Among the options for excimer laser refractive surgery, surface ablation is less invasive than LASIK and seems to structurally weaken the cornea to a lesser degree. Therefore, over the past decade, a trend has emerged favoring surface ablation techniques.1,2 Several modifications of the conventional PRK procedure have been introduced in efforts to minimize the disadvantages of surface ablation, which can include extended epithelial healing and visual recovery times, pain, and corneal haze. In these alternative methods, the means by which the corneal epithelium is removed prior to laser photoablation are modified to reduce the trauma caused by epithelial debridement.
AT A GLANCE
• The surgical maneuver described in this article combines chemical and mechanical actions and can be used to debride the corneal epithelium prior to surface photoablation.
• This debridement technique combines the initial chemical effect of a 20% ethanol solution, which loosens the corneal epithelium, with a nontraumatic mechanical effect produced by the circular movement of the cellulose sponge and subsequent epithelial peeling.
• Advantages of the procedure include minimized patient discomfort, potential improvement in the safety of the procedure, and a requirement of only basic surgical instruments.
Initially, alternative surface ablation procedures involved mechanical debridement using different types of rotating brushes or scalpel blades. In 1999, Camellin first described the laser-assisted subepithelial keratomileusis (LASEK) technique. This procedure involves the use of a cone filled with a dilute alcohol solution placed over the cornea, resulting in creation of a complete flap of epithelium. In another procedure, transepithelial PRK (trans-PRK), the excimer laser is used to remove the epithelium. In yet a third alternative technique, epi-LASIK, an epithelial microkeratome is used to separate the corneal epithelium from the underlying anterior stroma.
There is controversy surrounding the advantages and disadvantages of each method. In this article and accompanying Eyetube video (bit.ly/calabuig0516), we report a technique in which the corneal epithelium is peeled off prior to excimer laser surface photoablation. This technique combines both chemical and blunt mechanical processes in order to minimize patient discomfort and potentially improve the safety of the procedure. Our technique requires only basic surgical instruments.3
