
It was a hectic outdoor clinic and on-call emergency day when I was called by senior professor Nagendra Shekhawat, MS, to his chamber. Even before I entered, I could hear the cries of an anguished young man. Then I saw him, seated at the slit lamp with his eyes closed forcefully, wailing in pain. “I am the sole breadwinner for my family. I have to care for my ailing old parents. I am a gemstone worker, and my livelihood depends on my sight.” His pain seemed more mental anguish than just physical agony.
This 24-year-old man had been hit in his right eye by a piece of glass in a workplace scuffle. Distraught and fearful, he was not cooperative enough for a detailed slit-lamp evaluation, but examination under diffuse light revealed a full-thickness corneal tear of about 6 to 7 mm with a shallow anterior chamber and a traumatic cataract. The professor stated that he could detect no uveal prolapse but there was some cortical matter in the anterior chamber.
The patient's other eye had 6/6 vision. We patched the injured eye and tried to explain to the patient the guarded visual prognosis.
The factory had declined to take responsibility for this daily wage worker's injury. He had no means or insurance to go to a private clinic. At a government-run institution like ours, one often encounters destitute patients in devastating life situations, and we always want to do our best for them. He desperately did not want to lose vision in the injured eye. Pleading with us to do our best to save his vision, the patient signed the consent forms and was then sent for blood tests and scans.
CASE CONSULTATION
A discussion of the case ensued with assistant professor Vishal Agarwal, MD, FRCS, other consultants, and me. I was a recently passed postgraduate MS ophthalmologist, posted in the vitreoretinal unit. Suddenly I realized I was a part of the discussion because I was being chosen to perform this surgery solo and unsupervised.
During training, my trauma repair surgeries had been supervised by assistant professors in the operating rooms (ORs) where I was posted, and my skills had steadily improved. I had recently been allowed to operate some trauma cases unsupervised. Receiving approving nods from senior surgeons for ocular trauma repairs in the past few weeks had instilled in me some confidence. But, in this instant, my mind was suddenly filled with doubt. I would have somebody's vision in my hands, and his trauma, handled poorly, would be not merely a statistic but a life-altering event for the patient.
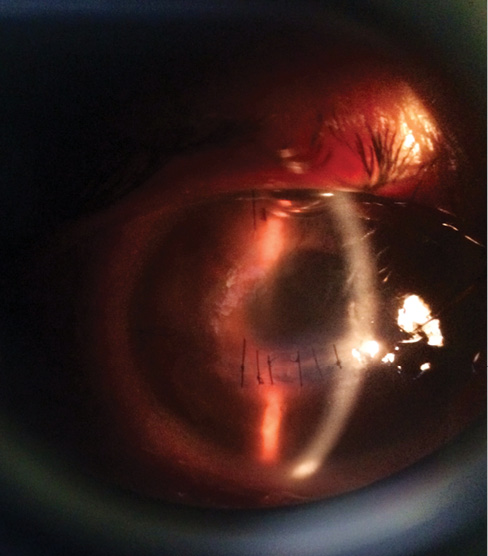
Figure 1. Slit-lamp photograph at 2 days postoperative.
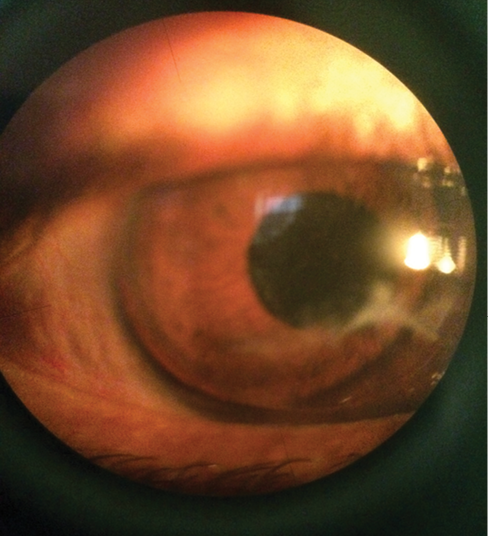
Figure 2. Slit-lamp photograph of the final result after suture removal, with the patient wearing a rigid contact lens.
As my mind reeled with these thoughts, the discussion continued. The factors favoring the patient were that he had reached the hospital within 3 hours of the injury and that the corneal laceration was below the pupillary axis. One consultant felt that, because it was a fresh injury with apparently clean wound margins and intact perception of light, the best approach would be to perform a primary repair of the corneal tear with primary traumatic cataract aspiration and implantation of posterior chamber IOL if the posterior capsule was found to be intact. Dr. Agarwal stated that the patient would have a better prognosis if the posterior segment and posterior capsule were intact. I asked about the nature of the IOL to be implanted; should it be hydrophobic acrylic or PMMA? One consultant suggested that a two-stage repair, with secondary IOL implantation, might be better than a prolonged one-stage surgery. Another consultant felt that final visual recovery from two surgeries would take much longer than from one surgery, however prolonged it might be. Trauma repair surgeries are followed by a sustained period of tissue healing and inflammation.
The consensus was that it would all come down to the integrity of the posterior capsule, and an IOL with power calculated for the patient's other eye should be kept ready if the capsule was found to be intact.
INTO SURGERY
The patient's scans revealed no intraocular foreign bodies. He was given a mild sedative before surgery. After cleaning and draping the patient, I finally saw the wound clearly under the microscope. With the help of the scrub nurse, I attached a Simcoe cannula onto the sterile drape near the bridge of the patient's nose using sterile adhesive and adjusted it so that there would be drop-by-drop irrigation of the surgical field.
