Point: A LASIK Rebrand is in Order
By Soosan Jacob, MS, FRCS, DNB; Amar Agarwal, MS, FRCS, FRCOphth; and Marc Mullie, MD, FRCSC
Rebrand Refractive Surgery by Introducing a New Procedure


Soosan Jacob, MS, FRCS, DNB; and Amar Agarwal, MS, FRCS, FRCOphth
Corneal refractive surgery has evolved over the years, progressing through techniques from cuts in the cornea (RK), to excimer laser surface ablation (PRK), to intrastromal ablation under a flap (LASIK). The last of these approaches has been the most successful technique thus far, with widespread worldwide acceptance and penetration.
WHAT YOUR PEERS ARE SAYING ABOUT LASIK REBRANDING
• Instead of rebranding LASIK specifically, it could be beneficial to rebrand refractive surgery generally.
• Because the surgical procedure of LASIK has changed so much, and the surgical results it provides have improved so much, it may benefit from a new name.
• Ophthalmologists talk about LASIK volumes being down, but it is likely more informative to look at refractive surgery volume overall.
• Instead of a total rebranding, what LASIK may need is increased public awareness of the safety of modern LASIK and the fact that now almost any complication can be fixed.
• LASIK is far from dead. The practices that will succeed in refractive surgery in the coming years will be those that figure out how to reach and attract the new, emerging market of millennials.
The LASIK flap itself has evolved, from being created with a mechanical microkeratome to being cut with a femtosecond laser. As with the evolution of medicine and any other surgical technique, refinements keep occurring, and rebranding of a procedure as something that is better, with definite advantages over the older version, is a perpetual phenomenon.
Based on extensive work by Sekundo et al1 and Shah et al,2 among others, small incision lenticule extraction (SMILE) is a recently introduced technique for refractive error correction that uses a femtosecond laser to create an intrastromal lenticule corresponding to the patient’s refractive error. This is done by creating two lamellar cuts: a posterior lenticule cut and an anterior cap cut, corresponding to the posterior and anterior surfaces of the lenticule, respectively. These two cuts intersect, and the intrastromal lenticule is then extracted through an incision that can be as small as 2 mm (Figure 1). The cap can be set to varying thicknesses; at present, a thickness of 120 µm is most commonly used.
It is our thought that, instead of rebranding LASIK specifically, we rebrand refractive surgery generally. This can be achieved by introducing patients to SMILE, the newest refractive surgery procedure. The advantages that this technique offers are numerous. For starters, the absence of a flap and the use of a small incision together act to eliminate flap-related complications such as striae, flap dislodgement, and epithelial ingrowth. Similarly, because of decreased disruption of the anterior corneal innervation, there is faster recovery of corneal sensitivity and less patient experience of dry eye than is seen with LASIK.3 Most important, the presence of the nearly intact anterior stromal layer of the cornea allows better maintenance of biomechanical strength after SMILE compared with LASIK.4,5 The entire procedure is completed with a single laser, thus decreasing surgical time and costs compared with LASIK using both excimer and femtosecond lasers. All these advantages, along with visual and refractive outcomes similar to those of LASIK, give SMILE a superior edge over LASIK.6,7 Disadvantages include inability to treat hyperopia with SMILE and absence of correction for cyclotorsion.8,9 However, nomogram adjustments may be made for the latter.
