because I am right-handed, the tunnel is superotemporal for a right eye and superonasal for a left eye.
Capsulorrhexis. Before the capsulorrhexis is initiated, posterior synechiae can be swept out with an iris repositor (Figure 3). The rhexis is performed with thin-bladed, sharp-tipped forceps (Rumex; Figure 4). The rhexis should be located as centrally on the lens as possible. It should not be more than 4 mm in diameter.
Iris hook placement. Two flexible nylon iris retractors (IrisCare; Madhu Instruments Pvt) are inserted through the two inferior openings, hooking the capsular bag. The hooks are then retracted and fastened so that the capsular bag is centered (Figure 5).
Hydrodissection. This maneuver is performed with a standard hydrocannula on a 5-cc syringe with balanced saline solution. Typically, the nucleus levitates itself out of the bag as the rhexis is stretched open by the two iris hooks at one end.
Phacoemulsification. Nuclear disassembly is carried out with moderate bottle height to prevent the bag from slipping off the hooks. The nucleus is directly chopped into four fragments, and they are emulsified with the Ozil torsional handpiece (Alcon) and reduced vacuum (Figure 6). Bimanual irrigation and aspiration follows, during which the surgeon must be careful not to exert too much traction on the bag as the zonules are already weak (Figure 7).
CTR injection. Injection of the CTR is prefaced by inflating the anterior chamber carefully with OVD (Healon; Abbott Medical Optics). I use a PMMA CTR from Care Group India and a CTR injector from Epsilon Eyecare. The ring is first drawn up into the injector barrel, and the nozzle of the injector is inserted into the clear corneal tunnel. Then the CTR is injected in a clockwise manner in such a way that the open end of the ring rests at the 12-o’clock position and the bulk of the ring supports the weakest part of the bag (Figure 8).
IOL preparation and fixation. Lens power is calculated before surgery using the IOLMaster 500 (Carl Zeiss Meditec) and rechecked with immersion biometry. The lens I use is the one-piece foldable hydrophilic acrylic square-edged C-Flex IOL (Rayner Intraocular Lenses), which is supplied with a disposable injector. The A-constant is the same as would normally be required for in-the-bag implantation for this lens, in this case 118.0.
The free end of a 10-0 polypropylene suture on a 1-in straight needle is tied to the midpoint of the leading IOL haptic (Figure 9). It is tied three times, tight enough to prevent slippage. The needle is first passed down the barrel of the IOL injector cartridge (Figure 10). Then the lens, with the suture tied to the leading haptic, is bedded down behind it in the injector. Next, the needle is passed through the clear corneal tunnel into the posterior chamber, where it is passed through the fornix of the capsular bag at the 6-o’clock position (Figure 11) and exits the eye through sclera at the 6-o’clock position, about 3.5 mm behind the limbus (Figure 12). Before the needle exits, a conjunctival peritomy is performed over the exit location in the sclera.
The IOL injector is inserted into the corneal tunnel, and the lens is injected into the bag (Figure 13) and dialed into place. The suture is pulled, centering the lens and capsular bag, and the iris hooks can then be removed. The straight needle is then passed twice, in a Z formation, through the sclera (Figure 14), and a single knot is tied and buried in a groove in the sclera (Figure 15). Finally, the conjuctiva is glued back into place with fibrin glue (ReliSeal; Reliance Life Sciences), and the viscoelastic material is aspirated from the eye.
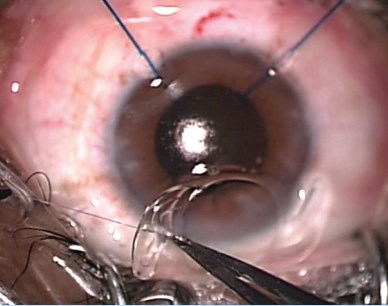
Figure 9. The free end of the polypropylene 10-0 suture is tied to the midpoint of the leading haptic.
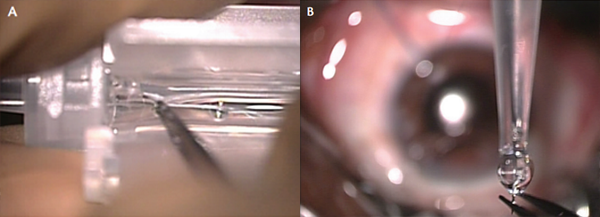
Figure 10. The needle is passed down the barrel of the injector (A). The needle exits the injector (B).
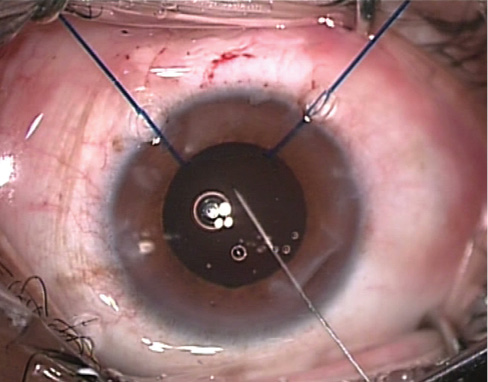
Figure 11. The needle passes through the scleral tunnel and then through the fornix of the capsular bag.
SURGICAL PEARLS
The steps described above are the basics of the bag-to-the-wall procedure for IOL implantation in eyes with compromised zonules. I leave you with seven pearls I have gathered in my clinical experience using this helpful technique.