combined epithelial debridement
Preoperatively, patients receive one drop of tetracaine 0.5% and preservative-free diclofenac 0.1%. Lashes and lids are cleaned with a swab of povidone-iodine 5% solution. A closed-loop lid speculum is placed, and another drop of tetracaine is instilled.
An 8- or 9-mm circular cellulose Weck-Cel sponge soaked in 20% ethanol solution is positioned over the central corneal surface for 50 seconds (Figure 1). If some solution leaks toward the periphery, it is dried with another Weck-Cel spear, thus avoiding damage to the limbal stem cells and irritation of the patient’s conjunctiva by the alcohol solution.
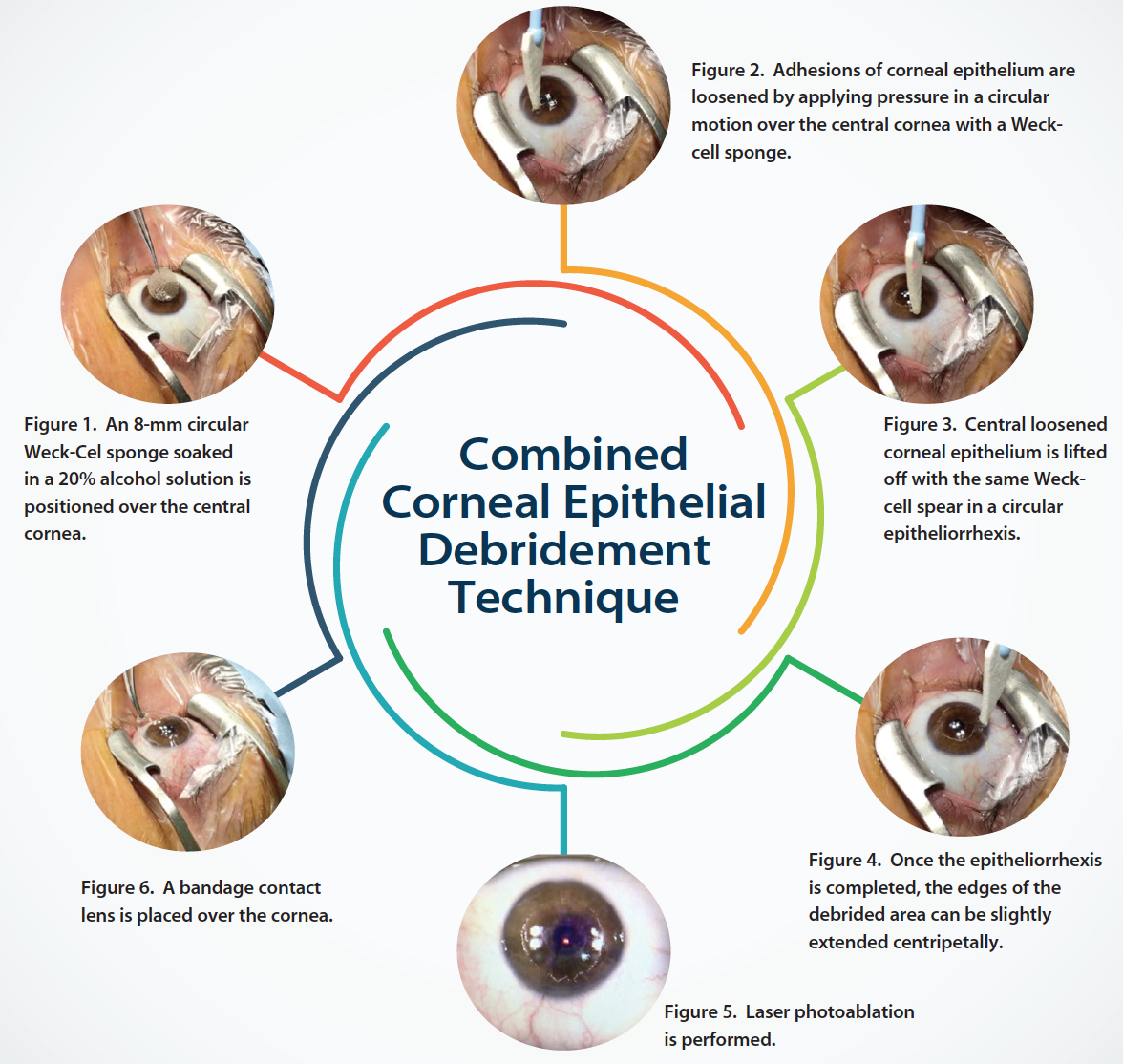
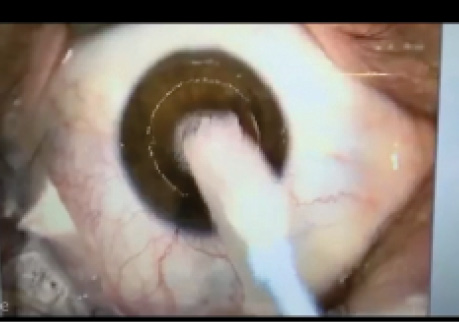
The circular sponge is discarded, and the surface of the eye is flushed twice with chilled balanced saline solution in order to remove residual alcohol. Adhesions of corneal epithelium are loosened by applying pressure with another Weck-Cel sponge using circular movements over the central surface of the cornea. The central corneal epithelium is then easily lifted off in a circular epitheliorrhexis manner (Figures 2 through 4).
The edges of the debrided area can be slightly extended toward the corneal periphery with the Weck-Cel spear or a blunt spatula. If the surgeon prefers to replace the epithelium over the stromal surface after laser ablation, he or she can do so, as the whole epithelial flap can be lifted unspoiled. If not, the epithelial flap is discarded. For hyperopic and high astigmatic treatments, the larger 9-mm circular sponge is preferred; the 8-mm diameter sponge is used in most myopic treatments, well centered over the pupil area.
Excimer laser photoablation is then carried out using our standard nomogram (Figure 5). After laser ablation, 0.02% mitomycin C (MMC) is applied on the ablated stroma. The duration of MMC application is 12 seconds when the depth of central ablation is less than 65 µm and 20 seconds if it is more than 65 µm. The eye is then thoroughly irrigated with 50 mL chilled balanced saline solution, and a silicone hydrogel contact lens (Acuvue Oasys; Johnson & Johnson Vision Care) is placed over the cornea until complete reepithelization has occurred (Figure 6). Moxifloxacin 0.5% and diclofenac 0.1% eye drops are instilled, and the patient is discharged.