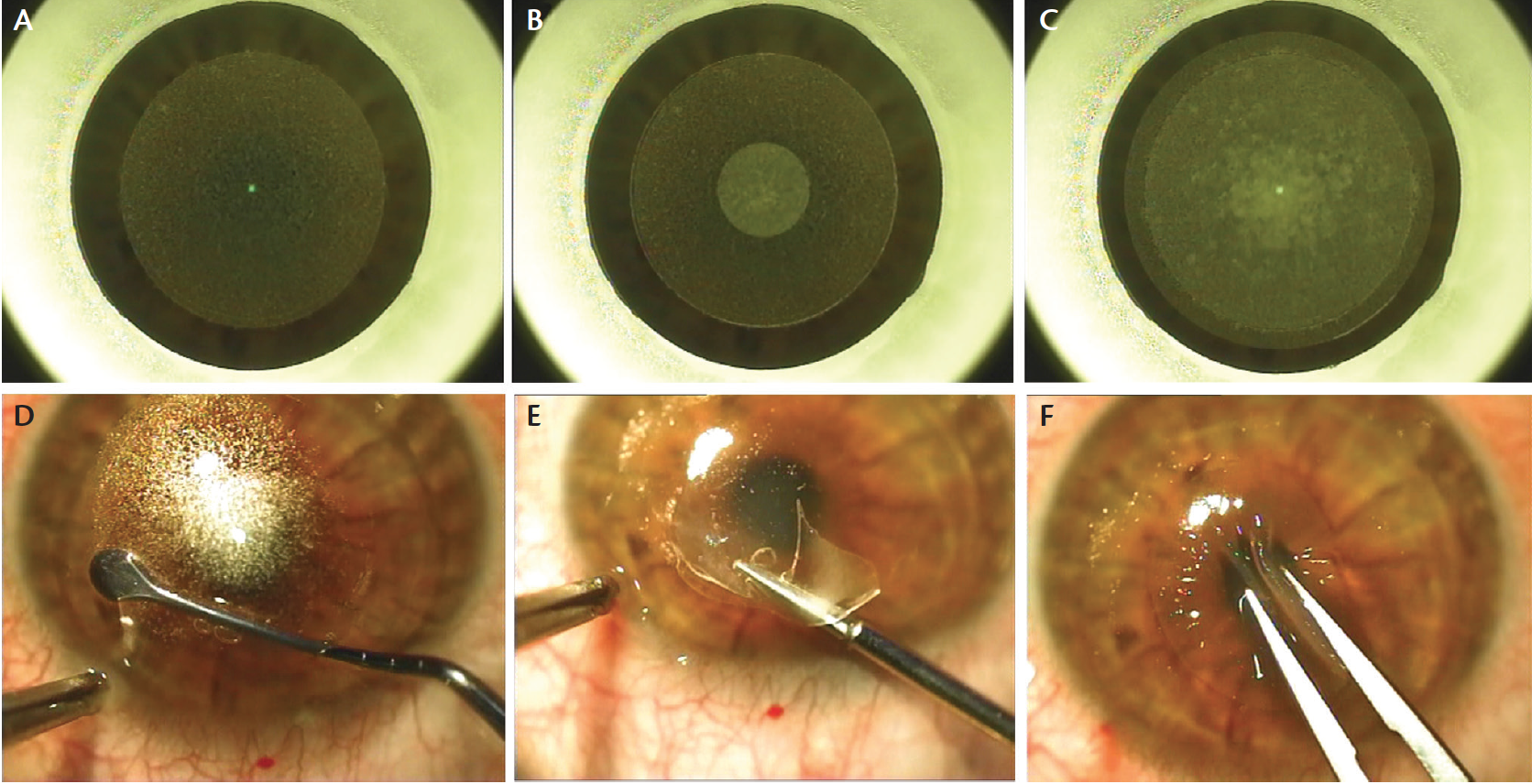
Patients with access to this procedure often prefer the advantages that SMILE offers and opt for it over LASIK. Further improvements will come along for this technology, including better and faster lasers, smaller incision cuts, better nomograms, better astigmatic correction, and identification and compensation for cyclotorsion. However, even now, this evolution in refractive surgery has come into its own. This will allow us to rebrand refractive surgery with a SMILE, as we can describe to our patients the distinct advantages this new procedure offers.
1. Sekundo W, Kunert KS, Blum M. Small incision corneal refractive surgery using the small incision lenticule extraction (SMILE) procedure for the correction of myopia and myopic astigmatism: results of a 6 month prospective study. Br J Ophthalmol. 2011;95(3):335-339.