Pearl No. 1: Do not overinflate the anterior chamber before putting in the iris hooks. Otherwise, the bag will be pushed back and the hooks will not engage the margin.
Pearl No. 2: If the lens is very subluxed and the capsular bag is poor, start the capsulorrhexis with a sharp needle. This is preferred to starting it by pinching with forceps.
Pearl No. 3: A small rhexis as central as possible is the cornerstone of this procedure. If the rhexis is large, the margin of anterior capsule will not be enough to stabilize the bag on the iris hooks. The bag will slip off the hooks and fall back every time the phaco tip infusion enters the eye. Make a small, central rhexis.
Pearl No. 4: Tie the knot securely to the midpoint of the leading haptic. Here the haptic is in the optimum position to support the capsular bag.
Pearl No. 5: Make sure the lens is centered before tying the knot on the sclera. If the lens is decentered and you tie the knot before checking its position, you will have to retie another suture to the leading haptic and pass the needle through again. Remember, the CTR only stabilizes the bag but does not center it.
Pearl No. 6: A streak of hyphema is common from the needle pass. It appears on the operating table but absorbs in 1 or 2 days.
Pearl No. 7: Because this is essentially an assisted in-the-bag implantation, the lens is very stable. As a result, iris chafing and lens tilt are not seen.
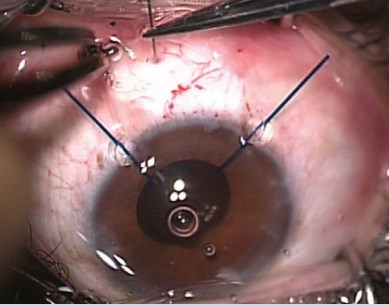
Figure 12. The needle passes through the pars plana and out through the sclera.
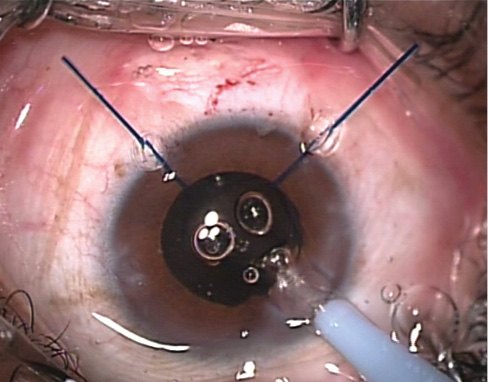
Figure 13. The IOL is injected into the capsular bag.
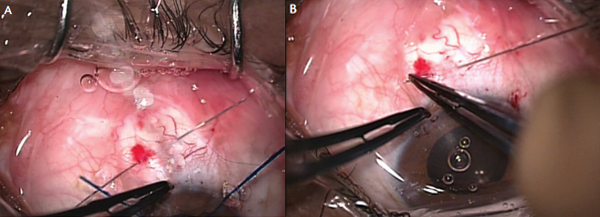
Figure 14. The needle is passed twice through sclera in a Z pattern (A). The iris hooks are removed and the suture locked by the second scleral pass (B).
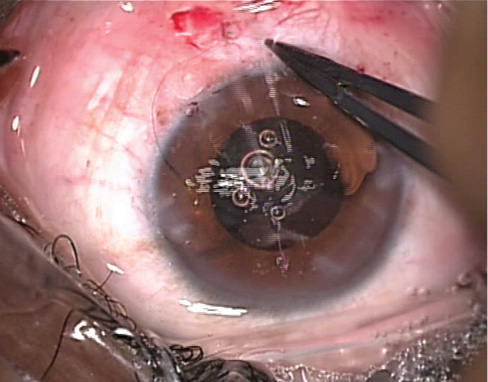
Figure 15. The suture is tied and the knot is buried in a groove.n
1. Kanski JJ. Closed intraocular microsurgery in ocular trauma. Trans Ophthalmol Soc UK. 1978; 98:51-54.
2. Peyman GA, Raichand M, Goldberg MF, Ritacca D. Management of subluxated and dislocated lenses with the vitrophage. Br J Ophthalmol. 1979;63:771-778.
3. Tsai Y-Y, Tseng S-H. Transscleral fixation of foldable intraocular lens after pars plana lensectomy in eyes with a subluxated lens. J Cataract Refract Surg. 1999;25:722-724.
4. Cionni RJ, Osher RH. Endocapsular ring approach to subluxed cataractous lens. J Cataract Refract Surg. 1995;21:245-249.
5. Novak J. Flexible iris hooks for phacoemulsification. J Cataract Refract Surg. 1997;23:828-831.
6. Hoffman RS, Fine IH, Packer M. Scleral fixation without conjunctival dissection. J Cataract Refract Surg. 2006;32:1907-1912.
7. Ton Y, Michaeli A, Assia EI. Repositioning and scleral fixation of the subluxated lens capsule using an intraocular anchoring device in experimental models. J Cataract Refract Surg. 2007;33:692-696.
8. Chen SX, Lee LR, Sii F, Rowley A. Modified cow-hitch suture fixation of transscleral sutured posterior chamber intraocular lenses: Long-term safety and efficacy. J Cataract Refract Surg. 2008;34:452-458.
Cyres Keiki Mehta, MS(Ophth), MCH(Ophth)
• Surgical Director and Chief, Dr. Cyres K. Mehta’s International Eye Centre, Mumbai, India
• CEO, ASSORT Surgical Management Systems
• cyresmehta@yahoo.com
• Financial disclosure: None