FOLLOW-UP CARE AND PRESCRIPTIONS
Postoperatively, topical preservative-free dexamethasone 0.1% and moxifloxacin 0.5% are prescribed every 6 hours for the first week as well as topical preservative-free diclofenac 0.1% every 6 hours for 2 days. For the first 3 days, oral analgesia is prescribed with a combination of acetaminophen 1 g every 8 hours and ibuprofen 600 mg three times daily.
IN OUR EXPERIENCE
Contact with the circular cellulose sponge soaked in ethanol solution is required for 50 seconds in order to easily loosen the corneal epithelium. When exposure time is shorter, removal of the epithelium with the Weck-Cel sponge is often incomplete, and the use of another rigid surgical instrument may be required thereafter.
No clinical adverse effects have been seen with this amount of alcohol solution exposure time, which is longer than that described in previous techniques.
Additionally, patient tolerance is excellent, as no pressure is applied over the globe. The technique also allows complete lifting of the epithelial flap, which can be repositioned over the corneal stroma after laser ablation or discarded, whichever the surgeon considers appropriate.
In week 2, the steroid drop is changed to fluorometholone 0.1%, which is tapered between the second and third month. Extensive use of artificial tears (0.15% sodium hyaluronate) is recommended during the first month and later as required by the patient’s symptoms.
Patients are monitored every 2 days postoperative until the epithelial defect has healed completely, and, at that time, the bandage contact lens is removed. Follow-up visits are scheduled for 1 week and 1, 3, and 6 months thereafter.
POTENTIALLY TRAUMATIC SURGICAL INSTRUMENTS NOT REQUIRED
Pain, slow vision recovery, myopic regression, and haze have been described as the adverse effects related to conventional PRK. Several safe and effective modifications of the initial PRK technique have been introduced in order to minimize these drawbacks.4 These include trans-PRK, deepithelization with diluted alcohol, epithelial mechanical scraping with scalpels or rotating brushes, and epi-LASIK.5-7
However, controversy remains regarding the advantages and disadvantages of each method,8 particularly in regard to postoperative pain, recovery of visual acuity, subepithelial scar formation, the toxic effect of alcohol, and the synergistic effect of MMC use.9-11
In contrast, our technique combines the initial chemical effect of a 20% ethanol solution, which loosens the corneal epithelium, with a nontraumatic mechanical effect produced by the circular movement of the cellulose sponge and subsequent epithelial peeling. This procedure unites the advantages of the two techniques (alcohol-assisted removal and mechanical scraping) and minimizes their adverse effects. The diluted alcohol separates the epithelium and corneal stroma, creating a smooth, regular surface; however, in contrast with the conventional alcohol-assisted technique, no pressure has to be applied to the ocular globe, and no spillage of the solution occurs. Therefore, patient discomfort and surgical trauma to the ocular surface are minimized. The mechanical effect in this technique is produced by a blunt sponge, and, thus, the use of sophisticated or potentially traumatic surgical instruments is unnecessary.
CONCLUSION
Since our description of this technique in 2011,3 most of the surgeons in our group have progressively abandoned their previous debridement methods and have changed to this technique. Those of us who use the combined corneal epithelial debridement technique described here have achieved uniform and easy corneal epithelial removal with minimal patient discomfort (see In Our Experience).
We have recently reported our safety and efficacy results for myopic PRK using this technique.12 In this report, our early refractive and anatomic results were consistent with those in previous reports by other authors using different epithelial debridement techniques for myopic PRK.13-16 Our results with this technique show excellent efficacy, predictability, and safety in eyes with low myopia. We have also used this maneuver for epithelial debridement in other surgical procedures such as CXL and PTK for anterior corneal disorders.
We have seen no adverse effects or unexpected corneal reactions, and the minimization of intraoperative ocular surface damage and reduction in patient discomfort have allowed us to optimize our surgical performance with this refractive procedure.
1. Pop, M, Payette Y. Photorefractive keratectomy versus laser in situ keratomileusis: a control matched study. Ophthalmology. 2000;107:251-257.