2. Shah R, Shah S, Sengupta S. Results of small incision lenticule extraction: all-in-one femtosecond laser refractive surgery. J Cataract Refract Surg. 2011;37(1):127-137.
3. Li M, Zhou Z, Shen Y, et al. Comparison of corneal sensation between small incision lenticule extraction (SMILE) and femtosecond laser-assisted LASIK for myopia. J Refract Surg. 2014;30:94-100.
4. Reinstein DZ, Archer TJ, Randleman JB. Mathematical model to compare the relative tensile strength of the cornea after PRK, LASIK, and small incision lenticule extraction. J Refract Surg. 2013;29(7):454-460.
5. Wu D, Wang Y, Zhang L, et al. Corneal biomechanical effects: Small-incision lenticule extraction versus femtosecond laser-assisted laser in situ keratomileusis. J Cataract Refract Surg. 2014;40:954-962.
6. Lin F, Xu Y, Yang Y. Comparison of the visual results after SMILE and femtosecond laser-assisted LASIK for myopia. J Refract Surg. 2014;30:248-254.
7. Ganesh S, Gupta R, Comparison of visual and refractive outcomes following femtosecond laser- assisted LASIK with SMILE in patients with myopia or myopic astigmatism, J Refract Surg. 2014;30:590-596.
8. Zhang J, Wang Y, Chen X. Comparison of moderate- to high-astigmatism corrections using wavefront-guided laser in situ keratomileusis and small-incision lenticule extraction. Cornea. 2016;35(4):523-530.
9. Chan TC, Ng AL, Cheng GP, et al. Vector analysis of astigmatic correction after small-incision lenticule extraction and femtosecond-assisted LASIK for low to moderate myopic astigmatism. Br J Ophthalmol. 2016;100(4):553-559.
Why We Need a New Acronym to Replace LASIK

Marc Mullie, MD, FRCSC
After more than 20 years, the acronym LASIK has become a dirty five-letter word, especially on the Internet. A procedure that was introduced more than 20 years ago and that took as many years to perfect has attracted to itself many negative comments, reviews, and testimonials on the Web, some of them quite old. Many websites are blindly devoted to badmouthing LASIK on the basis of complications that occurred 15 to 20 years ago. Because of this, and despite the overwhelmingly great results achieved with LASIK, the word induces fear, negativity, and confusion in many people. We may need a new name. But why?
When you think about it, little of what we were doing surgically when the term LASIK was introduced 20-plus years ago still exists. Back then we created flaps with crude mechanical keratomes and ablated corneas with broad-beam laser profiles, small optical zones, and poor or nonexistent eye tracking. We now employ femtosecond lasers for flap creation and high-speed, small-spot excimer lasers with large optical zones for ablation, using wavefront-optimized or topographic profiles, with superb eye trackers. So if the surgical procedure has changed so much, and the surgical results it provides have improved so much, why not give it a new name?
Try explaining to patients the origin of the term LASIK—from laser-assisted in situ keratomileusis—and watch as the blank stares come over their faces. The word keratomileusis, coined by Barraquer in the 1960s, referred to mechanical excision of tissue, not a laser ablation, so in a sense there is an internal contradiction in the term LASIK.
I hereby propose the term LACOREX (pronounced Ley-co-rex), an acronym for laser corneal excision, a simple term that the lay audience can readily understand. It is broad enough to encompass all variations of modern LASIK, easy to pronounce, easy to visualize in the mind’s eye, and it suggests the use of lasers to excise tissue from the core of the cornea (ie, in the stroma, under a flap).
An alternative might be LACORE (pronounced Ley-core), an acronym for laser corneal reshaping. To my mind, LACOREX is the better choice: It sounds more surgical and precise, and it is easy to pronounce in many languages.
The term LASIK just ain’t so sexy any longer. We have tried all kinds of marketing makeup to cover the LASIK wrinkles over the years, and they have not worked, so how about a surgical, etymological facelift?