I started by making a clean 1-mm corneal sideport incision superiorly, between the 11- and 12- o'clock positions. I filled the anterior chamber with cohesive OVD and tried to appose the corneal wound margins. The OVD formed the chamber slightly, and I began to place sutures on the cornea. The tear had a wave-like configuration, 6 to 7 mm long and below the pupillary axis. I applied about 10 interrupted 10-0 nylon sutures in the Rowsey-Hays pattern, with smaller suture bites, wider apart, in the center and longer but closer bites toward the ends of the tear.
I injected intracameral epinephrine and lidocaine so that the pupil would dilate and give me a good view of the cataract and anterior capsule. I checked the integrity of the sutures by washing away the OVD and refilling the chamber with balanced saline solution. I found a point of leak, resutured at two sites, and then buried all the sutures satisfactorily. When there was no leak and the pupil had dilated enough, a linear horizontal tear of approximately 5 mm could be seen in the anterior capsule, right beneath the corneal tear.
I stained the capsule using trypan blue dye, following the usual protocol of air injection, dye injection, washing out of the dye, and instillation of cohesive OVD. With the anterior chamber filled with cohesive OVD, I made a 2.2-mm uniplanar clear corneal temporal incision at the 9-o'clock position. After gently aspirating the cortical fibers in the anterior chamber, I refilled the chamber with cohesive OVD to flatten the anterior capsule.
Using Inamura capsulorrhexis forceps, I fashioned two semicircular capsulorrhexes, one on either side of the capsular tear. Thankfully, despite little cortical support and my slow and relatively inexperienced hands, the rhexis did not extend on either side. I now had an almost oval 5.5 X 6 mm opening in the anterior capsule.
After injecting dispersive OVD in the anterior chamber, I entered the anterior chamber with the phaco probe (Sovereign Compact WhiteStar; Abbott Medical Optics) to aspirate the fluffy, swollen cortical matter. Then I suddenly remembered that, due to the young age of the patient, the I/A probe would suffice for cortical removal.
The glow of the red reflex was visible, and I could visualize that, at least centrally, there was no tear in the capsule. After safe and deliberate I/A, I reformed the capsular bag with cohesive OVD. I implanted an acrylic foldable posterior chamber IOL in the bag and aspirated the OVD from the anterior chamber.
I formed the anterior chamber using balanced saline solution and a small bubble of air. Instead of hydrating the main and sideport incisions, I applied a single 10-0 nylon suture to each. The eye was padded and bandaged after a subconjunctival injection of antibiotic and steroid.
From start to finish, the surgery took almost 65 minutes, but I was satisfied that I had done my best for the patient surgically.
POSTOPerative COURSE
The next day when the bandage was removed, I saw a formed anterior chamber. Although there was some reaction in the anterior chamber, the patient could count fingers at 1 m. The professor examined the patient at the slit lamp and exclaimed, “Good job!” I was ecstatic, but the patient immediately complained, “I can only see a few fingers; how is it a good job?” The professor explained that healing of the tissues takes time and that the final outcome would come a few months later, after suture removal.
The patient was started on intensive topical antibiotics, topical steroids, timolol, and atropine eye drops for the inflammation. His inflammation began to decrease, and he was discharged 4 days after surgery with slightly improved vision (Figure 1).
Before leaving the ward, he again asked me if he would regain some vision. I was unsure what to promise, but I asked him to be patient and compliant with the medications. A doctor should know never to overpromise and underdeliver; I told the patient to wait for the final outcome.
At regular weekly follow-ups, his visual acuity steadily improved. His anxiety decreased significantly when he could read 6/36 partial unaided at the third postoperative week. At that time, indirect ophthalmoscopy showed that the posterior segment was not affected by the trauma. At subsequent follow-ups, the anterior chamber reaction decreased and the patient began to smile.
Before the suture removal, the patient had astigmatism of about -3.25 D. His BCVA was 6/9 by almost 2 months after surgery—improved from light perception at the time of his injury. On consulting the cornea expert, however, I learned that the astigmatism might be markedly different after suture removal, and I ought to prepare the patient mentally.
Two and a half months after primary surgery, I removed all sutures under topical anesthesia and restarted the topical antibiotic and steroid at a low dose. A week later, the patient was reading only 6/60 unaided and had astigmatism of about 4.75 D against-the-rule. I asked him again to be patient and to let me consult with experts in the cornea clinic, where I was luckily posted at the time. I performed manual keratometry and Pentacam (Oculus Optikgeräte) analysis in hope of seeing a different result, but, alas, the Pentacam showed even more astigmatism.
Because this patient would not be able to afford fancy astigmatism correction options such as a Sulcoflex supplementary IOL (Rayner Intraocular Lenses) or laser refractive surgery, I asked the cornea expert to help me try a rigid contact lens. The limited inventory of contact lenses available did not include a lens for this patient, and he became agitated after repeated visits to the cornea clinic.
But I did not give up hope. I found a senior optician who could order a customized rigid contact lens for the patient (Figure 2). Two weeks later, with a slightly tight-fitting contact lens, the patient could read 6/6 partial, and he was elated.
Yes, he had some problems such as foreign body sensation and getting used to the contact lens care. Maybe some day he will have the means for a better solution, but for now he has his sight back and is gainfully employed again.
CONCLUSION
Patience is the key to beautiful outcomes. However hard the situation may be, giving up is not an option. The outcome achieved with this patient reinforced my faith in the value of positive thinking and believing patiently in a higher power that helps us in periods of hardship. n
Sonal Kalia, MBBS, MS
• Senior Resident, Department of Ophthalmology, SMS Medical
College, Jaipur, India
• dr_sonal21@yahoo.co.in
• Financial disclosure: None