2. Hersh PS, Brint SF, Maloney RK, Durrie DS Gordon M, Michelson MA. Photorefractive keratectomy versus laser in situ keratomileusis for moderate to high myopia. A randomized prospective study. Ophthalmology. 1998;105:1512-1522.
3. Bilbao-Calabuig R, González-López F, Villada-Casaponsa JR. Combined ethanol-assisted and blunt mechanical corneal epithelial peeling technique. Journal of Emmetropia. 2014;5:145-149.
4. Campos M, Hertzog L, Wang XW, Fasano AP Mc Donnell PJ. Corneal surface after deepithelization using a sharp and a dull instrument. Ophthalmic Surg. 1992;23:618-621.
5. Melki SA, Azar DT. LASIK complications: etiology, management and prevention. Surv Ophthalmol. 2001;46:95-116.
6. Alio JL, Artola A, Claramonte PJ, et al. Complications of photorefractive keratectomy for myopia: two year follow-up of 3000 cases. J Cataract Refract Surg. 1998;24:619-626.
7. Pallikaris IG, Karoutis AD, Lydataky SE, Siganos DS. Rotating brush for fast removal of corneal epithelium. J Refract Corneal Surg. 1994;10:439-442.
8. Litwack S, Zadok D, García-de Quevedo V, Robledo N, Chayet A. Laser-assisted subepithelial keratectomy for the correction of myopia; a prospective comparative study. J Cataract Refract Surg. 2002;28:1330-1333.
9. Johnson DG, Kezirian GM, George SP, Casebeer JC, Ashton J. Removal of corneal epithelium with phototherapeutic technique during multizone, multipass photorefractive keratectomy. J Refract Surg. 1998;14:38-48.
10. Shah S, Doyle SJ, Chaterjee A, Williams BE Ilango B. Comparaison of 18% ethanol and mechanical debridement for epithelial removal before photorefractive keratectomy. J Refract Surg. 1998;14:S212-S214.
11. Kanitkar KD, Camp J, Humble H, Shen DJ, Wang MX. Pain after epithelial removal by ethanol-assisted mechanical versus transepithelial excimer laser debridement. J Refract Surg. 2000;16(5):519-522.
12. Bilbao-Calabuig R, Gonzalez-Lopez F, et al. Safety and efficacy of photorefractive keratectomy (PRK) for myopia using a new corneal epithelium debridement technique. J Emmetropia. 2015;3:133-137.
13. Einollahi B, Baradaran-Rafii A, Rezaei-Kanavi M, et al. Mechanical versus alcohol assisted epithelial debridement during photorefractive keratectomy: a confocal microscopic clinical trial. J Refract Surg. 2011;27(12):887-893.
14. Shortt AJ, Allan BD, Evans JR. Laser-assisted in-situ keratomileusis (LASIK) versus photorefractive keratectomy (PRK) for myopia. Cochrane Database Syst Rev. 2013;1:CD005135.
15. Shojaei A, Ramezanzadeh M, Soleyman-Jahi S, et al. Short-time mitomycin-C application during photorefractive keratectomy in patients with low myopia. J Cataract Refract Surg. 2013;39(2):197-203.
16. Sia RK, Coe CD, Edwards JD, et al. Visual outcomes after epi-LASIK and PRK for low and moderate myopia. J Refract Surg. 2012;28(1):65-71.
Jaime Beltrán, MD
• Clínica Baviera, Instituto Oftalmológico Europeo, Valencia, Spain
• Financial interest: None acknowledged
Rafael Bilbao-Calabuig, MD
• Clínica Baviera, Instituto Oftalmológico Europeo, Madrid, Spain
• rbilbaocalabuig@hotmail.com • Financial interest: None acknowledged
Miguel A. Calvo-Arrabal, MD
• Clínica Baviera, Instituto Oftalmológico Europeo, Madrid, Spain
• Financial interest: None acknowledged
Felix Gonzalez-Lopez, MD
• Clínica Baviera, Instituto Oftalmológico Europeo, Madrid, Spain
• Financial interest: None acknowledged
Jose R. Villada, MD
• Clínica Baviera, Instituto Oftalmológico Europeo, Albacete, Spain
• Financial interest: None acknowledged