Soosan Jacob, MS, FRCS, DNB
• Director and Chief, Dr. Agarwal’s Refractive and Cornea Foundation, Dr. Agarwal’s Group of Eye Hospitals, Chennai, India
• Senior Consultant, Cataract and Glaucoma Services, Dr. Agarwal’s Group of Eye Hospitals, Chennai, India
• Member, CRST Europe Global Advisory Board
• dr_soosanj@hotmail.com
• Financial interest: None acknowledged
Amar Agarwal, MS, FRCS, FRCOphth
• Professor and Head, Dr. Agarwal’s Eye Hospital and Eye Research Centre, Chennai, India
• dragarwal@vsnl.com
• Financial interest: None acknowledged
Marc Mullie, MD, FRCSC
• Laservue Clinic, Montreal, Canada
• marcmullie@laservue.ca
• Financial interest: None acknowledged
Counter: LASIK is Fine as Is
By Michael Lawless, MBBS, FRANZCO, FRACS; Dan Z. Reinstein, MD, MA(Cantab), FRCSC, DABO, FRCOphth, FEBO; Vance Thompson, MD; and J. Trevor Woodhams, MD
Rebranding LASIK in 2016 is Missing the Point

Michael Lawless, MBBS, FRANZCO, FRACS
The two biggest things that have made a difference to my refractive surgery practice over the past 2 years have been the introduction of SMILE for anyone with more than 3.00 D of myopia, with or without astigmatism, and transepithelial PRK. We have introduced these techniques without disparaging LASIK because we still need LASIK for hyperopes, for -2.00 D myopes, and just because some people are really keen on LASIK and are in the range where the difference between LASIK and SMILE is inconsequential. So, for anyone who is suitable for laser vision correction, there are three great choices: SMILE, LASIK, and no-touch transepithelial PRK.
Where is the branding of LASIK in this equation? Our service is not about LASIK, it is all about vision correction and making the right choice for the right patient. In the same way, it would be wrong to purely promote SMILE or no-touch transepithelial PRK because they will not be applicable to everybody. By promoting only one procedure, you are suggesting that other procedures are inferior. All three of these laser procedures offer great results when performed using the latest technology, in the right circumstances, for the right patient, by a good surgeon.
By all means, we can tell individual stories around new procedures, such as SMILE or no-touch PRK, or tout improvements in LASIK as they come along, but only within the context of the overwhelming good that comes from laser vision correction. We do not need to rebrand LASIK: We need to acknowledge that refractive surgery is more than LASIK, and we need to offer a range of procedures to address the right condition for each patient.
All Ophthalmologists Need Access to the Advanced Tools for Addressing Complications

Dan Z. Reinstein, MD, MA(Cantab), FRCSC, DABO, FRCOphth, FEBO
Let us be clear: LASIK is an outstandingly safe and effective procedure. It is one of the most thoroughly researched procedures in modern medicine, and its safety and efficacy are extensively documented in the literature.1-6 Patient satisfaction after LASIK is extremely high, surpassing patient satisfaction with contact lenses.7 The procedure is also popular among refractive surgeons: 63% of refractive surgeon candidates responding to a recent survey had undergone laser vision correction.8 I was recently added to that list, having undergone Presbyond laser blended vision LASIK earlier this year.
These facts are not surprising given the amount of investment in research and development into LASIK over the past 30 years and the more than 50 million procedures performed to date. Clinicians and researchers have had ample resources and opportunity to develop and fine-tune both the technology and the procedure.
However, the penetration of LASIK among spectacle and contact lens wearers is probably still only about 1% to 2%. Why is the market penetration not comensurate with LASIK’s phenomenal life-changing effects and extremely low risk profile? Most industries would consider such low adoption rates a commercial failure. These facts are not aligned.
