
Since the iStent Trabecular Micro-Bypass Stent (Glaukos) was introduced to the US market, I have combined its implantation with cataract surgery and endoscopic cyclophotocoagulation (ECP) using the E2 Microprobe Laser and Endoscopy System (Endo Optiks) to perform what has been dubbed the ICE procedure on patients with early glaucoma for whom I want to eliminate medication use (http://eyetube.net/?v=ipepu). Combining a procedure that increases aqueous outflow (implantation of a trabecular microbypass stent) with one that decreases aqueous production (ECP) has been an effective option for the medical management of my glaucoma patients. Being able to perform these two microinvasive procedures without sutures, through the same incision created for cataract surgery, offers unique advantages to patients with early to moderate glaucoma.
SURGICAL PROCEDURE
My protocol for performing ICE starts with positioning myself temporally, just as I would sit to perform cataract surgery. My first surgical step is clear corneal cataract surgery. After implanting the IOL, I remove the OVD from the capsular bag and place just enough OVD in the ciliary sulcus for me to see the entire ciliary process. I then perform ECP for 360º.
I remove the OVD from the ciliary sulcus and instill acetylcholine chloride intraocular solution to bring down the pupil so that I can visualize the angle and implantation of the stent (Figure 1). I administer additional sodium hyaluronate OVD in the anterior chamber in order to visualize the entire nasal angle. Next, I turn the patient’s head 30º to 45º away from me and tilt the microscope. I use a surgical gonioprism to view the angle and implant the stent by my usual technique through the cataract incision. I attempt to implant the device where I surmise a collector channel to be; I postulate this by visualizing the aqueous veins on the surface of the eye and also by looking for pigment collected over the trabecular meshwork or blood collected in the canal. After making sure I have removed all of the OVD, I check that the wounds are watertight before removing the speculum.
ICE can be performed under topical anesthesia, but, when the patient might not tolerate the discomfort of ECP, I administer a retrobulbar block. I instruct patients to use fluoroquinolone and difluprednate drops every 2 hours while awake on the day of surgery. I prescribe difluprednate to maximally decrease inflammation at the start of the postoperative period and then rapidly taper the dosage to four times a day for 1 week and then twice a day for 2 weeks. Unlike after typical cataract surgery or implantation of the trabecular microbypass stent on its own, I find it is necessary to be more aggressive with steroid treatment in order to achieve positive results with ECP. I see patients 1 day, 1 week, and 3 weeks postoperatively to monitor them for IOP spikes in response to steroid therapy.
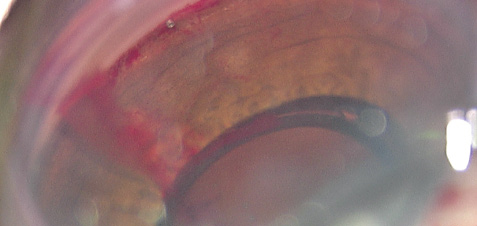
Figure 1. The iStent viewed with the endoprobe.
PATIENT SELECTION
Patients who have angle-closure glaucoma or plateau iris are typically better candidates for ECP alone, especially if there are any peripheral anterior synechiae. Patients with controlled open-angle glaucoma and cataract who are using multiple IOP-lowering medications are generally excellent candidates for ICE. For someone who has a visually significant cataract and is using a single IOP-lowering drug, either ECP or a trabecular microbypass stent will work well on its own. If the patient is taking more than one medication or is taking one medication but has an IOP just above the target, then ICE may be a better choice. Pigment dispersion glaucoma and pseudoexfoliation glaucoma are not contraindications for ICE.
I have also performed ICE on patients with moderate to advanced glaucoma who had a bad experience with filtering surgery in their other eye or who have already undergone glaucoma drainage device or filtration surgery in the same eye. The chance that ICE will eliminate their need for IOP-lowering medication is certainly lower than for individuals with early glaucoma. I therefore carefully educate patients with moderate to advanced glaucoma about the likelihood that they will need medication postoperatively, and I explain that they may later require canaloplasty or filtering surgery if their target IOP is not reached with ICE.
At a Glance
• Being able to perform a sutureless combination procedure with trabecular microbypass stent implantation and ECP through the same incision created for cataract surgery offers unique advantages to patients with early to moderate glaucoma.
• This treatment, dubbed the ICE procedure, retains the refractive aspect of cataract surgery, does not induce astigmatism or cause foreign body sensation, restores natural physiology in patients who desire the best visual outcomes, and carries no long-term risk of blebrelated infection, bleb leaks, or dysesthesia.
Watch it Now
Nathan Radcliffe, MD, describes the ICE procedure, which is a combination of iStent implantation, cataract extraction, and endocyclophotocoagulation.
CONCLUSION
My patients appreciate that ICE involves no external sutures and thus does not induce astigmatism or cause foreign body sensation, both of which are typical of trabeculectomy. Furthermore, this combined procedure does not produce an extraocular reservoir or subconjunctival filtration. For that reason, ICE carries no long-term risk of bleb-related infection, bleb leak, or dysesthesia.
In my experience, patients’ postoperative visual recovery is rapid. In fact, it is essentially the same as after cataract surgery alone. I would argue that ICE retains the refractive aspect of cataract surgery but changes the perception of glaucoma surgery from that of a desperate rescue to a procedure that restores natural physiology in patients who desire the best visual outcomes. n
Steven R. Sarkisian Jr, MD
• Glaucoma Fellowship Director, Dean McGee Eye Institute
• Clinical Professor, University of Oklahoma College of Medicine, Oklahoma City
• steven-sarkisian@dmei.org
• Financial disclosure: Investigator (MIGS Study Group and iStent Inject Study, both sponsored by Glaukos), Advisory board (Endo Optiks)