What is the missing link? In my experience, the most common reason patients express for choosing not to have LASIK is the fear that “if something goes wrong, it can’t be fixed.” The unfortunate reality is that this statement used to be true; for the first 10 years of LASIK, there was literally nothing that could be done. And, although layered anatomic diagnostic imaging9,10 and some effective repair tools have been developed since then, such as topography-guided custom ablation11,12 and transepithelial PTK,13-15 these resources are not accessible to the majority of refractive surgeons. Therefore, many patients with complications of LASIK are told that there is nothing more that can be done to help them, so the reputation of LASIK suffers when this expression is disseminated.
Most of us will probably never use the airbags in our cars, but few today would consider buying a car without them. I believe we are now in the era of LASIK with airbags, so to speak. We should be able to say to prospective patients, “If you have a complication, it would be extremely unlikely that we cannot fix it.” This was the reason that we started a Therapeutic Refractive Surgery section in the Journal of Refractive Surgery.16 We hope that, by providing a rigorous scientific forum for developing technology and reporting such cases, we can foster increased speed of development of new techniques and expand knowledge to surgeons who are currently unable to treat patients with corneal irregularities. Eventually we hope to realize the final goal: Any LASIK surgeon should be able to fix anything that is fixable, not just a selected subset of surgeons.
Does LASIK need to be rebranded? I would say that it does not need a total rebranding; it needs increased public awareness of the safety of modern LASIK and of the fact that we can now fix almost any complication. However, this last element must become a focus for laser manufacturers. The repair modules and techniques now available only to experts must be turned into standard features and common knowledge, not optional add-ons. We have the technological components of the LASIK puzzle at our fingertips; we just need to figure out how to piece it all together.
1. Reinstein DZ, Carp GI, Lewis TA, Archer TJ, Gobbe M. Outcomes for myopic LASIK with the MEL 90 excimer laser. J Refract Surg. 2015;31:316-321.
2. Khalifa MA, Mossallam EF, Massoud TH, Shaheen MS. Comparison of visual outcomes after variable spot scanning ablation versus wavefront-optimized myopic LASIK. J Refract Surg. 2015;31:22-28.
3. Meyer B, Sluyterman van Langeweyde G, Wottke M. Refractive outcomes of an advanced aspherically optimized profile for myopia corrections by LASIK: a retrospective comparison with the standard aspherically optimized profile. Clin Ophthalmol. 2015;9:379-392.
4. Yu CQ, Manche EE. Comparison of 2 femtosecond lasers for flap creation in myopic laser in situ keratomileusis: one-year results. J Cataract Refract Surg. 2015;41:740-748.
5. Ziaei M, Mearza AA, Allamby D. Wavefront-optimized laser in situ keratomileusis with the Allegretto Wave Eye-Q excimer laser and the Femto LDV Crystal Line femtosecond laser: 6 month visual and refractive results. Cont Lens Anterior Eye. 2015;38:245-249.
6. Reinstein DZ, Carp GI, Archer TJ, et al. Long-term visual and refractive outcomes after LASIK for high myopia and astigmatism from -8.00 to -14.25 D. J Refract Surg. 2016;32:290-297.
7. Price MO, Price DA, Bucci FA Jr, Durrie DS, Bond WI, Price FW Jr. Three-year longitudinal survey comparing visual satisfaction with LASIK and contact lenses [published online ahead of print May 18, 2016]. Ophthalmology.
8. Kezirian GM, Parkhurst GD, Brinton JP, Norden RA. Prevalence of laser vision correction in ophthalmologists who perform refractive surgery. J Cataract Refract Surg. 2015;41:1826-1832.
9. Reinstein DZ, Silverman RH, Raevsky T, et al. Arc-scanning very high-frequency digital ultrasound for 3D pachymetric mapping of the corneal epithelium and stroma in laser in situ keratomileusis. J Refract Surg. 2000;16:414-430.
10. Li Y, Tan O, Brass R, Weiss JL, Huang D. Corneal epithelial thickness mapping by Fourier-domain optical coherence tomography in normal and keratoconic eyes. Ophthalmology. 2012;119:2425-2433.
11. Reinstein DZ, Archer TJ, Gobbe M. Combined corneal topography and corneal wavefront data in the treatment of corneal irregularity and refractive error in LASIK or PRK using the Carl Zeiss Meditec MEL80 and CRS Master. J Refract Surg. 2009;25:503-515.
12. Stojanovic A, Suput D. Strategic planning in topography-guided ablation of irregular astigmatism after laser refractive surgery. J Refract Surg. 2005;21:369-376.
13. Chen X, Stojanovic A, Zhou W, Utheim TP, Stojanovic F, Wang Q. Transepithelial, topography-guided ablation in the treatment of visual disturbances in LASIK flap or interface complications. J Refract Surg. 2012;28:120-126.
14. Reinstein DZ, Archer TJ, Dickeson ZI, Gobbe M. Trans-epithelial phototherapeutic keratectomy protocol for treating irregular astigmatism based on population epithelial thickness measurements by Artemis very high-frequency digital ultrasound. J Refract Surg. 2014;30:380-387.
15. Vinciguerra P, Camesasca FI. Custom phototherapeutic keratectomy with intraoperative topography. J Refract Surg. 2004;20:S555-563.
16. Reinstein DZ. Therapeutic refractive surgery. J Refract Surg. 2015;31:6-8.
We Need to Consider Refractive Surgery Overall

Vance Thompson, MD
Ophthalmologists talk about LASIK volumes being down, but it is likely more informative if we look at refractive surgery volume overall. For instance, in my practice, refractive surgery consultations are up, not down. It may be, however, that today we are doing less LASIK and more lens work.
This is for a couple reasons. One is improved diagnostics. Take the example of a 55-year-old, 4.00 D myope who has come to us for LASIK. He reports some issues with nighttime image quality. As part of our workup, I will use the HD Analyzer (Visiometrics) and iTrace (Tracey Technologies) to see if there is optical scatter in the lens that might explain the nighttime issues. If I detect a degree of optical scatter in the lens, I will not do LASIK on that patient. I might talk to him instead about refractive lens exchange. Ten years ago, because he could be corrected to 20/20, I probably would have done LASIK, and then he would have continued to have those nighttime issues until we took care of his lens at a later date.
For patients whose lenses are not clear, we can steer them toward a lens-based procedure. The multifocal IOL technologies that we have now are greatly improved over earlier models, and they are making many patients happy. Again, though, diagnostics like the HD Analyzer and the iTrace come in handy, as they allow us to ensure there is not too much corneal multifocality. We would not want to add to that with a multifocal implant.
On the other hand, if our modern diagnostics show that the lens is clear, we can do LASIK successfully because the technology has never been better. Finally, if we determine that the lens is clear in our evaluation, especially for a presbyope who is not ready to have his or her lens replaced, corneal inlay technology offers a great option. The Kamra inlay (AcuFocus) has become important in our practice.
The point is this: Refractive surgery volume is healthy when you consider both cornea- and lens-based procedures. New diagnostic devices and treatment technologies are revolutionizing what we are capable of doing for patients today.
The Millennial Generation is Ready for LASIK

J. Trevor Woodhams, MD
I was a little taken aback by this point/counterpoint because my ongoing experience is that LASIK has come surging back in recent years. I now am doing more LASIK than IOL cases, as was once the situation 10 to 13 years ago. I suspect the reason for this has little to do with the LASIK procedure or its name and much more to do with knowing how to re-engineer the way we reach prospective patients. While word of mouth is always the best type of advertising, reaching a critical mass to sustain it usually requires ongoing paid communication with the public.
In the early days of LASIK, this was done with radio and print advertising. Those media (and, to a certain extent, television) were how members of the baby boom generation got their news and information on social trends and technologies. That generation, the massive post–World War II tsunami of affluent children, is now in its 50s to 70s. It has, therefore, moved decisively out of the marketplace for LASIK. Presbyopic lens exchange, despite its higher cost and risks, is now generally a better and more permanent solution for refractive (and lenticular) problems for the generation born between 1946 and 1964. LASIK practices ignore this demographic shift at their peril.
I would argue, therefore, that the dearth of LASIK patients has much more to do with demographic changes than with disenchantment over a procedure that has worn out its welcome. The generations that succeeded the baby boomers—generation X and generation Y—are much smaller and have had more economic challenges than their parents. This, combined with an attitude of entitlement fostered by a generation of generous government social programs, has naturally produced a significant drop in the number of patients able to afford an elective procedure paid for out of pocket.
However, the newest generation to enter the workforce—and, therefore, to have the discretionary income for an elective procedure such as LASIK—is huge, in fact, even bigger than the baby boom generation. The millennials, born from 1981 to about 2004, came of age with September 11, 2001, as their historical touchstone and the Internet and instant communication as their preferred avenue for news, personal contact, and awareness of social and technological trends. They do not listen to the radio, read newspapers or magazines, or necessarily believe what established organizations tell them.
In March 2014, the Pew Research Center issued a report about millennials in adulthood, noting that they tend to be detached from institutions but networked with friends.1 The report further said that millennials are more upbeat than older adults about America’s future. They are also increasingly skeptical of the ability of the state, either in the United States or in the European Union, to be able to provide what has been promised. Despite resistance, the gig economy—the reliance on freelance or Internet-based piecework such as driving for Uber, rather than full-time work—is increasingly becoming the norm.
The term LASIK is fine. The procedure has a great reputation for safety and efficacy. And, by now, no one expects somebody else (ie, the government or insurance) to pay for it. If anything, the term LASIK is becoming a generic term meaning “painless and safe elective eye surgery to see better,” when what is actually performed may be a corneal inlay, presbyopic lens exchange, or PRK.
To reach the new generation of prospective LASIK patients requires a familiarity with millennial behavior and the ability to reach these individuals through nontraditional means. These means are primarily the social networks of Facebook, Google+, Twitter, Snapchat, and a host of short-lived apps that a boomer like me sometimes cannot even understand.
Millennials do not trust anyone they perceive to be selling them something. And they can instantly check one’s credibility online.
LASIK is far from dead. Those who will succeed in refractive surgery in the coming years will be those who figure out how to reach and attract the new, emerging market of millennials.
1. FactTank: 6 new findings about millennials. Pew Research Center. March 7, 2014. http://www.pewresearch.org/fact-tank/2014/03/07/6-new-findings-about-millennials/. Accessed June 21, 2016.
Michael Lawless, MBBS, FRANZCO, FRACS
• Vision Eye Institute, Chatswood, New South Wales, Australia
• Clinical Associate Professor, Sydney Medical School, University of Sydney, New South Wales, Australia
• Member, CRST Europe Editorial Board
• michael.lawless@visioneyeinstitute.com.au
• Financial interest: None acknowledged
Dan Z. Reinstein, MD, MA(Cantab), FRCSC, DABO, FRCOphth, FEBO
• Medical Director, London Vision Clinic, London
• Adjunct Professor of Ophthalmology, Columbia University Medical Center, New York
• Associate Professor, Centre Hospitalier National d’Ophtalmologie, Paris
• Visiting Professor, School of Biomedical Sciences, University of Ulster, Coleraine, United Kingdom
• dzr@londonvisionclinic.com
• Financial disclosure: Consultant (Carl Zeiss Meditec); Proprietary interest (ArcScan)
Vance Thompson, MD
• Founder, Vance Thompson Vision, Sioux Falls, South Dakota
• Professor of Ophthalmology, University of South Dakota Sanford School of Medicine
• vance.thompson@vancethompsonvision.com
• Financial disclosure: Consultant (Abbott Medical Optics, Alcon, Bausch + Lomb, Carl Zeiss Meditec)
J. Trevor Woodhams, MD
• Surgical Director, Woodhams Eye Clinic, Atlanta, Georgia
• twoodhams@woodhamseye.com
• Financial interest: None acknowledged

